Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Very High Blood Lead Levels Among Adults — United States, 2002–2011
Please note: An erratum has been published for this article. To view the erratum, please click here.
Over the past several decades there has been a remarkable reduction in environmental sources of lead, improved protection from occupational lead exposure, and an overall decreasing trend in the prevalence of elevated blood lead levels (BLLs) in U.S. adults. As a result, the U.S. national BLL geometric mean among adults was 1.2 µg/dL during 2009–2010 (1). Nonetheless, lead exposures continue to occur at unacceptable levels (2). Current research continues to find that BLLs previously considered harmless can have harmful effects in adults, such as decreased renal function and increased risk for hypertension and essential tremor at BLLs <10 µg/dL (3–5). CDC has designated 10 µg/dL as the reference BLL for adults; levels ≥10 µg/dL are considered elevated (2). CDC's Adult Blood Lead Epidemiology and Surveillance (ABLES) program tracks elevated BLLs among adults in the United States (2). In contrast to the CDC reference level, prevailing Occupational Safety and Health Administration (OSHA) lead standards allow workers removed from lead exposure to return to lead work when their BLL falls below 40 µg/dL (6). During 2002–2011, ABLES identified 11,536 adults with very high BLLs (≥40 µg/dL). Persistent very high BLLs (≥40 µg/dL in ≥2 years) were found among 2,210 (19%) of these adults. Occupational exposures accounted for 7,076 adults with very high BLLs (91% of adults with known exposure source) and 1,496 adults with persistent very high BLLs. Adverse health effects associated with very high BLLs (4,5,7) underscore the need for increased efforts to prevent lead exposure at workplaces and in communities.
Forty-one states participated in the ABLES program in 2011.* These states received adult BLL data from laboratories and physicians through mandatory reporting. Adults were defined as persons aged ≥16 years at the time of BLL testing. Each state ABLES program assigned a unique identifier to each adult to protect individual privacy while permitting longitudinal analyses (2). For this analysis, a BLL ≥40 µg/dL was defined as a very high BLL. A very high BLL measured over a period ≥2 years was defined as a persistent very high BLL. The number of adults with very high BLLs and the number with persistent very high BLLs during 2002–2011 were counted. Persistent very high BLLs can result in spontaneous abortion, reduced newborn birthweight, neurocognitive deficits, sperm abnormalities, subclinical peripheral neuropathy, hypertension, anemia, kidney dysfunction, and nonspecific symptoms (4,5). As part of their regular activities, and to the extent resources allow, state ABLES programs 1) investigate the circumstances associated with reports of elevated BLLs; 2) contact health-care providers, workers, and employers to gather industry and occupation data and additional exposure information and provide information and educational materials; and 3) refer employers in occupational cases to OSHA offices for technical assistance or enforcement of the lead standards.
From 2002 to 2011, a total of 11,536 adults had very high BLLs among the 1,201,669 adults reported to the ABLES program during this period. Among these adults, 2,210 (19%) had persistent very high BLLs, 1,487 (13%) had BLLs ≥60 µg/dL, and 96 had BLLs ≥60 µg/dL for ≥2 years (Table 1). A total of 7,076 adults with very high BLLs (91% of adults with known exposure source) were exposed at work (Table 2), and 1,496 of these had persistent very high BLLs (93% of adults with known exposure source). These 7,076 workers were predominantly employed in the manufacturing, construction, services, or mining sectors. Within this group, 49% of the workers were employed in three subsectors (i.e., battery manufacturing, nonferrous metal production and processing, and painting and wall covering contractors). Shooting firearms; remodeling, renovating, or painting; and using lead-containing alternative medicines (Table 2) were the most common sources for nonoccupational very high BLLs. The following four case histories illustrate the persistent problem of adults with very high BLLs in the United States (Figure).
