National Health Care Surveys
NCHS Fact Sheet, May 2018
PDF Version (225 KB)
About NCHS
The National Center for Health Statistics (NCHS) is the nation’s principal health statistics agency, providing data to identify and address health issues. NCHS compiles statistical information to help guide public health and health policy decisions.
Collaborating with other public and private health partners, NCHS uses a variety of data collection mechanisms to obtain accurate information from multiple sources. This process provides a broad perspective on the population’s health, influences on health, and health outcomes.
National Health Care Surveys
The National Health Care Surveys are a group of surveys designed to provide information about the organizations and providers that deliver health care, the services rendered, and the patients served across diverse settings. Provider sites surveyed include doctors’ offices, community health centers, ambulatory surgery centers, hospital outpatient and emergency departments, inpatient hospital units, assisted living and similar residential care facilities, adult day services centers, nursing homes, home health agencies, and hospice organizations.
National Health Care Surveys are used to study:
- Resource use, including staffing
- Quality of care, including patient safety
- Clinical management of specific conditions
- Disparities in use and quality of care
- Diffusion of health care technologies, including drugs, surgical procedures, and information technologies
- Effects of policy changes
Recent findings
Electronic health records or electronic medical records
The Health Information Technology for Economic and Clinical Health Act of 2009 provided incentive payments through Medicare and Medicaid to health care providers that use certified electronic health record (EHR) systems to achieve specified improvements in care delivery.
The Department of Health and Human Services Office of the National Coordinator for Health Information Technology uses NCHS data to monitor provider adoption of EHRs or electronic medical records (EMRs). In 2017, 85.9% of office-based physicians reported using any type of EHR system, while 79.7% of office-based physicians had a certified system. In regards to interoperability and sharing of patient health information, among those office-based physicians who had an EHR system, 41.7% sent patient health information electronically, 43.0% received patient health information electronically, 32.1% integrated patient information electronically, and 56.1% searched for patient health information electronically. NCHS collects data from professionals, hospitals, and critical access hospitals. Eligible providers can fulfill the Meaningful Use Program (also known as Promoting Interoperability) public health reporting requirements by participating in NCHS surveys, which results in increased response rates.
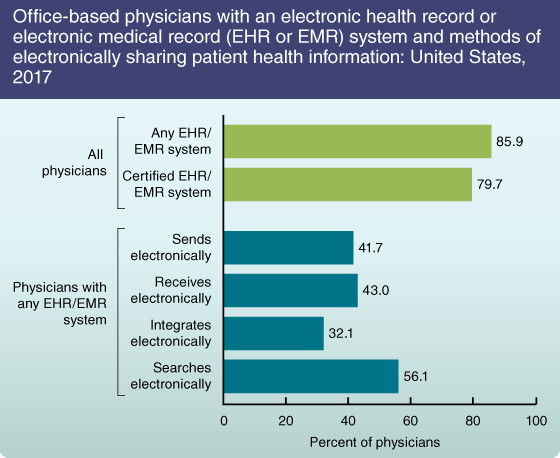
SOURCE: NCHS, National Electronic Health Records Survey, 2017.
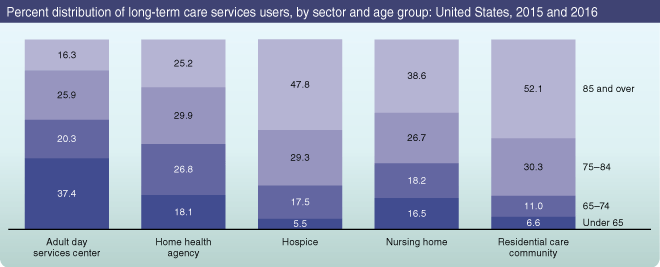
NOTE: Estimates may not add to 100 due to rounding.
SOURCE: NCHS, National Study of Long-Term Care Providers, 2015–2016.
Residential care
The majority of long-term care services users were aged 65 and over: 94.6% of hospice patients, 93.4% of residential care residents, 83.5% of nursing home residents, 81.9% of home health patients, and 62.5% of participants in adult day services centers. The age composition of services users varied by sector, with residential care communities (52.1%), hospices (47.8%), and nursing homes (38.6%) serving more persons aged 85 and over, and adult day services centers (37.4%) serving more persons under age 65 than other sectors.
Volume of emergency department visits affects wait time
Emergency department (ED) wait time is an indication of overcrowding. In 2016, mean wait times for ED treatment increased as the annual volume of visits increased. The mean wait time was 24.1 minutes in EDs with less than 20,000 annual visits, compared with 48.7 minutes in EDs with 50,000 or more annual visits.
In some hospitals, increased ED visit volume resulted in ED crowding (boarding admitted patients in hallways or other spaces), ambulance diversion, and increased wait times for minor problems and sometimes serious ones, such as myocardial infarction.
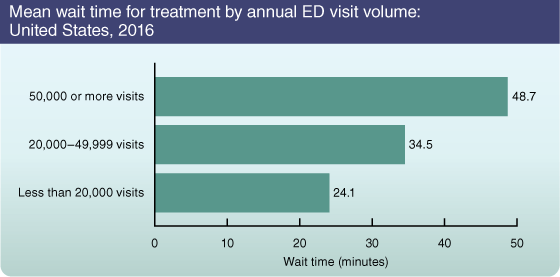
SOURCE: NCHS, National Hospital Ambulatory Medical Care Survey, 2016.
Challenges and future opportunities
- Continue to test methods of data collection of EHRs.
- Integrate existing surveys in the hospital setting to the new National Hospital Care Survey.
- Collect individual-level data on services users, expand content, and explore ways to extract data on services users in the National Study of Long-Term Care Providers.
- Expand range of providers and data currently collected for better coverage of the health care and long-term care system.
- Improve timeliness of data dissemination and reports.
- Use data in a preliminary way to address emerging health issues.
For more information about NCHS and its programs, visit https://www.cdc.gov/nchs.
For more information about National Health Care Surveys, visit https://www.cdc.gov/nchs/dhcs.htm.