Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
CDC Grand Rounds: Dietary Sodium Reduction — Time for Choice
This is another in a series of occasional MMWR reports titled CDC Grand Rounds. These reports are based on grand rounds presentations at CDC on high-profile issues in public health science, practice, and policy. Information about CDC Grand Rounds is available at http://www.cdc.gov/about/grand-rounds.
Excess dietary sodium is a major contributor to hypertension (high blood pressure) and a critical public health issue in the United States (1). Nearly one in three U.S. adults, or 68 million persons, has hypertension, and half of those do not have their condition under control (2). Hypertension is a major contributor to cardiovascular diseases, which are a leading cause of death, disability, and health-care costs in the United States (3). The average sodium intake among persons in the United States aged ≥2 years is 3,266 mg/day (excluding table salt) (4). Current dietary guidelines recommend that reducing consumption of sodium to <2,300 mg/day, and that blacks, persons aged ≥51 years, and persons of any age with hypertension, diabetes, or chronic kidney disease (about half of the U.S. population and the majority of adults) further reduce intake to 1,500 mg/day (5). Regardless of age or sex, sodium intake by most U.S. residents considerably exceeds recommended levels (Figure). Reducing sodium intake to 2,300 mg/day potentially could prevent 11 million cases of hypertension and save billions of dollars in health-care expenditures; reducing sodium intake further would yield additional benefits (6). To achieve those reductions and help consumers make healthful choices, expanded educational efforts and monitoring of the sodium content of the food supply are needed. Increased availability of lower sodium products and reductions in the amount of sodium in foods served or sold in the marketplace also are needed.
The causal link between sodium intake and high blood pressure levels is well-established (7). Numerous scientific bodies and professional health organizations, including the American Heart Association,* the American Medical Association,† and the American Public Health Association,§ support dietary sodium reduction to prevent and control high blood pressure. Decreasing systolic blood pressure by an average of 5 mm Hg within a population can lead to an estimated 14% reduction in stroke deaths and 9% reduction in coronary heart disease deaths (8). For persons with prehypertension (i.e., blood pressure that is elevated above normal but not high enough for medical intervention), reduction of sodium intake might be particularly beneficial because lower blood pressure typically translates to lower risk for heart disease and stroke (9). Nearly 30% of U.S. adults are prehypertensive (10).
Sodium in Foods
A major challenge to sodium intake reduction efforts is the widespread use of sodium in the U.S. food supply, leaving little to no opportunity for average consumers to adjust their intake. The majority of sodium intake (>75%) is from consuming packaged and restaurant foods (1,11). Only an estimated 12% of sodium consumption occurs from natural sources, and 11% results from adding salt while cooking or eating a meal (11). Salt and other sodium-containing ingredients are added to food by manufacturers for many reasons; salt in particular can play multiple roles in flavoring, food processing, and safety at relatively low cost (1). Sodium can change the properties of food in ways that are useful for food manufacturers, such as extending shelf life or altering texture. In many cases, however, sodium content exceeds the concentrations needed for food safety or essential food processing (1).
The U.S. Department of Agriculture (USDA) conducts food composition analyses to measure the sodium values of foods that constitute significant sources of dietary intake. Mean sodium values for the same portion of different brands of the same foods can vary substantially; for example, the sodium content of 4-ounce slices of cheese pizza (regular crust) purchased from major pizza restaurant chains can vary from 510 mg to 760 mg (12). This variation suggests that achieving substantial decreases in sodium levels of commonly consumed foods is feasible (1). Current labeling regulations are designed to ensure that measured samples of a product do not exceed labeled sodium values by more than 20%.¶ However, laboratory analyses serve as a critical adjunct to closely monitor changes in the sodium content of the food supply and complement food label data.
Consumer and Health-Care Provider Readiness for Sodium Reduction
Data from the Behavioral Risk Factor Surveillance System in 21 states indicate that U.S. adults already are taking steps to reduce their sodium intake. In 2007, >70% of U.S. adults with self-reported hypertension had been advised to reduce their salt intake, and >80% of those adults reported that they were already reducing their intake (13). Data collected by a national market panel mail survey weighted to the U.S. population indicate that the majority of adult consumers understand the relationship between sodium intake and health, and 68% of consumers aged >50 years are either thinking about lowering their intake, have taken steps to lower their intake, or already have lowered their intake (14).
Despite the good intentions of U.S. adults, the ubiquity of sodium in processed and prepared foods makes it difficult for them to control their own sodium intake (1). Thus, interventions that involve food industry participation hold promise as a critical pathway to address this public health problem.
Current Strategies to Reduce Sodium Intake
In 2010, the Institute of Medicine (IOM) issued a report, "Strategies to Reduce Sodium Intake in the United States," which concluded that labeling and education efforts to bring about behavior change alone did not succeed in reducing sodium intake in the United States (1). The primary strategy recommended in the IOM report is to pursue broad, gradual reductions in the sodium content of packaged and prepared foods in the United States through mandatory national standards. In advance of implementing national standards, IOM supports voluntary initiatives involving collaboration between industry, government, and others as a strategy to support sodium reduction. The National Salt Reduction Initiative (NSRI)** currently uses this partnership strategy as a framework to achieve its goal to reduce dietary sodium by 20% in 5 years by decreasing sodium content in packaged and restaurant foods by 25% over the same period.
The NSRI is a partnership of more than 85 organizations and local and state health authorities, aiming to reduce U.S. dietary sodium through voluntary sodium-content reductions by the food industry. Coordinated by the New York City Health Department, the NSRI strategy is to set feasible sodium reduction targets for 62 packaged food categories and 25 restaurant food categories based on industry feedback and analysis of the NSRI nutrition databases, and then to measure industry progress over time. Targets are set for 2012 and 2014. Twenty-eight companies, including packaged food companies, supermarkets, and restaurant chains, have signed on to meet at least one target. In addition, New York City developed an evaluation process to assess changes in population sodium intake in a representative sample of adult New York City residents.†† The baseline evaluation included a 24-hour urine collection and analysis, with additional diagnostic and self-reported measures. A follow-up study will be conducted to monitor changes over time.
