Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Trends in Smoking Before, During, and After Pregnancy — Pregnancy Risk Assessment Monitoring System, United States, 40 Sites, 2000–2010
Van T. Tong, MPH1
Patricia M. Dietz, DrPH1
Brian Morrow, MA1
Denise V. D'Angelo, MPH1
Sherry L. Farr, PhD1
Karilynn M. Rockhill1
Lucinda J. England, MD2
1Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, CDC
2Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC
Corresponding author: Van Tong, MPH, Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. Telephone: 770-488-6309; E-mail: vtong@cdc.gov.
Abstract
Problem: Smoking during pregnancy increases the risk for complications such as fetal growth restriction, preterm delivery, and infant death. In 2002, 5%–8% of preterm deliveries, 13%–19% of term infants with growth restriction, 5%–7% of preterm-related deaths, and 23%–34% of deaths from sudden infant death syndrome were attributable to prenatal smoking in the United States.
Reporting Period Covered: 2000–2010.
Description of System: The Pregnancy Risk Assessment Monitoring System (PRAMS) was initiated in 1987 and is an ongoing state- and population-based surveillance system designed to monitor selected maternal behaviors and experiences that occur before, during, and after pregnancy among females who deliver live-born infants in the United States. Self-reported questionnaire data are linked to selected birth certificate data and are weighted to represent all women delivering live infants in the state. Self-reported smoking data were obtained from the PRAMS questionnaire and birth certificates. This report provides data on trends (aggregated and site-specific estimates) in smoking before, during, and after pregnancy from 40 PRAMS sites during 2000–2010.
Results: For the majority of sites, smoking prevalence before, during, or after pregnancy did not change over time. During 2000–2010, smoking prevalence decreased in three sites (Minnesota, New York state, and Utah) for all three measures and in eight sites (Colorado, Illinois, New Jersey, New Mexico, New York City, Washington, Wisconsin and Wyoming) for one or two of the measures. Smoking prevalence increased for all three measures in three sites (Louisiana, Mississippi, and West Virginia); an increase in prevalence before pregnancy (only) occurred in Oklahoma, and an increase during and after pregnancy occurred in Maine. For a subgroup of 10 sites for which data were available for the entire 11-year study period (Alaska, Arkansas, Colorado, Hawaii, Maine, Nebraska, Oklahoma, Utah, Washington, and West Virginia), the prevalence of smoking before pregnancy remained unchanged, with approximately one in five women reporting smoking before pregnancy (23.6% in 2000 to 24.7% in 2010). The prevalence of smoking during pregnancy decreased (p = 0.04; linear trend assessed with logistic regression) from 13.3% in 2000 to 12.3% in 2010, and the prevalence of smoking after delivery decreased (p<0.01) from 18.6% in 2000 to 17.2% in 2010.
Interpretation: The results indicate that efforts to reduce smoking prevalence among female smokers before pregnancy have not been effective; however, tobacco-control efforts have been minimally effective in reducing smoking prevalence during and after pregnancy. Current tobacco-control efforts in most sites might be insufficient to reach national objectives related to reducing prevalence of smoking during pregnancy.
Public Health Action: States with no change in or increasing smoking prevalence before, during, and after pregnancy can help reduce prevalence through sustained and comprehensive tobacco-control efforts (e.g., mass media campaigns, coverage of tobacco cessation, 100% smoke-free policies, and tobacco excise taxes).
Introduction
Prenatal smoking remains one of the most common preventable causes of infant morbidity and mortality. Cigarette smoking can reduce fertility and delay conception among females (1), and smoking near conception is associated with cleft lip and cleft palate (2). Maternal cigarette smoking during pregnancy increases the risk for pregnancy complications (e.g., placenta previa, placental abruption, and premature rupture of the membrane) and poor infant outcomes (e.g., preterm delivery, restricted fetal growth, sudden infant death syndrome [SIDS], and preterm-related death) (1). Exposure to secondhand smoke after delivery increases an infant's risk for respiratory tract infections, ear infections, and SIDS (3). In 2002, 5%–8% of preterm deliveries, 13%–19% of term infants with growth restriction, 5%–7% of preterm-related deaths, and 23%–34% of SIDS deaths were attributable to prenatal smoking in the United States (4). In 2004, approximately $122 million in health-care costs for infant hospitalizations after delivery were attributable to prenatal smoking (5).
Three Healthy People 2020 national health objectives address smoking before and during pregnancy: 1) reduce the prevalence of smoking before pregnancy to 14% (objective MICH-16.3), 2) reduce the prevalence of cigarette smoking among pregnant women to 1.4% (objective MICH-11.3), and 3) increase the percentage of pregnant smokers who stop smoking during pregnancy to 30% (objective TU-6) (6).
To assess progress toward achieving the Healthy People 2020 objectives and to assist tobacco-control efforts that focus on females before, during, and after pregnancy, CDC analyzed data from the Pregnancy Risk Assessment Monitoring System (PRAMS) questionnaire for 2000–2010. A previous PRAMS report showed that the prevalence of smoking before pregnancy remained unchanged from 2000 to 2005, and smoking during and after pregnancy decreased slightly (7). This report updates PRAMS data on trends (aggregated and site-specific estimates) in smoking before, during, and after pregnancy and describes characteristics of smokers.
Methods
PRAMS is an ongoing state- and population-based surveillance system designed to monitor selected self-reported behaviors, health-care use, and maternal morbidities that occur before, during, and after pregnancy among women who deliver a live-born infant in the United States. PRAMS is administered by CDC in collaboration with state health departments. PRAMS began in 1987 with six sites (District of Columbia, Indiana, Maine, Michigan, Oklahoma, and West Virginia) and in 2013 includes 40 states (Alabama, Alaska, Arkansas, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Illinois, Iowa, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Nebraska, New Hampshire, New Jersey, New Mexico, New York, North Carolina, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, Tennessee, Texas, Utah, Vermont, Virginia, Washington, West Virginia, Wisconsin, and Wyoming), and New York City. Because New York state and New York City have separate vital records registries and collect data as independent projects, data for these two PRAMS sites are reported separately. The data from the 27 PRAMS sites with available data in 2010 represent approximately 52% of U.S. live births.
Data Collection
All health departments participating in PRAMS use a standardized data collection methodology developed by CDC. At each site, a stratified sample of 100–300 new mothers is selected systematically from birth certificates. Up to three self-administered questionnaires are mailed to selected mothers starting 2–3 months after the delivery of a live infant. If no mail response is received after approximately 60 days, nonresponders are contacted by telephone up to 15 times to complete the survey. All efforts to contact respondents by mail and telephone end 9 months postpartum. Survey data are linked to selected birth certificate data and weighted for sample design, nonresponse, and noncoverage. The PRAMS questionnaire is revised periodically, and data highlighted in this report were collected using the Phase Four (2000–2003), Phase Five (2004–2008), and Phase Six (2009–2011) versions of the questionnaire (8). Details concerning the PRAMS methodology have been described elsewhere (9).
To minimize nonresponse bias, PRAMS sites were included in the report if the overall weighted response rate for a given site and year was ≥70% for data collected during 2000–2006 and ≥65% for data collected starting in 2007. For the 2000–2010 study period, the following 40 PRAMS sites are included for ≥1 years to calculate aggregated total sites and site-specific smoking prevalence by year and to conduct aggregated and site-specific trend analysis (of those sites with at least three consecutive or nonconsecutive years of data): Alabama, Alaska, Arkansas, Colorado, Delaware, Florida, Georgia, Hawaii, Illinois, Louisiana, Maine, Maryland, Massachusetts, Michigan, Minnesota, Mississippi, Missouri, Montana, Nebraska, New Jersey, New Mexico, New York, New York City, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, South Dakota Tribal, Tennessee, Texas, Utah, Vermont, Washington, West Virginia, Wisconsin, and Wyoming. Data from 27 PRAMS sites with data available in 2010 were aggregated for the analysis of maternal characteristics by smoking measures: Alaska, Arkansas, Colorado, Delaware, Georgia, Hawaii, Maine, Maryland, Massachusetts, Michigan, Minnesota, Missouri, Nebraska, New Jersey, New York, New York City, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, Texas, Utah, Vermont, Washington, West Virginia, and Wyoming. Data from 10 PRAMS sites with data available for all 11 years during 2000–2010 were aggregated to analyze trends: Alaska, Arkansas, Colorado, Hawaii, Maine, Nebraska, Oklahoma, Utah, Washington, and West Virginia.
Variables Analyzed
This report presents data on measures of smoking behaviors before, during, and after pregnancy: 1) smoking during the 3 months before pregnancy, 2) smoking during the last 3 months of pregnancy, 3) quitting smoking by the last trimester of pregnancy among women who smoked during the 3 months before pregnancy, and 4) smoking after delivery (assessed at the time of questionnaire completion).
Smoking measures were analyzed in the aggregate for the 27 sites with available data for 2010 by selected maternal characteristics. Data on maternal age, race/ethnicity, and education were obtained from birth certificates; health-care insurance coverage data before pregnancy and during prenatal care or at delivery were obtained from PRAMS. Prevalence and 95% confidence intervals (CIs) were presented by year for each site. Variable definitions have been described in detail previously (7).
Statistical Analysis and Weighting
Statistical linear trends were assessed for the total sites aggregated per year, 10 PRAMS sites with data available for all 11 years of the study period, and PRAMS sites with at least 3 years (consecutive or nonconsecutive) of available data. Statistical linear trends were assessed using logistic regression with smoking as the outcome variable and the infant's birth year as the independent variable; other variables were included in the model with justification as follows. In a subanalysis, the Phase 6 filter question ("Have you smoked any cigarettes in the past 2 years?") had a significant effect on the prevalence estimates of smoking before pregnancy because a higher proportion of women who smoked <1 and 1–5 cigarettes per day responded "Yes" compared with when the Phase 5 filter question ("Have you smoked at least 100 cigarettes in the past 2 years?") was being used; however, the change in the filter question had no significant effect on the prevalence estimates of smoking during pregnancy or smoking after delivery (CDC, unpublished data, 2012). A categorical variable to control for the Phase 6 filter change was added to the logistic regression model to assess changes over time for two of the smoking measures (smoking during the 3 months before pregnancy and quitting smoking during pregnancy). For total sites aggregated per year, a categorical variable was also added to the logistic regression model to control for site-specific differences in prevalence.
To estimate the magnitude of change in the prevalence estimates among those sites with a statistically significant linear trend, the annual percentage point change was estimated from the beta coefficient of the infant's birth year with a standard intercept across all sites. Differences in smoking prevalence by maternal characteristics were assessed using the chi-square test for independence. Significance level for all statistical tests was set at p≤0.05.
Data were weighted to represent all women who delivered live births in each respective site in the given year. Unweighted numbers are provided to indicate respondents by smoking status. The data for the South Dakota Tribal project were weighted to represent women who delivered an American Indian infant in South Dakota and Sioux County, North Dakota, and are not representative of all live births in the state of South Dakota (10). Analyses were conducted using statistical software to account for the complex survey design (11,12).
Results
A total of 40 PRAMS sites had ≥1 years of data available during 2000–2010, with a total unweighted sample size of 444,614 females. The yearly site-specific sample size ranged from 585 respondents (New York City, 2007) to 2,518 respondents (Hawaii, 2000). The highest 1-year response rate (89%) was in Utah in 2004. The median 1-year response rate in 2010 was 68.2%. On the basis of aggregated data from 27 sites in 2010, the average age of infants for whom the PRAMS questionnaire was completed was 116.9 days (range: 93.8 days [Montana, 2002] to 146.7 days [Florida, 2005]).
Smoking During the 3 Months Before Pregnancy
On the basis of aggregated data from 40 PRAMS sites, the prevalence of smoking during the 3 months before pregnancy did not change significantly during 2000–2010 (Table 1). This was also the case for the subgroup of 10 sites for which data were available for all 11 years during 2000–2010 (Figure 1). Site-specific trends during the study period for the prevalence of smoking during the 3 months before pregnancy increased significantly for four sites: Louisiana (from 21.2% to 28.2%), Mississippi (from 21.9% to 29.8%), Oklahoma (from 30.2% to 33.6%), and West Virginia (from 36.2% to 46.2%) and decreased significantly for five sites: Minnesota (from 27.7% to 26.0%), New Mexico (from 21.3% to 18.8%), New York (from 27.1% to 24.8%), Utah (from 14.3% to 11.8%), and Wisconsin (from 30.0% to 26.5%). In 2010, among 27 sites with data available, site-specific prevalences of smoking during the 3 months before pregnancy ranged from 9.2% in New York City to 46.2% in West Virginia.
Of the 27 PRAMS sites with data available in 2010, only New York City and Utah have achieved the Healthy People 2020 goal of reducing prevalence of smoking during the 3 months before pregnancy to 14% in 2010 (Table 1). In 2010, on the basis of aggregated data from 27 sites, 23.2% of women reported smoking during the 3 months before pregnancy (Table 2). Demographic groups with the highest prevalence of smoking before pregnancy were women aged 20–24 years (34.7%), were American Indian/Alaska Native (55.1%), had 12 years of education (32.6%), and had Medicaid coverage before pregnancy (34.4%).
Smoking During Pregnancy
On the basis of aggregated data from 40 PRAMS sites with at least 1 year of data during 2000–2010, the prevalence of smoking during pregnancy significantly decreased over time (Table 3). For the aggregated data from the subgroup of 10 sites, smoking during pregnancy also decreased significantly from 13.3% in 2000 to 12.3% in 2010 (an estimated 0.1 percentage point decrease each year) (Figure 1; Table 3). During the study period, smoking during pregnancy increased significantly for four sites (Louisiana [from 11.9% to 17.7%], Maine [from 17.5% to 18.2%], Mississippi [from 13.5% to 16.6%], and West Virginia [from 24.5% to 30.5%]) and decreased significantly for seven sites (Colorado [from 10.2% to 8.1%], Illinois [from 12.5% to 9.2%], Minnesota [from 15.4% to 13.7%], New Jersey [from 9.0% to 6.6%], New York [from 17.0% to 11.4%], New York City [from 7.6% to 2.3%], and Utah [from 7.3% to 4.5%]) (Table 3). The largest annual percentage point decrease occurred in New York City (decrease of 1.5 percentage points). The site-specific prevalences of smoking during pregnancy among the 27 sites in 2010 ranged from 2.3% in New York City to 30.5% in West Virginia (Figure 2; Table 3). None of the 27 PRAMS sites with data available in 2010 have achieved the Healthy People 2020 goal of reducing prenatal smoking prevalence to 1.4%.
