Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Advice to a Modern-Day Rip Van Winkle: Changes in State and Local Public Health Practice During the MMWR Era at CDC
Corresponding author: Melvin A. Kohn, MD, 800 N.E. Oregon, Suite 930, Portland, OR 97232;Telephone: 971-673-1300; Fax 971-673-1361; E-mail: melvin.a.kohn@state.or.us.
Imagine for a moment a dedicated but exhausted state or local public health practitioner nodding off while reading the volume 10, number 1, issue of MMWR in January of 1961, only to awaken, a la Rip Van Winkle, 50 years later (1). What would be most surprising to our time-traveling colleague about state and local public health practice in 2011? Here is our top 10 list.
1. There are some "old" diseases about which you no longer have to worry much and some "new" ones you do.
Buy yourself an up-to-date infectious disease textbook. Vaccines have driven rates of many diseases that were common in 1961 to very low levels today in the United States. Polio, measles, invasive Haemophilus influenzae disease, and diphtheria are rarities, and smallpox has been eradicated (Table). In fact, it has become a challenge to get health practitioners to recognize these old diseases when they do occur and to mount a rapid, competent public health response to them unless a "senior" epidemiologist happens to be around. After your experiences with controlling polio in the United States during the 1950s, you might be amazed at the increasing problem of "vaccine hesitancy" (2). The rarity of many of the old diseases has made it difficult to convince a growing subset of parents to vaccinate their children against them.
On the treatment side, rates of tuberculosis (TB) have been driven to historic lows, and in many jurisdictionsTB expertise has all but disappeared. At the same time, drug treatment for TB and many other infectious diseases has become complicated by the continuing emergence of strains resistant to common treatments (3).
Read that new textbook carefully because many infectious diseases of importance today were unknown (or unrecognized) when you fell asleep in 1961. Legionnaires disease (4), toxic-shock syndrome (5), hantavirus pulmonary syndrome (6), Lyme disease (7), cryptosporidiosis (8), norovirus infection (9), and Escherichia coli O157:H7 infection (10) are a few examples. Most commonly, these new illnesses were identified as a result of outbreak investigations by CDC together with state health departments. A key to success at characterizing and controlling these new diseases has been an explosion of new laboratory techniques, such as pulsed-field gel electrophoresis and polymerase chain reaction (you may need a textbook on infectious disease laboratory testing as well), which have enabled more sensitive testing and more specific characterization of pathogens. The creation of national surveillance systems, such as PulseNet (11) (which allows comparison of the molecular "fingerprints" of foodborne pathogens from across the country), has helped in the detection of many more multistate outbreaks (and provided lots of practice on improving cross-jurisdictional and cross-agency coordination).
2. There is a global HIV pandemic.
The first five cases of what is now called acquired immunodeficiency syndrome (AIDS) were reported in MMWR in 1981 (12). Since then, human immunodeficiency virus (HIV, the virus that causes AIDS) has caused approximately 25 million deaths across the world, and in 2007 alone, 2.7 million new infections occurred (13), painfully showing the limits of traditional approaches to communicable disease control.
In 1961, control of sexually transmitted diseases focused primarily on providing health education, treatment, and contact tracing. For HIV, the lack of a cure and a vaccine has limited our ability to use these traditional tools. Moreover, traditional health education and contact tracing is more complicated and less useful among persons at highest risk in this country---men who have sex with men and injection drug users (drug use became epidemic while you slept) (14,15). To implement effective harm-reduction strategies, public health and health-care professionals have needed to work closely with those at highest risk and to partner with leaders and community-based organizations from these socially marginalized communities.
This work has brought public health into the dangerous shoals of culture wars around sexuality, homosexuality, abstinence, drug use, and personal responsibility. Today, managing conflicts with politicians and mainstream cultural beliefs is now part of routine work. Especially at the beginning of the AIDS epidemic in the 1980s, the lack of empowerment and stigmatization of homosexuals, racial and ethnic minorities, and women were major contributors to the behaviors that fueled the spread of HIV (16), and the emergence of HIV has highlighted for many practitioners the link between public health and human rights.
By providing the dispassionate imprimatur of solid science for issues such as needle exchange (17) and HIV reporting systems (18), CDC and MMWR have helped practitioners maintain focus on disease prevention as the primary objective. But on many occasions, politics have prevailed over good science, teaching the limits of pure science-based public health practice.
