Key points
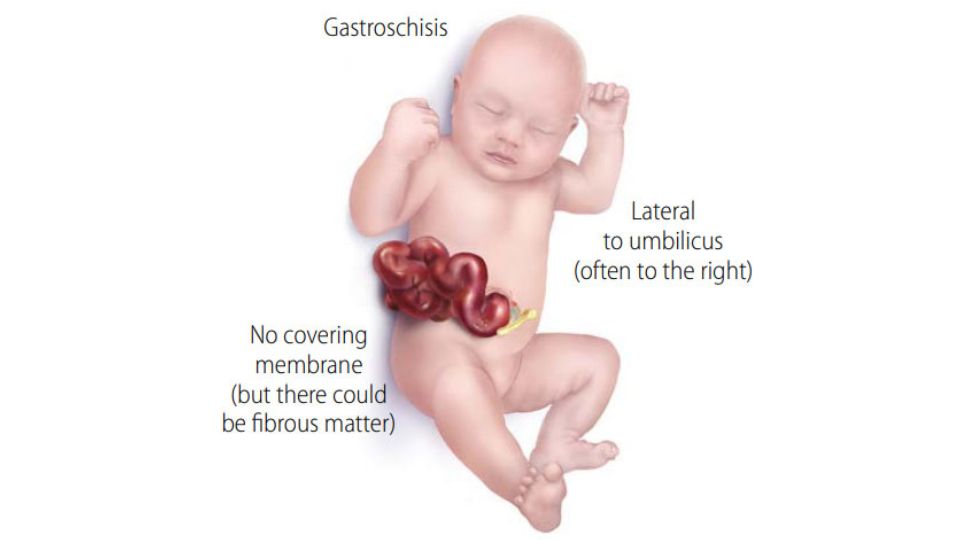
- Gastroschisis (gas-troh-skee-sis) is a condition where the intestines extend outside of the body through a hole beside the belly button.
- Surgery places the abdominal organs inside the baby’s body and repair the hole.
- Researchers estimate 1 in every 2,564 babies is born with gastroschisis in the US.
What it is
Gastroschisis is a birth defect where there is a hole in the abdominal (belly) wall beside the belly button. This results in the baby's intestines extending outside of the baby's body.
Sometimes other organs, such as the stomach and liver, can be found outside of the baby's body.
Gastroschisis occurs early during pregnancy and the hole is usually to the right side of the belly button. Because the intestines are not covered in a protective sac and are exposed to the amniotic fluid, they can become irritated. This can cause them to shorten, twist, or swell.
Risk factors
The causes of gastroschisis in most cases are unknown. It is likely caused by a combination of genes and other factors. Research studies have found some factors that might increase the risk of having a baby with gastroschisis:
Screening and diagnosis
Gastroschisis can be diagnosed during pregnancy or immediately after the baby is born. Gastroschisis might causes an abnormal result on a blood or serum screening test. It might also be seen during an ultrasound.
Treatment
Soon after birth, surgery will be needed to place the abdominal organs inside the baby's body and repair the hole. Even after the repair, infants can have problems with eating, digestion of food, and absorption of nutrients.
If only some of the intestine is outside of the belly, it is usually treated with surgery soon after birth. If many organs are outside of the belly, the repair might be done slowly, in stages. The exposed organs might be covered with a special material and slowly moved back, and then the opening is closed.
Babies with gastroschisis often need other treatments as well. These can include receiving nutrients through an IV, antibiotics to prevent infection, and careful attention to control their body temperature.
Resources
The views of this organization are its own and do not reflect the official position of CDC.
The Global Gastroschisis Foundation: The Global Gastroschisis Foundation helps children and families affected by gastroschisis. The website has resources for connecting with other families and ways to raise awareness about gastroschisis.
- Kirby RS, Marshall J, Tanner JP, et al.; for the National Birth Defects Prevention Network. Prevalence and correlates of gastroschisis in 15 states, 1995 to 2005. Obstet Gynecol. 2013 Aug; 122 (2 Pt 1):275-81.
- Jones AM, Isenburg J, Salemi JL, et al.; for the National Birth Defects Prevention Network. Increasing prevalence of gastroschisis—14 States, 1995-2012. MMWR morb Mortal Wkly Rep. 2016 Jan 22;65(2):23-6.
- Bird TM, Robbins JM, Druschel C, Cleves MA, Yang S, Hobbs CA, the National Birth Defects Prevention Study. Demographic and environmental risk factors for gastroschisis and omphalocele in the National Birth Defects Prevention Study. J Pediatr Surg. 2009;44:1546-1551.
- Feldkamp ML, Arnold KE, Krikov S, Reefhuis J, Almli LM, Moore CA, Botto LD. Risk of gastroschisis with maternal genitourinary infections, National Birth Defects Prevention Study 1997-2011. BMJ Open. 2019; 9:e026297.
- Stallings, E. B., Isenburg, J. L., Rutkowski, R. E., Kirby, R. S., Nembhard, W.N., Sandidge, T., Villavicencio, S., Nguyen, H. H., McMahon, D. M., Nestoridi, E., Pabst, L. J., for the National Birth Defects Prevention Network. National population-based estimates for major birth defects, 2016–2020. Birth Defects Research. 2024 Jan;116(1), e2301.