In 2010, on the basis of aggregated data from 27 sites (PRAMS only), 10.7% of women reported smoking during the last 3 months of pregnancy from (Table 3). Demographic groups with the highest prevalence of women who smoked during pregnancy were aged 20–24 years (17.6%), were American Indians/Alaska Natives (26.0%), had <12 years of education (17.4%), and had Medicaid coverage during pregnancy or at delivery (17.6%) (Table 2).
Quitting Smoking During Pregnancy
On the basis of aggregated data from 40 PRAMS sites with at least 1 year of data during 2000–2010, the percentage of women who smoked but quit by the last trimester increased significantly (Table 4). The percentage of smokers who quit smoking during pregnancy decreased significantly for one site (Louisiana [from 44.2% to 37.1%]) and increased significantly for four sites (Illinois [from 40.3% to 56.5%], Massachusetts [from 42.8% to 62.0%], Michigan [from 33.1% to 48.7%], and New Jersey [from 47.9% to 63.6%]). The site-specific percentages of women who quit smoking during pregnancy among the 27 sites in 2010 ranged from 34.3% in West Virginia to 74.6% in New York City. All 27 PRAMS sites with data available in 2010 have achieved the Healthy People 2020 goals of increasing smoking cessation during pregnancy to 30%.
In 2010, on the basis of aggregated data from 27 sites, 54.3% of women reported quitting smoking by the last 3 months of pregnancy (Table 2). Demographic groups with the highest percentage of quitting smoking during pregnancy were women who were aged <20 years (59.3%), were Asian/Pacific Islander (72.0%), had >12 years of education (65.7%), and had private insurance coverage during pregnancy or at delivery (68.2%) (Table 2).
Smoking After Delivery
On the basis of aggregated data from 40 PRAMS sites with at least 1 year of data during 2000–2010, the prevalence of smoking after delivery decreased significantly, and this was the case in the subgroup of 10 states with data available for all 11 years during the study period from 18.6% in 2000 to 17.2% in 2010 (a decrease of 0.2 percentage points per year) (Figure 1; Table 5). The prevalence of smoking after delivery increased significantly for four sites (Louisiana [from 18.7% to 23.4%], Maine [from 23.8% to 24.8%], Mississippi [from 20.0% to 21.3%], and West Virginia [from 31.6% to 37.5%]) and decreased significantly for 11 sites (Colorado [from 15.0% to 12.8%], Illinois [from 16.6% to 14.6%], Minnesota [from 19.9% to 18.1%], New Jersey [from 13.1% to 10.5%], New Mexico [from 16.0% to 13.1%], New York [from 22.4% to 17.4%], New York City [from 11.7% to 4.1%], Utah [from 9.5% to 7.2%], Washington [from 16.0% to 12.7%], Wisconsin [from 21.9% to 16.1%], and Wyoming [from 24.5% to 18.8%]). In 2010, the site-specific prevalences of smoking after delivery among the 27 states ranged from 4.1% in New York City to 37.5% in West Virginia.
In 2010, on the basis of aggregated data from 27 sites, 15.9% of women reported smoking approximately 4 months after delivery (Table 2). Demographic groups with the highest prevalence of smoking after delivery were women who were aged 20–24 years (25.5%), were American Indian/Alaska Native (40.1%), had 12 years of education (24.5%), and had Medicaid coverage during pregnancy or delivery (24.3%).
Discussion
During 2000–2010, moderate but significant decreases occurred in the prevalence of women smoking while pregnant (from 13.3% to 12.3%) and after delivery (from 18.6% to 17.2%) in a subgroup of 10 PRAMS sites. Several sites had significant reductions in smoking prevalence around the time of pregnancy. During 2000–2010, in three sites (Minnesota, New York State, and Utah), prevalence decreased for smoking before, during, and after pregnancy, and in eight sites (Colorado, Illinois, New Jersey, New Mexico, New York City, Washington, Wisconsin, and Wyoming), prevalence decreased for one or two of the measures (before, during, or after pregnancy). However, none of the PRAMS sites in 2010 reached the Healthy People 2020 goal of reducing prenatal smoking prevalence to 1.4%. If trends in smoking prevalence during pregnancy continue at the current pace (an estimated 0.1 percentage point decrease per year), then it could take another 100 years for the United States to reach this goal.
Furthermore, smoking prevalence before pregnancy remained unchanged from 2000 to 2010, with only two sites (New York City and Utah) reaching the Healthy People 2020 goal of reducing smoking prevalence before pregnancy to 14%. Smoking prevalence for the majority of PRAMS sites did not change over time in any of the measures (before, during, or after pregnancy). Three sites (Louisiana, Mississippi, and West Virginia) had an increase in prevalence in all three measures during the study period; Oklahoma had an increase in prevalence before pregnancy only, and Maine had increases in prevalence during and after pregnancy.
Implementing proven comprehensive tobacco-control strategies, including awareness campaigns, price increases, and 100% smoke-free policies, are needed to reach national goals of reducing smoking among pregnant women. PRAMS data from 29 states during 2000–2005 suggest that state tobacco-control policies reduced maternal smoking (13). For example, in one study, a $1.00 increase in cigarette taxes and prices increased quitting rates among pregnant women from 44.1% to 48.9% and decreased the percentage who relapsed in the early postpartum period. The study also found that implementing a full worksite smoking ban increased quitting rates by an estimated 5 percentage points. Additionally, higher cigarette prices reduced smoking and increased the probability of a full-term birth, with the largest improvements among low-income women (14). In the current analysis, among the five PRAMS states with any increases in smoking prevalence before, during, or after pregnancy, Louisiana, Mississippi, and West Virginia had cigarette excise taxes that were <$1.00 per pack (range: $0.36 per pack in Louisiana to $0.68 per pack in Mississippi), and Mississippi, Oklahoma, and West Virginia had no state smoke-free policy (15). In contrast, among the 11 PRAMS sites that experienced reductions in smoking prevalence, 10 sites had a state smoke-free policy, and nine sites had excise taxes >$1.00 per pack (range: $1.23 per pack in Minnesota to $4.35 per pack in the state of New York). The results in this report suggest that strong state tobacco-control policies can help significantly reduce smoking prevalence around the time of pregnancy.
Although tobacco-control policies are likely to have the most public health impact in reducing smoking prevalence (16), continued efforts are needed to develop more effective clinical interventions and to deliver these interventions to female smokers who need help quitting. The current best practice for prenatal smoking cessation entails psychosocial counseling delivered in the prenatal care setting (17). Counseling such as this has been shown to have a modest effect, with approximately 1 out of 20 women quitting (18). Because the safety and efficacy of nicotine replacement therapy during pregnancy has not been established, the therapy is recommended by the American College of Obstetricians and Gynecologists only if behavioral approaches fail (19). Studies of contingency management interventions, in which quitting is reinforced with financial incentives, show promise, with a quit rate of up to 34% in the intervention group (compared with 7.1% in the standard-of-care group) and improvements in infant birth weight (20). However, more research is needed to assess the effectiveness of contingency management for diverse populations and settings and to determine the cost-benefit of these interventions.
Reducing client out-of-pocket costs for cessation treatments has been shown to be effective in increasing cessation (17). For pregnant Medicaid beneficiaries, the Affordable Care Act requires states to provide tobacco-cessation counseling and medication without cost sharing (21). As of 2012, a total of 51 state Medicaid programs cover pharmacotherapy and 38 states cover counseling services for pregnant women (22). This is particularly important as, in the results of this report, Medicaid-enrolled women had the highest smoking prevalence before, during, and after pregnancy compared with women of other coverage groups. Starting in 2014, the Affordable Care Act mandates coverage without cost sharing for tobacco-use screening and cessation interventions for beneficiaries in the Medicaid expansion population for those states that choose to expand, and the law mandates that beginning in 2014, states are precluded from excluding tobacco-cessation drugs from coverage for traditional Medicaid enrollees (23). Thus, as cessation services expand for Medicaid enrollees, health-care providers and patients should be aware of this coverage.
Pregnancy can be an opportune time to encourage women to quit smoking. Pregnant smokers who are willing to quit should be offered effective smoking cessation interventions or referred to cessation services. Compared with those who continue to smoke during pregnancy, women who quit smoking during pregnancy were more likely to be abstinent up to 21 years after pregnancy (24). In the general U.S. adult population, quitting smoking before the age of 40 years reduced the risk for death associated with continued smoking by approximately 90%, resulting in approximately 1 decade of life gained (25). Because most women who give birth to children are young (mean age: 25 years), quitting smoking during pregnancy could have substantial long-term benefits for the mother.
Limitations
The findings in this report are subject to at least two limitations. First, pregnant women might underreport smoking and overreport quitting smoking. A validation study comparing self-reports with serum cotinine of a national sample found that 23% of pregnant smokers and 10% of nonpregnant smokers did not disclose their smoking (26). Because the PRAMS self-report is not biochemically validated, the data provided in this report likely underestimate the prevalence of smoking among pregnant women. Second, PRAMS only samples women who have delivered a live infant and cannot estimate the total prevalence of smoking among all pregnant women, specifically those who experience spontaneous abortions, ectopic pregnancies, or stillbirths. The report findings are generalizable only to the PRAMS sites included in the analyses.
Conclusion
PRAMS is an effective state-level tool to monitor and evaluate the impact of tobacco-control activities on smoking before, during, and after pregnancy. From 2000 to 2010, modest decreases in smoking prevalence occurred during pregnancy and after delivery, but no change occurred in smoking prevalence during the 3 months before pregnancy. Most sites had no change in smoking prevalence over time. Of the 27 PRAMS sites with data available in 2010, only two sites have met the Healthy People 2020 goal of reducing prevalence of preconception smoking to 14%, and no sites met the goal of reducing prenatal smoking prevalence to 1.4%. All 27 sites have met the goal of increasing smoking cessation during pregnancy to 30%.
Smoking during pregnancy is the most common cause of infant morbidity and mortality for which effective cessation interventions exist. Population-based tobacco-control measures can reduce adverse perinatal outcomes, such as preterm deliveries, small-for-gestational-age infants, and SIDS deaths (14,27–29). States can consider adopting sustained and comprehensive tobacco-controlled activities to prevent smoking initiation and reduce smoking during pregnancy. These activities include promoting policies that establish smoke-free environments in public places and workplaces, increasing tobacco excise taxes, banning all forms of tobacco advertisement, enforcing laws to prohibit tobacco sales to children and adolescents, using mass media campaigns, using state tobacco quit lines, and ensuring adequate health-care coverage for cessation services (30). Clinicians and pregnant women should be made aware of Medicaid coverage or other health insurance coverage for smoking cessation services.
Primary and prenatal health-care providers can assess the smoking status of their patients, offer smoking cessation interventions, or refer patients to effective cessation services (e.g., state telephone-based quit lines, such as 1-800-QUIT-NOW). Online training on best-practice approaches for helping pregnant women quit smoking is available for health-care professionals (31). Maternal and child health-care and state tobacco-control professionals can work together to achieve the Healthy People 2020 objectives of reducing smoking among pregnant women.
Acknowledgments
This report is based, in part, on contributions by Dabo Brantley, MPH, Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, CDC.
References
- CDC. The health consequences of smoking: a report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, CDC; 2004.
- CDC. How tobacco smoke causes disease: a report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, CDC; 2010.
- CDC. The health consequences of involuntary exposure to tobacco smoke: a report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, CDC; 2006.
- Dietz PM, England LJ, Shapiro-Mendoza CK, Tong VT, Farr SL, Callaghan WM. Infant morbidity and mortality attributable to prenatal smoking in the U.S. Am J. Prev Med 2010;39:45–52.
- Adams EK, Melvin CL, Raskind-Hood C, Joski PJ, Galactionova E. Infant delivery costs related to maternal smoking: an update. Nicotine Tob Res 2011;13:627–37.
- US Department of Health and Human Services. Healthy people 2020. Atlanta, GA: CDC. Available at http://www.healthypeople.gov/2020.
- CDC. Trends in smoking before, during, and after pregnancy—Pregnancy Risk Assessment Monitoring System (PRAMS), United States, 31 sites, 2000–2005. MMWR 2009;58(No. SS-4).
- CDC. Pregnancy Risk Assessment Monitoring System (PRAMS): phase 4 (2000–2003) core questions, phase 4 (2000–2003) standard questions, phase 5 (2004–2008) core questions and phase 5 (2004–2008) standard questions. Atlanta, GA: CDC. Available at www.cdc.gov/prams/Questionnaire.htm.
- Shulman HB, Gilbert BC, Lansky A. The Pregnancy Risk Assessment Monitoring System (PRAMS): current methods and evaluation of 2001 response rates. Public Health Rep 2006;121:74–83.
- Rinki C, Weng S, Irving JSD. Tribal PRAMS statewide surveillance report, June-November 2007 births. Aberdeen Area Tribal Chairmen's Health Board, Northern Plains Tribal Epidemiology Center, 2009. Available at http://www.aatchb.org/nptec/docs/SDT%20PRAMS%20Statewide%20Surveillance%20Report.pdf.
- SAS Institute. SAS: version 9.3. Cary, NC: SAS Institute; 2010.
- Research Triangle Institute. SUDAAN: version 11.0. Research Triangle Park, NC: Research Triangle Institute; 2010.
- Adams EK, Markowitz S, Kannan V, Dietz PM, Tong VT, Malarcher AM. Reducing prenatal smoking: the role of state policies. Am J Prev Med 2012;43:34–40.
- Markowitz S, Adam EK, Dietz PM, Kannan V, Tong VT. Tobacco control policies, birth outcomes, and maternal human capital. J Human Capital 2013;7:130–60.
