Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Respiratory Syncytial Virus Activity --- United States, July 2008--December 2009
Respiratory syncytial virus (RSV) is the most common cause of bronchiolitis and pneumonia in children aged <1 year worldwide. Each year in the United States, an estimated 75,000--125,000 infants are hospitalized with RSV (1). Among adults aged >65 years, an estimated 177,000 hospitalizations and 14,000 deaths a year have been attributed to RSV infections (2). In temperate climates, the RSV season generally begins during the fall and continues through the winter and spring, but the exact timing of RSV circulation varies by location and year (3). In the United States, data from the National Respiratory and Enteric Virus Surveillance System (NREVSS) are used to monitor the seasonal occurrence of RSV. During the 2008--09 season, onset occurred from mid-October to late December in the 10 U.S. Department of Health and Human Services (HHS) regions,* excluding Florida, which had onset in mid-July. Season offset in all regions occurred from mid-February to mid-April. Florida is reported separately because it has an earlier season onset and longer duration than the rest of the country (4). During the current 2009--10 season, onset occurred in all 10 HHS regions by February 20, 2010. These patterns are similar to previous years and confirm differences in RSV seasonal characteristics across regions. Knowledge of RSV seasonality can be used by clinicians and public health officials to determine when to consider RSV as a cause of acute respiratory illnesses and when to provide RSV immunoprophylaxis to children at high risk for serious disease (5).
NREVSS is a voluntary, laboratory-based system that tracks temporal and geographic trends in the circulation of RSV and other viral pathogens. Laboratories report the number of RSV tests and the proportion that are positive, by collection date. For this analysis, the onset of the RSV national and regional season onset is the first of 2 consecutive weeks during which the mean percentage of specimens testing positive for RSV antigen is ≥10%. RSV season offset is defined as the last of 2 consecutive weeks during which the mean percentage of positive specimens is ≥10%. Season duration is the number of weeks between season onset and offset. For consistency, only antigen detection tests, which were used by 97% of participating laboratories during 2008-2009, were included in the analysis. Additionally, only data from laboratories that reported ≥30 weeks and averaged ≥10 specimens tested per week using antigen detection methods were included in the analysis for the 2008--09 season. For the initial phase of the 2009--10 reporting season, data from laboratories that reported ≥1 week and averaged ≥1 antigen detection test per week were included in the analysis. Persons might be tested, and therefore represented in the data, more than once.
During July 2008--June 2009 (weeks ending July 5, 2008--June 27, 2009), 238 (33%) of 718 reporting laboratories from 45 states met inclusion criteria. These laboratories reported a total of 404,798 tests, of which 60,793 (15%) were positive.† The national 2008--09 RSV season onset occurred the week ending November 1, 2008, and continued for 20 weeks until the season offset, the week ending March 21, 2009 (Table). When data from Florida were excluded (onset date in July), the national RSV season onset began 2 weeks later (week ending November 15, 2008); the season offset was not affected.
The 2008--09 season onset for all 10 HHS regions, excluding Florida, ranged from mid-October (week ending October 11, 2008) to late-December (week ending December 27, 2008) (Table and Figure). The season onset for Florida was the week ending July 12, 2008 and continued until the week ending February 7, 2009 (Figure). The 2008--09 season offset for all 10 HHS regions and Florida ranged from early February (week ending February 7, 2008) to mid-April (week ending April 11, 2009) (Table and Figure). Excluding Florida, the median season duration among the 10 HHS regions was 16 weeks (range: 14--23 weeks) (Table). The region with the shortest season was Region 3 (Philadelphia region) (14 weeks), and the longest season was in Region 4 (Atlanta region) (23 weeks). Preliminary data for the current 2009--10 RSV season (week ending July 28, 2009--February 20, 2010) were reported by 634 laboratories from all 50 states and the District of Columbia. A total of 316,453 RSV antigen detection tests were performed, and 50,070, (16%) positive results were reported to NREVSS. The season onset had occurred in all 10 HHS regions by February 20, 2010. Nationally, the 2009--10 RSV season onset occurred during the week ending November 14, 2009; however, when data from Florida were excluded, the national season onset occurred 1 week later (week ending November 21, 2009) (Table). Weekly updates showing RSV national, regional, and state trends are available from the NREVSS website at http://www.cdc.gov/surveillance/nrevss. Additional information about Florida RSV trends is available from the Florida Department of Health website at http://www.doh.state.fl.us/disease_ctrl/epi/rsv/rsv.htm.
