Key points
- For most people, cytomegalovirus (CMV) infection is not a serious health problem.
- Diagnose, treat, and monitor children with congenital CMV to help improve their health outcomes.
- Perform CMV testing, evaluation, and treatment per routine institutional protocols.

Types
CMV is a member of the herpesvirus family, which includes:
- Herpes simplex virus types 1 and 2
- Varicella-zoster virus
- Epstein-Barr virus
These viruses share a characteristic ability to establish lifelong latency. Once a person becomes infected, the virus remains latent and resides in cells without causing detectable damage or illness.
CMV may reactivate occasionally. Reactivation of CMV infection rarely causes disease unless the person’s immune system is suppressed due to therapeutic drugs or disease.
Who is at risk
For most people, CMV infection is not a serious health problem. However, certain groups are at high risk for serious complications from CMV infection:
- Infants infected in utero (congenital CMV infection)
- Very low birth weight and premature infants
- People with compromised immune systems, such as from organ and bone marrow transplants, and people infected with human immunodeficiency virus (HIV)
The risk of CMV complications to the fetus is greatest if a primary infection occurs during the first trimester.
How it spreads
CMV is spread through:
- Contact with infectious body fluids (urine, saliva, blood, tears, semen, and breast milk)
- Sexual contact
- Transplanted organs and blood transfusions
- Contact with the mother's genital secretions during delivery
Although the virus is not highly contagious, it has been shown to spread among household members and young children in daycare centers.
A pregnant woman can pass CMV to their baby following a:
- Primary infection
- Reinfection with a different CMV strain
- Reactivation of a previous infection during pregnancy
Risk of transmission for primary infection is 30 to 40% in the first and second trimesters, and 40 to 70% in the third trimester. The risk of transmission following non-primary infection is much lower (3%).
Signs and symptoms
Most healthy people, children, and infants who acquire CMV after birth have few symptoms and no long-term health complications from infection.
Some people who acquire CMV infection may experience a mononucleosis-like condition with prolonged fever and hepatitis.
At birth
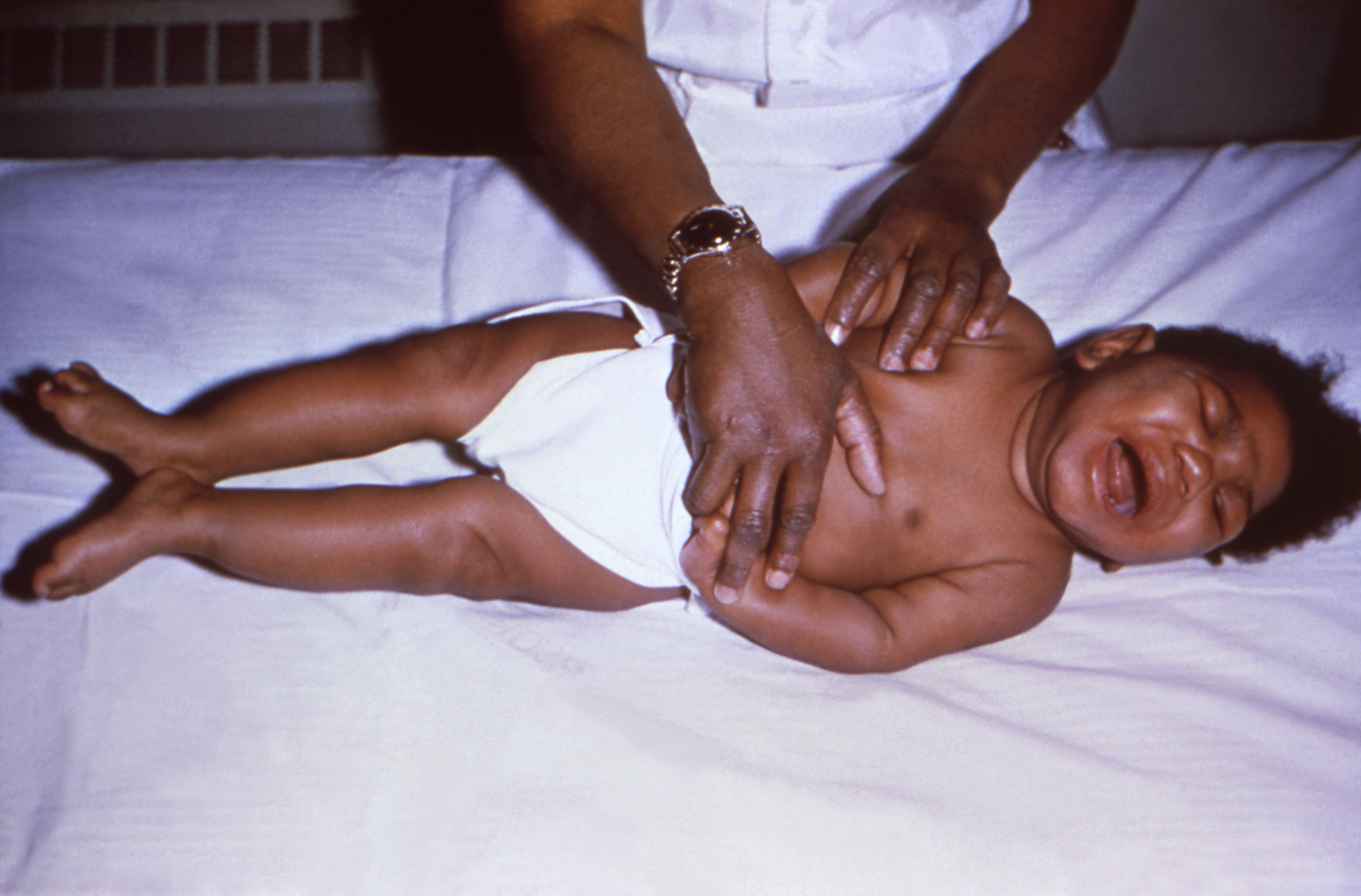
Most infants born with CMV infection never have health problems. About 10% of infants with congenital CMV infection will have signs at birth, which include:
- Petechiae/purpura (blood spots)
- Jaundice (yellowing of the skin or whites of the eyes)
- Microcephaly (small head)
- Intrauterine growth (low birth weight)
- Hepatosplenomegaly (enlarged liver and spleen)
- Seizures
- Retinitis (damaged eye retina)
Long-term health problems
About 40 to 60% of infants born with signs of congenital CMV disease at birth will have long-term health problems. These can be:
- Hearing loss
- Developmental and motor delay
- Vision loss
- Microcephaly (small head)
- Lack of coordination or weakness
- Seizures
Some babies may have hearing loss that may or may not be detected by newborn hearing test.
Prevention
CMV is common in children and can be found in especially high amounts in young children’s saliva and urine. Avoiding contact with saliva and urine from young children might reduce the risk of CMV infection. Healthcare providers should follow standard precautions.
CMV vaccines are currently in clinical trials. Learn more about how vaccines are licensed and recommended.