- CDC. Tobacco control state highlights 2012. Atlanta, GA: US Department of Health and Human Services, CDC; 2013.Available at http://www.cdc.gov/tobacco/data_statistics/state_data/state_highlights/2012.
- Kim SY, England LJ, Kendrick JS, Dietz PM, Callaghan WM. The contribution of clinic-based interventions to reduce prenatal smoking prevalence among U.S. women. Am J Public Health 2009;99:893–8.
- Fiore MC, Bailey WC, Cohen SJ, Dorfman SF, Goldstein MG, Gritz ER. Treating tobacco use and dependence: clinical practice guidelines. Rockville, MD: US Department of Health and Human Services, Public Health Service; 2008.
- Lumley J, Chamberlain C, Dowswell T, Oliver S, Oakley L, Watson L. Interventions for promoting smoking cessation during pregnancy. Cochrane Database Syst Rev 2009;3:CD001055.
- American College of Obstetricians and Gynecologists. Committee opinion no. 471: smoking cessation during pregnancy. Obstet Gynecol 2010;116:1241–4.
- Higgins ST, Washio Y, Heil SH, et al. Financial incentives for smoking cessation among pregnant and newly postpartum women. Prev Med 2012;55(Suppl):S33–40.
- Centers for Medicare & Medicaid Services, US Department of Health and Human Services. New Medicaid tobacco cessation services, SDL # 11–007. Baltimore, MD: Centers for Medicare & Medicaid Services; 2011. Available at http://downloads.cms.gov/cmsgov/archived-downloads/SMDL/downloads/smd11-007.pdf.
- McMenamin SB, Halpin HA, Ganiats TG. Medicaid coverage of tobacco-dependence treatment for pregnant women: impact of the Affordable Care Act. Am J Prev Med 2012;43:e27–9.
- Centers for Medicare & Medicaid Services, US Department of Health and Human Services. New Medicaid tobacco cessation services, SDL # 13–002. Baltimore, MD: Centers for Medicare & Medicaid Services; 2013. Available at http://medicaid.gov/Federal-Policy-Guidance/Downloads/SMD-13-002.pdf.
- Rattan D, Mamun A, Najman J, Williams G, Doi S. Smoking behaviour in pregnancy and its impact on smoking cessation at various intervals during follow-up over 21 years: a prospective cohort study. BJOG 2013;120:288–96.
- Jha P, Ramasundarahettige C, Landsman V, et al. 21st-century hazards of smoking and benefits of cessation in the United States. N Engl J Med 2013;368:341–50.
- Dietz PM, Homa D, England LJ, et al. Estimates of nondisclosure of cigarette smoking among pregnant and nonpregnant women of reproductive age in the United States. Am J Epidemiol 2011;173:355–9.
- Cox B, Martens E, Nemery B, Vangronsveld J, Nawrot TS. Impact of a stepwise introduction of smoke-free legislation on the rate of preterm births: analysis of routinely collected birth data. BMJ 2013;346:f441.
- Mackay DF, Nelson SM, Haw SJ, Pell JP. Impact of Scotland's smoke-free legislation on pregnancy complications: retrospective cohort study. PLoS Med 2012;9:e1001175.
- Markowitz S. The effectiveness of cigarette regulations in reducing cases of Sudden Infant Death Syndrome. J Health Econ 2008;27:106–33.
- CDC. Best practices for comprehensive tobacco control programs—August 1999. Atlanta, GA: US Department of Health and Human Services, CDC; 1999.
- Tong VT, Dietz PM, England LJ. "Smoking cessation for pregnancy and beyond: a virtual clinic," an innovative web-based training for healthcare professionals. J Womens Health (Larchmt) 2012;21:1014–7.
Pregnancy Risk Assessment Monitoring System Working Group
Alabama: Izza Afgan; Alaska: Kathy Perham-Hester; Arkansas: Mary McGehee; Colorado: Alyson Shupe; Connecticut: Jennifer Morin; Delaware: George Yocher; Florida: Avalon Adams-Thames; Georgia: Chinelo Ogbuanu; Hawaii: Emily Roberson; Illinois: Theresa Sandidge; Iowa: Sarah Mauch; Louisiana: Amy Zapata; Maine: Tom Patenaude; Maryland: Diana Cheng; Massachusetts: Emily Lu; Michigan: Cristin Larder; Minnesota: Judy Punyko; Mississippi: Brenda Hughes; Missouri: Venkata Garikapaty; Montana: JoAnn Dotson; Nebraska: Brenda Coufal; New Hampshire: David J. Laflamme; New Jersey: Lakota Kruse; New Mexico: Eirian Coronado; New York state: Anne Radigan-Garcia; New York City: Candace Mulready-Ward; North Carolina: Kathleen Jones-Vessey; North Dakota: Sandra Anseth; Ohio: Connie Geidenberger; Oklahoma: Alicia Lincoln; Oregon: Kenneth Rosenberg; Pennsylvania: Tony Norwood; Rhode Island: Sam Viner-Brown; South Carolina: Mike Smith; South Dakota Tribal: Jennifer Irving; Texas: Rochelle Kingsley; Tennessee: David Law; Utah: Lynsey Gammon; Vermont: Peggy Brozicevic; Virginia: Marilyn Wenner; Washington: Linda Lohdefinck; West Virginia: Melissa Baker; Wisconsin: Katherine Kvale; Wyoming: Amy Spieker; PRAMS Team, Applied Sciences Branch, Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, CDC.
|
Site
|
Year
|
|
2000
(N = 19 sites)
|
2001
(N = 22 sites)
|
2002
(N = 27 sites)
|
2003
(N = 27 sites)
|
2004
(N = 27 sites)
|
2005
(N = 26 sites)
|
2006
(N = 24 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites¶
|
23.0
|
(22.2–23.8)
|
23.5
|
(22.7–24.2)
|
23.2
|
(22.5–23.9)
|
23.5
|
(22.8–24.1)
|
23.6
|
(22.9–24.2)
|
22.0
|
(21.4–22.7)
|
22.0
|
(21.4–22.7)
|
|
10 PRAMS sites**
|
23.6
|
(22.6–24.7)
|
24.3
|
(23.3–25.4)
|
24.0
|
(23.0–25.1)
|
23.1
|
(22.1–24.1)
|
23.9
|
(22.9–25.0)
|
23.6
|
(22.7–24.6)
|
24.0
|
(23.0–25.1)
|
|
Alabama
|
23.0
|
(20.4–25.7)
|
26.9
|
(24.3–29.7)
|
24.3
|
(21.8–27.1)
|
22.9
|
(20.3–25.7)
|
—††
|
—
|
—
|
—
|
—
|
—
|
|
Alaska
|
30.8
|
(28.2–33.5)
|
27.2
|
(24.8–29.7)
|
31.9
|
(29.4–34.6)
|
30.9
|
(28.3–33.5)
|
30.9
|
(28.0–33.9)
|
29.5
|
(26.7–32.4)
|
29.8
|
(26.9–32.8)
|
|
Arkansas
|
28.6
|
(25.5–31.9)
|
32.3
|
(29.6–35.2)
|
29.4
|
(26.7–32.3)
|
31.0
|
(28.3–34.0)
|
34.5
|
(31.8–37.3)
|
32.6
|
(30.0–35.3)
|
30.6
|
(28.0–33.3)
|
|
Colorado
|
19.9
|
(17.8–22.1)
|
21.3
|
(19.1–23.7)
|
20.1
|
(18.1–22.3)
|
18.7
|
(16.6–20.9)
|
21.3
|
(18.9–24.0)
|
20.2
|
(17.8–22.9)
|
20.3
|
(17.9–22.9)
|
|
Delaware§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Florida§§
|
17.2
|
(14.8–20.0)
|
19.7
|
(17.1–22.5)
|
19.5
|
(17.0–22.4)
|
21.3
|
(18.6–24.3)
|
22.1
|
(19.5–25.0)
|
17.9
|
(15.7–20.4)
|
—
|
—
|
|
Georgia§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
19.4
|
(16.7–22.4)
|
19.1
|
(16.5–21.9)
|
17.5
|
(15.2–20.2)
|
|
Hawaii
|
20.2
|
(18.5–22.0)
|
20.8
|
(19.2–22.6)
|
19.8
|
(17.7–22.0)
|
20.8
|
(18.7–23.0)
|
20.6
|
(18.9–22.5)
|
21.2
|
(19.2–23.2)
|
21.2
|
(19.2–23.3)
|
|
Illinois
|
20.3
|
(18.5–22.3)
|
21.1
|
(19.3–23.1)
|
21.6
|
(19.6–23.6)
|
21.9
|
(19.8–24.2)
|
22.3
|
(20.3–24.4)
|
18.8
|
(16.8–20.9)
|
21.6
|
(19.5–23.9)
|
|
Louisiana§§
|
21.2
|
(19.2–23.4)
|
24.2
|
(22.0–26.5)
|
22.7
|
(20.5–25.1)
|
24.4
|
(22.1–26.9)
|
28.2
|
(25.8–30.8)
|
—
|
—
|
—
|
—
|
|
Maine
|
31.2
|
(28.1–34.4)
|
29.8
|
(26.9–33.0)
|
28.9
|
(26.0–32.1)
|
29.0
|
(25.9–32.2)
|
31.0
|
(28.0–34.2)
|
32.1
|
(29.0–35.3)
|
30.7
|
(27.6–33.9)
|
|
Maryland§§
|
—
|
—
|
18.9
|
(15.9–22.4)
|
18.4
|
(15.5–21.7)
|
20.6
|
(17.5–23.9)
|
20.3
|
(17.3–23.7)
|
17.9
|
(14.9–21.3)
|
15.1
|
(12.6–18.0)
|
|
Massachusetts
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Michigan§§
|
—
|
—
|
29.3
|
(25.9–33.1)
|
28.9
|
(26.4–31.6)
|
27.6
|
(25.1–30.2)
|
31.7
|
(28.8–34.7)
|
28.8
|
(26.1–31.6)
|
32.1
|
(28.9–35.4)
|
|
Minnesota§§
|
—
|
—
|
—
|
—
|
27.7
|
(24.4–31.2)
|
24.6
|
(22.0–27.4)
|
27.6
|
(24.7–30.6)
|
27.2
|
(24.4–30.2)
|
25.6
|
(23.5–27.9)
|
|
Mississippi§§
|
—
|
—
|
—
|
—
|
—
|
—
|
21.9
|
(19.3–24.8)
|
21.4
|
(18.8–24.2)
|
—
|
—
|
25.8
|
(22.5–29.4)
|
|
Missouri
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Montana
|
—
|
—
|
—
|
—
|
29.7
|
(26.9–32.6)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Nebraska
|
24.8
|
(22.5–27.3)
|
26.9
|
(24.9–29.1)
|
27.6
|
(25.1–30.2)
|
25.7
|
(23.4–28.2)
|
26.1
|
(23.7–28.7)
|
25.8
|
(23.4–28.3)
|
26.2
|
(23.6–29.0)
|
|
New Jersey§§
|
—
|
—
|
—
|
—
|
17.2
|
(14.8–19.8)
|
15.7
|
(14.3–17.3)
|
16.7
|
(15.3–18.3)
|
16.1
|
(14.6–17.7)
|
14.8
|
(13.4–16.3)
|
|
New Mexico§§
|
21.3
|
(19.2–23.5)
|
24.0
|
(21.7–26.5)
|
19.8
|
(17.7–22.0)
|
18.4
|
(16.3–20.7)
|
20.7
|
(18.5–23.0)
|
18.8
|
(16.5–21.4)
|
—
|
—
|
|
New York§§, †††
|
27.1
|
(24.0–30.4)
|
24.8
|
(21.9–28.0)
|
23.3
|
(20.4–26.6)
|
25.6
|
(22.6–28.9)
|
28.4
|
(25.1–32.0)
|
23.0
|
(20.1–26.2)
|
22.3
|
(18.2–26.9)
|
|
New York City§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
14.2
|
(11.4–17.6)
|
12.4
|
(10.0–15.2)
|
10.7
|
(8.8–12.9)
|
|
North Carolina§§
|
24.4
|
(21.9–27.1)
|
21.3
|
(18.8–24.0)
|
22.5
|
(20.0–25.2)
|
23.6
|
(20.9–26.5)
|
26.7
|
(24.0–29.6)
|
22.5
|
(19.4–25.9)
|
—
|
—
|
|
North Dakota
|
—
|
—
|
—
|
—
|
26.4
|
(23.7–29.3)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Ohio
|
28.6
|
(25.6–31.8)
|
27.2
|
(24.3–30.3)
|
26.6
|
(23.7–29.9)
|
32.5
|
