Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Babesiosis Surveillance — 18 States, 2011
Babesiosis is caused by protozoan parasites of the genus Babesia that infect red blood cells. Babesia infection can range from asymptomatic to life threatening. Clinical manifestations might include fever, other nonspecific influenza-like symptoms, and hemolytic anemia (1). Babesia parasites in nature usually are tickborne but they also are transmissible via blood transfusion or congenitally (1,2). In recent years, reports of tickborne and transfusion-associated cases have increased in number and geographic distribution (2–6). However, the lack of a standard case definition hindered the ability of public health authorities to monitor cases and to develop evidence-based prevention and control measures. In January 2011, national surveillance for human babesiosis was begun in 19 jurisdictions (18 states and one city), using a standard case definition developed jointly by CDC and the Council of State and Territorial Epidemiologists (7). This report summarizes the results for 2011. For the first year of babesiosis surveillance, health departments notified CDC of 1,124 confirmed and probable cases. Cases were reported by 15 of the 18 states where babesiosis was reportable; however, 1,092 cases (97%) were reported by seven states (Connecticut, Massachusetts, Minnesota, New Jersey, New York [including New York City], Rhode Island, and Wisconsin). Cases were identified in persons aged <1–98 years; 57% were in persons aged ≥60 years. Among patients for whom data were available, 82% (717 of 879) had symptom onset dates during June–August. Ongoing national surveillance using the standard case definition will provide a foundation for developing evidence-based prevention and control measures to reduce the burden of babesiosis.
Health departments notify CDC of cases of babesiosis via the National Notifiable Diseases Surveillance System (NNDSS), using a standard case definition (Table 1). In addition to basic demographic information (e.g., age, sex, and county of residence) provided via NNDSS, supplemental data (e.g., symptoms and history of transfusion) can be submitted to CDC using a disease-specific case report form (CRF). In 2011, babesiosis was reportable in 18 states and one city (Table 2) (8). Because babesiosis has been a reportable condition in some states for years, state-developed CRFs already had been in use to capture supplemental data. To promote standard data collection, CDC developed a babesiosis CRF, which was approved by the Office of Management and Budget in August 2011.* Supplemental data, derived from CDC's or a state's CRF, were merged manually with NNDSS records by matching a case identification number or demographic data. If case records had conflicting data, the more detailed record was considered correct.
In this summary, data for confirmed and probable cases were combined. Incidence rates were calculated by using 2010 population data from the U.S. Census Bureau (9). The seven states with well-established foci of zoonotic transmission (Connecticut, Massachusetts, Minnesota, New Jersey, New York, Rhode Island, and Wisconsin) are referred to as Babesia microti–endemic states (2). The Wilcoxon rank-sum test was used to compare the ranked distributions of ordinal variables.
For 2011, CDC was notified via NNDSS of 1,124 cases of babesiosis: 847 were classified as confirmed cases and 277 as probable cases. Supplemental data were provided for 797 (71%) of the 1,124 cases. The median age of patients was 62 years (range: <1–98 years); 63% were male, 34% were female, and the sex was unknown for 3% (Table 2). Among the 583 cases for which data on both race and ethnicity were available, more cases were reported in non-Hispanic whites than in persons of other races and ethnicities.
The 1,124 cases occurred in residents of 15 of the 18 states in which babesiosis was a reportable disease in 2011 (Table 2); 1,092 cases (97%) were reported by the seven main B. microti–endemic states. County-level incidence rates ranged from 0 to >100 cases per 100,000 persons (Figure 1). The state in which exposure occurred was available for 202 patients, 192 (95%) of whom became infected in their state of residence and 10 (5%) in a different state. Of the 295 patients for whom data were available, 156 (53%) recalled a tick bite in the 8 weeks before symptom onset. Reports for nine patients indicated that they also were diagnosed with another tickborne disease, either Lyme disease or anaplasmosis.
Ten cases of babesiosis in transfusion recipients were classified by the reporting health departments as transfusion associated, and two blood donors were reported. Each of the two blood donors was linked to one recipient; linked donors were not reported for eight of the 10 cases. Four other patients received blood transfusions before symptom onset, but whether these cases were transfusion associated was not known. One reported case was attributed to congenital transmission.
Babesia laboratory data were provided for 748 patients (574 with confirmed cases and 174 with probable cases). More than one test result was reported for 243 patients; 345 patients had positive blood-smear results, 409 had positive polymerase chain reaction (PCR) results, and 272 were seropositive (174 were classified as having probable cases, one of whom also had positive PCR results). Species-level data were provided for 429 cases, all of which were caused by B. microti. None of the reported cases were known to be caused by Babesia species other than B. microti.
