Translation Research
Translation research explores how scientific work moves into practice and benefits society. Although this new field of research has not received much attention in occupational safety and health, it can have a valuable impact on workers everywhere. Today’s workplaces need research findings and products that can improve the quality of life, health, and work. Through translation research, NIOSH studies the process, drivers, and barriers for turning knowledge into practical applications that create these improvements for the safety and health of workers.
Translation researchers apply scientific investigative approaches to study how the outputs of basic and applied research can be effectively translated into practice and have an impact. This includes studying how knowledge and interventions are spread, accepted, applied, and institutionalized.
Activities in translation research range across the basic-to-applied continuum, and studies referred to as intervention research and translation research often overlap. NIOSH delineates the two in this way: intervention research involves improving an intervention or designing a new one, whereas translation research involves studying processes for putting research outputs into practice or use. These processes can include activities such as efficacy research (testing interventions in a realistic setting) and effectiveness research (testing interventions in a wide range of settings). Translation research also includes limited proof-of-concept testing and large-scale studies of research outputs and their impact.
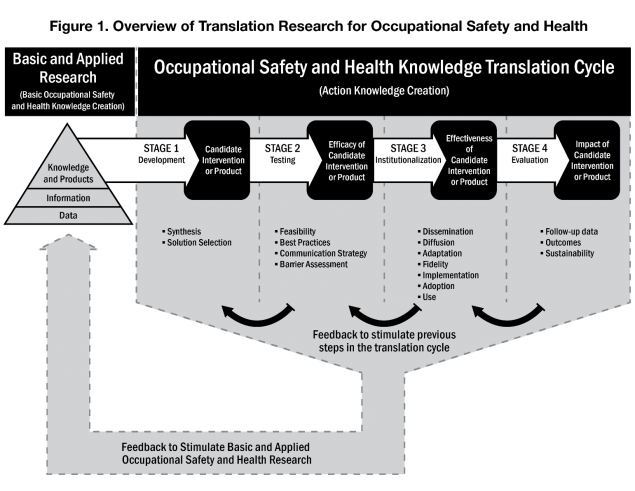
Translation research has four stages (Table 1):
- Stage 1, development translation research, studies how a discovery made in a laboratory, field or pilot study or findings of risks, can move into a potential health and safety application to be tested.
- Stage 2, testing translation research, assesses the value of a new finding, invention, process, training program, or intervention. It looks for larger-scale workplace safety and health practices aimed at a specific work sector or across two or more work sectors.
- Stage 3, institutionalization translation research, studies how evidence-based technology and recommendations become well-accepted workplace safety and health practices that are communicated and used on a large scale.
- Stage 4, evaluation translation research, explores the “real world” health benefits and effects of moving these discoveries and interventions into large-scale practice. This phase examines impact over time through ongoing surveillance and evaluation.
Table 1. Examples of Translation Research for Different Types of Hazards
| Problem/Hazard | Stage | ||||
| 0* Hazard/Problem Identification |
1 Development | 2 Testing | 3 Institutionalization | 4 Evaluation | |
| Physical Agent: Noise-Induced Hearing Loss |
Occupational noise–induced hearing loss [1] |
Development of protocol for testing hearing protection devices [2] |
Hearing protector effectiveness study [3], [4] |
Identifying attitude and behaviors associated with wearing hearing protection [5] |
Impact of hearing conservation on incidence of hearing loss [6], [7] |
| Hazardous Substance: Silicosis in Mining |
Identification of silicosis in mining [8] |
Development of an intervention [9] |
Testing worker response to intervention [10] |
Development of guidelines for widespread use [11] |
Utilization of on-going or new surveillance data to determine impact |
| Psychosocial Hazard: Stress |
Identification of stress hazards in healthcare workers [12] |
Development of interventions in healthcare [13] |
Testing the effects of modifying the psychosocial work environment [14] |
Systematic review of effectiveness of various interventions [15] |
Surveillance [16] |
| Safety Hazard: Winch Entanglements Resulting in Severe Traumatic Injuries and Fatalities |
Identification of injuries involving winches [17] |
Development of ancillary stopping switch [18], [19] |
Testing interventions in target users [20] |
Examining methods of implementation [21] |
Surveillance of injuries [22] |
* Stage 0 is the basic or applied research finding that becomes the focus for study in Stages 1–4 of the translation research framework. It is not part of that framework.