(29.2–36.0)
|
—
|
—
|
32.0
|
(28.7–35.6)
|
30.8
|
(27.7–34.0)
|
|
Oklahoma
|
30.2
|
(26.9–33.8)
|
31.8
|
(28.4–35.4)
|
31.2
|
(27.9–34.6)
|
28.6
|
(25.4–32.0)
|
31.8
|
(28.4–35.4)
|
31.6
|
(28.4–35.0)
|
31.4
|
(28.0–35.0)
|
|
Oregon
|
—
|
—
|
—
|
—
|
—
|
—
|
20.2
|
(17.1–23.9)
|
23.6
|
(20.4–27.0)
|
21.6
|
(18.7–24.8)
|
21.2
|
(18.3–24.5)
|
|
Pennsylvania§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Rhode Island
|
—
|
—
|
—
|
—
|
21.3
|
(18.9–24.1)
|
21.6
|
(19.1–24.2)
|
22.2
|
(19.7–24.8)
|
21.9
|
(19.4–24.6)
|
24.2
|
(21.6–27.2)
|
|
South Carolina§§
|
23.2
|
(20.1–26.7)
|
22.8
|
(19.6–26.3)
|
22.0
|
(18.6–25.8)
|
23.7
|
(20.3–27.5)
|
24.7
|
(21.3–28.4)
|
25.8
|
(22.3–29.5)
|
24.8
|
(20.3–29.9)
|
|
South Dakota Tribal§§,§§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Tennessee
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Texas§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Utah
|
14.3
|
(12.1–16.8)
|
13.8
|
(12.0–15.8)
|
13.6
|
(11.4–16.1)
|
11.5
|
(9.6–13.7)
|
12.3
|
(10.9–13.9)
|
10.2
|
(9.0–11.7)
|
12.1
|
(10.8–13.7)
|
|
Vermont§§
|
—
|
—
|
30.4
|
(28.0–32.8)
|
28.4
|
(25.8–31.1)
|
25.1
|
(22.8–27.6)
|
29.8
|
(27.0–32.7)
|
26.9
|
(24.3–29.8)
|
25.9
|
(23.3–28.6)
|
|
Washington
|
21.4
|
(18.5–24.6)
|
20.5
|
(17.6–23.7)
|
22.3
|
(19.2–25.6)
|
21.4
|
(18.5–24.6)
|
19.8
|
(17.0–22.8)
|
18.6
|
(15.9–21.6)
|
21.3
|
(18.5–24.4)
|
|
West Virginia§§
|
36.2
|
(33.1–39.5)
|
39.1
|
(35.7–42.5)
|
37.0
|
(33.8–40.4)
|
38.9
|
(35.6–42.3)
|
39.5
|
(34.9–44.3)
|
45.8
|
(42.4–49.2)
|
41.8
|
(38.4–45.2)
|
|
Wisconsin
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Wyoming
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Site
|
Year
|
p value†
|
Annual
percentage
point
change§
|
|
2007
(N = 31 sites)
|
2008
(N = 29 sites)
|
2009
(N = 29 sites)
|
2010
(N = 27 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites¶
|
22.5
|
(21.9–23.2)
|
23.0
|
(22.3–23.7)
|
25.2
|
(24.4–25.9)
|
23.2
|
(22.4–23.9)
|
0.14
|
NA
|
|
10 PRAMS sites**
|
24.3
|
(23.3–25.3)
|
22.6
|
(21.6–23.6)
|
26.1
|
(25.1–27.2)
|
24.7
|
(23.7–25.8)
|
0.26
|
NA
|
|
Alabama
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.69
|
NA
|
|
Alaska
|
27.6
|
(24.9–30.4)
|
27.9
|
(25.1–31.0)
|
32.7
|
(29.7–35.8)
|
33.8
|
(30.5–37.3)
|
0.14
|
NA
|
|
Arkansas
|
31.2
|
(28.4–34.0)
|
31.4
|
(28.5–34.4)
|
31.6
|
(28.2–35.3)
|
32.7
|
(29.7–36.0)
|
0.33
|
NA
|
|
Colorado
|
19.9
|
(17.6–22.5)
|
16.9
|
(14.8–19.3)
|
23.2
|
(20.7–25.8)
|
20.9
|
(18.6–23.5)
|
0.08
|
NA
|
|
Delaware§§
|
20.9
|
(17.9–24.3)
|
24.3
|
(22.0–26.8)
|
28.7
|
(26.0–31.4)
|
24.9
|
(22.4–27.5)
|
0.73
|
NA
|
|
Florida§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.29
|
NA
|
|
Georgia§§
|
16.9
|
(13.2–21.5)
|
17.5
|
(14.2–21.3)
|
19.7
|
(16.0–23.9)
|
19.9
|
(16.3–24.1)
|
0.29
|
NA
|
|
Hawaii
|
19.8
|
(18.0–21.8)
|
18.9
|
(17.1–20.9)
|
22.4
|
(19.9–25.1)
|
20.9
|
(18.5–23.6)
|
0.40
|
NA
|
|
Illinois
|
19.7
|
(17.8–21.8)
|
19.2
|
(17.2–21.4)
|
20.9
|
(18.8–23.2)
|
—
|
—
|
0.15
|
NA
|
|
Louisiana§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
<0.01¶¶
|
1.5
|
|
Maine
|
31.6
|
(28.5–34.9)
|
32.3
|
(29.2–35.6)
|
37.2
|
(33.8–40.6)
|
33.5
|
(30.2–37.0)
|
0.24
|
NA
|
|
Maryland§§
|
17.5
|
(14.8–20.7)
|
19.1
|
(16.2–22.2)
|
17.3
|
(14.6–20.5)
|
18.9
|
(16.0–22.2)
|
0.30
|
NA
|
|
Massachusetts
|
15.6
|
(13.0–18.6)
|
19.5
|
(16.7–22.7)
|
22.3
|
(19.3–25.6)
|
17.7
|
(15.0–20.8)
|
0.87
|
NA
|
|
Michigan§§
|
28.9
|
(26.3–31.7)
|
26.9
|
(24.4–29.6)
|
33.2
|
(30.5–36.0)
|
32.7
|
(29.9–35.7)
|
0.59
|
NA
|
|
Minnesota§§
|
24.7
|
(22.4–27.1)
|
22.1
|
(19.9–24.6)
|
26.4
|
(24.0–29.0)
|
26.0
|
(23.4–28.7)
|
0.01¶¶
|
-0.6
|
|
Mississippi§§
|
—
|
—
|
26.0
|
(23.2–29.1)
|
29.8
|
(26.9–32.9)
|
—
|
—
|
0.01¶¶
|
1.0
|
|
Missouri
|
31.7
|
(28.8–34.8)
|
—
|
—
|
35.2
|
(32.1–38.4)
|
33.5
|
(30.6–36.4)
|
0.44
|
NA
|
|
Montana
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Nebraska
|
27.8
|
(25.0–30.7)
|
22.8
|
(20.2–25.6)
|
29.3
|
(26.8–31.9)
|
25.5
|
(23.1–28.0)
|
0.31
|
NA
|
|
New Jersey§§
|
14.1
|
(12.6–15.8)
|
15.8
|
(14.0–17.7)
|
19.2
|
(17.3–21.3)
|
18.2
|
(16.3–20.2)
|
0.07
|
NA
|
|
New Mexico§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.02¶¶
|
-0.8
|
|
New York§§, †††
|
23.4
|
(20.3–26.8)
|
21.4
|
(18.5–24.6)
|
—
|
—
|
24.8
|
(21.5–28.4)
|
0.02¶¶
|
-0.5
|
|
New York City§§
|
11.3
|
(9.3–13.6)
|
—
|
—
|
—
|
—
|
9.2
|
(7.5–11.3)
|
0.11
|
NA
|
|
North Carolina§§
|
22.9
|
(20.5–25.6)
|
22.3
|
(19.9–25.0)
|
—
|
—
|
—
|
—
|
0.76
|
NA
|
|
North Dakota
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Ohio
|
28.5
|
(25.3–31.8)
|
32.1
|
(28.9–35.5)
|
35.2
|
(31.8–38.7)
|
31.1
|
(27.7–34.6)
|
0.06
|
NA
|
|
Oklahoma
|
37.8
|
(34.1–41.5)
|
31.9
|
(28.5–35.5)
|
34.8
|
(31.3–38.4)
|
33.6
|
(30.1–37.4)
|
0.04¶¶
|
0.4
|
|
Oregon
|
21.2
|
(18.1–24.6)
|
20.1
|
(16.9–23.8)
|
25.7
|
(22.4–29.3)
|
26.6
|
(23.6–29.7)
|
0.60
|
NA
|
|
Pennsylvania§§
|
27.8
|
(23.3–32.8)
|
28.1
|
(25.2–31.2)
|
28.1
|
(25.0–31.3)
|
29.2
|
(26.0–32.6)
|
0.66
|
NA
|
|
Rhode Island
|
22.9
|
(20.3–25.7)
|
22.4
|
(19.8–25.3)
|
22.3
|
(19.7–25.2)
|
21.7
|
(19.2–24.6)
|
0.28
|
NA
|
|
South Carolina§§
|
22.8
|
(19.4–26.6)
|
—
|
—
|
—
|
—
|
—
|
—
|
0.49
|
NA
|
|
South Dakota Tribal§§,§§§
|
52.5
|
(50.0–55.1)
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Tennessee
|
—
|
—
|
30.7
|
(26.5–35.1)
|
34.3
|
(29.9–39.0)
|
—
|
—
|
***
|
NA
|
|
Texas§§
|
—
|
—
|
—
|
—
|
19.3
|
(17.1–21.8)
|
18.6
|
(16.5–21.0)
|
***
|
NA
|
|
Utah
|
10.6
|
(9.2–12.2)
|
10.4
|
(9.1–11.9)
|
13.1
|
(11.4–14.9)
|
11.8
|
(10.2–13.6)
|
<0.01¶¶
|
-0.9
|
|
Vermont§§
|
29.6
|
(26.9–32.4)
|
29.6
|
(26.9–32.4)
|
33.1
|
(30.2–36.1)
|
31.4
|
(28.6–34.3)
|
0.78
|
NA
|
|
Washington
|
19.9
|
(17.2–22.9)
|
20.2
|
(17.5–23.1)
|
22.5
|
(19.7–25.6)
|
20.2
|
(17.6–23.1)
|
0.29
|
NA
|
|
West Virginia§§
|
40.5
|
(37.2–43.8)
|
39.4
|
(36.5–42.3)
|
43.0
|
(40.1–46.0)
|
46.2
|
(43.0–49.4)
|
0.01¶¶
|
0.4
|
|
Wisconsin
|
30.0
|
(26.8–33.5)
|
22.9
|
(19.8–26.2)
|
26.5
|
(23.3–30.0)
|
—
|
—
|
<0.01¶¶
|
-6.3
|
|
Wyoming
|
32.0
|
(28.7–35.6)
|
28.7
|
(25.4–32.3)
|
32.6
|
(29.0–36.5)
|
29.8
|
(26.5–33.3)
|
0.09
|
NA
|
|
Maternal characteristic
|
Smoked before pregnancy†
|
Smoked during pregnancy§
|
Quit smoking during pregnancy¶
|
Smoked after delivery**
|
|
Unweighted (N = 9,808)
|
Unweighted (N = 6,097)
|
Unweighted (N = 4,712)
|
Unweighted (N = 7,023)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total
|
23.2
|
(22.4–23.9)
|
10.7
|
(10.2–11.2)
|
54.3
|
(52.4–56.1)
|
15.9
|
(15.3–16.5)
|
|
Age group (yrs)
|
|
<20
|
32.2
|
(29.2–35.4)
|
13.6
|
(11.6–15.9)
|
59.3
|
(53.6–64.7)
|
24.3
|
(21.7–27.2)
|
|
20–24
|
34.7
|
(32.9–36.6)
|
17.6
|
(16.2–19.0)
|
50.0
|
(46.8–53.3)
|
25.5
|
(23.9–27.2)
|
|
25–34
|
19.8
|
(18.9–20.8)
|
8.8
|
(8.1–9.4)
|
55.9
|
(53.3–58.5)
|
12.8
|
(12.0–13.6)
|
|
≥35
|
12.5
|
(11.1–14.0)
|
5.7
|
(4.8–6.7)
|
54.7
|
(48.6–60.7)
|
7.6
|
(6.6–8.8)
|
|
Race/Ethnicity
|
|
White, non-Hispanic
|
29.3
|
(28.2–30.3)
|
14.3
|
(13.5–15.2)
|
51.5
|
(49.3–53.7)
|
20.1
|
(19.2–21.1)
|
|
Black, non-Hispanic
|
19.7
|
(18.0–21.5)
|
8.9
|
(7.8–10.2)
|
55.9
|
(51.0–60.6)
|
16.2
|
(14.7–17.9)
|
|
Hispanic
|
11.8
|
(10.3–13.4)
|
3.4
|
(2.7–4.3)
|
71.2
|
(64.8–76.8)
|
6.5
|
(5.4–7.7)
|
|
American Indian/Alaska Native
|
55.1
|
(48.3–61.8)
|
26.0
|
(20.5–32.3)
|
53.1
|
(43.4–62.5)
|
40.1
|
(33.3–47.2)
|
|
Asian/Pacific Islander
|
7.5
|
(6.1–9.1)
|
2.1
|
(1.5–2.9)
|
72.0
|
(63.1–79.3)
|
3.6
|
(2.9–4.6)
|
|
Other
|
24.4
|
(20.1–29.4)
|
13.9
|
(10.5–18.2)
|
43.1
|
(32.9–54.0)
|
17.8
|
(14.2–22.0)
|
|
Education (yrs)
|
|
<12
|
28.1
|
(26.2–30.2)
|
17.4
|
(15.8–19.1)
|
39.1
|
(35.1–43.3)
|
22.9
|
(21.2–24.8)
|
|
12
|
32.6
|
(30.9–34.3)
|
16.4
|
(15.2–17.7)
|
50.2
|
(47.1–53.4)
|
24.5
|
(23.0–26.1)
|
|
>12
|
17.3
|
(16.4–18.2)
|
5.9
|
(5.4–6.5)
|
65.7
|
(63.0–68.2)
|
9.7
|
(9.1–10.4)
|
|
Health insurance coverage††
|
|
Private
|
17.0
|
(16.1–17.9)
|
5.2
|
(4.7–5.7)
|
68.2
|
(65.4–70.8)
|
9.3
|
(8.6–10.0)
|
|
Medicaid
|
34.4
|
(32.3–36.5)
|
17.6
|
(16.6–18.6)
|
45.7
|
(43.3–48.2)
|
24.3
|
(23.1–25.5)
|
|
Other insurance§§
|
26.7
|
(22.6–31.3)
|
10.7
|
(7.9–14.5)
|
55.2
|
(45.0–65.1)
|
15.6
|
(12.3–19.6)
|
|
Uninsured
|
29.8
|
(28.1–31.6)
|
6.6
|
(4.1–10.6)
|
56.7
|
(38.1–73.6)
|
7.9
|
(4.9–12.5)
|
FIGURE 1. Prevalence of smoking before pregnancy, during pregnancy, and after delivery,* by year —Pregnancy Risk Assessment Monitoring System, United States, 10 sites,† 2000–2010
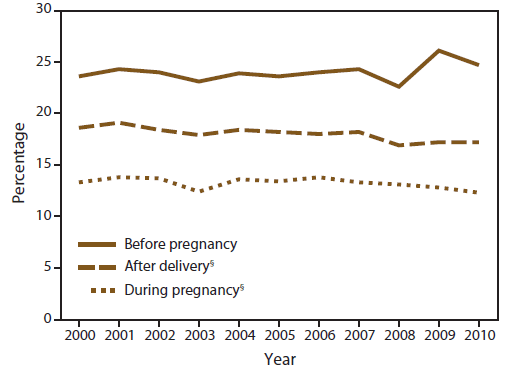
Alternate Text: The figure is a line graph that presents the prevalence of smoking among women before, during, and after pregnancy by year from 10 selected sites across the United States from 2000 to 2010.