The median intervals from date of illness onset, date of diagnosis, and date of laboratory testing to the date of report to CDC were 147 days (n = 879 cases; range: 7–475 days), 176 days (n = 116; range: 6–393 days), and 204 days (n = 112; range: 15–380 days), respectively.
Among the patients for whom data were available, 82% (717 of 879) had symptom onset dates during June–August (Figure 2). Symptoms were reported for 794 patients; one patient was asymptomatic. The most frequently reported clinical manifestations included fever (85% [550 of 650 patients]), chills (66% [389 of 590]), and myalgia (64% [371 of 576]). Of the 689 patients for whom data were available, 314 (46%) were hospitalized at least overnight. The median length of hospital stay was 4 days (range: 1–34 days). The patients who were hospitalized were significantly older than those who were not (median age of 68 years [range: <1–96 years] and median age of 58 years [range: 3–89 years], respectively; p-value <0.001). Twenty-four patients were known to be asplenic, 19 (79%) of whom were hospitalized. Four deaths were reported. One patient's death was not attributed to babesiosis; whether babesiosis contributed to the other three patients' deaths is not known.
Reported by
Barbara L. Herwaldt, MD, Susan Montgomery, DVM, Dana Woodhall, MD, Elizabeth A. Bosserman, MPH, Div of Parasitic Diseases and Malaria, Center for Global Health, CDC. Corresponding contributor: Elizabeth A. Bosserman, ebosserman@cdc.gov, 404-718-4745.
Editorial Note
Babesiosis is a preventable and treatable tickborne disease that can be severe and even life-threatening, especially in persons who are asplenic, elderly, or immunosuppressed (1). If the diagnosis of babesiosis is being considered, a nonautomated review of blood smears by a laboratory technician should be requested explicitly. Confirmation by a reference laboratory might be needed. Molecular techniques can be used to detect low levels of parasites. The diagnosis of babesiosis should be confirmed parasitologically whenever possible; however, antibody detection by serologic testing can provide supportive evidence for infection.† Persons with asymptomatic Babesia infection typically do not require treatment. Symptomatic persons usually are treated for at least 7–10 days, either with atovaquone plus azithromycin, or, for severe cases, with clindamycin plus quinine (1).
In 2011, the reported cases of babesiosis occurred most frequently in the spring and summer and in the Northeast and upper Midwest, but cases also were identified in other seasons and regions (e.g., because of travel or non-vectorborne transmission). In part because of concerns about the potential expansion of the geographic range of babesiosis, documenting where infection was acquired is important. For persons who live in or near B. microti–endemic areas, determining the state of exposure can be difficult. Most patients did not recall a tick bite. The 10 travel-associated cases accounted for five of the 32 cases reported outside of the B. microti–endemic states; information on location of exposure was not provided for the other 27 patients. Even for patients reportedly infected in their states of residence, differentiating between infection resulting from the expanding range of babesiosis and infection acquired during travel to a B. microti–endemic region within a state can be challenging.
Ten cases of transfusion-associated babesiosis in blood recipients were reported via national babesiosis surveillance. Currently, no licensed tests for screening U.S. blood donors for evidence of Babesia infection are available (10). Persons who test positive for Babesia infection should be advised to refrain indefinitely from donating blood.
The findings in this report are subject to at least three limitations. First, diagnosis of babesiosis requires a high index of suspicion, in part because the clinical manifestations are nonspecific; even severe cases can be missed (1,2). Second, babesiosis was a reportable condition in only 18 states in 2011; diagnosed cases of babesiosis in residents of states in which babesiosis was not reportable are not included in this surveillance summary. Finally, even for reported cases, the validity of the diagnosis of babesiosis and the case classification was dependent on the completeness and accuracy of the data provided.
Timely, accurate, and complete surveillance data will enable public health authorities to detect trends in the frequency and distribution of tickborne and transfusion transmission of Babesia infection. Subsequent years of surveillance data will allow public health authorities to monitor for unusual geographic or demographic patterns, such as changing areas of endemicity. Ongoing national surveillance using a standard case definition and report form will provide a foundation for developing evidence-based prevention and control measures to reduce the overall burden of babesiosis.
Persons who live in or travel to regions where babesiosis is found should avoid tick-infested areas, apply repellents and wear long pants and long-sleeved shirts when outdoors, shower soon after being outdoors, and check their entire bodies for ticks (1).§
Acknowledgments
State and local health departments that provided information to CDC.
