Key points
- Each year, up to 225 people in the U.S. and 250,000 around the world are diagnosed with leprosy.
- Leprosy was once feared as a highly contagious, devastating disease.
- We now know that it's hard to spread and easily treatable.
- People with leprosy can live an active life during and after treatment.
What it is
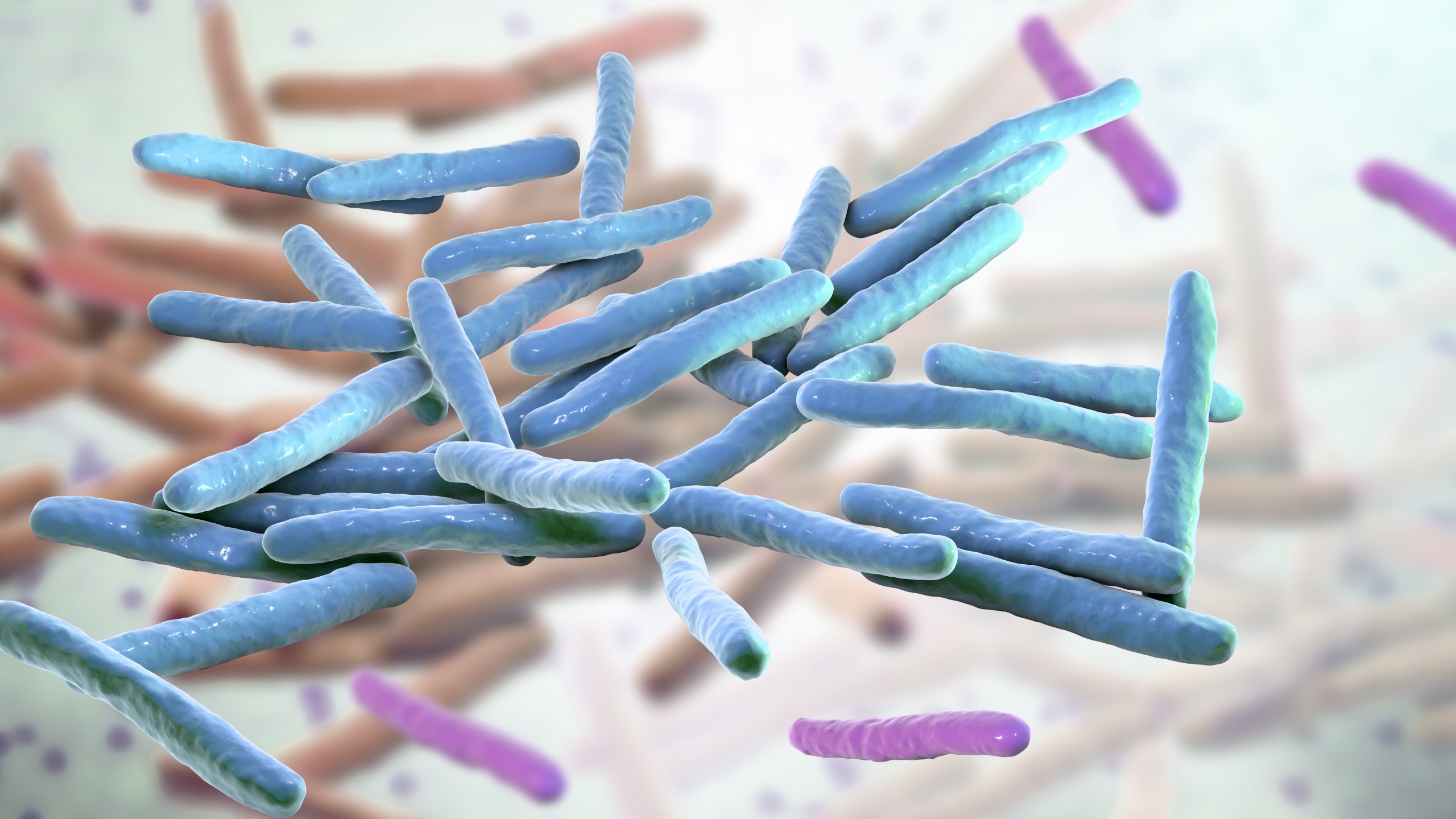
Leprosy (Hansen's disease) is caused by slow-growing bacteria called Mycobacterium leprae and Mycobacterium lepromatosis. The disease can affect the nerves, skin, eyes, and lining of the nose. In some cases, body parts may lose their sense of touch and pain, increasing the likelihood of injuries such as cuts and burns
Despite the disease being hard to catch and completely curable, a lot of stigma and prejudice remains against those who have leprosy. People affected by the disease often face social isolation and discrimination, particularly in regions where the illness is more common.
Signs and symptoms
The bacteria that causes leprosy grows very slowly. It may take up to 20 years after contact with the bacteria to develop signs of the disease.
Symptoms mainly affect the skin, nerves, and lining of the nose. If it's left untreated or treated late, it can cause serious complications and disabilities.
Where it occurs
In the United States, leprosy is rare. Most people with leprosy in the United States became infected in a country where it is more common.
