Skin Exposures and Effects
Overview
Some chemicals can enter the body through the skin and injure individual organs or groups of organs. Absorbing workplace chemicals through the skin can cause diseases and disorders that include occupational skin diseases.
Most efforts to address chemical hazards have focused on breathing chemicals in rather than absorbing through skin. Because of this, researchers have developed many ways to assess the effects of chemicals that workers inhale. However, there are fewer methods to assess skin exposures.
NIOSH assigns skin notations. They describe what happens when chemicals contact the skin and directly damage organs or prompt the body’s immune response. The immune response causes skin conditions like allergic contact dermatitis or skin irritation.
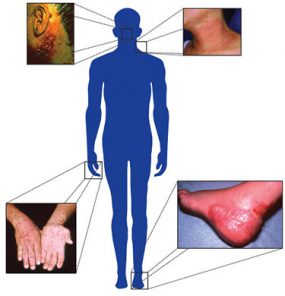
Occupational skin diseases are one of the most common types of workplace diseases. They can take different forms, such as:
- Rash (contact dermatitis) caused by skin irritation
- Rash caused by skin allergies
- Skin cancers
- Skin infections
- Skin injuries
- Other skin diseases
Occupations at Risk
Workers in multiple industries and sectors may face risks of absorbing chemicals through their skin.

Dermal Absorption
Dermal absorption happens when a chemical goes through the skin and travels into the body. Many chemicals used in the workplace can damage organs if they penetrate the skin and enter the bloodstream. Examples of these chemicals include pesticides and organic solvents.
How fast the skin absorbs chemicals depends largely on the outer layer of the skin called the stratum corneum. The stratum corneum provides a barrier by keeping molecules from passing into and out of the skin. This barrier protects the lower layers of skin. How much the skin absorbs chemicals depends on the following factors:
- Skin integrity (damaged or intact)
- The place on the skin where the chemicals are absorbed. (This includes features like thickness and water content of stratum corneum and skin temperature.)
- Physical and chemical properties of the chemical
- Concentration of the chemical on the skin surface
- How long the skin absorbs the chemical
- The surface area of skin that absorbs the chemical
Contact Dermatitis
Contact dermatitis, also called eczema, happens when the skin becomes inflamed from contact with a chemical. Contact dermatitis is the most common form of reported occupational skin disease. Research suggests that contact dermatitis makes up 90–95% of occupational skin disease cases in the United States. Common symptoms of dermatitis include the following:
- Itching
- Pain
- Redness
- Swelling
- Small blisters or wheals (itchy, red circles with a white center) on the skin
- Dry, flaking, scaly skin that may crack
Occupational contact dermatitis is often placed into two categories:
- Irritant contact dermatitis involves a chemical directly damaging and inflaming skin. The damage often occurs only to the place where the skin absorbs the chemical. The following factors may cause irritant contact dermatitis:
- Phototoxic responses (such as tar)
- Brief contact with highly irritating chemicals (such as acids, bases, or oxidizing/reducing agents)
- Mild irritants that cause damage over time (such as water, detergents, or weak cleaning agents).
- Allergic contact dermatitis happens when a chemical that the skin absorbs causes the body’s immune system to produce an allergic reaction. For this to happen, a worker must be sensitive or allergic to the allergen. When the skin absorbs the chemical allergen again, the chemical may cause an immune reaction that inflames the skin. The reaction can go beyond the place where the skin absorbed the chemical. The following factors may cause allergic contact dermatitis:
- Industrial compounds (such as metals, epoxy and acrylic resins, or rubber additives)
- Agrochemicals (such as pesticides and fertilizers)
- Commercial chemicals
The symptoms and the appearance of irritant contact dermatitis and allergic contact dermatitis are similar. Clinical testing (such as patch testing) is often necessary to tell the difference between them. Contact dermatitis can be mild or severe, depending on many factors that include the following:
- Characteristics of the chemical
- Concentration of the chemical
- How often the skin absorbs the chemical
- Environmental factors, such as temperature or humidity
- Condition of the skin, such as healthy or damaged, dry, or wet
