About Child & Teen BMI
Body mass index (BMI) is a person’s weight in kilograms divided by the square of height in meters. It is an inexpensive and easy way to screen for weight categories that may lead to health problems. For children and teens, BMI is age- and sex-specific and is often referred to as BMI-for-age.
Regardless of the current BMI-for-age category, help your child or teen develop healthy weight habits and talk with your doctor or other healthcare provider as part of ongoing tracking of BMI-for-age. If your child has significant weight loss or gain, he or she should be referred to and guided by a doctor or other healthcare provider.
Tracking growth patterns over time can help you make sure your child is achieving or maintaining a healthy weight. A single BMI-for-age calculation is not enough to evaluate long-term weight status because your child’s height and weight will change as they grow. With individuals, health care providers should consider BMI along with other factors such as family history, blood pressure, blood sugar levels, and eating patterns and physical activity level.
- What are the health consequences of obesity during childhood and what can adults do about it?
- How is BMI calculated for children and teens?
- What is a BMI percentile and how is it interpreted?
- How is BMI used with children and teens?
- Is BMI interpreted the same way for children and teens as it is for adults?
- Why can’t healthy weight ranges be provided for children and teens like they are for adults?
- How can I tell if my child is overweight or has obesity?
- Can I determine if my child or teen has obesity by using an adult BMI calculator?
- My two children have the same BMI values, but their healthcare provider considered one to have obesity and the other to not. Why is that?
- If an athlete or other person with a lot of muscle has a high BMI, is that person still considered overweight?
What are the health consequences of obesity during childhood and what can adults do about it?
Obesity during childhood can harm the body in a variety of ways, now and in the future. Learn more about the health consequences of obesity for children.
To help reduce the health risks associated with having obesity during childhood, encourage children and teens to practice healthy habits by:
- Eating healthy food and drinking plenty of water.
- Making mealtimes a family affair. Have your children help with cooking and let them choose healthy foods as well.
- Helping children find a physical activity they enjoy and participating in physical activity on most (preferably all) days of the week.
- Getting adequate sleep.
- Limiting screen time.
- Taking time for self-care and stress reduction. Try strategies like breathing exercises, meditation, yoga, and journaling.
For more information, see Tips to Promote Healthy Eating and Physical Activity for Children and Teens.
How is BMI calculated for children and teens?
Calculating BMI using the BMI Percentile Calculator involves the following steps:
- Measure height and weight. Refer to Measuring Children’s Height and Weight Accurately At Home for guidance.
- Use the Child and Teen BMI Calculator to calculate BMI. The BMI number is calculated using standard formulas.
What is a BMI percentile and how is it interpreted?
After BMI is calculated for children and teens, it is expressed as a percentile obtained from either a graph for boys [PDF-62.4KB] and girls [PDF-67.9KB] or a percentile calculator. These percentiles express a child’s BMI relative to US children who participated in national surveys from 1963-65 to 1988-944. Weight and height change during children’s growth and development, as does their relation to body fatness. Consequently, a child’s BMI must be interpreted relative to other children of the same sex and age.
The BMI-for-age percentile growth charts are the most commonly used indicator to measure the size and growth patterns of children and teens in the United States. BMI-for-age weight status categories and the corresponding percentiles were based on expert committee recommendations and are shown in the following table.
| Weight Status Category | Percentile Range |
| Underweight | Less than the 5th percentile |
| Healthy Weight | 5th percentile to less than the 85th percentile |
| Overweight | 85th to less than the 95th percentile |
| Obesity | Equal to or greater than the 95th percentile |
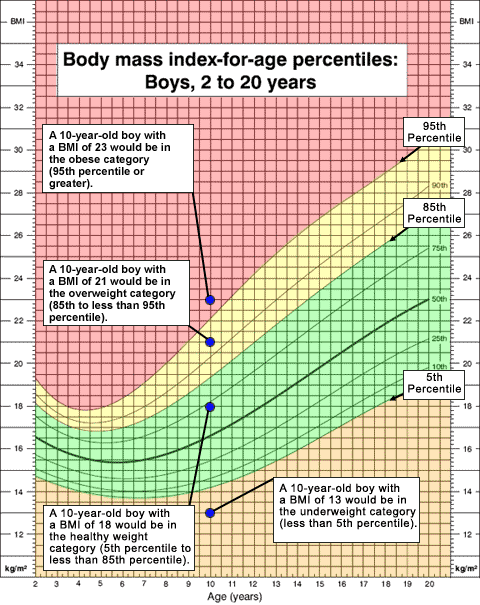
The following is an example of how sample BMI numbers would be interpreted for a 10-year-old boy.
The CDC BMI-for-age growth charts are available at: CDC Growth Charts: United States.
How is BMI used with children and teens?
For children and teens, BMI screens for potential weight and health-related issues. If children or teens have a high BMI for their age and sex, a health care provider may perform further assessments such as skinfold thickness measurements, and evaluations of family history, eating patterns, and physical activity. The American Academy of Pediatrics recommends using BMI to screen for overweight and obesity in children beginning at 2 years old. For children under the age of 2 years old, consult the World Health Organization (WHO) standards.