References
- Vannier E, Krause PJ. Human babesiosis. N Engl J Med 2012;366:2397–407.
- Herwaldt BL, Linden JV, Bosserman E, et al. Transfusion-associated babesiosis in the United States: a description of cases. Ann Intern Med 2011;155:509–19.
- Joseph JT, Roy SS, Shams N, et al. Babesiosis in Lower Hudson Valley, New York, USA. Emerg Infect Dis 2011;17:843–7.
- Herwaldt BL, McGovern PC, Gerwel MP, Easton RM, MacGregor RR. Endemic babesiosis in another eastern state: New Jersey. Emerg Infect Dis 2003;9:184–8.
- Weld ED, Eimer KM, Saharia K, Orenstein A, Hess JR. The expanding range and severity of babesiosis. Transfusion 2010;50:290–1.
- Holman MS, Caporale DA, Goldberg J, et al. Anaplasma phagocytophilum, Babesia microti, and Borrelia burgdorferi in Ixodes scapularis, southern coastal Maine. Emerg Infect Dis 2004;10:744–6.
- CDC. National Notifiable Diseases Surveillance System. Available at http://www.cdc.gov/osels/ph_surveillance/nndss/nndsshis.htm. Accessed July 5, 2012.
- Council of State and Territorial Epidemiologists. CSTE state reportable conditions assessment. Babesiosis reportability. Atlanta, GA: Council of State and Territorial Epidemiologists; 2012. Available at http://www.cste.org/dnn/programsandactivities/publichealthinformatics/statereportableconditionsqueryresults/tabid/261/default.aspx. Accessed July 5, 2012.
- US Census Bureau. State & county QuickFacts. Washington, DC: US Census Bureau; 2012. Available at http://quickfacts.census.gov/qfd/index.html. Accessed July 5, 2012.
- Leiby DA. Transfusion-transmitted Babesia spp.: bull's-eye on Babesia microti. Clin Microbiol Rev 2011;24:14–28.
* The CDC-developed babesiosis CRF is available at http://www.cdc.gov/parasites/babesiosis/resources/babesiosis_case_report_form.pdf.
† Additional information available at http://dpd.cdc.gov/dpdx/html/babesiosis.htm.
§ Additional information available at http://www.cdc.gov/parasites/babesiosis.
What is already known on this topic?
Babesiosis in humans is a preventable and treatable parasitic disease that ranges in severity from asymptomatic to life threatening. Babesia parasites are transmitted primarily by the bite of an infected tick but also can be transmitted through blood transfusion. In the United States, tickborne transmission mainly occurs in parts of the Northeast and upper Midwest and usually peaks during the spring and summer.
What is added by this report?
For the first time, U.S. cases of babesiosis were reported using a standard national case definition. In 2011, a total of 1,124 cases of babesiosis were reported. Over half (57%) of the cases were in persons aged ≥60 years, and 97% of cases were reported by seven states.
What are the implications for public health practice?
Tickborne and transfusion-associated cases of babesiosis occur in multiple parts of the United States, including outside of areas of known endemicity. Ongoing national surveillance using the standard case definition will provide a foundation for developing evidence-based prevention and control measures to reduce the burden of babesiosis.