3. Health care dominates the United States economy, but many public health agencies do not see many patients anymore.
The health-care industry accounted for 17% of the U.S. gross national product in 2009 (19), compared with 5% in 1960 (20), and its political and financial clout today is considerable (think military--industrial complex of your day to get an idea of its influence). Health care is now competing---and usually winning---against public health programs and many other public needs for a growing slice of the government budget pie. Since 1961, large national health insurance programs have been implemented (called Medicare for elderly and disabled persons and Medicaid for poor persons), although many Americans remain uncovered. The private medical-care system also has grown tremendously, and large for-profit health systems are a dominant force. Prevention outside of the health-care provider's office gets comparatively little attention or funding. As costs have risen, health insurance financing has become the dominant focus of public policymaking related to health.
Despite---or perhaps because of---the growth of the health-care industry, many public health departments have stopped providing direct clinical services. Most health departments have few clinicians on staff (21) and limited influence over or engagement with the inner workings of the health-care system, except in times of large disease outbreaks, which are relatively rare. As a consequence, the gap between health care and public health has widened. Although most health-care providers still look to CDC as an authoritative source of information about health issues, and MMWR is widely respected, often the public health system and the health-care system are on independent tracks. Health-care providers, who should be public health's closest collaborators and allies, often have little interaction with and understanding of the public health system.
4. Tobacco use in the United States peaked in 1963.
Per capita cigarette consumption peaked in the United States only 2 years after you read that first CDC-published MMWR (Figure 1) (22). Although tobacco is still the leading preventable cause of morbidity and mortality in the United States, today only 19% of adults smoke (23). This amazing turnaround was achieved through innovative tobacco control and nonsmokers' rights movements that blazed a new path for public health practice, creating a model focused on promoting environmental and policy change, rather than providing individual health education services. So, while in 1961 few public health practitioners would have embraced promotion of a tax as part of their toolbox, today promoting increases in taxation of tobacco products has been effective and is an evidence-based practice. And all around the country health departments have helped pass laws to prevent exposure to secondhand smoke (don't even think about lighting up next time you get in an airplane).
Experience with tobacco control also has demonstrated that comprehensive approaches that support behavior change in a coordinated, synergistic, and reinforcing way are needed to effectively change a complex health behavior like smoking (24). Increasingly the public health workforce is developing skills related to this new paradigm. And, because most government public health agencies are constrained in how actively they can pursue legislative advocacy, collaboration with the nongovernment advocacy community has become increasingly important.
5. Tobacco has a serious new competitor for the leading preventable cause of death and disability: obesity.
While you slept, another major driver of chronic diseases snuck up on public health. Obesity has become epidemic in the United States, driving up rates of diabetes, heart disease, and many other chronic health problems (Figure 2). This epidemic has been driven by changes in the ease of making poor food choices and avoiding physical activity. Although each of these changes was small and occurred gradually, in retrospect their cumulative effect has been dramatic (25). For example, concerns about safety now result in most kids being driven rather than walking to schools. U.S. teens consume >10% of their calories from sugar-sweetened beverages (26). And the United States has become a nation addicted to large portions (you will not believe how large), quick-to-prepare, inexpensive, "fast foods."Just as tobacco control activities brought public health up against powerful corporate interests, similar battles are brewing with the food industry, and conflict between health and profit will undoubtedly continue to have a major influence on public health practice.
An extensive research base informs tobacco control. However, public health is still learning how to reverse the obesity epidemic and how best to increase physical activity and improve nutrition.
6. Everyone in the health department has a personal computer on his or her desk.
Don't pull out that slide rule you depended on in 1961 or, at best, you'll be viewed as a quaint relic of a bygone era. Powerful computers (machines that rapidly perform calculations, among many other functions) now sit on your desk or your lap and make possible almost instantaneous analysis of data. And new techniques for statistical analysis, unknown in 1961, are widely used today.
These "personal computers" (PCs) also have made possible creation of visual aids for presenting data. Color images and photographs, as well as text and tables, can now be projected onto large screens and easily manipulated and shared, even to excess. Computers also can be used to design and produce photographs and other graphics on paper. Beautiful reports and newsletters can now easily be published from anyone's desk. Curiously, all of this has not improved our presentations as much as you might predict.
