Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Outbreak of Cryptosporidiosis Associated with a Firefighting Response — Indiana and Michigan, June 2011
On June 20, 2011, the Indiana Department of Homeland Security notified the Indiana State Department of Health (ISDH) of an Indiana fire station that reported gastrointestinal illness among a substantial percentage of their workers, causing missed workdays and one hospitalization as a result of cryptosporidiosis. All ill firefighters had responded to a barn fire in Michigan, 15 miles from the Michigan-Indiana border on June 6; responding firefighters from Michigan also had become ill. ISDH immediately contacted the Michigan Department of Community Health (MDCH) concerning this outbreak. The investigation was led by MDCH in partnership with ISDH and the Michigan local health department (LHD). Among 34 firefighters who responded to the fire, 33 were interviewed, and 20 (61%) reported gastrointestinal illness ≤12 days after the fire. Cryptosporidium parvum was identified in human stool specimens, calf fecal samples, and a swimming pond. Based on these findings, the following public health recommendations were issued: 1) discontinue swimming in the pond, 2) practice thorough hygiene to reduce fecal contamination and fecal-oral exposures, and 3) decontaminate firefighting equipment properly. No additional primary or secondary cases associated with this exposure have been reported. The findings highlight a novel work-related disease exposure for firefighters and the need for public education regarding cryptosporidiosis prevention.
On June 6, 2011, a fire occurred in a barn housing approximately 240 week-old calves. A total of 34 firefighters responded from three Michigan fire stations and one Indiana fire station. Local hydrant water and onsite swimming pond water were used to extinguish the fire. Investigators hypothesized that exposures to calves or contaminated drinking water were potential infection sources. A retrospective cohort study was performed among responding firefighters to identify additional ill persons, assess possible risk factors, and guide implementation of control measures. A clinical case was defined as diarrhea (three or more loose stools in a 24-hour period) or gastrointestinal illness (four or more symptoms [e.g., abdominal cramps, nausea, vomiting, or fever]) in a person within 12 days after the fire response. Using CDC case definitions (1), a confirmed case was defined as a clinical case with Cryptosporidium organisms detected in stool, intestinal fluid, or tissue samples; Cryptosporidium antigens in stool or intestinal fluid; or Cryptosporidium nucleic acid in stool. A probable case was defined as a clinical case that lacked laboratory confirmation but was linked epidemiologically to a confirmed case.
Beginning on June 22, MDCH and LHD interviewed firefighters using a standardized telephone questionnaire. Of 34 firefighters from all four fire stations, 33 (97%) completed the interview. Twenty (61%) of 33 study participants had illness meeting the probable (n = 17) or confirmed (n = 3) case definition (Figure). All patients were men; median age was 33 years (range: 21–58 years). Median time from exposure to illness onset was 5 days (range: 2–10 days). Common symptoms included diarrhea (n = 20 [100%]), abdominal cramps (n = 15 [75%]), fatigue (n = 11 [55%]), gas/bloating (n = 11 [55%]), nausea (n = 10 [50%]), and weight loss (n = 10 [50%]). Among 17 (85%) patients whose symptoms had resolved before interview, median illness duration was 4 days (range: 0.5–15 days). Nine (45%) ill firefighters sought medical care; six submitted stool specimens to their health-care providers. A previously healthy immunocompetent man was hospitalized and underwent a cholecystectomy for acalculous cholecystitis secondary to cryptosporidiosis. No deaths were reported.
In bivariate analysis, patients were statistically more likely than nonpatients to have had direct calf contact (e.g., carrying or leading calves from the barn) (relative risk = 2.88; 95% confidence interval = 1.04–12.76); patients also were more likely to have been from the Indiana fire station, had exposure to pond water through drinking or washing themselves, or drunk from a cooler filled with water from an undetermined source, but these associations did not reach statistical significance (Table 1).
The environmental investigation began on June 27. LHD requested stool specimens from symptomatic or recently recovered Michigan patients for confirmatory Cryptosporidium testing (Table 2). Five firefighters provided stool specimens, which were split into three sample tubes (formalin, polyvinyl alcohol, and Cary-Blair) and submitted to MDCH's Bureau of Laboratories and CDC. Twenty-five calf fecal specimens were collected from stalls and submitted to CDC for Cryptosporidium and Giardia testing. Water samples from the swimming pond and drinking well were submitted to CDC's Waterborne Disease Prevention Branch and the Michigan State University Environmental and Molecular Microbiology Laboratory for Cryptosporidium (both laboratories) and Giardia (Michigan State University only) testing. Additionally, a well water sample was submitted to a local water quality–testing laboratory for standard bacterial testing.
Cryptosporidium antigen was detected in one human stool specimen (from the hospitalized patient). Cryptosporidium parvum was identified in two human stool specimens, 10 calf fecal samples, and pond water samples (Table 2). Giardia species were detected in pond water. Four calf fecal samples tested positive for Giardia duodenalis. No human specimens tested positive for Giardia. Although well water tested negative for Cryptosporidium and Giardia, LHD testing revealed that well water had high bacterial (non–Escherichia coli) concentrations and was unsafe for drinking.