|
TABLE 1. National surveillance case definition for babesiosis* |
|
|---|---|
|
Clinical evidence |
Objective One or more of the following: fever, anemia, or thrombocytopenia. Subjective One or more of the following: chills, sweats, headache, myalgia, or arthralgia. |
|
Epidemiologic evidence for transfusion transmission |
For the purposes of surveillance, epidemiologic linkage between a transfusion recipient and a blood donor is demonstrated if all of the following criteria are met: In the transfusion recipient Received one or more red blood cell (RBC) or platelet transfusions within 1 year before the collection date of a specimen with laboratory evidence of Babesia infection; and At least one of these transfused blood components was donated by the donor described below; and Transfusion-associated infection is considered at least as plausible as tickborne transmission; and In the blood donor Donated at least one of the RBC or platelet components that was transfused into the above recipient; and The plausibility that this blood component was the source of infection in the recipient is considered equal to or greater than that of blood from other involved donors. (More than one plausible donor can be linked to the same recipient.) |
|
Laboratory criteria for diagnosis |
Laboratory confirmatory Identification of intraerythrocytic Babesia organisms by light microscopy in a Giemsa, Wright, or Wright-Giemsa–stained blood smear; or Detection of Babesia microti DNA in a whole blood specimen by polymerase chain reaction (PCR); or Detection of Babesia spp. genomic sequences in a whole blood specimen by nucleic acid amplification; or Isolation of Babesia organisms from a whole blood specimen by animal inoculation. Laboratory supportive Demonstration of a Babesia microti indirect fluorescent antibody (IFA) total immunoglobulin (Ig) or IgG antibody titer of ≥1:256 (or ≥1:64 in epidemiologically linked blood donors or recipients); or Demonstration of a Babesia microti immunoblot IgG positive result; or Demonstration of a Babesia divergens IFA total Ig or IgG antibody titer of ≥1:256; or Demonstration of a Babesia duncani IFA total Ig or IgG antibody titer of ≥1:512. |
|
Case classification |
|
|
Confirmed |
A case that has confirmatory laboratory results and meets at least one of the objective or subjective clinical evidence criteria, regardless of the mode of transmission (can include clinically manifest cases in transfusion recipients or blood donors). |
|
Probable |
A case that has supportive laboratory results and meets at least one of the objective clinical evidence criteria (subjective criteria alone are not sufficient); or A case that is in a blood donor or recipient epidemiologically linked to a confirmed or probable babesiosis case (as defined above) and Has confirmatory laboratory evidence but does not meet any objective or subjective clinical evidence criteria; or Has supportive laboratory evidence and might or might not meet any subjective clinical evidence criteria but does not meet any objective clinical evidence criteria. |
|
* Adapted from CDC's Case Definitions for Infectious Conditions Under Public Health Surveillance, available at http://www.cdc.gov/osels/ph_surveillance/nndss/casedef/index.htm. The case definition was developed in collaboration with epidemiologists at CDC and the Council of State and Territorial Epidemiologists. |
|
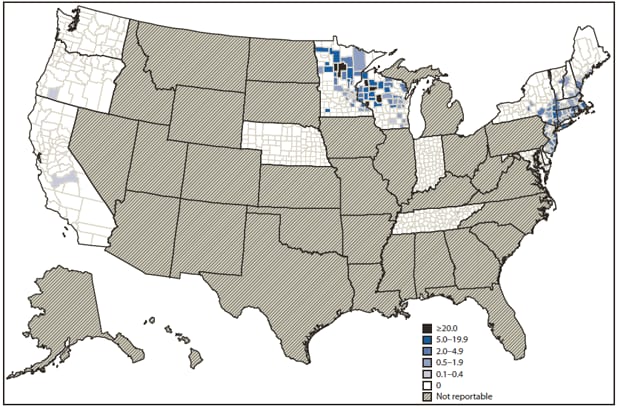
* Per 100,000 persons.
† N = 1,116; county of residence was unknown for eight of the 1,124 patients.
§ California, Connecticut, Delaware, Indiana, Maine, Maryland, Massachusetts, Minnesota, Nebraska, New Hampshire, New Jersey, New York, Oregon, Rhode Island, Tennessee, Vermont, Washington, and Wisconsin.
Alternate Text: The figure above shows incidence of reported cases of babesiosis, by county of residence, in 18 states during 2011. The 1,124 cases occurred in residents of 15 of the 18 states in which babesiosis was a reportable disease in 2011; 1,092 cases (97%) were reported by the seven main B. microti-endemic states. County-level incidence rates ranged from 0 to >100 cases per 100,000 persons.
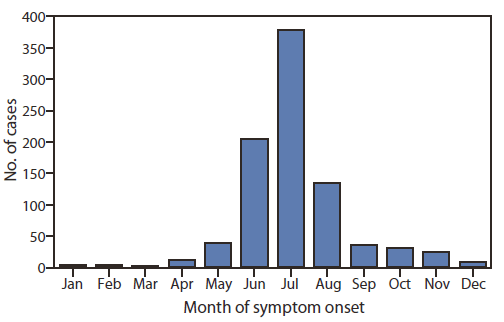
* N = 879.
† Data for two patients with symptom onset in late December 2010 are not included.
§ California, Connecticut, Delaware, Indiana, Maine, Maryland, Massachusetts, Minnesota, Nebraska, New Hampshire, New Jersey, New York, Oregon, Rhode Island, Tennessee, Vermont, Washington, and Wisconsin.
Alternate Text: The figure above shows the number of reported cases of babesiosis, by month of symptom onset, in 18 states during 2011. Among the patients for whom data were available, 82% (717 of 879) had symptom onset dates during June-August.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