Virtually all aspects of life in 2011 have been altered by computers. However, public health practice has one additional unique connection with PCs. One of the richest men in the world made his fortune from creating computer programs for these machines and then donated much of that fortune to a foundation working to improve global health (27).
Fortunately, wisdom has not gone the way of your slide rule. Much of what an ace epidemiologist in 1961 knew about data remains critical today. The adage "garbage in, garbage out" still applies, despite the newer statistical manipulations. And, although multiple pathways to statistically significant p values are now well within the reach of even the most junior analysts, just because an association is statistically significant still does not mean it is useful or even true. A 2x2 table still can take you a long way to understanding what the data are trying to tell you.
7. The speed and volume of information flow have increased exponentially since 1961.
Since 1961, an information revolution has occurred. The widespread availability of PCs and cell phones (tiny cordless telephones that work anywhere in the world) has made use of e-mail and text messaging (instant electronic communication between PCs or cell phones) and the Internet (a global, interactive storehouse of information used for almost anything you can imagine) accessible to everyone 24/7 (24 hours a day, 7 days a week, commonly used to describe our availability for doing work in 2011). Not all of that information is good; practitioners today receive lots of e-mail spam (the name of the canned meat that you ate in 1961 has been borrowed to describe unwanted e-mails). Although these tools have increased our connectivity with one another, they also have raised expectations for instant (yet accurate) responses. Practitioners today spend a great deal of time answering e-mail, taking time away from reading and face-to-face interactions, not to mention thought, rest, and vacation.
The creation of the Internet, 24-hour television news, and other communications channels have created an insatiable demand for health information, and public health practitioners are often put on the spot, expected to have that information at their fingertips on a moment's notice. Many are uncomfortable working with the media and ill equipped to play this new role. Public health's culture still values data, science, detail, and subtlety, and that culture makes uttering sound bites (short pithy sentences that play to the new time-compressed media) an unnatural act.
"Social media" tools are also used by today's public health practitioners. These venues are evolving from moment to moment like a Twitter message (don't worry, most current public health practitioners don't really know what Twitter is either) as new tools emerge. Practitioners today commonly use "Google" (an "engine" for searching for information on the Internet) and subscribe to "listservs" (computer services that send correspondence to groups automatically). Even the MMWR makes material available through "podcasts" (audio recordings that can be obtained through the Internet and loaded onto portable playback devices).
8. State and local health department employees are increasingly virtual federal staff.
Although no constitutional amendment has yet given the federal government primary responsibility for protecting the public's health, Washington, D.C., rather than state government, has become the primary source of funding for state health departments (28). Federal policymakers have become the dominant force shaping agendas and programs.
This has its advantages. Federal funding has helped drive adoption and standardization of science-based programs. For example, in contrast to 1961, all states and many local jurisdictions have at least some programming in chronic disease, primarily provided by CDC funding (29). During the past few years, this federal funding also has partially protected state and local health departments from state budget cuts resulting from the worst fiscal crisis in the United States since the MMWR began publication at CDC.
But there are downsides too. Federal funding comes most often through categorical grants (financing for predefined public health programs) (29). So even though we have not become farmers, you will hear references to "program silos" that some say inhibit leveraging of resources and creativity. Federal priorities often displace the priorities of states and localities, just because federal grant funds are available. In fact, the dominance of funding for federal priorities has made it easier for state and local elected officials, and even some health departments, to avoid doing their own priority setting. That lack of engagement at the state and local levels has weakened public health practice.
Despite a great deal of federal support, substantial gaps remain in the capacity of most health departments to address important areas of public health practice. For example, although injuries are the leading cause of death for persons aged 1-44 years (30), most state and local health departments have limited resources, if any, to address this public health concern. Despite the great increase during the last 50 years in public concern about environmental toxins, few environmental public health programs at the state and local level have been able to go very far beyond the essential services they were performing in 1961, such as restaurant inspections and oversight of drinking water systems and sewage disposal, and include substantial investigations of and research about exposure to environmental toxins in their routine work.