Case Histories
Worker A. Worker A is a man aged 48 years who was working for a bridge painting firm and was responsible for recycling grit and steel shot from sandblasting operations. His primary protection from lead exposure was an air-supplied sandblasting hood. This worker had BLLs of 67 µg/dL in May and June of 2010. He was removed from all work and received chelation treatments (therapy to remove heavy metals from the body). His BLL dropped to 42 µg/dL in July and to 26 µg/dL in September 2010. At last contact in February 2011, he continued to be removed from work per physician orders.
Worker B. Worker B is a painter for a small construction company, aged 46 years, who, in December 2007, was seen in a hospital emergency department because of severe stomach pain. His BLL was 143 µg/dL; he was given a chelation treatment and was followed at an occupational health clinic. His last BLL on record in February 2010 was 13 µg/dL. At the time of initial testing, this worker was scraping paint from a house that was >100 years old. He used no respirator and wore no protective clothing except for gloves. He was not informed about lead hazards. His employer did not provide laundry services or disposable clothing. No other source of lead exposure was identified.
Worker C. Worker C is a man aged 45 years who began working for a battery manufacturing company in May 2000. He worked in maintenance and was responsible for cleaning under lead pots. He did not use a respirator as instructed by his employer because of the heat in the factory. His first BLL was 25 µg/dL in March 2001, and by August 2002 his BLL was 60 µg/dL. Because of the very high BLL, the company moved him into a job with low likelihood of lead exposure. After his BLL dropped below 40 µg/dL in November 2002, he was reassigned to job duties with high likelihood of lead exposure. When his BLL rose to 40 µg/dL again in April 2003, the company issued him a full-face respirator and required him to use it. He was also instructed to shower at the end of the day and for breaks and lunch. He later transferred into jobs at the plant with lower lead exposures and his BLL continued to drop. His most recent BLL in August 2011 was 14 µg/dL.
Adult D. Adult D is a man aged 60 years with a BLL of 84 µg/dL in March 2009 who had no known occupational exposure. His known exposures were target shooting at an indoor shooting range and casting bullets. He was given a chelation treatment in April 2009. Approximately 100 BLLs analyzed through June 2012 ranged from 6 µg/dL to 84 µg/dL, with a mean of 28 µg/dL. He and his physician were informed about the detrimental effects of lead and how to limit his exposure, but the patient continues his two hobbies.
Reported by
Kathryn Kirschner, Indiana Univ. Kathy Leinenkugel, MPA, Div of Environmental Health, Iowa Dept of Public Health. Mike Makowski, MPH, Div of Environmental Health Epidemiology, Pennsylvania Dept of Health. Alicia M. Fletcher, MPH, Bur of Occupational Health and Injury Prevention, New York State Dept of Health. Carol R. Braun, Bur of Environmental Epidemiology, Missouri Dept of Health and Senior Svcs. Walter A. Alarcon, MD, Marie H. Sweeney, PhD, Geoffrey M. Calvert, MD, Div of Surveillance, Hazard Evaluations, and Field Studies, National Institute for Occupational Safety and Health, CDC. Corresponding contributor: Walter A. Alarcon, wda7@cdc.gov, 513-841-4451.
Editorial Note
Reducing lead exposures at work and in the community is essential to avoid adverse health effects in humans. Reducing by 10% the rate of persons who have elevated BLLs (i.e., BLLs ≥10 µg/dL) from work exposures is a Healthy People 2020 objective (OHS-7) (8). The 2010 baseline rate for BLLs ≥10 µg/dL is 26.4 adults per 100,000 employed adults (2). Reducing adverse health effects resulting from lead exposures requires 1) adherence to engineering controls and safe work practices; 2) BLL testing and management of elevated BLLs according to the most current medical guidelines and recommendations; and 3) education in the workplace and community (4–7,9). OSHA lead standards give the examining physician broad flexibility to tailor special protective procedures to the needs of individual employees (6). Therefore, the most current guidelines for management of lead-exposed adults (4,5,7) should be implemented by the medical community at the current CDC reference BLL of 10 µg/dL (2), including consideration of removal from lead exposure at lower levels than the current OSHA lead standards require. Increasing the number and timeliness of referrals to OSHA of workplaces identified by state ABLES programs fosters prompt intervention and mitigation of lead exposure hazards.
