Purpose
Efforts to improve the drowning-related syndromes in ESSENCE led to the discovery of some interesting seasonal trends when applied to de-identified national data over a one-year period. Epidemiologists and data analysts are encouraged to apply these learnings in their own jurisdictions. The code definition can easily be tailored to include local bodies of water.

A leading cause of unintentional injury death
Drowning ranks fifth among the leading causes of unintentional injury death in the United States, with an average of 3,536 fatal unintentional non-boating drownings per year in the United States from 2005 through 2014. About 20% of these deaths occur in children 14 years of age and younger. For every child who dies from drowning, another five receive emergency department (ED) care for their submersion injuries.1
Following the process outlined in the International Society of Disease Surveillance (ISDS) Syndrome Definition Committee's recently published Developing, Evaluating, and Disseminating Definitions for Syndromic Surveillance in Public Health Practice: A Guidance Document,2 this article describes how the NSSP team assessed whether drowning and submersion surveillance queries in ESSENCE could be improved.
Background: existing syndromes
This work by NSSP began as a side project in 2018 to test the viability of and to improve drowning-related syndromes in ESSENCE. At the time, the only available syndrome was the ESSENCE Chief Complaint SubSyndrome "DrowningOrSubmersion." This syndrome uses the Chief Complaint field, searching for one or more of the following terms: DROWN, DROWNED, DROWNING, SUBMERSION, SUBMERGE, or UNDER WATER.
This DrowningOrSubmersion ESSENCE SubSyndrome does not leverage other fields and sometimes captures a few false positives and misses true drowning or submersion visits. Keep in mind, however, that the subsyndrome in ESSENCE captures intended ED visits quite well. In this walkthrough, we are improving upon an already successful syndrome definition.
Scope and purpose
Improvements to the drowning-related query are intended to supplement injury prevention work and more accurately track drowning-related injury trends. The goals are to limit false positives present in the existing subsyndrome returns and leverage other fields to increase accurate visit counts. This query should work on the nationwide de-identified ESSENCE Chief Complaint Query Validation (CCQV) data and function in existing syndromic surveillance systems across most states and public health jurisdictions. To further encourage use, the query will be executed in the CCDD field, a concatenation of the ESSENCE-processed Chief Complaint and the Discharge Diagnosis fields.
More query help
Components
Drowning-related discharge diagnosis codes include:
- W16.__1—W16 codes for any external cause of morbidity involving a fall, jump, or dive into specific types of water. The 1 in the 6th place of this code indicates an external cause led to drowning or submersion
- W16.[49]1X—W16 codes that end with 41X or 91X involve fall, jump, or dive into unspecified water
- Y21—This is an event of undetermined intent code involving drowning and submersion
- X71— Intentional self-harm by drowning and submersion
- V90—Drowning and submersion due to accident to watercraft
- W65—Accidental drowning and submersion while in bathtub
- W67—Accidental drowning and submersion while in swimming pool
- W69—Accidental drowning and submersion while in natural water
- W73—Other specified cause of accidental non-transport drowning and submersion
- W74—Unspecified cause of accidental drowning and submersion
- X92—Assault by drowning and submersion
- W22.041—Striking against wall of swimming pool causing drowning and submersion
- V92—Drowning and submersion due to accident on board watercraft
- T75.1—Unspecified effects of drowning and nonfatal submersion
SNOMED codes for drowning and submersion events have not yet been assessed for this query.
Keywords
The subsyndrome already in use provided an excellent starting point. We looked at the two terms that have a major influence over how data returns for this syndrome: DROWN and SUBMER.
- SUBMER appears to work very well. After a quick review, we noticed some false positives but nearly all true positives.
- DROWN (when searched as a free-text query) already negates some false positives that are artifacts of the way ESSENCE's fuzzy-matching algorithms work. These are, for example, false positives from Chief Complaints like "molar recently CROWNED" or misspelled words like "patient DROWSING from meds." Two other negations were selected for common false positives: FEEL DROWN and FELT DROWN.
Next, we reviewed CCQV data to identify other drowning-related key terms. We focused on text contained in positive visit data and other Chief Complaint text indicating possible drownings, submersion, and related location or activities.
- BOTTOM OF POOL—A lot of unintended visits are due to patients hitting their heads on the bottom of a pool. Most true positive visits already have a positive ICD-10 code. What seems to capture the rest is the code ^FOUND^BOTTOM^POOL^ or ^NOTE^BOTTOM^POOL^.
- WATER IN LUNGS—The code ^WATER^LUNG^ returns a lot of visits (878), and a quick review revealed that most are not the visit types we intend to capture. Also, the crossover between WATER^LUNGS and the identified ICD-10 is only 35 (4%) ED visits across CCQV data from January through November 2018. For reference, the term ^SUBMER^ returns 737 visits during the same period, and the crossover between these data and the ICD-10 positive visits is 363 (49%). We chose to not include this term because it pulls too many false positives, and the likelihood that a portion of true-positives will be captured by other terms and codes.
- UNRESPONSIVE IN POOL—The code ^UNRESPONSIVE^,and,^POOL^ doesn't return many visits. After removing ICD-10-positive cases and spot-checking the remaining data, about half the returned visits referred to a true pool accident whereas the half referred to a pool of bodily fluids. We decided not to use this term.
- UNDERWATER—The code ^Under^Water^ returns a lot of false positives. Most true positives were already picked up by the ICD-10 portion. A lower false positive count can be achieved with the code ^UNDER^WATER^,and,(,^TUB^,or,^POOL^,or,^BATH^,or,^SWIM^,or,^LAKE^,or,^POND^,or,^OCEAN^,or,^WAVE^,).
