Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Hepatitis C Virus Infection Among Adolescents and Young Adults --- Massachusetts, 2002--2009
Hepatitis C virus (HCV) infection is a major cause of liver disease and hepatocellular carcinoma in the United States (1,2). Of the estimated 2.7--3.9 million persons with active HCV infection, most were born during 1945--1964 and likely were infected during the 1970s and 1980s, before the advent of prevention measures (3). Nationwide, rates of acute, symptomatic HCV infection declined during 1992--2005 and then began to level (4). Declines also were observed in rates of newly reported HCV infection in Massachusetts. Although these declines were evident among reported cases overall in Massachusetts during 2002--2006, an increase was observed among cases in the 15--24 year age group. In response to this increase, the Massachusetts Department of Public Health (MDPH) launched a surveillance initiative to collect more detailed information on cases reported during 2007--2009 among this younger age group and to examine the data for trends through 2009. This report describes results of both efforts, which revealed continued increases in rates of newly reported HCV infection among persons aged 15--24 years. These cases were reported from all areas of the state, occurred predominantly among non-Hispanic white persons, and were equally distributed among males and females. Of cases with available risk data, injection drug use (IDU) was the most common risk factor for HCV transmission. The increase in case reports appears to represent an epidemic of HCV infection related to IDU among new populations of adolescents and young adults in Massachusetts. The findings indicate the need for enhanced surveillance of HCV infection and intensified hepatitis C prevention efforts targeting adolescents and young adults.
MDPH currently uses an electronic data system for disease surveillance. All positive laboratory results indicating HCV infection are reportable to MDPH. A positive laboratory result on a previously unreported case prompts a case report form to be sent to the health-care provider (e.g., clinician) ordering the test. This one-page form collects information on demographics, symptoms, and risk history. In accordance with CDC case definitions, HCV infection cases are classified as either confirmed (i.e., positive by an anti-HCV antibody assay with a nucleic acid test [NAT] result confirming active infection) or probable (i.e., positive antibody test result with confirmatory NAT either not conducted or not reported to MDPH). For this analysis, all confirmed and probable cases of HCV infection were included.
In 2006, anecdotal information received from community-based partners about HCV infection cases among adolescents and young adults prompted a review of state surveillance data. Although an overall decline in rates of newly reported HCV infection (from 181 to 128 cases per 100,000 population) was observed during 2002--2006, an increase (from 65 to 102 cases per 100,000 population) was observed among persons aged 15--24 years. At the time, 75% of 2005 surveillance reports for cases among persons in this age group lacked risk history; therefore, the sources of infection were unknown. Beginning in 2007, MDPH sent HCV infection case report forms (CRFs) to reporting clinicians to collect additional information when a report of newly identified HCV antibody (anti-HCV) positivity among persons aged 15--24 years was received. Clinicians also were sent reminders to fill out CRFs if more than 30 days had passed from the date the form was sent and a completed form had not yet been received by MDPH.
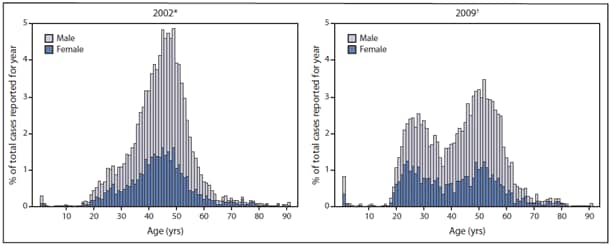
During 2002--2009, rates of newly reported HCV infection (confirmed and probable) among persons aged 15--24 years increased from 65 to 113 cases per 100,000 population (Figure 1). The number of confirmed cases of HCV infection reported in Massachusetts was further examined by age and compared for the years 2002 and 2009 (Figure 2). The data shifted from a unimodal age distribution in 2002 to a bimodal age distribution in 2009, with the latter showing substantially more reports of HCV infection among adolescents and young adults compared with the earlier period.