The findings of this report demonstrate that many adults in the United States continue to have very high BLLs. The fact that some adults had persistent very high BLLs is of grave concern. These adults were chronically exposed to lead above BLLs known to cause neurologic, cardiovascular, reproductive, hematologic, and kidney adverse effects (3–5). The risks for adverse chronic health effects are even higher if the exposure is maintained for many years (4,5,7).
The findings in this report are subject to at least three limitations, all of which suggest that ABLES underestimates the number of adults with elevated BLLs. First, employers might not provide BLL testing to all lead-exposed workers as required by OSHA regulations (10). Second, nonoccupationally exposed adults might not be tested. Finally, some laboratories might not report all tests as required by state laws or regulations (Susan Payne, California Department of Public Health, personal communication, June 18, 2012).
Possible factors contributing to the persistence of very high BLLs include 1) prevailing OSHA lead standards require medical removal from lead exposures only after a construction worker's BLL reaches or exceeds 50 µg/dL or a general industry worker's BLL reaches or exceeds 60 µg/dL; 2) examining physicians rarely recommend more stringent worker protections, which the OSHA lead standards allow but do not require; 3) some employers fail to implement appropriate engineering protections and workplace controls; 4) some adults fail to comply with safe practices and behaviors; and 5) state ABLES programs do not always have the resources to investigate and refer to OSHA all cases with very high BLLs.
Very high BLLs continue to be documented in adults in the United States. Actions that might decrease the number of adults with harmful BLLs include 1) increased employer efforts to reduce work-related lead exposure (6,9) and to comply with current guidance (4,7) for testing and managing lead-exposed workers; 2) adherence by lead-exposed workers to safe work practices, such as properly using personal protective equipment, washing before eating, and showering and changing clothes before going home; 3) education of the medical community to use current guidelines and recommendations for management of lead-exposed adults with BLLs ≥10 µg/dL (4,5,7); and 4) increased involvement of the public health community to prevent nonoccupational lead exposures.
Acknowledgments
ABLES program coordinators in Alaska, Alabama, Arizona, California, Colorado, Connecticut, Florida, Georgia, Hawaii, Iowa, Illinois, Indiana, Kansas, Kentucky, Louisiana, Massachusetts, Maryland, Maine, Michigan, Minnesota, Missouri, Montana, North Carolina, Nebraska, New Hampshire, New Jersey, New Mexico, New York, Ohio, Oklahoma, Oregon, Pennsylvania, Rhode Island, South Carolina, Tennessee, Texas, Utah, Vermont, Washington, Wisconsin, and Wyoming.
References
- CDC. Fourth national report on human exposure to environmental chemicals. Updated tables, September 2013. Atlanta, GA: US Department of Health and Human Services, CDC; 2012. Available at http://www.cdc.gov/exposurereport/pdf/fourthreport_updatedtables_sep2013.pdf.
- CDC. Adult Blood Lead Epidemiology and Surveillance (ABLES). Cincinnati, OH: US Department of Health and Human Services, CDC, National Institute for Occupational Safety and Health; 2013. Available at http://www.cdc.gov/niosh/topics/ables/description.html.
- National Toxicology Program. Health effects of low-level lead evaluation. Research Triangle Park, NC: US Department of Health and Human Services, National Toxicology Program; 2013. Available at http://ntp.niehs.nih.gov/go/36443.
- Association of Occupational and Environmental Clinics. Medical management guidelines for lead-exposed adults. Washington, DC: Association of Occupational and Environmental Clinics; 2007. Available at http://www.aoec.org/documents/positions/MMG_FINAL.pdf.
- Kosnett MJ, Wedeen, RP, Rothenberg SJ, et al. Recommendations for medical management of adult lead exposure. Environ Health Perspect 2007;115:463–71.