FIGURE 2. Prevalence of smoking during pregnancy*— Pregnancy Risk Assessment Monitoring System, United States, 27 sites,† 2010
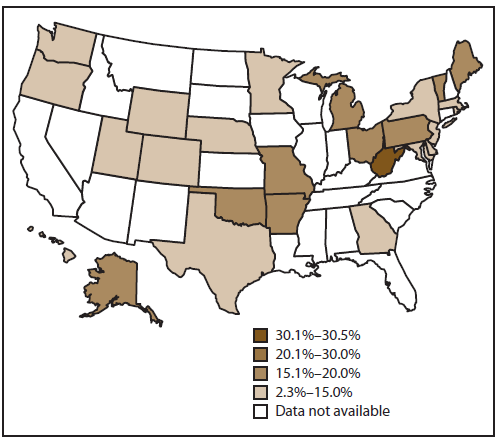
Alternate Text: The figure is a U.S. map that presents the prevalence of smoking among women during pregnancy from 27 selected sites in 2010.
|
Site
|
Year
|
|
2000
(N = 19 sites)
|
2001
(N = 22 sites)
|
2002
(N = 27 sites)
|
2003
(N = 27 sites)
|
2004
(N = 27 sites)
|
2005
(N = 26 sites)
|
2006
(N = 24 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites¶
|
13.2
|
(12.6–13.9)
|
13.4
|
(12.8–14.0)
|
13.1
|
(12.6–13.7)
|
13.0
|
(12.5–13.5)
|
12.9
|
(12.4–13.4)
|
12.2
|
(11.7–12.8)
|
11.8
|
(11.2–12.3)
|
|
10 PRAMS sites††
|
13.3
|
(12.5–14.1)
|
13.8
|
(13.0–14.6)
|
13.7
|
(12.9–14.6)
|
12.4
|
(11.7–13.2)
|
13.6
|
(12.8–14.5)
|
13.4
|
(12.6–14.2)
|
13.8
|
(13.0–14.7)
|
|
Alabama
|
14.0
|
(12.0–16.2)
|
15.6
|
(13.5–17.9)
|
14.4
|
(12.4–16.7)
|
13.3
|
(11.3–15.6)
|
—§§
|
—
|
—
|
—
|
—
|
—
|
|
Alaska
|
16.8
|
(14.9–19.0)
|
14.7
|
(12.9–16.6)
|
17.7
|
(15.8–19.8)
|
16.7
|
(14.8–18.9)
|
17.4
|
(15.1–19.9)
|
16.0
|
(13.9–18.4)
|
14.8
|
(12.7–17.0)
|
|
Arkansas
|
20.3
|
(17.6–23.2)
|
20.1
|
(17.8–22.5)
|
19.2
|
(16.9–21.7)
|
18.5
|
(16.3–20.9)
|
23.1
|
(20.8–25.6)
|
20.9
|
(18.7–23.2)
|
19.4
|
(17.3–21.8)
|
|
Colorado
|
10.2
|
(8.7–11.9)
|
11.4
|
(9.8–13.3)
|
10.6
|
(9.1–12.2)
|
10.6
|
(9.0–12.4)
|
10.4
|
(8.7–12.3)
|
10.2
|
(8.4–12.3)
|
10.4
|
(8.7–12.4)
|
|
Delaware¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Florida¶¶
|
9.1
|
(7.3–11.2)
|
9.4
|
(7.7–11.6)
|
10.0
|
(8.1–12.2)
|
10.6
|
(8.7–12.9)
|
10.0
|
(8.2–12.1)
|
8.3
|
(6.8–10.1)
|
—
|
—
|
|
Georgia¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
10.5
|
(8.4–12.9)
|
10.3
|
(8.4–12.6)
|
9.3
|
(7.5–11.4)
|
|
Hawaii
|
8.4
|
(7.3–9.6)
|
9.5
|
(8.4–10.8)
|
8.1
|
(6.8–9.6)
|
9.3
|
(7.9–11.0)
|
8.1
|
(6.9–9.4)
|
8.4
|
(7.1–9.8)
|
9.4
|
(8.0–11.0)
|
|
Illinois
|
12.5
|
(11.0–14.1)
|
12.6
|
(11.1–14.2)
|
11.4
|
(10.0–13.0)
|
12.6
|
(11.0–14.5)
|
12.1
|
(10.6–13.8)
|
10.4
|
(8.9–12.1)
|
11.4
|
(9.8–13.2)
|
|
Louisiana¶¶
|
11.9
|
(10.4–13.7)
|
12.8
|
(11.2–14.7)
|
11.8
|
(10.2–13.7)
|
14.5
|
(12.6–16.6)
|
17.7
|
(15.7–20.0)
|
—
|
—
|
—
|
—
|
|
Maine
|
17.5
|
(15.0–20.2)
|
17.3
|
(14.9–20.0)
|
15.9
|
(13.5–18.6)
|
16.2
|
(13.8–18.9)
|
20.0
|
(17.5–22.9)
|
17.5
|
(15.0–20.2)
|
17.1
|
(14.7–19.9)
|
|
Maryland¶¶
|
—
|
—
|
9.4
|
(7.3–12.1)
|
8.3
|
(6.4–10.7)
|
11.1
|
(8.9–13.9)
|
10.3
|
(8.1–12.9)
|
10.0
|
(7.7–12.8)
|
7.8
|
(6.0–10.1)
|
|
Massachusetts
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Michigan¶¶
|
—
|
—
|
20.0
|
(16.9–23.4)
|
17.4
|
(15.3–19.7)
|
15.6
|
(13.6–17.8)
|
18.9
|
(16.6–21.5)
|
15.8
|
(13.7–18.2)
|
18.0
|
(15.5–20.9)
|
|
Minnesota¶¶
|
—
|
—
|
—
|
—
|
15.4
|
(12.9–18.3)
|
14.9
|
(12.8–17.3)
|
15.9
|
(13.7–18.5)
|
15.6
|
(13.4–18.1)
|
13.6
|
(11.9–15.5)
|
|
Mississippi¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
13.5
|
(11.4–15.8)
|
13.9
|
(11.8–16.4)
|
—
|
—
|
14.4
|
(11.9–17.4)
|
|
Missouri
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Montana
|
—
|
—
|
—
|
—
|
15.9
|
(13.7–18.3)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Nebraska
|
14.0
|
(12.2–16.0)
|
14.8
|
(13.2–16.7)
|
14.4
|
(12.4–16.6)
|
13.0
|
(11.2–15.0)
|
16.0
|
(14.0–18.3)
|
15.2
|
(13.3–17.3)
|
14.9
|
(12.8–17.4)
|
|
New Jersey¶¶
|
—
|
—
|
—
|
—
|
9.0
|
(7.5–10.7)
|
7.9
|
(7.0–8.9)
|
7.9
|
(7.0–8.8)
|
6.7
|
(5.9–7.6)
|
5.7
|
(5.0–6.4)
|
|
New Mexico¶¶
|
9.3
|
(7.9–10.9)
|
10.7
|
(9.0–12.5)
|
8.2
|
(6.9–9.8)
|
8.2
|
(6.7–9.9)
|
9.9
|
(8.3–11.6)
|
8.6
|
(7.0–10.5)
|
—
|
—
|
|
New York¶¶,†††
|
17.0
|
(14.4–19.9)
|
14.4
|
(12.1–17.0)
|
14.6
|
(12.2–17.4)
|
14.6
|
(12.2–17.4)
|
15.6
|
(12.9–18.7)
|
12.9
|
(10.7–15.6)
|
12.2
|
(9.1–16.1)
|
|
New York City¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
7.6
|
(5.5–10.3)
|
5.0
|
(3.5–7.1)
|
3.9
|
(2.8–5.4)
|
|
North Carolina¶¶
|
13.9
|
(12.0–16.2)
|
12.2
|
(10.3–14.4)
|
11.7
|
(9.9–13.8)
|
13.2
|
(11.2–15.6)
|
14.8
|
(12.7–17.2)
|
13.3
|
(10.9–16.2)
|
—
|
—
|
|
North Dakota
|
—
|
—
|
—
|
—
|
15.6
|
(13.5–18.0)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Ohio
|
17.1
|
(14.7–19.8)
|
17.5
|
(15.1–20.1)
|
17.6
|
(15.0–20.4)
|
19.0
|
(16.3–22.0)
|
—
|
—
|
21.6
|
(18.7–24.8)
|
17.0
|
(14.5–19.7)
|
|
Oklahoma
|
16.9
|
(14.3–19.9)
|
20.3
|
(17.4–23.5)
|
20.0
|
(17.2–23.0)
|
16.2
|
(13.7–19.1)
|
19.0
|
(16.2–22.1)
|
19.6
|
(16.9–22.6)
|
19.3
|
(16.5–22.5)
|
|
Oregon
|
—
|
—
|
—
|
—
|
—
|
—
|
12.1
|
(9.5–15.2)
|
13.7
|
(11.2–16.7)
|
13.7
|
(11.3–16.5)
|
10.7
|
(8.6–13.3)
|
|
Pennsylvania¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Rhode Island
|
—
|
—
|
—
|
—
|
12.9
|
(11.0–15.2)
|
10.5
|
(8.8–12.5)
|
11.3
|
(9.5–13.4)
|
11.7
|
(9.8–13.8)
|
13.4
|
(11.3–15.9)
|
|
South Carolina¶¶
|
12.4
|
(10.1–15.2)
|
13.0
|
(10.6–15.9)
|
13.1
|
(10.5–16.3)
|
11.4
|
(9.0–14.4)
|
13.9
|
(11.3–17.0)
|
14.9
|
(12.2–18.1)
|
10.9
|
(8.0–14.8)
|
|
South Dakota Tribal¶¶,§§§
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Tennessee
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Texas¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Utah
|
7.3
|
(5.7–9.3)
|
7.7
|
(6.4–9.3)
|
6.8
|
(5.2–8.7)
|
3.9
|
(2.9–5.2)
|
6.6
|
(5.5–7.8)
|
5.1
|
(4.2–6.1)
|
6.1
|
(5.1–7.1)
|
|
Vermont¶¶
|
—
|
—
|
17.8
|
(15.9–19.9)
|
18.2
|
(16.0–20.6)
|
15.3
|
(13.4–17.4)
|
18.0
|
(15.7–20.5)
|
16.4
|
(14.2–18.8)
|
15.5
|
(13.4–17.8)
|
|
Washington
|
11.1
|
(9.0–13.7)
|
9.9
|
(7.8–12.4)
|
11.8
|
(9.5–14.7)
|
10.2
|
(8.2–12.7)
|
10.3
|
(8.3–12.8)
|
9.2
|
(7.3–11.7)
|
12.2
|
(10.0–15.0)
|
|
West Virginia¶¶
|
24.5
|
(21.7–27.4)
|
26.1
|
(23.3–29.2)
|
25.3
|
(22.5–28.3)
|
27.5
|
(24.5–30.7)
|
28.4
|
(24.3–32.9)
|
31.9
|
(28.8–35.2)
|
29.4
|
(26.4–32.5)
|
|
Wisconsin
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Wyoming
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Site
|
Year
|
p value†
|
Annual
percentage
point
change§
|
|
2007
(N = 31 sites)
|
2008
(N = 29 sites)
|
2009
(N = 29 sites)
|
2010
(N = 27 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites¶
|
12.4
|
(11.9–13.0)
|
12.8
|
(12.3–13.3)
|
12.4
|
(11.8–12.9)
|
10.7
|
(10.2–11.2)
|
<0.01**
|
-0.1
|
|
10 PRAMS sites††
|
13.3
|
(12.5–14.2)
|
13.1
|
(12.3–13.9)
|
12.8
|
(12.0–13.6)
|
12.3
|
(11.5–13.1)
|
0.04**
|
-0.1
|
|
Alabama
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.33
|
NA
|
|
Alaska
|
15.5
|
(13.5–17.7)
|
15.0
|
(12.9–17.5)
|
15.3
|
(13.3–17.7)
|
16.8
|
(14.3–19.6)
|
0.47
|
NA
|
|
Arkansas
|
18.8
|
(16.6–21.2)
|
24.0
|
(21.4–26.8)
|
18.8
|
(16.1–21.9)
|
18.6
|
(16.1–21.3)
|
0.68
|
NA
|
|
Colorado
|
10.1
|
(8.4–12.1)
|
8.1
|
(6.6–10.0)
|
9.0
|
(7.5–10.9)
|
8.1
|
(6.7–9.9)
|
<0.01**
|
-0.3
|
|
Delaware¶¶
|
12.6
|
(10.2–15.4)
|
13.3
|
(11.5–15.3)
|
16.6
|
(14.5–19.0)
|
12.8
|
(11.0–14.9)
|
0.34
|
NA
|
|
Florida¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.86
|
NA
|
|
Georgia¶¶
|
7.6
|
(5.2–11.1)
|
8.1
|
(5.9–11.0)
|
8.5
|
(6.1–11.6)
|
8.3
|
(6.0–11.4)
|
0.08
|
NA
|
|
Hawaii
|
8.4
|
(7.1–9.8)
|
8.5
|
(7.3–10.0)
|
9.6
|
(7.9–11.7)
|
7.8
|
(6.2–9.8)
|
0.72
|
NA
|
|
Illinois
|
10.7
|
(9.2–12.4)
|
9.6
|
(8.2–11.3)
|
9.2
|
(7.7–10.8)
|
—
|
—
|
<0.01**
|
-0.3
|
|
Louisiana¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
<0.01**
|
1.1
|
|
Maine
|
19.9
|
(17.3–22.8)
|
19.5
|
(16.9–22.4)
|
21.2
|
(18.4–24.2)
|
18.2
|
(15.5–21.2)
|
0.02**
|
0.2
|
|
Maryland¶¶
|
9.3
|
(7.2–11.8)
|
10.9
|
(8.7–13.6)
|
9.1
|
(7.1–11.6)
|
9.3
|
(7.3–11.8)
|
0.93
|
NA
|
|
Massachusetts
|
8.8
|
(6.9–11.3)
|
9.8
|
(7.7–12.4)
|
11.5
|
(9.1–14.3)
|
6.7
|
(5.0–8.9)
|
0.30
|
NA
|
|
Michigan¶¶
|
14.9
|
(12.9–17.2)
|
16.0
|