The translation research process should be a never-ending loop of research and translation, allowing for ongoing integration of effective approaches. This focus on improving the implementation of science shows NIOSH’s value as the nation’s primary occupational safety and health research institute. Translation research findings add great value to occupational safety and health research by helping us understand how science can better achieve practical benefits and what factors stand in the way of scientific work leading to useful outcomes. Translation research reveals how discoveries and guidance improve the lives of workers.
The phrases translation research, translational research, and translational science have been used to describe the systematic effort to convert basic research outputs into practical applications to enhance human health and well-being. Generally, these uses of the phrase translational research refer to harnessing knowledge from basic medical science and bringing it into clinical practice (so-called bench-to-bedside models). In contrast, NIOSH defines the phrase translation research to refer to the study of the process of moving “research-to-practice-to-impact” and the methods, barriers and facilitators, context, and issues encountered in this process. However, in the scientific literature, the two descriptors of research—translation versus translational—overlap.
In 2016 NIOSH developed a framework for a wide-ranging plan for translation research. The plan will help NIOSH study how to move research findings into practice as quickly as possible, to improve worker safety.
NIOSH created its Translation Research Program to nurture, promote, and coordinate translation research and to more effectively transform science into useful actions and products. Translation research explores the processes by which research findings are successfully implemented in the workplace.
Compared with other workplace safety and health efforts, translation research is a new field without a large base of scientific papers. The program builds on previous NIOSH health communication work and research into effective interventions. It also includes research on social and behavioral science topics and on how scientific innovations spread and become practical benefits to society.
The research-to-practice process starts with research and ends with useful innovations. The Translation Research Program’s efforts focus on the research-to-practice continuum to learn how to make any given step better and how to improve its impact. The goal is to develop relevant, widely applied knowledge that creates a safer and healthier work environment.
This work faces challenges, however:
- Identifying translation research priorities, to focus limited resources yet achieve maximum impact
- Focusing on how decision-makers get and use workplace safety and health information, as well as barriers that prevent such information from reaching those who need it
- Finding which approaches work best in making safety and health research products that will have the most effective benefits.
NIOSH continues to gather translation research, promote goals for internal research competitions, and develop the skills of staff. Its work outside the institute may include offering dedicated funding opportunities and developing and promoting training for translation research.
Publications which have guided the development of the NIOSH Translation Research Program include the following:
- Schulte PA; Cunningham TR; Nickels L; Felknor S; Guerin R; Blosser F; Chang C-C; Check P; Eggerth D; Flynn M; Forrester C; Hard D; Hudson H; Lincoln J; McKernan LT; Pratap P; Stephenson CM; Van Bogaert D; Menger-Ogle L [2017]. Translation research in occupational safety and health: a proposed framework. Am J Ind Med 2017 Dec; 60(12):1011-1022.
- Dugan, A.G. & Punnett, L. Dissemination and Implementation Research for Occupational Safety and Health. Occup Health Sci (2017) 1: 29.
- Tinc PJ, Gadomski A, Sorensen JA, Weinehall L, Jenkins P, Lindvall K. Adapting the T0-T4 implementation science model to occupational health and safety in agriculture, forestry, and fishing: A scoping review. Am J Ind Med. 2018;61:51–62.
- Khoury MJ, Gwinn M, Ioannidis JPA [2010]. The emergence of translational epidemiology: from scientific discovery to population health impact. American Journal Epidemiology 172: 517-524.
- Lucas DL, Kincl LD, Bovbjerg VE and Lincoln JM [2014]. Application of a translational research model to assess the progress of occupational safety research in the international commercial fishing industry. Safety Science 64:71-81.
- Ogilvie D, Craig P, Griffin S, Macintyre S and Wareham NJ [2009]. A translational framework for public health research. BMC Public Health 9(1):116.
- NIOSH Translation Research Roadmap and Implementation presentation to the Board of Scientific Counselors Meeting, March 2016
- Hager LD. BLS occupational hearing loss report for 2007. CAOHC Update. 2009; 21: 7-9.
- Berger EH, Franks JR, Behar A, et al. Development of a new standard laboratory protocol for estimating field attenuation of hearing protection devices. Part III. The validity of using subject-fit data. J Acoust Soc Am. 1998; 103: 665-672.