Reported by
National Respiratory and Enteric Virus Surveillance System laboratories. GR Villarruel, MPH, GE Langley, MD, GR Abedi, LJ Anderson, MD, Div of Viral Diseases, National Center for Immunization and Respiratory Diseases, CDC.
Editorial Note
During the July 2008--June 2009 surveillance period, the national and regional RSV seasonal trends in onset, offset, and duration were similar to those reported for previous years, although the season started 1--3 weeks later during 2008--09 compared with 2007--08 in 10 HHS regions (4). The season onset was earlier and the duration was longer in Florida compared with other regions, which is consistent with a previous report (4). CDC alerts practitioners and public health officials about the timing of the season by posting timely data on the NREVSS website.
Reasons for regional and state differences in seasonality patterns might include variations in weather conditions that affect the transmissibility or viability of the virus (6). Social and demographic factors, such as household crowding and population density, also might contribute to differences in the timing and duration of RSV seasons (7).
Symptoms of RSV can be similar to those of other common respiratory pathogens, such as seasonal and pandemic H1N1 influenza. Knowing the timing of the RSV season can help determine when to consider it in the diagnosis of patients with respiratory illnesses. Determining the etiology of these illnesses has implications for treatment and control efforts.
Knowledge about the onset of RSV season can help determine when to initiate prevention strategies. RSV is transmitted person-to-person via direct or close contact with contaminated secretions, including respiratory droplets or fomites. In the community, attention to hand hygiene and limiting exposure of high-risk groups to settings where transmission is common, such as day-care settings, is recommended (5). Transmission of RSV in health-care settings can cause considerable morbidity in young children and older adults already at high risk for RSV (8). Infection control practices, including standard precautions, contact precautions, and cohorting of infected persons, are recommended (5).
Additionally, the data have been used to help determine when to administer prophylaxis with the monoclonal anti-RSV antibody, palivizumab (9). Palivizumab, which has been shown to reduce RSV hospitalizations in select infants and children with congenital heart disease, chronic lung disease, and compromised immune systems, or those born prematurely, is given as monthly intramuscular injections during the RSV season (9). The most recent policy statement from the American Academy of Pediatrics should be consulted for specific recommendations, including which specific infants and children are recommended for prophylaxis and the duration of prophylaxis (9).
The findings in this report are subject to at least two limitations. First, NREVSS relies on voluntary reporting, and the findings might not represent actual circulation of the virus at the national, regional, or state level. However, analyses have shown a correlation between NREVSS findings and RSV hospitalizations in children (10). Second, the definitions of onset and offset might not capture periods of low RSV activity. Despite these limitations, the data in this report provide epidemiologic information to guide diagnostic testing and help determine the timing of prevention programs.
References
- Shay DK, Holman RC, Newman RD, Liu LL, Stout JW, Anderson LJ. Bronchiolitis-associated hospitalizations among U.S. children, 1980--1996. JAMA 1999;282:1440--6.
- Falsey AR, Hennessey PA, Formica MA, Cox C, Walsh EE. Respiratory syncytial virus infection in elderly and high-risk adults. N Engl J Med 2005;352:1749--59.
- Mullins JA, LaMonte AC, Bresee JS, Anderson LJ. Substantial variability in community RSV season timing. Pediatr Infect Dis J 2003;22:857--62.
- CDC. Respiratory syncytial virus activity---United States, July 2008--December 2008. MMWR 2008;57:1355--8.
- American Academy of Pediatrics. Respiratory syncytial virus. In: Pickering LK, Baker CJ, Kimberlin DW, Long SS, eds. Red book: 2009 Report of the Committee on Infectious Diseases. 28th ed. Elk Grove Village, IL: American Academy of Pediatrics; 2009:560--9.
- Welliver RC Sr. Temperature, humidity, and ultraviolet B radiation predict community respiratory syncytial virus activity. Pediatr Infect Dis J 2007;26:S29--35.
- Zachariah P, Shah S, Gao D, Simoes EA. Predictors of the duration of the respiratory syncytial virus season. Pediatr Infect Dis J 2009;28:772--6.
- Hall CB. Nosocomial respiratory syncytial virus infections: the "Cold War" has not ended. Clin Infect Dis 2000;31:590--6.