You may be at risk for the disease if you live in a country where the disease is widespread. According to data from 2023:
- Brazil, India, and Indonesia reported more than 10,000 new cases
- Bangladesh, Democratic Republic of the Congo, Ethiopia, Madagascar, Mozambique, Myanmar, Nepal, Nigeria, the Philippines, Somalia, Sri Lanka, and the United Republic of Tanzania each reported 1,000–10,000 new cases.
How it spreads
Person-to-person
Leprosy does not spread easily between people. You must have prolonged, close contact with someone with untreated leprosy over many months to catch the disease.
Leprosy likely spreads when a person sick with the disease coughs or sneezes and a healthy person breathes in the droplets repeatedly over a long period of time.
Around 95% of people cannot get leprosy because their immune system can fight off the bacteria that causes it. It’s not spread through sex, and it is not passed to the fetus during pregnancy.
Armadillos
In the southern United States, some armadillos are naturally infected with the bacteria that cause leprosy, and it may be possible that the animals can spread it to people. However, the risk is very low and most people who come into contact with armadillos are unlikely to get leprosy.
Testing and diagnosis
Healthcare providers can diagnose leprosy by conducting an exam and running diagnostic tests, like skin biopsies. They may look for patches of skin that look lighter, darker, or redder than the person's normal skin and determine if those patches have a loss of feeling.
To confirm the diagnosis, healthcare providers will take a skin or nerve sample to look for the bacteria that cause leprosy under the microscope. They may also do tests to rule out other skin diseases.
Treatment and recovery
Leprosy is treated with a combination of antibiotics. Treatment usually lasts between one to two years. The illness can be cured if treatment is completed as prescribed.
In the United States, people with leprosy may be treated at specialized clinics run by the National Hansen's Disease Program. There are several federally supported outpatient clinics throughout the continental United States and Puerto Rico.
Myths and misconceptions
Myth: Leprosy is very contagious.
Fact: Leprosy does not spread easily from person to person. You cannot get it through casual contact such as shaking hands, sitting next to, or talking to someone who has the disease.
Myth: There is no cure for leprosy.
Fact: Leprosy is curable. People being treated for the disease can live a normal life among their family and friends and can continue to attend work or school.
Myth: Leprosy makes your fingers and toes fall off.
Fact: Fingers and toes do not just “fall off” due to leprosy. The bacteria that cause the disease attacks the nerves of the fingers and toes, causing them to become numb. Injuries like burns, ulcers, and cuts on numb parts can go unnoticed, which may lead to permanent damage or infection, causing loss of the digit. Sometimes, the nerve damage makes muscles in the fingers and toes so weak that the muscles and bones are reabsorbed by the body, making them look shorter.
- Britton WJ, Lockwood NJ. Leprosy. Source: Lancet. 2004;363:1209-1219.
- Bruce S, Schroeder TL, Ellner K, Rubin H, Williams T, Wolf JE Jr. Armadillo exposure and Hansen's disease: an epidemiologic survey in southern Texas. Source: J Am Acad Dermatol. 2000;43(2 Pt1):223-228.
- Hansen's Disease | Technical Instructions for Civil Surgeons | Immigrant and Refugee Health | CDC Last updated: 2024 May 14. Accessed: 2024 June 6.
- Hartzell JD, Zapor M, Peng S, Straight T. Leprosy: a case series and review. Source: South Med J. 2004;97:1252-1256.
- Martiniuk F, Rao SD, Rea TH, et al. Leprosy as Immune Reconstitution Inflammatory Syndrome in HIV-positive Persons. Source: Emerging Infectious Diseases. 2007;13(9):1438-1440. doi:10.3201/eid1309.070301.
- Nolen L, Haberling D, Scollard D, et al. Incidence of Hansen's Disease — United States, 1994–2011. Source: Morbidity and Mortality Weekly Report (MMWR). 2014 / 63(43);969-972.
- Ooi WW, Moschella SL. Update on leprosy in immigrants in the United States: status in the year 2000. Source: Clin Infect Dis. 2001;32:930-937.
- Scollard DM, Adams LB, Gillis TP, Krahenbuhl JL, Truman RW, Williams DL. The continuing challenges of leprosy. Source: Clinical Microbiology Reviews. 2006;19(2):338-381.
- Truman, RW, Singh, P., Sharma, R, Busso, JP, Rougemont, J, Paniz-Mondolfi, A, Kapopoulou, A, Brisse, S, Scollard, DM, Gillis, TP, and Cole, ST. Probable Zoonotic Leprosy in the Southern United States. Source: N Engl J Med. 2011;364:1626-1633.
- Williams D, Hagino T, Sharma R, et al. Primary Multidrug-Resistant Leprosy, United States. Source: Emerging Infectious Diseases. 2013;19(1):179-181. doi:10.3201/eid1901.120864.
- Woodall P, Scollard DM, Rajan L. Hansen Disease among Micronesian and Marshallese Persons Living in the United States. Source: Emerging Infectious Diseases. 2011;17(7):1202-1208. doi:10.3201/eid1707.102036.
- World Health Organization. Surveillance of drug resistance in leprosy: 2010. Source: Wkly Epidemiol Rec. 2011;86:237–240.
- World Health Organization. Global leprosy update, 2015: time for action, accountability and inclusion. Source: Wkly Epidemiol Rec. 2016; 91:405–420.
- Worobec SM. Current approaches and future directions in the treatment of leprosy. Source: Res Rep Trop Med. 2012;3:79–91.
