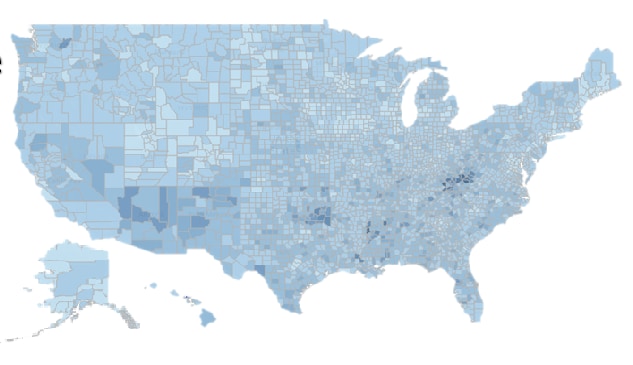
Social Determinants of Health, Health Equity, and Vision Loss

Did you know that social factors such as where a person lives and how much money a person makes can increase the risk of vision loss?
These and other social determinants may be affecting vision health more than you know.
Social determinants of health (SDOH) are the conditions in places where people are born, live, learn, work, play, worship, and age that affect a wide range of health risks and outcomes. Healthy People 2030 breaks SDOH into five key domains:
Education includes educational attainment—graduating from high school and enrollment in higher education—language and literacy, and early childhood education and development.
Health and health care include access to primary care, health insurance coverage, and health literacy.
Neighborhood and built environment objectives include neighborhood crime and violence, quality of housing, access to transportation, availability of healthy foods, and air and water quality.
Social and community context objectives include community cohesion, civic participation, discrimination, conditions in the workplace, and incarceration.
Economic stability includes poverty, employment, food and nutrition security, and housing stability.
Why are SDOH important? They are key drivers of health inequities—especially among communities of color—that increase the risk for poor health outcomes. Reducing and eliminating these disparities is essential to reaching health equity.
Vision loss ranks among the top 10 causes of disability in the US.
Learn more about the burden of vision loss.
Burden of Vision Loss
Vision loss ranks among the top 10 causes of disability in the United States. An estimated 7 million Americans have vision impairment, including 1 million who are blind.1 Of this group, about 2 million children and adults aged 40 years and younger have uncorrectable vision impairment or blindness.1 These numbers are expected to double by 2050 because of the aging US population and the expected increase in chronic diseases that can cause vision loss, such as diabetes.2
The leading causes of blindness and vision impairment are primarily age-related eye diseases, such as diabetic retinopathy, glaucoma, age-related macular degeneration, and cataracts.
- Diabetic retinopathy is the leading cause of severe vision loss and blindness among working-age Americans. More than 34 million people in the United States have diabetes, and 1 out of 3 Americans will develop diabetic retinopathy.
- Glaucoma is one of the leading causes of irreversible blindness in the United States, and currently there is no cure. More than 3 million Americans have glaucoma. By 2050, that number is expected to rise to 6.3 million.
- Age-related macular degeneration (AMD) is the leading cause of permanent vision loss among people aged 65 years and older. Nearly 2 million Americans aged 40 years and older are affected by AMD. The number of people with AMD is estimated to rise to 5.4 million by 2050.
- Cataracts can occur at any age because of many causes, but most are age-related and develop as people get older. An estimated 20.5 million Americans aged 40 years and older have a cataract in one or both eyes. That number is expected to more than double to about 50 million by 2050.
Vision Health Equity
Risk factors for eye disease include race/ethnicity, age, sex, and having a chronic health condition such as diabetes, high blood pressure, or heart disease. Also, behavioral factors such as smoking and being physically inactive can increase the risk of vision loss.
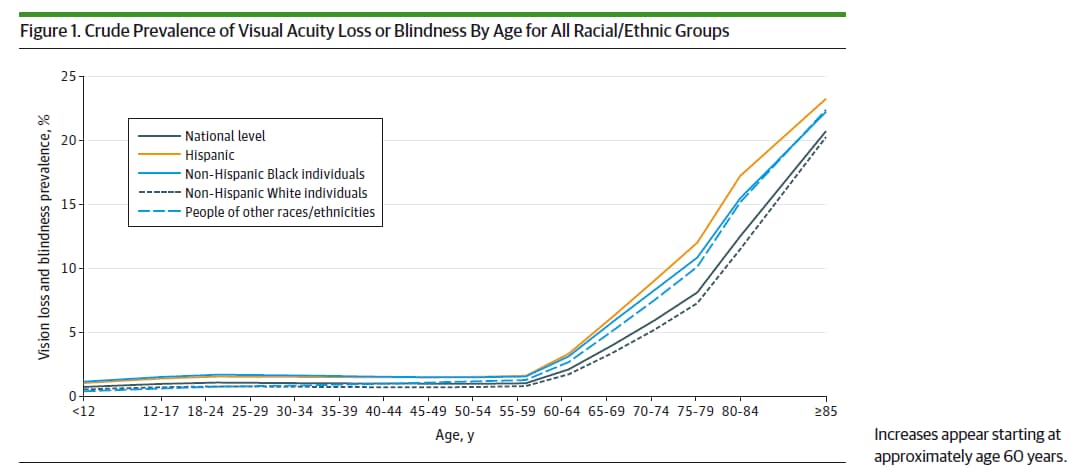
Research has shown that SDOH are also linked to vision loss.3 A recent study found that people who reported having visual difficulty were more likely to:
- Have a lower education level.