- Berger EH, Franks JR, Behar A, et al. Development of a new standard laboratory protocol for estimating field attenuation of hearing protection devices. Part III. The validity of using subject-fit data. J Acoust Soc Am. 1998; 103: 665-672.
- Murphy WJ, Davis RR, Byrne DC, Franks JR. Advanced hearing protector study. Cincinnati, OH: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, NIOSH EPHB Report No. 312-11a; 2007. https://ntrl.ntis.gov/NTRL/dashboard/searchResults/titleDetail/PB2008113769.xhtml
- Stephenson CM, Stephenson MR. Hearing loss prevention for carpenters. Part 1-using health communication and health promotion models to develop training that works. Noise Health.2011; 13: 113-121.
- Davies H, Marion S, Teschke K. The impact of hearing conservation programs on incidence of noise-induced hearing loss in Canadian workers. Am J Ind Med.2008; 51: 923-931.
- Masterson EA, Deddens JA, Themann CL, Bertke S, Calvert GM. Trends in worker hearing loss by industry sector, 1981-2010. Am J Ind Med. 2015; 58: 392-401.
- Wagner GR. The inexcusable persistence of silicosis. Am J Public Health. 2005; 85: 1346-1347. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1615617/
- Cecala AB, O’Brien AD. Here comes the Helmet-CAM: A recent advance in technology can improve how mine operators investigate and assess respirable dust. Rock Prod. 2014; 117: 26-30.
- Haas EJ, Willmer D., Cecala AB. Formative research to reduce mine worker respirable silica dust exposure: A feasibility study to integrate technology into behavioral interventions. Pilot Feasibility Study. 2016; 2: 6.
- Reed WR, Kwitowski AJ, Helfrich WJ, Cecala AB, Joy GJ. Guidelines for performing a helmet-CAM respirable dust survey and conducting subsequent analysis with the Enhanced Video Analysis of Dust Exposures (EVADE) software. Pittsburgh, PA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, DHHS, (NIOSH) Publication No. 2014-133; 2014. https://www.cdc.gov/niosh/mining/UserFiles/works/pdfs/2014-133.pdf
- Bourbonnais R, Comeau M, Vézina M. Job strain and evolution of mental health among nurses. J Occup Health Psychol. 1999; 4: 92-107.
- Bourbonnais R, Brisson C, Vinet A, Vézina M, Lower A. Development and implementation of a participative intervention to improve the psychosocial work environment and mental health in an acute care hospital. Occup Environ Med. 2006; 63: 326-334.
- Jimmieson NL, Hobman EV, Tucker MK, Bordia P. Change in psychosocial work factors predicts follow-up employee strain: An examination of Australian employees. J Occup Environ Med. 2016; 58: 1002-1013.
- Ruotsalainen JH, Verbeek JH, Mariné A, Serra C. Preventing occupational stress in healthcare workers. Cochrane Database Syst Rev. 2015; 4: D002892.
- Dollard M, Skinner N, Tuckey MR, Bailey T. National surveillance of psychosocial risk factors in the workplace: An international overview. Work Stress. 2997; 21: 1-29.
- NIOSH. Commercial fishing vessel shipper dies after being pulled into a deck winch-Alaska. Anchorage, AK: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health, Fatality Assessment and Control Evaluation (FACE) Program, State FACE Reports-Alaska: Report No. FACE AK-95-23; 1995. https://www.cdc.gov/niosh/face/stateface/ak/95ak023.html
- Lincoln JM, Lucas DL, McKibbin RW, Woodward CC, Bevan JE. Reducing commercial fishing deck hazards with engineering solutions for winch design. J Safety Res. 2008; 39: 231-235.
- Lincoln JM, Woodward CC, King GW, Case SL, Lucas DL, Teske TD. Preventing fatal winch entanglements in the US southern shrimp fleet: A research to practice approach. J Safety Res. 2017; 60: 119-123.
- Levin JL, Gilmore K, Wickman A, et al. Workplace safety interventions for commercial fishermen of the gulf. J Agromedicine. 2016; 21: 178-189.
- Teske TD, Victoroff T. Increasing adoption of safety technologies in commercial fishing. Study in progress. Anchorage, AK: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health (NIOSH); 2017.
- CDC. Fatal and nonfatal injuries involving fishing vessel winches- Southern shrimp fleet, United States, 2000-2011. MMWR. 2013; 62: 157-160. https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6209a1.htm