During 2007--2009, MDPH received 1,925 reports of new cases of HCV infection among persons aged 15--24 years. Of these, 1,026 (53%) were classified as confirmed cases of HCV infection; the remainder were classified as probable. Although some clustering of cases was observed in urban areas, cases were reported from all areas of the state, including large metropolitan areas, suburban areas of Boston, smaller cities, and rural areas. Cases occurred with nearly the same frequency among men and women.
Of the 1,925 CRFs sent to reporting sources for completion, 1,448 (75%) were returned to MDPH, providing details of 802 confirmed and 646 probable cases. Of those returned, 252 (17%) CRFs did not have sufficient information to assess risk, and of these, 148 (59%) contained no risk data.
Of the total 1,448 CRFs returned, 1,357 (94%) included information on race. Of these, 1,052 (78%) indicated cases among persons who were white, 37 (3%) who were black, and 21 (2%) who were Asian; four indicated cases among persons who were American Indian/Alaska Native, and two indicated cases among persons who were Native Hawaiian or other Pacific Islanders. Ninety-four CRFs indicated cases in persons reported as being of unknown race, and 147 indicated "other" or multiple race categories. Of 1,154 (80%) cases with ethnicity information, 98 (8%) were among persons identified as Hispanic. Eight percent of the 1,448 cases with completed CRFs were among persons who were homeless or incarcerated.
By far, the most common risk identified was IDU. Of 1,196 cases with a reported risk history, 860 (72%) were in persons who reported current or past IDU; of these, 719 (84%) reported injecting drugs during the preceding 12 months. In addition, 445 (34%) reported some history of intranasal drug use. All but 34 of the cases for which intranasal drug use was listed also indicated IDU. Of the 719 cases for which IDU during the preceding 12 months was reported, 615 (85%) were among persons who reported heroin use, 220 (29%) cocaine use, seven (1%) methamphetamine use, and 31 (4%) use of other drugs, including opiates other than heroin (categories are not mutually exclusive because more than one drug could be reported). Additional commonly reported potential exposures included "other" blood exposures (24%) (further detail is missing for most cases for which this was reported; for those cases with this information included, a majority of "other" exposures listed were related to IDU), tattoos (23%), and a history of incarceration (20%); however, most cases involving these exposures were among persons who also were exposed through IDU.
Reported by
Shauna Onofrey, MPH, Daniel Church, MPH, Patricia Kludt, MPH, Alfred DeMaria, MD, Kevin Cranston, MDiv, Massachusetts Dept of Public Health. Geoff A. Beckett, MPH, Scott D. Holmberg, MD, John W. Ward, MD, Deborah Holtzman, PhD, Div of Viral Hepatitis, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention, CDC. Corresponding contributor: Deborah Holtzman, CDC, 404-718-8555, dholtzman@cdc.gov.
Editorial Note
The Massachusetts surveillance data indicate an increase in HCV infection cases among adolescents and young adults during 2002--2009. These cases were primarily among non-Hispanic white residents in urban, suburban, and rural communities. Although calculating an incidence rate from the surveillance data or determining the duration of infection for persons who tested positive for anti-HCV antibody is not possible, the findings suggest that most persons aged 15--24 years with HCV infection likely acquired their infections within a few years of being tested and reported. Although similar increases in human immunodeficiency virus (HIV) infection were not identified for this age group, increases in reports of HCV infection among injection drug users might be a harbinger of increases in IDU-associated HIV.
Other states have indicated similar increases in HCV infection among adolescents and young adults. For example, in 2008, New York reported an increase in HCV infection among persons aged <30 years in suburban Buffalo (5). Since that time, surveillance data have indicated continued transmission and possibly new activity in other areas of New York (Elena Rizzo, New York State Department of Health, personal communication, 2011).