(14.0–18.3)
|
17.8
|
(15.7–20.2)
|
16.9
|
(14.7–19.5)
|
0.33
|
NA
|
|
Minnesota¶¶
|
15.0
|
(13.1–17.0)
|
11.6
|
(9.9–13.6)
|
14.4
|
(12.5–16.5)
|
13.7
|
(11.7–16.0)
|
0.03**
|
-0.2
|
|
Mississippi¶¶
|
—
|
—
|
15.6
|
(13.3–18.2)
|
16.6
|
(14.3–19.1)
|
—
|
—
|
0.03**
|
0.4
|
|
Missouri
|
18.4
|
(16.0–21.0)
|
—
|
—
|
18.9
|
(16.5–21.6)
|
16.7
|
(14.6–19.1)
|
0.39
|
NA
|
|
Montana
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Nebraska
|
14.7
|
(12.5–17.2)
|
14.0
|
(11.8–16.4)
|
13.6
|
(11.8–15.7)
|
12.5
|
(10.7–14.6)
|
0.28
|
NA
|
|
New Jersey¶¶
|
6.2
|
(5.3–7.2)
|
6.8
|
(5.8–8.0)
|
6.5
|
(5.6–7.6)
|
6.6
|
(5.7–7.7)
|
<0.01**
|
-0.3
|
|
New Mexico¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.40
|
NA
|
|
New York¶¶,†††
|
13.7
|
(11.2–16.5)
|
11.9
|
(9.7–14.6)
|
—
|
—
|
11.4
|
(9.0–14.3)
|
<0.01**
|
-0.3
|
|
New York City¶¶
|
4.7
|
(3.4–6.4)
|
—
|
—
|
—
|
—
|
2.3
|
(1.5–3.5)
|
<0.01**
|
-1.5
|
|
North Carolina¶¶
|
14.3
|
(12.3–16.6)
|
12.5
|
(10.6–14.6)
|
—
|
—
|
—
|
—
|
0.79
|
NA
|
|
North Dakota
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Ohio
|
18.0
|
(15.4–21.0)
|
18.9
|
(16.3–21.9)
|
21.0
|
(18.1–24.2)
|
16.5
|
(13.9–19.5)
|
0.46
|
NA
|
|
Oklahoma
|
21.3
|
(18.3–24.6)
|
16.9
|
(14.3–19.9)
|
18.5
|
(15.7–21.6)
|
19.3
|
(16.4–22.6)
|
0.64
|
NA
|
|
Oregon
|
10.4
|
(8.2–13.1)
|
11.2
|
(8.7–14.3)
|
12.1
|
(9.7–15.0)
|
10.1
|
(8.1–12.5)
|
0.09
|
NA
|
|
Pennsylvania¶¶
|
15.4
|
(11.8–19.8)
|
15.6
|
(13.3–18.2)
|
14.0
|
(11.7–16.7)
|
15.1
|
(12.7–17.9)
|
0.82
|
NA
|
|
Rhode Island
|
12.4
|
(10.4–14.7)
|
10.8
|
(8.9–13.0)
|
9.4
|
(7.6–11.6)
|
9.7
|
(8.0–11.9)
|
0.06
|
NA
|
|
South Carolina¶¶
|
12.4
|
(9.8–15.6)
|
—
|
—
|
—
|
—
|
—
|
—
|
0.82
|
NA
|
|
South Dakota Tribal¶¶,§§§
|
31.4
|
(29.1–33.8)
|
—
|
—
|
—
|
—
|
—
|
—
|
***
|
NA
|
|
Tennessee
|
—
|
—
|
19.7
|
(16.3–23.7)
|
22.2
|
(18.5–26.6)
|
—
|
—
|
***
|
NA
|
|
Texas¶¶
|
—
|
—
|
—
|
—
|
7.2
|
(5.8–8.8)
|
7.0
|
(5.7–8.6)
|
***
|
NA
|
|
Utah
|
5.3
|
(4.3–6.6)
|
5.1
|
(4.2–6.2)
|
5.9
|
(4.8–7.3)
|
4.5
|
(3.5–5.7)
|
<0.01**
|
-0.3
|
|
Vermont¶¶
|
17.5
|
(15.3–19.8)
|
18.1
|
(15.8–20.5)
|
17.5
|
(15.3–20.0)
|
17.9
|
(15.6–20.4)
|
0.57
|
NA
|
|
Washington
|
9.4
|
(7.5–11.8)
|
11.2
|
(9.2–13.7)
|
9.3
|
(7.4–11.6)
|
8.9
|
(7.0–11.2)
|
0.21
|
NA
|
|
West Virginia¶¶
|
30.0
|
(27.0–33.1)
|
28.7
|
(26.1–31.4)
|
28.9
|
(26.3–31.7)
|
30.5
|
(27.6–33.5)
|
<0.01**
|
0.2
|
|
Wisconsin
|
17.4
|
(14.8–20.5)
|
13.2
|
(10.8–16.0)
|
13.9
|
(11.4–16.9)
|
—
|
—
|
0.12
|
NA
|
|
Wyoming
|
17.6
|
(15.0–20.6)
|
16.1
|
(13.4–19.1)
|
16.2
|
(13.5–19.4)
|
14.8
|
(12.3–17.6)
|
0.19
|
NA
|
|
Site
|
Year
|
|
2000
(N = 19 sites)
|
2001
(N = 22 sites)
|
2002
(N = 27 sites)
|
2003
(N = 27 sites)
|
2004
(N = 27 sites)
|
2005
(N = 26 sites)
|
2006
(N = 24 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites**
|
43.2
|
(41.3–45.2)
|
43.9
|
(42.1–45.7)
|
44.5
|
(42.8–46.2)
|
45.7
|
(44.0–47.4)
|
45.2
|
(43.6–46.9)
|
44.8
|
(43.1–46.5)
|
46.9
|
(45.1–48.6)
|
|
10 PRAMS sites§§
|
45.1
|
(42.6–47.7)
|
44.5
|
(42.1–47.0)
|
44.6
|
(42.1–47.2)
|
47.5
|
(44.9–50.1)
|
43.0
|
(40.5–45.5)
|
43.6
|
(41.2–46.1)
|
42.8
|
(40.3–45.3)
|
|
Alabama
|
41.7
|
(35.4–48.3)
|
41.4
|
(35.5–47.5)
|
41.6
|
(35.6–47.9)
|
44.2
|
(37.5–51.1)
|
—¶¶
|
—
|
—
|
—
|
—
|
—
|
|
Alaska
|
45.7
|
(40.5–50.9)
|
46.6
|
(41.4–51.8)
|
46.1
|
(41.3–50.9)
|
46.8
|
(41.8–51.8)
|
44.5
|
(38.9–50.3)
|
46.1
|
(40.3–51.9)
|
50.8
|
(45.0–56.6)
|
|
Arkansas
|
31.9
|
(26.2–38.3)
|
37.4
|
(32.3–42.8)
|
35.6
|
(30.3–41.3)
|
40.3
|
(34.9–46.0)
|
33.1
|
(28.6–37.8)
|
36.1
|
(31.5–40.9)
|
36.4
|
(31.6–41.5)
|
|
Colorado
|
49.3
|
(43.2–55.3)
|
47.6
|
(41.6–53.7)
|
49.3
|
(43.5–55.2)
|
46.0
|
(39.7–52.3)
|
52.0
|
(45.3–58.6)
|
50.1
|
(43.0–57.2)
|
49.3
|
(42.5–56.1)
|
|
Delaware***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Florida***
|
47.8
|
(39.5–56.2)
|
53.7
|
(46.0–61.3)
|
49.8
|
(42.0–57.6)
|
51.5
|
(43.9–59.1)
|
54.7
|
(47.6–61.7)
|
53.7
|
(46.4–60.7)
|
—
|
—
|
|
Georgia***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
46.1
|
(37.8–54.5)
|
46.3
|
(38.4–54.4)
|
48.5
|
(40.7–56.4)
|
|
Hawaii
|
59.3
|
(54.6–63.9)
|
56.0
|
(51.4–60.5)
|
59.1
|
(53.2–64.8)
|
55.6
|
(49.8–61.3)
|
61.3
|
(56.3–66.1)
|
61.0
|
(55.7–66.1)
|
55.8
|
(50.3–61.2)
|
|
Illinois
|
40.3
|
(35.2–45.7)
|
41.3
|
(36.4–46.4)
|
47.4
|
(42.3–52.7)
|
44.5
|
(38.9–50.4)
|
45.8
|
(40.7–51.0)
|
44.7
|
(38.8–50.7)
|
47.3
|
(41.6–53.0)
|
|
Louisiana***
|
44.2
|
(38.7–49.7)
|
46.2
|
(40.9–51.7)
|
49.1
|
(43.2–54.9)
|
39.7
|
(34.2–45.4)
|
37.1
|
(32.2–42.4)
|
—
|
—
|
—
|
—
|
|
Maine
|
43.9
|
(37.9–50.1)
|
41.6
|
(35.7–47.7)
|
46.6
|
(40.3–53.0)
|
45.5
|
(39.1–52.0)
|
35.1
|
(29.6–41.1)
|
45.2
|
(39.3–51.2)
|
43.5
|
(37.4–49.8)
|
|
Maryland***
|
—
|
—
|
53.8
|
(44.3–63.1)
|
54.5
|
(45.2–63.6)
|
45.5
|
(36.9–54.4)
|
49.5
|
(40.7–58.3)
|
44.3
|
(34.7–54.3)
|
48.4
|
(38.9–58.1)
|
|
Massachusetts
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Michigan***
|
—
|
—
|
33.1
|
(26.8–40.2)
|
39.9
|
(34.7–45.3)
|
44.2
|
(38.8–49.8)
|
39.9
|
(34.5–45.7)
|
44.9
|
(39.3–50.7)
|
43.6
|
(37.4–49.9)
|
|
Minnesota***
|
—
|
—
|
—
|
—
|
45.3
|
(38.3–52.4)
|
39.9
|
(33.9–46.3)
|
42.7
|
(36.6–49.0)
|
42.9
|
(36.9–49.1)
|
47.5
|
(42.5–52.6)
|
|
Mississippi***
|
—
|
—
|
—
|
—
|
—
|
—
|
39.0
|
(32.2–46.2)
|
35.3
|
(28.9–42.4)
|
—
|
—
|
43.2
|
(35.6–51.0)
|
|
Missouri
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Montana
|
—
|
—
|
—
|
—
|
48.1
|
(42.3–54.0)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Nebraska
|
43.6
|
(38.0–49.2)
|
46.5
|
(41.8–51.3)
|
47.7
|
(42.1–53.5)
|
50.8
|
(45.2–56.4)
|
38.5
|
(33.1–44.1)
|
40.7
|
(35.4–46.3)
|
43.9
|
(37.8–50.1)
|
|
New Jersey***
|
—
|
—
|
—
|
—
|
47.9
|
(39.8–56.2)
|
51.3
|
(45.9–56.6)
|
53.0
|
(48.1–57.8)
|
58.5
|
(53.4–63.3)
|
62.3
|
(57.2–67.1)
|
|
New Mexico***
|
58.6
|
(52.9–64.0)
|
55.3
|
(49.5–61.0)
|
58.3
|
(52.3–64.1)
|
56.8
|
(50.2–63.2)
|
52.1
|
(46.0–58.1)
|
53.6
|
(46.3–60.8)
|
—
|
—
|
|
New York***,§§§
|
37.3
|
(30.7–44.3)
|
43.4
|
(36.4–50.6)
|
38.4
|
(31.3–45.9)
|
44.7
|
(37.6–52.1)
|
45.2
|
(38.1–52.5)
|
44.5
|
(37.1–52.1)
|
45.3
|
(34.6–56.4)
|
|
New York City***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
46.2
|
(34.8–58.0)
|
60.9
|
(49.4–71.2)
|
63.0
|
(52.9–72.1)
|
|
North Carolina***
|
44.5
|
(38.4–50.8)
|
43.4
|
(36.8–50.3)
|
50.5
|
(43.9–57.1)
|
45.4
|
(38.7–52.3)
|
45.1
|
(39.0–51.3)
|
42.4
|
(34.5–50.7)
|
—
|
—
|
|
North Dakota
|
—
|
—
|
—
|
—
|
43.1
|
(37.0–49.3)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Ohio
|
39.7
|
(33.5–46.2)
|
36.9
|
(30.8–43.4)
|
34.8
|
(28.6–41.7)
|
41.0
|
(34.7–47.7)
|
—
|
—
|
33.3
|
(27.4–39.8)
|
45.0
|
(38.8–51.3)
|
|
Oklahoma
|
46.4
|
(39.6–53.4)
|
37.6
|
(31.4–44.3)
|
38.2
|
(32.0–44.7)
|
44.7
|
(38.0–51.7)
|
39.2
|
(32.8–46.0)
|
38.0
|
(32.1–44.2)
|
39.0
|
(32.6–45.8)
|
|
Oregon
|
—
|
—
|
—
|
—
|
—
|
—
|
43.5
|
(34.3–53.3)
|
42.6
|
(34.7–50.9)
|
37.3
|
(29.8–45.5)
|
49.4
|
(41.0–57.7)
|
|
Pennsylvania***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Rhode Island
|
—
|
—
|
—
|
—
|
38.0
|
(31.5–45.0)
|
51.9
|
(45.1–58.6)
|
49.0
|
(42.4–55.6)
|
46.7
|
(40.1–53.5)
|
44.3
|
(37.7–51.1)
|
|
South Carolina***
|
45.6
|
(37.5–53.9)
|
43.3
|
(35.1–52.0)
|
44.8
|
(35.6–54.5)
|
49.6
|
(40.7–58.6)
|
42.7
|
(34.6–51.2)
|
42.8
|
(34.9–51.1)
|
55.0
|
(43.7–65.7)
|
|
South Dakota Tribal***,¶¶¶
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Tennessee
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Texas***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Utah
|
49.8
|
(40.7–58.9)
|
45.6
|
(38.3–53.1)
|
49.7
|
(40.5–58.9)
|
65.8
|
(56.4–74.0)
|
47.0
|
(40.5–53.5)
|
51.3
|