- Have health care coverage through Medicaid.
- Have food insecurity.
- Have problems paying medical bills.
- Have trouble finding a doctor.
- Skip doses of medicine because of cost.
- Identify as a gay male.
The following social factors play an important role in vision loss:
- Income: People with lower incomes are less likely to have had preventive care, including an eye exam, or to be able to afford eyeglasses and are more likely to have vision loss due to diabetic retinopathy.4-7
- Education: People with less than a high school education are less likely to have had an eye care visit in the last year compared with people who have more than a high school education.4
- Neighborhood: Neighborhood safety could affect diabetes-related stress, physical activity, weight management, and blood sugar levels—all of which are risk factors for chronic conditions that can lead to vision loss.8
- Access to care: People living with a disability such as vision impairment or blindness report having more problems in accessing care, such as cost of care, availability of insurance coverage, transportation issues, and refusal of services by providers. People who have vision impairment are more likely to be uninsured compared with people who do not.9
Addressing these barriers is key to eliminating health disparities and reaching vision health equity.
What the Vision Health Initiative Is Doing
The Vision Health Initiative (VHI) is partnering with professional organizations, tribes, scientific researchers, community organizations, and community members to support programs and initiatives to prevent vision loss and blindness in communities that are underserved. The following examples provide snapshots of VHI efforts.
Vision and Eye Health Surveillance System
VHI partnered with National Opinion Research Center (NORC) at the University of Chicago to develop the National Vision and Eye Health Surveillance System (VEHSS) to understand the scope of vision loss, eye disorders, and eye care services in the United States. NORC uses innovative statistical modeling to integrate data sources to estimate the prevalence of vision loss and eye disease across the nation. VEHSS is currently working on including data on SDOH to enable community programs and interventions to help identify social factors associated with vision impairment in their area.
VHI’s Glaucoma Program
The glaucoma program is working with three funded academic institutions and a coordinating center to develop strategies to reach populations disproportionately affected by vision loss. These populations are less likely to have access to eye care to detect and manage glaucoma and other eye diseases in community-based settings. The University of Alabama at Birmingham, Columbia University, and the University of Michigan established the Screening and Interventions for Glaucoma and Eye Health Through Telemedicine (SIGHT) studies to improve glaucoma detection and management among populations at high risk for glaucoma. By bringing eye care services to under-resourced communities, the SIGHT studies are addressing barriers such as unemployment, lack of health insurance, poverty, and inadequate educational systems, transportation, and community resources such as optometrists and ophthalmologists.
VHI’s State Partnership Projects
VHI works with the National Association of Chronic Disease Directors (NACDD) to support and build state capacity focusing on leadership development, effective partnerships, and carrying out effective and sustainable interventions to improve vision and eye health. In partnership with NACDD, VHI funds eight state partners working to improve vision health equity in populations at higher risk of vision loss and least likely to have access to eye care. These projects provide access to vision screening in local health departments and community health clinics and by innovative telehealth services to people who are most likely to have health conditions such as diabetes that cause vision loss. As the sites move to a self-sustaining model, patients will benefit from having a more permanent local resource for eye care.
References
- Flaxman AD, Wittenborn JS, Robalik T, et al. The prevalence of visual acuity loss or blindness in the US: a Bayesian meta-analysis. JAMA Ophthalmol. Published online May 13, 2021. doi:10.1001/jamaophthalmol.2021.0527
- Varma R, Vajaranant TS, Burkemper B, et al. Visual impairment and blindness in adults in the United States: demographic and geographic variations from 2015 to 2050. JAMA Ophthalmol. 2016;134(7):802–809.
- Su NH, Moxona NR, Wang A, French DD. Associations of social determinants of health and self-reported visual difficulty: analysis of the 2016 National Health Interview Survey. Ophthalmic Epidemiology. 2020;27(2):93–97.
- Zhang X, Cotch MF, Ryskulova A, et al. Vision health disparities in the United States by race/ethnicity, education, and economic status: findings from two nationally representative surveys. Am J Ophthalmol. 2012;154:S53–S62.
- Barsegian A, Kotlyar B, Lee J, Salifu MO, McFarlane SI. Diabetic retinopathy: focus on minority populations. Int J Clin Endocrinol Metab. 2017;3(1):34–45.
- Saydah SH, Gerzoff RB, Saaddine JB, Zhang X, MD, Cotch MF. Eye care among US adults at high risk for vision loss in the United States in 2002 and 2017. JAMA Ophthalmol. 2020;138(5):479–489.
- Gibson DM. Food insecurity, eye care receipt, and diabetic retinopathy among US adults with diabetes: Implications for primary care. J Gen Intern Med. 2019;34:1700–1702.
- Tamayo A, Karter AJ, Mujahid MS, et al. Associations of perceived neighborhood safety and crime with cardiometabolic risk factors among a population with type 2 diabetes. Health Place. 2016;39:116–21.
- Spencer C, Frick K, Gower EW, Kempen JH, Wolff JL. Disparities in Access to Medical Care for Individuals with Vision Impairment. Ophthalmic Epidemiology. 2009;16(5):281–288.