During the period when increases in HCV infection were being observed, Massachusetts experienced a concomitant increase in heroin use among adolescents and young adults. Data from MDPH-funded substance abuse programs showed a rise in the percentage of admissions (for all drug use) among persons aged 15--24 years, from 19% in 2002 to 23% in 2008.* Furthermore, the percentage of program clients who reported needle use when admitted increased from 29% in 2002 to 38% in 2008 among persons aged 15--24 years, whereas the percentage among all other age groups during this same period remained relatively constant at approximately 30%. Although the occurrence of IDU-associated HCV infection has been documented for decades, the recent epidemic in reported cases among adolescents and young adults and its apparent association with increases in drug injection and sharing of injection equipment in this population is a disturbing trend. Law enforcement data suggest this trend might be occurring in other states. During 2002--2009, the estimated average annual number of heroin initiates in the United States increased from 100,000 to 180,000.† Law enforcement reporting from the Great Lakes, Mid-Atlantic, New England, New York/New Jersey, Southeast, and West Central regions also suggests that heroin use is increasing, particularly among younger users.§
Addressing the epidemic of HCV infection among adolescents and young adults presents unique challenges in terms of education, outreach, and other interventions. Studies have shown that the incidence of HCV infection among injection drug users aged <30 years ranges from 10 to 37 cases per 100 person-years (6,7). Moreover, among adolescents and young adults who inject drugs, HCV positivity has been associated with duration and frequency of injection (6). Adolescents and young adults might be more likely to share drug equipment because of the nature of their social networks, which are characterized by trust and sharing (6). The nature of these interactions must be taken into account when developing educational materials. Adolescents and young adults are likely to have participated in other risky behaviors before initiation of injecting and might have multiple physical, mental, and emotional health needs (8). The recent Institute of Medicine report on viral hepatitis and liver cancer noted that younger injection drug users might be at highest risk for seroconversion in the years immediately following initiation of injection practices (2).
The findings in this report are subject to at least four limitations. First, the surveillance data only include information for persons who have access to and obtain serologic testing and thus might underrepresent the number of persons with HCV infection. This also might explain, in part, the demographic patterns that were observed. Second, efforts by MDPH to raise awareness of the increase in case rates among this age group might have contributed to an increase in testing and reporting of cases after 2007. Although data were not available to ascertain whether this actually occurred, and if so, what the magnitude of such an effect might have been, increases in the case rate among adolescents and young adults in Massachusetts were evident in the years before 2007 and, in fact, were more pronounced. In addition, recent research on injection drug users showed that, although persons aged 18--24 years had the highest rate of being tested for HIV, they had the lowest rate of HCV testing despite national recommendations for counseling and screening of injection drug users (9,10). Third, differences by county of residence could not be determined because of infrequent recording of residence information on laboratory results not accompanied with a matching CRF. Finally, differences in testing and reporting by county might also exist. Further studies are needed to better characterize the population groups that are at increased risk and those persons who are infected with HCV. Health-care providers need to be encouraged to ask about risks for HCV infection, especially IDU, and to screen patients at risk.
One important outcome of this study is that CDC, in collaboration with state and local health departments, is examining HCV surveillance data to determine whether similar trends are occurring in other reporting areas. In addition, MDPH and CDC are conducting an in-depth investigation of the causes of HCV transmission among adolescents and young adults in Massachusetts to recommend and implement targeted prevention measures.
This report highlights the important role of surveillance for HCV infection and reporting of all laboratory tests positive for HCV, along with the capacity to collect data of sufficient quality for meaningful analysis of trends in transmission and disease. By 2010, 43 states (including Massachusetts) and the District of Columbia required reporting of all laboratory tests indicative of HCV infections.¶ However, despite the laboratory reporting requirement, most states have limited resources dedicated to surveillance of viral hepatitis and lack capacity to investigate reported cases and forward reliable data to CDC for national reporting. The Institute of Medicine noted this deficiency in public health surveillance as a major weakness in the prevention of viral hepatitis and liver cancer and recommended federal assistance for states to effectively conduct surveillance for all forms of hepatitis C (2).
This report also strongly indicates the need for expanded and intensified hepatitis C prevention efforts targeting adolescents and young adults. The Institute of Medicine notes that multicomponent, comprehensive risk reduction programs are likely to be the most successful at addressing HCV infection prevention needs of persons who use illicit drugs. Some interventions that could be implemented include access to sterile syringes and drug preparation equipment through syringe exchange services, expanded school-based education that includes viral hepatitis prevention messages, expanded harm reduction programs directed toward young drug users, entry to drug treatment for young injection drug users, and access to comprehensive health services that include HCV testing and linkage to care.