(44.1–58.3)
|
50.3
|
(43.8–56.8)
|
|
Vermont***
|
—
|
—
|
42.9
|
(38.2–47.7)
|
37.5
|
(32.3–43.0)
|
39.1
|
(33.7–44.7)
|
39.9
|
(34.4–45.6)
|
39.2
|
(33.5–45.2)
|
40.6
|
(34.7–46.6)
|
|
Washington
|
49.7
|
(41.4–57.9)
|
54.8
|
(46.2–63.2)
|
49.7
|
(41.2–58.1)
|
54.1
|
(45.7–62.2)
|
47.9
|
(39.7–56.2)
|
50.5
|
(41.8–59.1)
|
43.3
|
(35.5–51.4)
|
|
West Virginia***
|
32.7
|
(27.7–38.1)
|
32.8
|
(27.9–38.2)
|
32.8
|
(27.9–38.1)
|
30.2
|
(25.4–35.4)
|
28.1
|
(21.8–35.4)
|
30.2
|
(25.7–35.1)
|
29.9
|
(25.4–34.9)
|
|
Wisconsin
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Wyoming
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Site
|
Year
|
p value§
|
Annual
percentage
point
change¶
|
|
2007
(N = 31 sites)
|
2008
(N = 29 sites)
|
2009
(N = 29 sites)
|
2010
(N = 27 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites**
|
44.9
|
(43.2–46.6)
|
44.5
|
(42.8–46.1)
|
51.7
|
(50.0–53.4)
|
54.3
|
(52.4–56.1)
|
0.02††
|
0.3
|
|
10 PRAMS sites§§
|
45.1
|
(42.6–47.6)
|
42.1
|
(39.5–44.6)
|
51.2
|
(48.8–53.7)
|
50.7
|
(48.3–53.2)
|
0.07
|
NA
|
|
Alabama
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.62
|
NA
|
|
Alaska
|
43.8
|
(38.1–49.7)
|
46.0
|
(39.9–52.4)
|
52.9
|
(47.2–58.4)
|
50.3
|
(44.1–56.6)
|
0.96
|
NA
|
|
Arkansas
|
39.9
|
(34.8–45.3)
|
23.3
|
(18.9–28.4)
|
40.9
|
(34.4–47.6)
|
43.8
|
(38.2–49.7)
|
0.15
|
NA
|
|
Colorado
|
49.6
|
(42.9–56.4)
|
51.9
|
(44.6–59.1)
|
61.4
|
(55.2–67.3)
|
61.7
|
(55.2–67.8)
|
0.43
|
NA
|
|
Delaware***
|
39.9
|
(31.8–48.7)
|
46.1
|
(40.4–51.9)
|
42.3
|
(36.9–47.9)
|
48.9
|
(42.9–54.9)
|
0.05
|
NA
|
|
Florida***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.31
|
NA
|
|
Georgia***
|
54.8
|
(41.5–67.6)
|
52.8
|
(41.7–63.6)
|
56.9
|
(45.7–67.4)
|
61.0
|
(50.0–71.0)
|
0.15
|
NA
|
|
Hawaii
|
58.1
|
(52.6–63.4)
|
54.8
|
(49.1–60.3)
|
57.8
|
(51.2–64.2)
|
62.6
|
(55.6–69.1)
|
0.60
|
NA
|
|
Illinois
|
45.8
|
(40.2–51.5)
|
50.1
|
(44.2–56.1)
|
56.5
|
(50.6–62.2)
|
—
|
—
|
0.02††
|
0.9
|
|
Louisiana***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.01††
|
-2.2
|
|
Maine
|
37.1
|
(31.3–43.3)
|
39.8
|
(34.0–45.9)
|
42.6
|
(36.9–48.4)
|
45.7
|
(39.4–52.1)
|
0.16
|
NA
|
|
Maryland***
|
47.8
|
(38.7–57.1)
|
43.7
|
(35.2–52.5)
|
49.0
|
(39.9–58.2)
|
52.1
|
(43.0–61.1)
|
0.12
|
NA
|
|
Massachusetts
|
42.8
|
(33.5–52.6)
|
50.7
|
(41.9–59.4)
|
49.2
|
(41.0–57.4)
|
62.0
|
(52.6–70.5)
|
0.02††
|
10.4
|
|
Michigan***
|
48.9
|
(43.3–54.7)
|
41.1
|
(35.5–47.0)
|
47.4
|
(42.2–52.5)
|
48.7
|
(43.2–54.3)
|
0.02††
|
1.1
|
|
Minnesota***
|
39.8
|
(34.5–45.2)
|
47.8
|
(41.8–53.9)
|
46.4
|
(41.0–51.9)
|
47.3
|
(41.4–53.3)
|
0.40
|
NA
|
|
Mississippi***
|
—
|
—
|
40.3
|
(34.0–46.9)
|
44.4
|
(38.6–50.3)
|
—
|
—
|
0.43
|
NA
|
|
Missouri
|
42.1
|
(36.5–47.9)
|
—
|
—
|
46.6
|
(41.1–52.3)
|
49.7
|
(44.4–55.1)
|
0.44
|
NA
|
|
Montana
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Nebraska
|
47.7
|
(41.5–54.0)
|
38.9
|
(32.5–45.8)
|
53.6
|
(48.3–58.8)
|
51.0
|
(45.3–56.7)
|
0.17
|
NA
|
|
New Jersey***
|
56.2
|
(50.0–62.2)
|
57.1
|
(50.8–63.2)
|
66.4
|
(61.1–71.3)
|
63.6
|
(58.0–68.9)
|
0.02††
|
1.5
|
|
New Mexico***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.17
|
NA
|
|
New York***,§§§
|
41.6
|
(34.0–49.6)
|
43.9
|
(36.2–52.0)
|
—
|
—
|
54.1
|
(45.9–62.0)
|
0.24
|
NA
|
|
New York City***
|
58.1
|
(47.9–67.7)
|
—
|
—
|
—
|
—
|
74.6
|
(64.5–82.7)
|
0.21
|
NA
|
|
North Carolina***
|
38.0
|
(32.0–44.4)
|
44.5
|
(38.2–51.0)
|
—
|
—
|
—
|
—
|
0.20
|
NA
|
|
North Dakota
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Ohio
|
36.7
|
(30.4–43.6)
|
41.5
|
(35.5–47.9)
|
41.2
|
(35.2–47.4)
|
47.2
|
(40.5–54.0)
|
0.37
|
NA
|
|
Oklahoma
|
43.6
|
(37.5–49.9)
|
47.1
|
(40.5–53.8)
|
46.9
|
(40.6–53.3)
|
42.7
|
(36.3–49.4)
|
0.51
|
NA
|
|
Oregon
|
50.9
|
(42.1–59.6)
|
43.9
|
(34.4–53.8)
|
54.4
|
(46.3–62.2)
|
61.9
|
(54.9–68.5)
|
0.22
|
NA
|
|
Pennsylvania***
|
44.6
|
(34.6–55.1)
|
44.8
|
(38.7–51.0)
|
50.6
|
(43.8–57.2)
|
48.6
|
(42.0–55.4)
|
0.79
|
NA
|
|
Rhode Island
|
45.9
|
(39.3–52.7)
|
52.9
|
(45.9–59.8)
|
57.8
|
(50.7–64.6)
|
55.9
|
(48.8–62.7)
|
0.18
|
NA
|
|
South Carolina***
|
43.8
|
(35.0–52.9)
|
—
|
—
|
—
|
—
|
—
|
—
|
0.86
|
NA
|
|
South Dakota Tribal***,¶¶¶
|
40.2
|
(36.8–43.8)
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Tennessee
|
—
|
—
|
35.6
|
(27.9–44.2)
|
35.7
|
(28.3–43.9)
|
—
|
—
|
†††
|
NA
|
|
Texas***
|
—
|
—
|
—
|
—
|
65.1
|
(58.5–71.1)
|
62.9
|
(56.2–69.2)
|
†††
|
NA
|
|
Utah
|
50.4
|
(42.7–58.2)
|
51.0
|
(43.7–58.2)
|
54.9
|
(47.5–62.0)
|
62.3
|
(54.6–69.4)
|
0.69
|
NA
|
|
Vermont***
|
41.0
|
(35.6–46.6)
|
39.7
|
(34.2–45.4)
|
46.8
|
(41.5–52.3)
|
42.8
|
(37.4–48.3)
|
0.75
|
NA
|
|
Washington
|
51.9
|
(43.5–60.3)
|
44.9
|
(37.2–52.8)
|
59.1
|
(51.4–66.3)
|
57.1
|
(49.1–64.7)
|
0.16
|
NA
|
|
West Virginia***
|
25.9
|
(21.6–30.8)
|
27.0
|
(23.0–31.4)
|
32.8
|
(28.7–37.3)
|
34.3
|
(30.0–39.0)
|
0.01††
|
-0.9
|
|
Wisconsin
|
42.1
|
(35.4–49.0)
|
43.2
|
(35.5–51.2)
|
49.1
|
(41.5–56.7)
|
—
|
—
|
0.83
|
NA
|
|
Wyoming
|
46.5
|
(39.8–53.2)
|
44.1
|
(37.1–51.4)
|
50.4
|
(43.2–57.7)
|
50.5
|
(43.6–57.4)
|
0.75
|
NA
|
|
Site
|
Year
|
|
2000
(N = 19 sites)
|
2001
(N = 22 sites)
|
2002
(N = 27 sites)
|
2003
(N = 27 sites)
|
2004
(N = 27 sites)
|
2005
(N = 26 sites)
|
2006
(N = 24 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites**
|
18.9
|
(18.2–19.6)
|
19.0
|
(18.3–19.7)
|
18.2
|
(17.6–18.8)
|
18.9
|
(18.3–19.5)
|
18.2
|
(17.6–18.8)
|
17.1
|
(16.5–17.7)
|
16.5
|
(15.9–17.1)
|
|
10 PRAMS sites§§
|
18.6
|
(17.7–19.6)
|
19.1
|
(18.1–20.0)
|
18.4
|
(17.5–19.4)
|
17.9
|
(17.0–18.8)
|
18.4
|
(17.5–19.3)
|
18.2
|
(17.3–19.1)
|
18.0
|
(17.1–19.0)
|
|
Alabama
|
19.5
|
(17.2–22.1)
|
22.4
|
(20.0–25.0)
|
19.7
|
(17.5–22.2)
|
17.8
|
(15.5–20.4)
|
—¶¶
|
—
|
—
|
—
|
—
|
—
|
|
Alaska
|
24.4
|
(22.0–26.9)
|
20.4
|
(18.3–22.6)
|
24.3
|
(22.1–26.6)
|
22.1
|
(19.9–24.4)
|
23.6
|
(21.0–26.4)
|
20.7
|
(18.3–23.3)
|
20.5
|
(18.1–23.1)
|
|
Arkansas
|
25.0
|
(22.1–28.2)
|
25.9
|
(23.4–28.6)
|
25.3
|
(22.8–28.0)
|
26.1
|
(23.5–28.8)
|
28.6
|
(26.0–31.2)
|
27.5
|
(25.1–30.1)
|
25.6
|
(23.2–28.2)
|
|
Colorado
|
15.0
|
(13.2–17.0)
|
15.9
|
(14.0–18.1)
|
14.0
|
(12.3–15.9)
|
14.0
|
(12.2–15.9)
|
15.3
|
(13.2–17.7)
|
14.8
|
(12.6–17.2)
|
14.9
|
(12.8–17.3)
|
|
Delaware***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Florida***
|
14.8
|
(12.6–17.3)
|
14.7
|
(12.5–17.1)
|
14.3
|
(12.1–16.8)
|
16.7
|
(14.4–19.4)
|
16.1
|
(13.8–18.6)
|
12.8
|
(11.0–15.0)
|
—
|
—
|
|
Georgia***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
14.8
|
(12.4–17.6)
|
15.4
|
(13.1–18.0)
|
14.0
|
(11.9–16.4)
|
|
Hawaii
|
13.7
|
(12.3–15.2)
|
15.0
|
(13.5–16.5)
|
13.0
|
(11.4–14.9)
|
14.8
|
(13.1–16.8)
|
13.1
|
(11.7–14.7)
|
14.1
|
(12.5–15.8)
|
14.3
|
(12.6–16.2)
|
|
Illinois
|
16.6
|
(14.9–18.4)
|
17.2
|
(15.5–19.0)
|
16.8
|
(15.1–18.7)
|
17.8
|
(15.9–20.0)
|
17.1
|
(15.4–19.1)
|
14.7
|
(12.9–16.6)
|
16.2
|
(14.4–18.3)
|
|
Louisiana***
|
18.7
|
(16.8–20.8)
|
20.5
|
(18.4–22.6)
|
19.2
|
(17.2–21.5)
|
21.9
|
(19.6–24.3)
|
23.4
|
(21.1–25.8)
|
—
|
—
|
—
|
—
|
|
Maine
|
23.8
|
(21.1–26.8)
|
22.7
|
(20.0–25.6)
|
21.6
|
(18.9–24.6)
|
20.8
|
(18.1–23.7)
|
24.5
|
(21.7–27.5)
|
23.4
|
(20.7–26.4)
|
20.9
|
(18.2–23.9)
|
|
Maryland***
|
—
|
—
|
14.6
|
(11.9–17.6)
|
12.8
|
(10.4–15.7)
|
16.4
|
(13.7–19.6)
|
16.3
|
(13.5–19.4)
|
13.7
|
(11.0–16.8)
|
11.8
|
(9.5–14.5)
|
|
Massachusetts
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Michigan***
|
—
|
—
|
24.3
|
(21.1–27.9)
|
23.4
|
(21.1–26.0)
|
22.7
|
(20.4–25.2)
|
25.6
|
(22.9–28.5)
|
22.4
|
(20.0–25.1)
|
26.3
|
(23.3–29.5)
|
|
Minnesota***
|
—
|
—
|
—
|
—
|
19.9
|
(17.1–23.0)
|
19.4
|