Because of the increasing importance of federal funding in the budgets of state and local public health agencies, federal policy choices about the scope and role of government have a large impact on state and local public health agencies. This makes it especially important for the public health system to be able to articulate what it does and demonstrate its value in ways that are compelling for federal policy makers and the public that elects them.
9. There is an Emergency Operations Center in our basement.
Since 1961, we have gotten better at handling public health emergencies. After the terrorist events of 2001, federal and state governments increased attention and funding for terrorism and emergency management. Other public health events, such as the outbreak of severe acute respiratory syndrome (SARS) in 2003; Hurricane Katrina, which flooded New Orleans in 2005; and 2009 pandemic influenza A (H1N1), helped focus attention on emergencies and how we handle them. Together these crises have led to a massive federal investment in preparedness infrastructure at state and local health departments, aiming to fix the results of many years of neglect of buildings, data systems, and the public health workforce.
The Incident Command System methodology has become the standard of practice for managing public health response in these settings (31). Health departments around the country now routinely activate an "Emergency Operations Center" or "EOC" (Figure 3) at the outset of an emergency to identify and oversee the multiple independent streams of work needed to respond competently and ensure routine and clear communications to policy makers and the public, one of the most important elements of effective response.
The incorporation of preparedness into public health practice has not been easy. The less hierarchic and more collaborative culture of public health differs substantially from the more military culture of law enforcement or emergency response, and this cultural divide has created its own set of communication and coordination challenges.
A lot of us have also worried about whether the new emphasis on preparedness activities has diverted resources and distracted attention from our most important day-to-day mission: preventing the major causes of death and disability. For example, despite the dire consequences of the obesity epidemic, much less funding has been made available for obesity prevention work than for preparing for the rare possibility of a terrorism event. On the bright side, the visibility afforded public health in emergency situations, particularly when the public health system is generally perceived to have performed well (as in the 2009 pandemic [H1N1] outbreak), might help the public and policymakers better understand the relevance of public health and build the political will to support public health system in other areas.
10. Our art is becoming science through research and evidence-based practice.
Since 1961, the evidence base for public health programs has grown, but the demand for additional evidence has only increased. Today, to an increasing extent, funders and policymakers want to see proof of our effectiveness and are holding us accountable for the performance of our programs. Groups such as the Cochrane Collaboration (32) and the U.S. Task Force on Community Preventive Services (33) have helped apply and enhance the rigor of this technique for public health practice and services.
When you fell asleep, public health nursing and home visiting had long been important tools in public health practice, especially at the local level. While you slept, rigorous evaluation has demonstrated substantial impacts of home visiting by nurses, including improved prenatal health, fewer childhood injuries, fewer subsequent unplanned pregnancies, increased intervals between births, increased maternal employment and improved school readiness (34). Expansion of these programs is likely to continue to be an important part of local public health practice in the future.
That is just one of many areas in which rigorous research and evaluation have confirmed and refined what state and local public health practitioners do. The refinement and widespread use of meta-analysis has allowed us to pool the results of many small studies and increased the robustness and validity of research findings in many areas. In truth, these efforts also have highlighted the dearth of rigorous evaluation of much of what we do in public health and the standards for acceptable evidence of effective community-based practices are evolving. Increasingly we see the need for practice-based evidence as well as evidence-based practice (35) to continue to hone our work. But better science has raised expectations that our work is evidence based and demonstrably effective. In most settings today, personal credibility alone will not drive public health action unless it is coupled with the accumulated and synthesized scientific information available.
The Future
"I am your father!" cried he---"Young Rip van Winkle once---old Rip Van Winkle now!---
Does nobody know poor Rip Van Winkle!"
---Washington Irving, Rip Van Winkle (1)
This retrospective look begs for a brief prospective glance into the future. What if the events leading to the long sleep of our hapless, hypothetical 1961 public health practitioner repeated themselves and he nodded off again, only to awaken in 2061?
Prediction is a risky business. Nevertheless, we'll go out on a limb and venture to predict that many of the trends described above will have continued. More old infectious diseases will be gone or much reduced because we are likely to have highly effective vaccines for malaria, tuberculosis, HIV, and influenza. More new diseases will be identified. The rest of the world probably will have caught up with the developed world in terms of the epidemiologic transition from infectious to chronic disease. Undoubtedly spectacular new information technologies will dramatically transform our lives. And when we are really feeling optimistic we can even predict with some confidence that the obesity epidemic, so long in the making, will be well on its way to being defeated.