Children and teen’s BMI-for-age should be checked at least once a year, but a healthcare provider may check it more often. Tracking growth patterns over time can help make sure a child or teen is achieving or maintaining a healthy weight. A single BMI-for-age calculation is not enough to evaluate long-term weight status because children and teen’s height and weight will change as they grow.
Is BMI interpreted the same way for children and teens as it is for adults?
BMI is interpreted differently for children and teens even though it is calculated with the same formula. Due to changes in weight and height with age, as well as their relation to body fatness, BMI levels among children and teens are expressed relative to other children of the same sex and age. These percentiles are calculated from the CDC growth charts, which were based on national survey data collected from 1963-65 to 1988-944.
Obesity is defined as a BMI at or above the 95th percentile for children and teens of the same age and sex. For example, a 10-year-old boy of average height (56 inches) who weighs 102 pounds would have a BMI of 22.9 kg/m2. This would place the boy in the 95th percentile for BMI, and he would be considered to have obesity. This means that the child’s BMI is greater than the BMI of 95% of 10-year-old boys in the reference population.
Access the CDC Growth Charts.
For adults, BMI is interpreted as weight status categories that are not dependent on sex or age. Read more: How to interpret BMI for adult BMI
Why can’t healthy weight ranges be provided for children and teens like they are for adults?
For children and teens, healthy weight status is based on BMI between the 5th and 85th percentile on the CDC growth charts. It is difficult to provide healthy weight ranges for children and teens because the interpretation of BMI depends on weight, height, age, and sex. For adults, the interpretation of BMI depends only on height and weight.
How can I tell if my child is overweight or has obesity?
Overweight is defined as a BMI in the 85th to less than the 95th percentile. Obesity is defined as a BMI at or above the 95th percentile for children and teens of the same age and sex.
For information on helping children maintain a healthy weight, see Tips for Parents – Ideas and Tips to Help Prevent Childhood Obesity.
Can I determine if my child or teen has obesity by using an adult BMI calculator?
People 20 years old and older should use the Adult BMI Calculator. The adult calculator provides only the BMI value and not the BMI percentile. Consequently, it is not appropriate to use the adult BMI calculator to assess the BMI of children and teens.
My two children have the same BMI values, but their healthcare provider considered one to have obesity and the other to not. Why is that?
The interpretation of BMI varies by age and sex. So, if the children are not the same age and the same sex, the interpretation of BMI has different meanings.
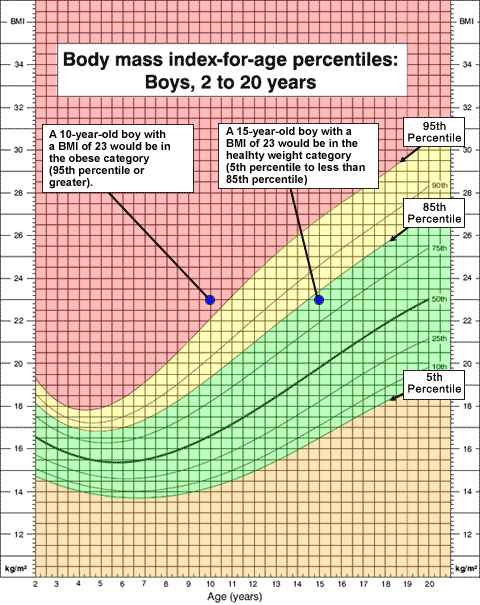
See the following illustration for a 10-year-old boy and a 15-year-old boy who both have a BMI-for-age of 23. (Note that two children of different ages are plotted on the same growth chart to illustrate a point. Normally the measurement for only one child is plotted on a growth chart.)
If an athlete or other person with a lot of muscle has a high BMI, is that person still considered overweight?
Athletes may have a high BMI because of increased muscularity rather than increased body fatness. A trained healthcare provider can perform appropriate health assessments to evaluate an individual’s health status and risks. Because no single body fat measure clearly distinguishes health from disease or identifies risk of disease, BMI should serve as the initial screening. Other factors, such as fat distribution, genetics, diet, and fitness level contribute to an individual’s disease risk.
References
1Garrow, J.S. & Webster, J., 1985. Quetelet’s index (W/H2) as a measure of fatness. Int. J. Obes., 9(2), pp.147–153.
2Freedman, D.S., Horlick, M. & Berenson, G.S., 2013. A comparison of the Slaughter skinfold-thickness equations and BMI in predicting body fatness and cardiovascular disease risk factor levels in children. Am. J. Clin. Nutr., 98(6), pp.1417–24.
3Wohlfahrt-Veje, C. et al., 2014. Body fat throughout childhood in 2647 healthy Danish children: agreement of BMI, waist circumference, skinfolds with dual X-ray absorptiometry. Eur. J. Clin. Nutr., 68(6), pp.664–70.
4Kuczmarski, R.J. et al., 2002. 2000 CDC Growth Charts for the United States: methods and development. Vital Health Stat. 11., 11(246), pp.1–190.