LHD recommended that the farmer who owned the barn treat the well water with chlorine and, until the water was declared safe, boil water used for human consumption. On the basis of the presence of Giardia and Cryptosporidium in the swimming pond, difficulty of decontamination, and likely continued contamination with wildlife and livestock fecal matter, LHD recommended the farmer's family no longer use the pond for swimming. The family also was notified by LHD and MDCH of the presence of Cryptosporidium and Giardia in their calf population. Practicing thorough hygiene to reduce fecal contamination and fecal-oral exposures was recommended to the family and firefighters. Furthermore, recommendations were provided to decontaminate firefighter tanker trucks, clothing, and other equipment to prevent further exposure. No secondary cases were identified through firefighter interviews or state disease surveillance system reports.
Reported by
Jo Ann Wilczynski, MS, Branch-Hillsdale-St. Joseph Community Health Agency, Coldwater; Rebecca Ives, MS, Michigan State Univ; Susan Peters, DVM, Tiffany Henderson, MPH, Michigan Dept of Community Health. Jennifer House, DVM, Indiana State Dept of Health. Vincent Hill, PhD, Chandra Schneeberger, Lihua Xiao, DVM, PhD, Theresa Dearen, National Center for Emerging and Zoonotic Infectious Diseases; Jenna Webeck, DVM, EIS Officer, CDC. Corresponding contributor: Jenna Webeck, jwebeck@cdc.gov, 517-335-8165.
Editorial Note
The cryptosporidiosis outbreak described in this report involved 20 firefighters who responded to a fire in a barn housing preweaned calves. Cryptosporidium parvum, the protozoan isolated in this outbreak, can infect humans and ruminants and is more prevalent among preweaned calves than older calves (2). Cryptosporidium previously has been implicated in gastrointestinal illness outbreaks associated with recreational waterparks, contaminated municipal water sources, and exposure to young livestock (1,3). This is the first reported occupational exposure of firefighters to Cryptosporidium species.
Cryptosporidium was detected in the stool of three of six patients tested; two specimens were identified as containing C. parvum, and one was identified only as positive for Cryptosporidium spp. C. parvum also was detected in swimming pond water and calf fecal samples. Failure to detect Cryptosporidium in some infected patients is typical; the parasite is shed intermittently, and often only one stool specimen is collected per patient. Health-care providers do not request Cryptosporidium testing regularly, and routine laboratory testing of stool specimens often does not include Cryptosporidium (1). The actual number of infected firefighters might have been larger than reported because healthy persons infected with Cryptosporidium frequently are asymptomatic and thus they would not have met the case definition. Symptoms typically are self-limiting and can include watery diarrhea, abdominal cramps, low-grade fever, nausea, vomiting, and weight loss (1,4). In this outbreak, the immunocompetent hospitalized patient who experienced cholecystitis likely received an excess of the infectious dose of Cryptosporidium, having fallen into a manure pit while rescuing calves.
Direct contact with calves was linked epidemiologically to illness. Among 20 ill persons, only two did not report direct calf contact. These two patients had both washed themselves at the farm using water that might have been contaminated with Cryptosporidium oocysts. Only 15 of 33 firefighters were asked about pond water exposure because that question was added to the interview tool after interviews had begun. Five of nine firefighters who reported pond water exposure became ill. Although other gastrointestinal pathogens might have contributed to the symptoms experienced by some of the firefighters, the fact that Cryptosporidium was found in stool specimens from three of six firefighters tested suggests that Cryptosporidium was the primary cause of the outbreak.
General prevention and control measures for Cryptosporidium include 1) practicing proper hygiene (e.g., thorough hand washing, not swimming while experiencing diarrhea, and minimizing contact with animal feces); 2) treating or avoiding contaminated water (e.g., not swallowing water while swimming and not drinking untreated water); 3) exercising caution while traveling; and 4) avoiding fecal exposure during sexual activity (1,4). Cryptosporidium is a chlorine-tolerant organism and is not inactivated readily by alcohol-based hand sanitizers.
Although occupationally acquired cryptosporidiosis has been reported among veterinary personnel (5,6), this is the first report of cryptosporidiosis transmitted during a firefighting response. To prevent similar outbreaks, adequate drinking water during firefighting responses and decontamination of firefighting equipment are recommended. Firefighters should only consume treated or bottled water, or sports drinks. Firefighting equipment and clothing should be decontaminated at the scene whenever possible, especially if grossly contaminated with feces, to reduce transmission of Cryptosporidium, Giardia, and other zoonotic enteric pathogens (e.g., E. coli, Salmonella, and Campylobacter). Clothing contaminated with feces should be machine-washed and heat-dried on the highest clothes dryer heat setting for 30 minutes whenever possible (7); all other non–machine-washable items and equipment should be cleaned with soap and water to remove gross fecal contamination, air-dried, and left in the sun for at least 4 hours after drying. For equipment that cannot be cleaned with soap and water or equipment that contacts the mouth (e.g., respirator pieces), soaking in 3% hydrogen peroxide solution for 20 minutes is recommended after consulting manufacturer guidelines (7).