(17.1–22.0)
|
21.4
|
(18.9–24.3)
|
21.3
|
(18.8–24.1)
|
19.0
|
(17.0–21.1)
|
|
Mississippi***
|
—
|
—
|
—
|
—
|
—
|
—
|
20.0
|
(17.5–22.7)
|
17.7
|
(15.3–20.4)
|
—
|
—
|
21.1
|
(18.1–24.6)
|
|
Missouri
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Montana
|
—
|
—
|
—
|
—
|
20.8
|
(18.4–23.5)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Nebraska
|
19.4
|
(17.3–21.7)
|
21.4
|
(19.5–23.4)
|
19.9
|
(17.7–22.3)
|
18.8
|
(16.7–21.1)
|
20.8
|
(18.6–23.3)
|
20.1
|
(17.9–22.4)
|
19.2
|
(16.9–21.8)
|
|
New Jersey***
|
—
|
—
|
—
|
—
|
13.1
|
(11.1–15.3)
|
12.2
|
(11.0–13.6)
|
12.0
|
(10.9–13.3)
|
11.5
|
(10.3–12.8)
|
10.1
|
(9.0–11.3)
|
|
New Mexico***
|
16.0
|
(14.2–18.0)
|
16.2
|
(14.2–18.3)
|
13.6
|
(11.9–15.5)
|
12.5
|
(10.8–14.5)
|
14.5
|
(12.7–16.5)
|
13.1
|
(11.1–15.4)
|
—
|
—
|
|
New York***,§§§
|
22.4
|
(19.5–25.6)
|
20.6
|
(17.9–23.6)
|
19.3
|
(16.6–22.3)
|
19.2
|
(16.5–22.3)
|
21.6
|
(18.6–25.0)
|
17.5
|
(14.9–20.5)
|
16.9
|
(13.3–21.2)
|
|
New York City***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
11.7
|
(9.1–14.9)
|
8.8
|
(6.8–11.3)
|
6.8
|
(5.4–8.6)
|
|
North Carolina***
|
20.1
|
(17.7–22.6)
|
17.6
|
(15.4–20.2)
|
17.8
|
(15.6–20.3)
|
20.5
|
(18.0–23.3)
|
20.7
|
(18.2–23.4)
|
16.9
|
(14.2–20.0)
|
—
|
—
|
|
North Dakota
|
—
|
—
|
—
|
—
|
21.8
|
(19.4–24.5)
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Ohio
|
24.2
|
(21.4–27.2)
|
23.8
|
(21.1–26.7)
|
22.6
|
(19.8–25.7)
|
28.0
|
(24.9–31.4)
|
—
|
—
|
27.4
|
(24.2–30.8)
|
22.5
|
(19.8–25.5)
|
|
Oklahoma
|
25.8
|
(22.6–29.1)
|
27.2
|
(24.0–30.7)
|
27.0
|
(23.9–30.3)
|
24.7
|
(21.7–28.0)
|
26.3
|
(23.1–29.7)
|
26.3
|
(23.2–29.5)
|
25.0
|
(21.9–28.4)
|
|
Oregon
|
—
|
—
|
—
|
—
|
—
|
—
|
15.5
|
(12.7–18.9)
|
17.8
|
(15.0–21.0)
|
15.9
|
(13.3–18.9)
|
15.0
|
(12.5–18.0)
|
|
Pennsylvania***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Rhode Island
|
—
|
—
|
—
|
—
|
17.0
|
(14.7–19.5)
|
15.1
|
(13.1–17.5)
|
16.6
|
(14.4–19.0)
|
15.8
|
(13.6–18.2)
|
18.9
|
(16.4–21.6)
|
|
South Carolina***
|
18.6
|
(15.8–21.8)
|
20.3
|
(17.3–23.7)
|
17.8
|
(14.8–21.3)
|
20.1
|
(16.9–23.7)
|
19.2
|
(16.2–22.7)
|
21.5
|
(18.3–25.1)
|
16.4
|
(12.7–21.0)
|
|
South Dakota Tribal***,¶¶¶
|
|
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Tennessee
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Texas***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Utah
|
9.5
|
(7.7–11.6)
|
10.1
|
(8.6–11.9)
|
9.0
|
(7.2–11.1)
|
7.6
|
(6.1–9.5)
|
8.7
|
(7.5–10.1)
|
7.3
|
(6.2–8.5)
|
8.3
|
(7.2–9.6)
|
|
Vermont***
|
—
|
—
|
22.2
|
(20.1–24.4)
|
21.5
|
(19.2–24.1)
|
17.6
|
(15.6–19.9)
|
22.8
|
(20.3–25.5)
|
21.0
|
(18.5–23.6)
|
18.4
|
(16.2–20.9)
|
|
Washington
|
16.0
|
(13.5–18.9)
|
14.9
|
(12.4–17.8)
|
15.7
|
(13.1–18.8)
|
15.5
|
(13.0–18.4)
|
14.6
|
(12.1–17.3)
|
13.0
|
(10.7–15.6)
|
14.9
|
(12.5–17.8)
|
|
West Virginia***
|
31.6
|
(28.6–34.7)
|
34.3
|
(31.2–37.6)
|
33.7
|
(30.6–37.0)
|
33.6
|
(30.5–36.9)
|
33.5
|
(29.2–38.1)
|
39.3
|
(36.0–42.7)
|
35.0
|
(31.8–38.2)
|
|
Wisconsin
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Wyoming
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
|
Site
|
Year
|
p value§
|
Annual
percentage
point
change¶
|
|
2007
(N = 31 sites)
|
2008
(N = 29 sites)
|
2009
(N = 29 sites)
|
2010
(N = 27 sites)
|
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
%
|
(95% CI)
|
|
Total sites**
|
17.2
|
(16.6–17.8)
|
17.6
|
(17.0–18.2)
|
17.6
|
(17.0–18.3)
|
15.9
|
(15.3–16.5)
|
<0.01††
|
-0.2
|
|
10 PRAMS sites§§
|
18.2
|
(17.3–19.2)
|
16.9
|
(16.1–17.8)
|
17.2
|
(16.3–18.1)
|
17.2
|
(16.3–18.1)
|
<0.01††
|
-0.2
|
|
Alabama
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.18
|
NA
|
|
Alaska
|
20.3
|
(18.0–22.9)
|
21.7
|
(19.1–24.5)
|
21.4
|
(19.0–24.1)
|
24.1
|
(21.1–27.3)
|
0.44
|
NA
|
|
Arkansas
|
25.4
|
(22.9–28.1)
|
26.9
|
(24.2–29.8)
|
24.0
|
(20.9–27.4)
|
24.8
|
(22.1–27.8)
|
0.58
|
NA
|
|
Colorado
|
14.6
|
(12.6–17.0)
|
11.3
|
(9.5–13.2)
|
12.8
|
(11.0–14.9)
|
12.8
|
(11.0–15.0)
|
<0.01††
|
-0.3
|
|
Delaware***
|
16.7
|
(13.9–19.8)
|
18.9
|
(16.8–21.2)
|
22.4
|
(20.0–25.0)
|
17.5
|
(15.3–19.8)
|
0.44
|
NA
|
|
Florida***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.69
|
NA
|
|
Georgia***
|
13.1
|
(9.8–17.3)
|
12.9
|
(10.0–16.3)
|
15.3
|
(12.1–19.3)
|
15.6
|
(12.4–19.6)
|
0.87
|
NA
|
|
Hawaii
|
13.3
|
(11.7–15.0)
|
12.4
|
(10.9–14.1)
|
13.4
|
(11.4–15.7)
|
12.7
|
(10.7–15.0)
|
0.12
|
NA
|
|
Illinois
|
14.7
|
(13.0–16.6)
|
14.2
|
(12.5–16.1)
|
14.6
|
(12.8–16.5)
|
—
|
—
|
<0.01††
|
-0.3
|
|
Louisiana***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
<0.01††
|
0.9
|
|
Maine
|
23.5
|
(20.7–26.6)
|
25.3
|
(22.4–28.4)
|
26.1
|
(23.1–29.3)
|
24.8
|
(21.8–28.1)
|
0.05††
|
0.2
|
|
Maryland***
|
13.3
|
(10.8–16.2)
|
14.1
|
(11.7–17.0)
|
13.4
|
(10.9–16.3)
|
13.7
|
(11.1–16.7)
|
0.30
|
NA
|
|
Massachusetts
|
11.6
|
(9.4–14.3)
|
13.5
|
(11.1–16.4)
|
14.9
|
(12.3–17.8)
|
10.9
|
(8.7–13.5)
|
0.89
|
NA
|
|
Michigan***
|
22.2
|
(19.8–24.8)
|
22.5
|
(20.1–25.0)
|
24.8
|
(22.4–27.4)
|
23.3
|
(20.8–26.1)
|
0.81
|
NA
|
|
Minnesota***
|
19.0
|
(17.0–21.3)
|
15.3
|
(13.4–17.5)
|
18.5
|
(16.4–20.8)
|
18.1
|
(15.8–20.5)
|
<0.01††
|
-0.4
|
|
Mississippi***
|
—
|
—
|
22.5
|
(19.8–25.4)
|
21.3
|
(18.7–24.0)
|
—
|
—
|
0.05††
|
0.4
|
|
Missouri
|
25.9
|
(23.1–28.8)
|
—
|
—
|
26.1
|
(23.3–29.0)
|
25.3
|
(22.7–28.1)
|
0.83
|
NA
|
|
Montana
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Nebraska
|
20.2
|
(17.7–22.9)
|
18.7
|
(16.3–21.4)
|
20.1
|
(17.9–22.4)
|
16.9
|
(14.9–19.2)
|
0.09
|
NA
|
|
New Jersey***
|
9.6
|
(8.4–10.9)
|
11.2
|
(9.8–12.8)
|
12.3
|
(10.8–13.9)
|
10.5
|
(9.2–12.1)
|
0.05††
|
-0.3
|
|
New Mexico***
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
0.01††
|
-0.6
|
|
New York***,§§§
|
17.9
|
(15.2–21.0)
|
16.1
|
(13.6–19.0)
|
—
|
—
|
17.4
|
(14.5–20.8)
|
<0.01††
|
-0.5
|
|
New York City***
|
8.8
|
(7.1–11.0)
|
—
|
—
|
—
|
—
|
4.1
|
(3.1–5.6)
|
<0.01††
|
-2.0
|
|
North Carolina***
|
17.9
|
(15.6–20.4)
|
17.5
|
(15.3–19.9)
|
—
|
—
|
—
|
—
|
0.21
|
NA
|
|
North Dakota
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Ohio
|
22.9
|
(20.0–26.1)
|
24.9
|
(21.9–28.0)
|
26.7
|
(23.6–30.1)
|
22.0
|
(19.0–25.3)
|
0.81
|
NA
|
|
Oklahoma
|
29.6
|
(26.2–33.2)
|
23.9
|
(20.9–27.2)
|
26.1
|
(23.0–29.5)
|
26.1
|
(22.8–29.6)
|
0.85
|
NA
|
|
Oregon
|
13.2
|
(10.8–16.2)
|
13.7
|
(11.0–17.0)
|
16.6
|
(13.8–19.8)
|
16.7
|
(14.2–19.5)
|
0.71
|
NA
|
|
Pennsylvania***
|
22.8
|
(18.6–27.6)
|
22.0
|
(19.4–24.9)
|
20.2
|
(17.5–23.1)
|
21.7
|
(18.9–24.9)
|
0.59
|
NA
|
|
Rhode Island
|
16.3
|
(14.0–18.8)
|
15.0
|
(12.9–17.5)
|
14.9
|
(12.7–17.4)
|
14.8
|
(12.6–17.3)
|
0.21
|
NA
|
|
South Carolina***
|
16.2
|
(13.3–19.7)
|
—
|
—
|
—
|
—
|
—
|
—
|
0.28
|
NA
|
|
South Dakota Tribal***,¶¶¶
|
45.1
|
(42.6–47.7)
|
—
|
—
|
—
|
—
|
—
|
—
|
†††
|
NA
|
|
Tennessee
|
—
|
—
|
26.0
|
(22.1–30.4)
|
27.2
|
(23.2–31.7)
|
—
|
—
|
†††
|
NA
|
|
Texas***
|
—
|
—
|
—
|
—
|
12.7
|
(10.9–14.7)
|
11.6
|
(9.9–13.5)
|
†††
|
NA
|
|
Utah
|
7.6
|
(6.4–9.0)
|
7.1
|
(6.0–8.3)
|
8.0
|
(6.7–9.5)
|
7.2
|
(5.9–8.6)
|
<0.01††
|
-0.4
|
|
Vermont***
|
21.6
|
(19.3–24.2)
|
22.7
|
(20.2–25.4)
|
21.9
|
(19.4–24.6)
|
21.0
|
(18.6–23.7)
|
0.70
|
NA
|
|
Washington
|
13.0
|
(10.8–15.7)
|
13.9
|
(11.7–16.5)
|
11.9
|
(9.7–14.4)
|
12.7
|
(10.5–15.2)
|
<0.01††
|
-0.4
|
|
West Virginia***
|
36.6
|
(33.5–39.9)
|
34.9
|
(32.1–37.7)
|
35.6
|
(32.8–38.5)
|
37.5
|
(34.5–40.7)
|
0.01††
|
0.2
|
|
Wisconsin
|
21.9
|
(19.0–25.1)
|
18.6
|
(15.9–21.8)
|
16.1
|
(13.4–19.1)
|
—
|
—
|
0.01††
|
-2.4
|
|
Wyoming
|
24.5
|
(21.5–27.8)
|
20.9
|
(18.0–24.2)
|
22.2
|
(19.0–25.8)
|
18.8
|
(16.1–21.8)
|
0.02††
|
-1.2
|