On the other hand, in at least three critically important areas of public health practice 50 years from now, the outcomes seem too close to call; the factor that determines whether we are "alone and forgotten"---like Rip Van Winkle---may be us.
1. The need to contain health-care costs could profoundly improve the linkage between health care and public health. Or not.
It is frequently said these days that the rate of increase in the costs of providing health care in the United States is unsustainable. There is less agreement on the solution. Although health-care system improvements will be important, investments in public health systems that support community-based programs to address the determinants of health, improve access to quality health care, and emphasize the delivery of preventive services by the health-care system and at the community level also are needed. Without those investments to address the drivers of the need for health care, the United States will not have a sustainable business model for its health-care system.
The current funding crisis and the potential for investments in public health provide an opportunity for public health to sharpen its focus on the core functions of assessment, policy development, and assurance (36) and for the public health and health-care systems to articulate more clearly their complementary roles and link together more closely, closing the chasm between health care and public health and creating one system that truly helps "assure the conditions in which people can be healthy" (36). Electronic clinical data systems, if designed with both clinical and state and local public health needs in mind, will support this linkage.
But even though opportunity exists, the outcome in this area is not assured. To reach this goal will require vision, leadership, and a new spirit of collaboration between public health practitioners and clinicians.
2. The structure of our antiquated public health system will have changed, either because of us or despite us.
It has been said that "if you've seen one health department, you've seen one health department" (37) to illustrate the wide variation in agency structure, services, budget, and political accountability across the country. Some variation allows us to meet different needs and take advantage of different opportunities across the country. However, in a world that is increasingly interconnected, with instantaneous national and international communication and concerns, the current profound differences in funding and capacity among state and local health departments are likely to be more and more counterproductive.
The huge differences among health departments are inefficient and obstruct efforts to achieve economies of scale, transparency, and reliable system governance. In a time when the public demands evidence of performance and accountability from state and local health departments, these differences make it much harder to explain to the public why we do what we do---which in turn makes advocating for resources and political support much more difficult. New performance standards (38) and accreditation processes (39) might help bring data on state and local health department performance and capacity to the surface in a standardized way that will facilitate communication and meaningful interpretation, but as in other areas of public health practice, data are only one input into public health action, and the data generated by these tools alone will not power structural changes. They are necessary but not sufficient.
We are pretty certain that 50 years from now the structure of the U.S. public health system will have changed profoundly. The public's health will benefit the most if we embrace the need for change and lead this process rather than dig in our heels about the status quo and allow it to be imposed on public health from the outside.
3. Depending on how well we have addressed the current leading causes of preventable death and disability, government public health agencies will either be empowered or marginalized.
Much of the increase in average life span we have enjoyed over the past 100 years has resulted from such public health programs as immunization, improved sanitation, and public health services for young mothers (40). But times are changing, and what we do every day in state and local health departments has been slow to catch up. As rates of death and disease from infections, as well as rates of infant and maternal mortality, fell and rates of death from chronic disease rose, our structure and programs did not evolve well in response to this epidemiologic transition (41). Paradoxically our remarkable historical victories place us at increasing risk for becoming victims of our own success because we are viewed as focusing too much attention and resources on causes of morbidity and mortality that were dominant in past decades.
To remain relevant over the next 50 years, we will have to better balance protecting our successes with attacking our challenges. Preventing injury, reducing disability associated with aging, mitigating the effects of global warming, and preventing mental health and substance abuse problems are just a few emerging areas in which public health could make a big difference but currently is not doing enough. Also, the increasing diversity of the U.S. population and the recognition of the profound influence of social determinants of health on health outcomes demand that public health practice at all levels develop and implement coherent and effective strategies to tackle these foundational drivers of health. To meet the demands in these areas at state and local health departments, staff across the system will need to have not only subject-area expertise but also strong skills in changing systems, environments, and policy; using media; building coalitions; and convening and leading a broad array of partners well beyond those of today's public health mainstream.
In summary, the crystal ball is cloudy and public health practice in 2061 is likely to look at least as different from today's practice as today's practice looks from that of 1961. The most profound changes are likely to be the ones that are unimaginable today. Amidst all this uncertainty, perhaps the safest prediction to make is that MMWR will be there to tell us about it.