Acknowledgments
Karen Griffith, Kim Brown, Branch-Hillsdale-St. Joseph Community Health Agency, Coldwater; Jordan Assenmacher, Joan Rose, PhD, Michigan State Univ; Jennie Finks, DVM, Corinne Miller, PhD, Bur of Disease Control, Prevention, and Epidemiology, James Rudrik, PhD, Bur of Laboratories, Michigan Dept of Community Health. Jothikumar Narayanan, PhD, Amy Kahler, MS, Jonathan Yoder, MSW, MPH, National Center for Emerging and Zoonotic Infectious Diseases; Jevon McFadden, MD, Office of Surveillance and Public Health Preparedness; Sheryl Lyss, MD, Betsy Cadwell, MSPH, Office of Surveillance, Epidemiology, and Laboratory Services, CDC.
References
- CDC. Cryptosporidiosis surveillance—United States, 2006–2008. MMWR 2010;59(No. SS-6).
- Santin M, Trout JM, Xiao L, Zhou L, Greiner E, Faver R. Prevalence and age-related variation of Cryptosporidium species and genotypes in dairy calves. Vet Parasitol 2004;122:103–17.
- Kiang KM, Scheftel JM, Leano FT, et al. Recurrent outbreaks of cryptosporidiosis associated with calves among students at an educations farm programme, Minnesota, 2003. Epidemiol Infect 2006;134:878–86.
- CDC. Prevention and control of cryptosporidiosis. Atlanta, GA: US Department of Health and Human Services, CDC; 2010. Available at http://www.cdc.gov/parasites/crypto/prevention.html. Accessed February 29, 2012.
- Levine JF, Levy MG, Walker RL, Crittenden S. Cryptosporidiosis in veterinary students. J Am Vet Med Assoc 1988;193:1413–4.
- Konkle DM, Nelson KM, Lunn DP. Nosocomial transmission of Cryptosporidium in a veterinary hospital. J Vet Intern Med 1997;11:340–3.
- CDC. Control measures for outbreaks: intensified cryptosporidiosis (crypto) control measures for the child care setting. Atlanta, GA: US Department of Health and Human Services, CDC; 2011. Available at http://www.cdc.gov/parasites/crypto/daycare/outbreak.html. Accessed February 29, 2012.
What is already known on this topic?
Cryptosporidiosis has been implicated in outbreaks involving recreational water use, contaminated municipal water, and exposure to infected animals.
What is added by this report?
This is the first report of cryptosporidiosis being a potential occupational hazard for rural firefighters. Twenty of 34 firefighters responding to a fire in a barn housing week-old calves became ill with gastrointestinal symptoms; three of six tested were positive for Cryptosporidium. Cryptosporidium parvum was identified in samples from two of the firefighters, the calves, and a nearby swimming pond.
What are the implications for public health practice?
Firefighters, like other visitors to facilities housing livestock, are at potential risk for Cryptosporidium infection. This investigation highlights the continued importance of public education regarding cryptosporidiosis prevention and control, in particular the importance of minimizing contact with animal feces, practicing thorough hygiene, and not drinking from untreated water sources.
FIGURE. Number of probable and confirmed cryptosporidiosis cases* among firefighters who responded to a barn fire, by date of illness onset and fire department — Indiana and Michigan, June 2011
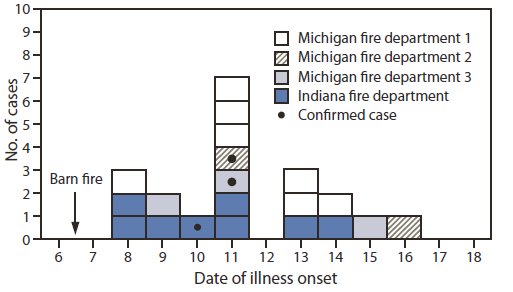
* A clinical case was defined as diarrhea (three or more loose stools in a 24-hour period) or gastrointestinal illness (four or more symptoms [e.g., abdominal cramps, nausea, vomiting, or fever]) in a person within 12 days after the fire response. A confirmed case was defined as a clinical case with Cryptosporidium organisms detected in stool, intestinal fluid, or tissue samples; antigens in stool or intestinal fluid; or nucleic acid in stool. A probable case was defined as a clinical case that lacked positive laboratory confirmation but was linked epidemiologically to a confirmed case. Cases not marked as confirmed are probable cases.
Alternate Text: The figure above shows the number of probable and confirmed cryptosporidiosis cases among firefighters who responded to a barn fire, by date of illness onset and fire department, in Indiana and Michigan during June 2011. Of 34 firefighters from all four fire stations, 33 (97%) completed the interview. Twenty (61%) of 33 study participants had illness meeting the probable (n = 17) or confirmed (n = 3) case defini¬tion.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