- American Academy of Pediatrics Committee on Infectious Diseases. Modified recommendations for use of palivizumab for prevention of respiratory syncytial virus infections. Pediatrics. 2009;124:1694 --701.
- Light M, Bauman J, Mavunda K, Malinoski F, Eggleston M. Correlation between respiratory syncytial virus (RSV) test data and hospitalization of children for RSV lower respiratory tract illness in Florida. Pediatr Infect Dis J 2008;27:512--8.
* The 10 HHS regions (listed by region number and headquarters city) are Region 1 (Boston), Region 2 (New York), Region 3 (Philadelphia), Region 4 (Atlanta), Region 5 (Chicago), Region 6 (Dallas), Region 7 (Kansas City), Region 8 (Denver), Region 9 (San Francisco), and Region 10 (Seattle).
† Surveillance Data, Inc. (SDI), a private company that conducts RSV surveillance with support from MedImmune, Inc. (Gaithersburg, Maryland), contributes laboratory data to NREVSS.
What is already known of this topic?
The respiratory syncytial virus (RSV) season generally begins during the fall and continues through the winter and spring months, but the exact timing of RSV circulation can vary by location and year.
What is added by this report?
This report describes the timing of the two most recent RSV seasons: for 2008--09, the season onset for the 10 U.S. Health and Human Services (HHS) regions, excluding Florida, occurred from mid-October to late December and in mid-July in Florida, and offset occurred from mid-February to mid-April; in the current 2009--10 season, onset occurred in all 10 HHS regions by February 20, 2010.
What are the implications for public health practice?
The timing of RSV season was similar to previous reports and again demonstrated the variation in onset, offset, and duration by HHS regions and Florida; knowledge of RSV seasonality can be used by clinicians and public health officials to determine when to consider RSV as a cause of acute respiratory illnesses and when to provide RSV immunoprophylaxis to children at high risk for serious disease.
FIGURE. Duration of respiratory syncytial virus season, by U.S. Department of Health and Human Services region* and Florida --- National Respiratory and Enteric Virus Surveillance System, July 2008--June 2009
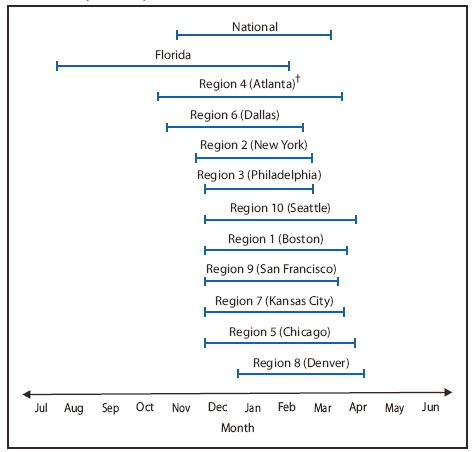
* Listed by region number and headquarters city. Region 1 (Boston): Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, and Vermont. Region 2 (New York): New Jersey and New York. Region 3 (Philadelphia): Delaware, District of Columbia, Maryland, Pennsylvania, Virginia, and West Virginia. Region 4 (Atlanta): Alabama, Florida, Georgia, Kentucky, Mississippi, North Carolina, South Carolina, and Tennessee. Region 5 (Chicago): Illinois, Indiana, Michigan, Minnesota, Ohio, and Wisconsin. Region 6 (Dallas): Arkansas, Louisiana, New Mexico, Oklahoma, and Texas. Region 7 (Kansas City): Iowa, Kansas, Missouri, and Nebraska. Region 8 (Denver): Colorado, Montana, North Dakota, South Dakota, Utah, and Wyoming. Region 9 (San Francisco): Arizona, California, Hawaii, and Nevada. Region 10 (Seattle): Alaska, Idaho, Oregon, and Washington. Maine, New Hampshire, District of Columbia, New Mexico, Nebraska, Montana, and Idaho did not have any participating laboratories in the 2008--09 season analysis.
† Excludes data from Florida.
Alternate Text: The figure above shows the duration of respiratory syncytial virus season, by U.S. Department of Health and Human Services (HHS) region and Florida derived from the National Respiratory and Enteric Virus Surveillance System, reporting for July 2008-June 2009. The 2008-09 season onset for all 10 HHS regions, excluding Florida, ranged from mid-October (week ending October 11, 2008) to late-December (week ending December 27, 2008).
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