On the local level, New York City has introduced several innovative, policy-based strategies to reduce sodium intake. A Mayoral Executive Order in 2008 made New York City the first major U.S. city to set nutrition standards for all food purchased and served by city agencies.§§ The city also has initiated a citywide media campaign that included subway posters and newspaper advertisements to increase public awareness about the sodium content of processed foods. Other projects include an educational initiative about sodium for the city's independent restaurants and development of retail food standards for hospitals.
Summary
Sodium reduction is an urgent public health priority that should be addressed by coordinated attention by multiple levels of government, the food industry, and other diverse stakeholders. Average daily sodium intake for U.S. adults is more than double the recommended dietary limit for the majority of this population, leading to adverse health outcomes and economic impacts. The majority of U.S. adults recognize the health consequences of a high-sodium diet and are interested in reducing their sodium intake. However, packaged and restaurant foods often contain excessive amounts of sodium, which limits the choices of U.S. consumers about how much sodium they consume in those foods. USDA and the Food and Drug Administration recently collected public comments and research to help inform future sodium reduction-related activities.¶¶ In the interim, the NSRI is a promising voluntary process to encourage public commitments by industry to sodium reduction. Reducing sodium in the food supply will increase consumer choice, has been shown to be feasible for the food industry, and will save thousands of lives and billions of health-care dollars each year.
Reported by
Janelle P. Gunn, MPH, Nicole A. Blair, MPH, Mary E. Cogswell, DrPH, Robert K. Merritt, MA, Darwin R. Labarthe, MD, PhD, National Center for Chronic Disease Prevention and Health Promotion, CDC. Christine J. Curtis, MBA, New York City Dept of Health and Mental Hygiene. Jeremiah Fasano, PhD, Food and Drug Admin. Amy V. Neuwelt, MPH, Office of Surveillance, Epidemiology, and Laboratory Svcs; Tanja Popovic, MD, PhD, Office of the Director, CDC. Corresponding contributor: Janelle P. Gunn, jperalezgunn@cdc.gov, 770-488-8231.
Acknowledgment
Joanne Holden, Agricultural Research Srvc, US Dept of Agriculture.
References
- Institute of Medicine. Strategies to reduce sodium intake in the United States. Washington, DC: The National Academies Press; 2010.
- CDC. Vital signs: prevalence, treatment, and control of hypertension—United States, 1999–2002 and 2005–2008. MMWR 2011;60:103–8.
- Heidenreich PA, Trogdon JG, Khavjou OA, et al. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation 2011;123:933–44.
- CDC. Vital signs: food categories contributing the most to sodium consumption—United States, 2007–2008. MMWR 2012;61:92–8.
- US Department of Health and Human Services, US Department of Agriculture. Dietary guidelines for Americans, 2010. 7th ed. Washington, DC: US Government Printing Office; 2010.
- Palar K, Sturm R. Potential societal savings from reduced sodium consumption in the U.S. adult population. Am J Health Promot 2009;24:49–57.
- Institute of Medicine. Dietary reference intakes for water, potassium, sodium, chloride, and sulfate. Washington, DC: The National Academies Press; 2005.
- Stamler R. Implications of the INTERSALT study. Hypertension 1991;17(suppl1):I16–20.
- Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003;42:1206–52.
- Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease and stroke statistics—2012 update: a report from the American Heart Association. Circulation 2012;125:e2–220.
- Mattes RD, Donnelly D. Relative contributions of dietary sodium sources. J Am Coll Nutr 1991;10:383–93.
- US Department of Agriculture. National nutrient database for standard reference. Release 24. Washington, DC: US Department of Agriculture, Agricultural Research Service; 2001. Available at http://ndb.nal.usda.gov. Accessed February 3, 2012.
- Ellis C, Grubaugh A, Egede LE. The effect of minority status and rural residence on actions to control high blood pressure in the U.S. Public Health Rep 2010;125:801–9.
- CDC. Public health grand rounds. Sodium reduction: time for choice. Atlanta, GA: US Department of Health and Human Services, CDC; 2011. Available at http://www.cdc.gov/about/grand-rounds/archives/2011/april2011.htm. Accessed September 19, 2011.
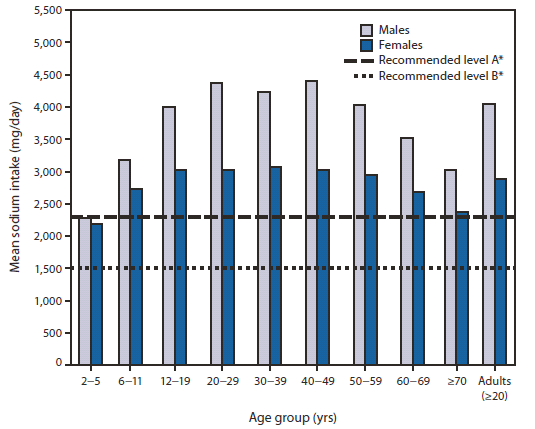
FIGURE. Mean sodium intake (excluding table salt), by age and sex, and recommended levels* — National Health and Nutrition Examination Survey, United States, 2007–2008
Alternate Text: The figure above shows mean sodium intake (excluding table salt), by age and sex, in the United States, during 2007-2008, according to the National Health and Nutrition Examination Survey, and current recommended levels of dietary sodium. Regardless of age or sex, sodium intake by most U.S. residents considerably exceeds recommended levels.