- Occupational Safety and Health Administration. Lead standards: general industry (29 CFR 1910.1025) and construction industry (29 CFR 1926.62). Washington, DC: US Department of Labor, Occupational Safety and Health Administration; 1978. Available at https://www.osha.gov/sltc/lead.
- California Department of Public Health. Medical guidelines for the lead-exposed worker. Richmond, CA: California Department of Public Health, Occupational Lead Poisoning Prevention Program; 2009. Available at http://www.cdph.ca.gov/programs/olppp/documents/adultmgtguide.pdf.
- US Department of Health and Human Services. Healthy people 2020: occupational safety and health objective 7. Washington, DC: US Department of Health and Human Services; 2013. Available at http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicid=30.
- Occupational Safety and Health Administration. OSHA technical manual (OTM). Section V: chapter 3. Controlling lead exposures in the construction industry: engineering and work practice controls. Washington, DC: US Department of Labor, Occupational Safety and Health Administration; 1999. Available at http://www.osha.gov/dts/osta/otm/otm_v/otm_v_3.html#2.
- Whittaker SG. Lead exposure in radiator repair workers: a survey of Washington State radiator repair shops and review of occupational lead exposure registry data. J Occup Environ Med 2003;45:724–33.
* Federal funding for state ABLES program was discontinued in September 2013. The ABLES program continues to provide technical assistance to states with adult blood lead surveillance programs and maintains the ABLES website for reporting ongoing analyses of ABLES data.
What is already known on this topic?
The vast majority of elevated blood lead levels (BLLs) in the United States are workplace-related. Most lead exposures at work occur in the manufacturing, construction, services, and mining industries. Current research has found that even BLLs <10 µg/dL can cause harm in adults. CDC considers BLLs ≥10 µg/dL to be elevated. In contrast to the CDC reference level, prevailing Occupational Safety and Health Administration (OSHA) lead standards allow workers removed from lead exposure to return to lead work when their BLL falls below 40 µg/dL.
What is added by this report?
Data collected by the Adult Blood Lead Epidemiology and Surveillance program during 2002–2011 identified 11,536 adults with very high BLLs (≥40 µg/dL), of whom 19% had elevated BLLs recorded during ≥2 years. Among those with known exposure source, occupational exposures accounted for 91% of adults with very high BLLs.
What are the implications for public health practice?
The finding that many workers have harmful BLLs, some that are persistent for ≥2 years, is of grave concern. Examining physicians should be aware that the OSHA lead standards give them broad flexibility to tailor protections to the worker's needs, including consideration of removal from lead exposure at BLLs lower than the current OSHA lead standards require. To prevent adverse health outcomes caused by very high BLLs, public health practitioners need to increase lead exposure prevention activities directed at employers, workers, health-care providers, and the community.
FIGURE. Four adults with very high blood lead levels (BLL ≥40 µg/dL) in multiple years, by year — Adult Blood Lead Epidemiology and Surveillance (ABLES) Program, United States, 2002–2011
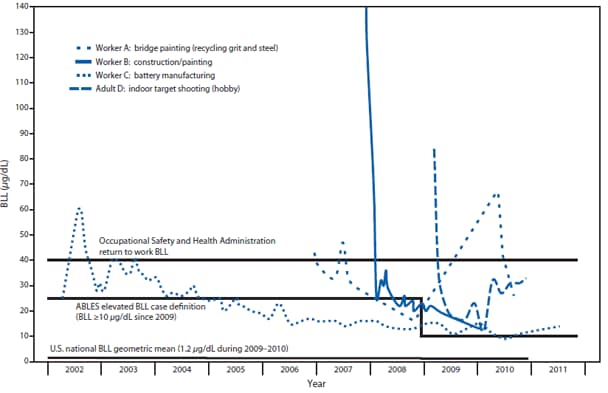
Alternate Text: The figure above indicates blood lead levels (BLLs) in four adults with very high BLLs (≥40 μg/dL) in multiple years, by year, in the United States during 2002-2011.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