Testing and diagnosis
Because the signs of CMV infection are similar to other medical conditions, laboratory testing is needed to confirm congenital CMV. Testing should be done within 2 to 3 weeks after birth. If testing is done after 3 weeks, it's not possible to distinguish between congenital CMV infection and infection acquired after birth.
Testing should be done on the baby’s saliva, urine, or blood using polymerase chain reaction (PCR) to detect CMV DNA. A PCR on saliva is preferred, with a confirmation test on urine. Congenital CMV infection cannot be diagnosed with antibody testing (IgG and IgM).
Treatment and recovery
No treatment is currently indicated for CMV infection in healthy people. Antiviral treatment is used for people with compromised immune systems who have either sight-related or life-threatening illnesses due to CMV infection.
Treat early
Antiviral medications such as ganciclovir or valganciclovir may improve hearing and developmental outcomes in newborns with signs of congenital CMV. Ganciclovir can have serious side effects and has only been studied in infants with symptomatic congenital CMV disease. There is limited information on the effectiveness of ganciclovir or valganciclovir to treat infants with hearing loss alone.
Monitor symptoms
Any newborn diagnosed with congenital CMV infection should have regular hearing and vision tests. Most infants with congenital CMV grow up healthy. Some babies may have hearing loss that may or may not be detected by newborn hearing test. Hearing loss can be present at birth or develop later and may progress with age.
Help parents get services their children need
As a healthcare provider, you play an important role in helping parents understand the services a child with congenital CMV infection may need. This can include getting hearing aids, regular hearing and vision screenings, and speech, occupational, and physical therapy.
Patient counseling
CMV spreads more from primary infection
In the United States, nearly half of women have been infected with CMV before their first pregnancy. Of women who have never had a CMV infection, it is estimated that 1 to 4% of them will be infected during pregnancy.
A pregnant woman who has a primary CMV infection during pregnancy is more likely to pass CMV to the fetus than someone who has a subsequent infection during pregnancy. However, in the United States, 50 to 75% of congenital CMV infections occur among infants born to mothers who were infected with CMV before they became pregnant.
Routine screening is not recommended
Routine screening for primary CMV infection during pregnancy is not recommended in the United States.
Reasons:
- Most laboratory tests currently available to identify a first-time infection can be difficult to interpret.
- Current tests cannot predict if the fetus may become infected or harmed by infection.
- The lack of a proven treatment to prevent or treat infection of the fetus reduces the potential benefits of prenatal screening.
Breastfeeding
There are no recommendations against breastfeeding by mothers who are CMV-seropositive. However, infants born <30 weeks gestational age and <1500g who acquire CMV from breast milk may be at risk of developing a late-onset sepsis-like syndrome.
Consider the potential benefits of human milk versus the risk of CMV transmission when making a decision about the breastfeeding of very premature babies by CMV-seropositive mothers.
Freezing and pasteurization of breast milk can decrease the risk of transmission. However, freezing does not eliminate risk.