References
- Irving W. Rip Van Winkle and other stories. New York, NY. Puffin; 1996:1--29.
- Diekma DS, Committee on Bioethics. Responding to parental refusals of immunization of children. Pediatrics 2005;115:1428--431.Reaffirmed May 2009.
- Division of Healthcare Quality Promotion, CDC. Antibiotic/antimicrobial resistance [updated 2010 July 19. Available at http://www.cdc.gov/drugresistance/index.html.
- CDC. Follow-up on respiratory illness---Philadelphia. MMWR 1997;46:50--6.
- CDC. Toxic-shock syndrome---United States. MMWR 1980;29:229--30.
- CDC. Outbreak of acute illness---southwestern United States. MMWR 1993;421--4.
- CDC. Lyme disease---United States, 1980. MMWR 1981;30:489--92,497.
- MacKenzie WR, Hoxie NJ, Proctor ME, et al. A massive outbreak in Milwaukee of Cryptosporidium infection transmitted through the public water supply. N Engl J Med 1994;331:161--7.
- CDC. Surveillance for foodborne disease outbreaks---United States, 2007. MMWR 2010;59:973--9.
- CDC. Preliminary report: foodborne outbreak of Escherichia coli O157:H7 infections from hamburgers---western United States, 1993. MMWR 1993;42:85--6.
- CDC. PulseNet [updated 2009 April 28].Available at http://www.cdc.gov/pulsenet.
- CDC. Pneumocystis pneumonia---Los Angeles. MMWR 1981;30:250--2.
- Joint United Nations Program on HIV/AIDS (UNAIDS). 2008 report on the global AIDS epidemic. Geneva, Switzerland: World Health Organization; 2008. Available at http://www.unaids.org/en/KnowledgeCentre/HIVData/GlobalReport/2008/2008_Global_report.asp.
- National Institute on Drug Abuse International Program. Methadone research Web guide. Available at http://www.international.drugabuse.gov/collaboration/guide_methadone/parta_question2.html.
- Hogben M, McNally T, McPheeters M, Hutchinson AB, Task Force on Community Preventive Services. The effectiveness of HIV partner counseling and referral services in increasing identification of HIV-positive individuals; a systematic review. Am J Prev Med 2007;33:S89--100.
- Mahajan AP, Sayles JN, Patel VA, et al. Stigma in the HIV/AIDS epidemic: a review of the literature and recommendations for the way forward. AIDS.2008;22(Suppl 2):S67--79.
- CDC. Syringe exchange programs---United States 2005. MMWR 2007;56:1164--7.
- CDC. Guidelines for national human immunodeficiency virus case surveillance, including monitoring for human immunodeficiency virus infection and acquired immunodeficiency syndrome. MMWR 1999;48(No. RR-13).
- Sisko AM, Truffler CJ, Keehan SP, Poisal JA, Clemens MK, Madison AJ. National health spending projections: the estimated impact of reform through 2019.Health Aff 2010:29;1933--41.
- Levit KR, Lazenby HC, Sivarajan L. Health care spending in 1994: slowest in decades. Health Aff 1996;15:130--44.
- Reichart A, Lewis M.2007 State public health workforce survey results. Washington, DC. Association of State and Territorial Health Officials. Available at http://www.astho.org/Display/AssetDisplay.aspx?id=500.
- CDC. Smoking and tobacco use: consumption data. Available at http://www.cdc.gov/tobacco/data_statistics/tables/economics/consumption.
- CDC. Vital Signs: current cigarette smoking among adults aged ≥18 years---United States, 2005--2010. MMWR 2011;60:1207--12.
- CDC. Best practices for comprehensive tobacco control programs---2007. Atlanta, GA: US Department of Health and Human Services, CDC, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 2007.
- Levi J, Vinter S, St. Lauren R, Segal LM.F as in fat: how obesity threatens America's future. Washington, DC: Trust for America's Health; 2010.Available at http://healthyamericans.org/reports/obesity2010/Obesity2010Report.pdf.
- Jacobson MF. Liquid candy: how soft drinks are harming America's health. Washington, DC: Center for Science in the Public Interest. Available at http://www.cspinet.org/new/pdf/liquid_candy_final_w_new_supplement.pdf.