- INHALED WATER —The code ^INHALE^WATER^ appears to be working all right, but improvements were made similar to the UNDERWATER term to create ^WATER^,and,^INHAL^,and,(,^TUB^,or,^POOL^,or,^BATH^,or,^SWIM^,or,^LAKE^,or,^POND^,or,^OCEAN^,or,^WAVE^,).
- SINK—This term brings up an excessive number of bathroom sinks and is not a good term for the intent of this query.
- FOUND POOL, TUB, BATH, SWIM—A brief review of the returns for these terms showed a lot of false positives. Other than the already discussed ^FOUND^BOTTOM^POOL^ or ^NOTE^BOTTOM^POOL^, these terms were excluded.
We encourage others to tailor this definition to the types of bodies of water in their regions. Some ideas could be assessing terms like Rocks, Logs, Rip Tides, Currents, Rivers, and Creeks.
Putting it together
(,^DROWN^,andnot,(,^FEEL^DROWN^,or,^FELT^DROWN^,),),or,(,(,^NOTE^,or,^FOUND^,),and,^BOTTOM^,and,^POOL^,),or,(,(,(,^UNDER^WATER^,),or,(,^WATER^,and,^INHAL^,),),and,(,^TUB^,or,^POOL^,or,^BATH^,or,^SWIM^,or,^LAKE^,or,^POND^,or,^OCEAN^,or,^WAVE^,),),or,(,^[;/ ]W16.__1^,or,^[;/ ]W22.041^,or,^[;/ ]T75.1^,or,^[;/ ]W16[0-9]_1^,or,^W16.[49]1X^,or,^W16[49]1X^,or,^[;/ ]W22041^,or,[;/ ]^T751^,or,^[;/ ]Y21^,or,^[;/ ]X71^,or,^[;/ ]V90^,or,^W6[579]^,or,^[;/ ]W7[34]^,or,^[;/ ]X92^,or,^[;/ ]V92^,)
Vital resource
Reviewing the syndrome
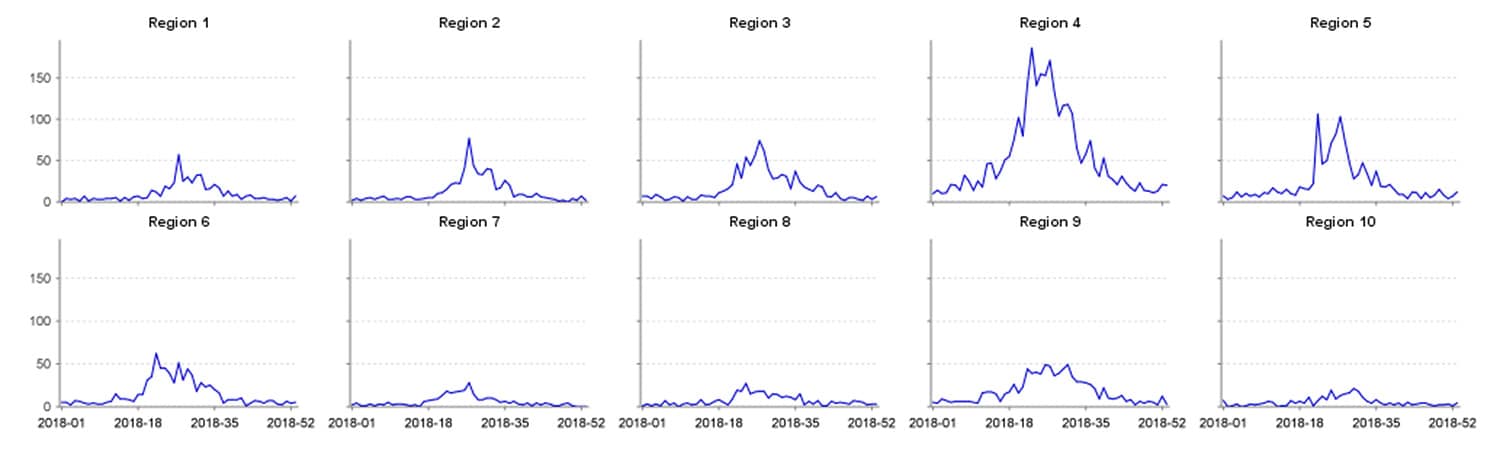
The syndrome, with all its subsequent parts, gives an interesting seasonal trend when applied to weekly CCQV data through 2018, showing a sharp incline starting near the end of April and a peak occurring the first week of July. Following the July peak, the trend slowly declines into the winter months with a baseline of around 50 visits per week. Six separate weeks of CCQV data (January–November 2018) were randomly selected and visits manually reviewed. We selected MMWR weeks 1, 13, 17, 19, 27, and 32, and visits for the six weeks totaled 1,205. Of these visits, 1,156 (96%) were deemed true positives, 44 (4%) were likely false positives, and five visits were undetermined. There were no trends in false positive returns that lent themselves to easy negation.
From this point forward, we reached the steps in the SDC guidance document that advise "further refinement followed by dissemination of this query." The feedback we receive from the community will help determine our next steps toward improving this syndrome definition. We encourage epidemiologists and data analysts in different public health jurisdictions to experiment with this preliminary work and modify the code above to suit different needs. This syndrome was developed on de-identified national data. We encourage others to tailor this definition to the types of bodies of water in their region.
This article about syndrome definitions was written by Senior Data Analyst Zachary Stein, a specialist in syndromic surveillance and a contributing author to Developing, Evaluating, and Disseminating Definitions for Syndromic Surveillance in Public Health Practice: A Guidance Document. Stein is an avid outdoorsman who spends a lot of time on the water and has personal experience with drowning-related scares. He believes that drowning injuries are an excellent opportunity for public health education and intervention, especially among younger populations. Injuries related to drowning are highly likely to present at an emergency department and are opportunities for syndromic surveillance to bolster existing public health prevention activities.
