Signs and Symptoms
Early signs and symptoms are not specific to RMSF (including fever and headache). However, the disease can rapidly progress to a serious and life-threatening illness. See your healthcare provider if you become ill after having been bitten by a tick or having been in the woods or in areas with high brush where ticks commonly live.
Signs and symptoms can include:
- Fever
- Headache
- Rash
- Nausea
- Vomiting
- Stomach pain
- Muscle pain
- Lack of appetite
Rash
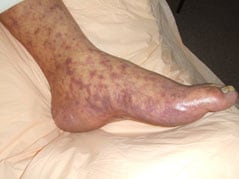
Figure 1. Late stage rash in a patient with Rocky Mountain spotted fever.
Rash is a common sign in people who are sick with RMSF. Rash usually develops 2-4 days after fever begins. The look of the rash can vary widely over the course of illness. Some rashes can look like red splotches and some look like pinpoint dots. While almost all patients with RMSF will develop a rash, it often does not appear early in illness, which can make RMSF difficult to diagnose.
Long-term Health Problems
- RMSF does not result in chronic or persistent infections.
- Some patients who recover from severe RMSF may be left with permanent damage, including amputation of arms, legs, fingers, or toes (from damage to blood vessels in these areas); hearing loss; paralysis; or mental disability. Any permanent damage is caused by the acute illness and does not result from a chronic infection.