Acknowledgments
This report is based, in part, on contributions by Massachusetts local health departments.
References
- Wise M, Bialek S, Finelli L, Bell BP, Sorvillo F. Changing trends in hepatitis C-related mortality in the United States, 1995--2004. Hepatol 2008;47:1128--31.
- Institute of Medicine. Hepatitis and liver cancer: a national strategy for prevention and control of hepatitis B and C. Washington, DC: National Academies Press; 2010.
- Armstrong GL, Wasley A, Simard EP, McQuillan GM, Kuhnert WL, Alter MJ. The prevalence of hepatitis C virus infection in the United States, 1999 through 2002. Ann Intern Med 2006;144:705--14.
- CDC. Surveillance for acute viral hepatitis---United States, 2005. MMWR 2007;56(No. SS-3).
- CDC. Use of enhanced surveillance for hepatitis C virus infection to detect a cluster among young injection-drug users---New York, November 2004--April 2007. MMWR 2008;57:517--21.
- Miller CL, Johnston C, Spittal PM, et al. Opportunities for prevention: hepatitis C prevalence and incidence in a cohort of young injection drug users. Hepatol 2002;36:737--42.
- Hahn JA, Page-Schafer K, Lum PJ, et al. Hepatitis C virus seroconversion among young injection drug users: relationships and risks. J Infect Dis 2002;186:1558--64.
- Fuller CM, Vlahov D, Arria AM, Ompad DC, Garfein R, Strathdee SA. Factors associated with adolescent initiation of injection drug use. Public Health Rep 2001;116:136--45.
- CDC. Recommendations for prevention and control of hepatitis C virus (HCV) infection and HCV-related chronic disease. MMWR 1998;47(No. RR-19).
- CDC. HIV-associated behaviors among injecting-drug users---23 cities, United States, May 2005--February 2006. MMWR 2009;58:329--32.
What is already known on this topic?
In the United States, hepatitis C virus (HCV) infection is an important cause of morbidity and mortality, especially in its chronic form. Persons who inject drugs are at greatest risk for HCV infection.
What is added by this report?
The Massachusetts surveillance data indicate an increase in cases of HCV infection among adolescents and young adults (i.e., persons aged 15--24 years) during 2002--2009. The increase in case reports appears to represent an epidemic of HCV infection related to injection drug use in this age group.
What are the implications for public health practice?
This report highlights the essential role of surveillance for HCV infection and reporting of all laboratory tests positive for HCV, along with the collection of case data sufficient to assess disease burden and transmission patterns. This report also strongly indicates the need for expanded and intensified hepatitis C prevention efforts targeting adolescents and young adults.
FIGURE 1. Rates of newly reported cases of hepatitis C virus infection (confirmed and probable) among persons aged 15--24 years and among all other age groups --- Massachusetts, 2002--2009
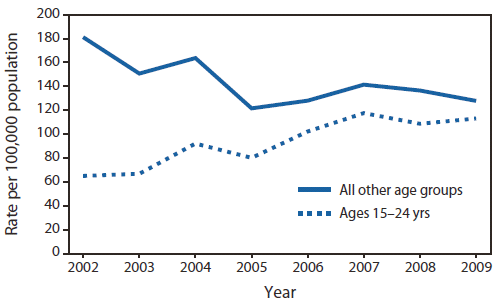
Alternate Text: The figure above shows rates of newly reported cases of hepatitis C virus infection (confirmed and probable) among persons aged 15-24 years and among all other age groups in Massachusetts during 2002-2009. Rates increased from 65 to 113 cases per 100,000 population.
FIGURE 2. Age distribution of newly reported confirmed cases of hepatitis C virus infection --- Massachusetts, 2002 and 2009
Alternate Text: The figure above shows age distribution of newly reported confirmed cases of hepatitis C virus infection in Massachusetts for 2002 and 2009. The data shifted from a unimodal age distribution in 2002 to a bimodal age distribution in 2009, with the latter showing substantially more reports of HCV infection among adolescents and young adults compared with the earlier period