Global Polio Eradication
Updated December 1, 2023
Polio Cases Have Decreased by More than 99%
In 1988, the World Health Assembly passed a resolution to eradicate polio, leading to the establishment of the Global Polio Eradication Initiative (GPEI). As a result, partners including CDC are working together to ensure that every child receives several doses of polio vaccine.
Since the launch of GPEI, polio cases have decreased by more than 99%. In addition, polio vaccines have prevented an estimated 20 million cases of paralysis in children since 1988.
Vaccines have stopped the spread of wild poliovirus in all but two countries: Afghanistan and Pakistan. However, other countries have experienced outbreaks of poliovirus variants, which can emerge in areas where immunization rates are low.
GPEI set a goal of ending all types of polio in 2023 and is working to address barriers to reaching this goal. Because of the COVID-19 pandemic, routine childhood immunization programs and global polio vaccination campaigns were disrupted. GPEI is working to increase global polio vaccination to make up for lost ground.
Success in eradicating polio will mean that no more children will have to experience the devastating effects of the disease. Failure to eradicate polio could cause poliovirus to reappear around the world with an estimated 150,000-200,000 new cases expected every year within 10 years.
Two Types of Vaccines are Available to Prevent Polio
Two types of vaccines are used to prevent global polio: oral polio vaccines (OPV) and inactivated polio vaccines (IPV), which are given as an injection.
OPV is the vaccine most used globally and is needed in the fight to eradicate polio, which is more likely to spread in areas with poor access to hand-washing and sanitation. In those settings, OPV offers an inexpensive and efficient solution for immunizing populations against polio.
The advantages of using OPV include:
- Oral polio vaccines do not have to be injected. This makes it easier for countries to give multiple doses of oral polio vaccines to all children, using trained volunteers. It also allows countries to combine polio vaccine campaigns with other public health interventions, like vitamin A supplementation, which helps reduce disease and death among children without access to complete nutrition.
- Oral polio vaccines create intestinal tract immunity that helps block the spread of poliovirus in those who receive the vaccine, while inactivated polio vaccine does not.
- Oral polio vaccines help create contact immunity, which means that people in close contact with a person who received the vaccine can become immune to poliovirus, even without being vaccinated themselves.
- Oral polio vaccines are considered to be safe and effective overall, having met rigorous standards set by international health authorities.
Since 2000, only IPV has been used in the U.S. Learn more about polio vaccination in the U.S.
Polio Eradication is Possible
It is possible to eradicate polio. However, significant challenges remain in reaching this goal.
As long as wild poliovirus continues to circulate in Afghanistan and Pakistan, all countries are at risk of wild poliovirus being imported. For example, an outbreak of wild poliovirus (imported from Pakistan) occurred in Southeastern Africa in 2021 and 2022. Ongoing conflicts and competing health priorities in these countries make it challenging to vaccinate all children.
In some other countries, poliovirus variants (also known as vaccine-derived poliovirus) present an additional challenge. Variant poliovirus outbreaks emerge when not enough children are vaccinated against polio.
Three actions are urgently needed to end polio once and for all:
- Strengthen routine polio immunization, ensuring all infants receive several doses of polio vaccines before one year of age.
- Detect polio cases in a timely manner.
- Rapidly respond to outbreaks with high-quality vaccination campaigns.
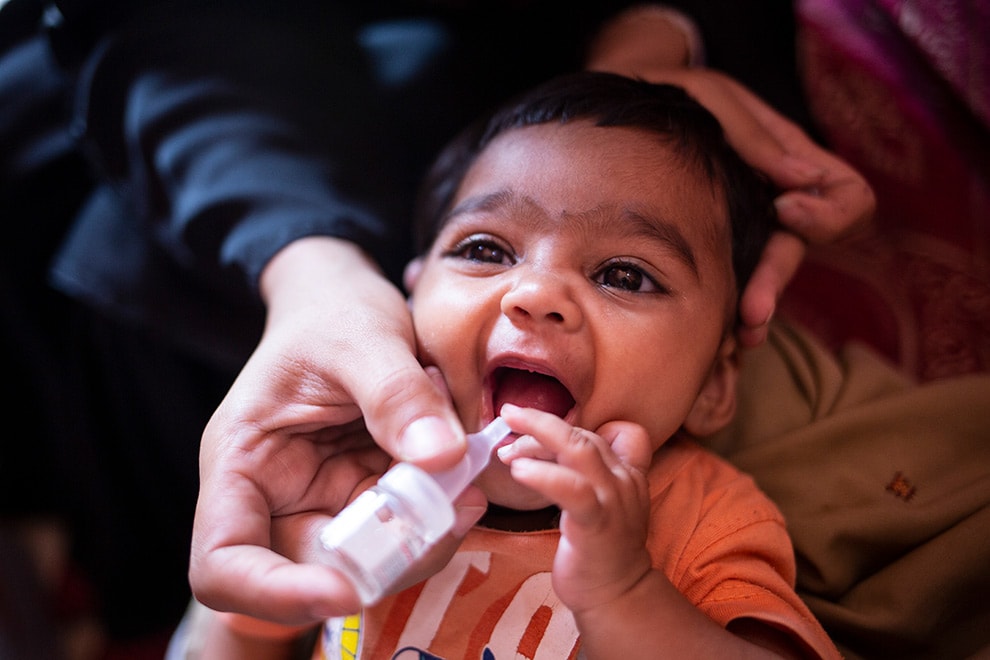
An infant in Pakistan gets an oral polio vaccine. Pakistan and Afghanistan are the only countries in the world where wild poliovirus is still endemic (consistently present). Credit: ©UNICEF/U.S. CDC/UN0828390/Bashir
More information from the Global Polio Eradication Initiative (GPEI):