- Bill and Melinda Gates Foundation. Global Health Program. Available at http://www.gatesfoundation.org/global-health/Pages/overview.aspx.
- Association of State and Territorial Health Officials. Profile of state public health, volume 1.Washington, DC. Association of State and Territorial Health Officials; 2007: 46.Available at http://www.astho.org/Display/AssetDisplay.aspx?id=2882.
- CDC. Grant funding profiles [updated 2010 September 15]. Available at http://www.cdc.gov/fundingprofiles/.
- CDC. 10 leading causes of death by age group, United States---2007.Available at http://www.cdc.gov/injury/wisqars/pdf/Death_by_Age_2007-a.pdf.
- CDC. Emergency Operations Center (EOC) [updated 2010 July 19].Available at http://emergency.cdc.gov/cdcpreparedness/eoc.
- The Cochrane Collaboration. Available at http://www.cochrane.org.
- The Task Force on Community Preventive Services [updated July 26, 2010].Available at http://www.thecommunityguide.org/about/task-force-members.html.
- American Academy of Pediatrics, Council on Child and Adolescent Health. The Role of Home-Visitation Programs in Improving Health Outcomes for Children and Families. Pediatrics. 1998;3:486-9.
- Green LW, Glasgow RE. Evaluation the relevance, generalization, and applicability of research: issues in external validation and translation methodology. Eval Health Prof 2006;29:126--53.
- Committee for the Study of the Future of Public Health, Institute of Medicine. The future of public health. Washington, DC: National Academy Press; 1988:7--8.
- Menkens AJ, Stone D, Wood BW. Local public health department accreditation: thoughts from North Carolina. J Public Health Manag Pract 2009;15:443--5.
- Division of Public Health Performance Improvement (DPHPI) [updated 2009 July 31].Available at http://www.cdc.gov/ostlts/about/DPHPI.html.
- Public Health Accreditation Board. Available at http://www.phaboard.org.
- CDC. Ten great public health achievements---United States, 1900--1999.MMWR 1999;48:241--3.
- Frieden TR. Asleep at the switch; local public health and chronic disease. Am J Public Health 2004;94:2059--61.
FIGURE 1. Chesterfield cigarette advertisement on back of 1953 Metropolitan Opera program, featuring Arthur Godfrey, popular entertainer and smoker who later died of lung cancer.

Photo: CDC
Alternate Text: The figure is a replication of an advertisement for Chesterfield cigarettes on the back of a Metropolitan Opera Program in 1953
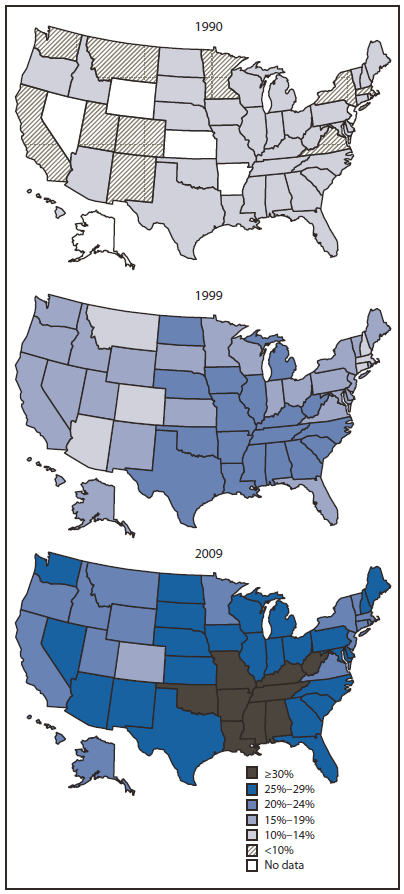
Abbreviation: BRFSS=Behavioral Risk Factor Surveillance System.
Source: http://www.cdc.gov/obesity/data/trends.html.
* Body mass index ≥30, or about 30 lbs. overweight for a 5'4" person.
Alternate Text: The figure is three U.S. maps presenting obesity trends among U.S. adults in 1990, 1999, and 2009.

Photo: CDC
Alternate Text: The figure is a photo of workers at the Oregon Public Health Agency Operations Center during the 2009 H1N1 influenza pandemic.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


