Complications of Measles
Measles can be serious. Children younger than 5 years of age and adults older than 20 years of age are more likely to suffer from complications. Common complications are ear infections and diarrhea. Serious complications include pneumonia and encephalitis.
People and groups at risk of measles complications
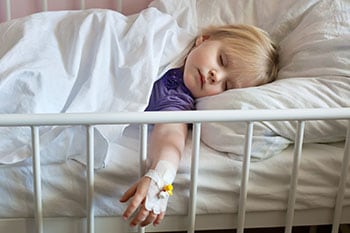
Measles can be serious in all age groups. However, there are several groups that are more likely to suffer from measles complications:
- Children younger than 5 years of age
- Adults older than 20 years of age
- Pregnant women
- People with compromised immune systems, such as from leukemia or HIV infection
Prevent measles: talk to your health provider about the measles, mumps, and rubella (MMR) vaccine.
Common complications
- Ear infections occur in about one out of every 10 children with measles.
- Diarrhea is reported in less than one out of 10 people with measles.
Severe complications in children and adults
Some people may suffer from severe complications, such as pneumonia (infection of the lungs) and encephalitis (swelling of the brain). They may need to be hospitalized and could die.

Hospitalization. About 1 in 5 unvaccinated people in the U.S. who get measles is hospitalized.
Pneumonia. As many as 1 out of every 20 children with measles gets pneumonia, the most common cause of death from measles in young children.
Encephalitis. About 1 child out of every 1,000 who get measles will develop encephalitis (swelling of the brain) that can lead to convulsions and can leave the child deaf or with intellectual disability.

Death. Nearly 1 to 3 of every 1,000 children who become infected with measles will die from respiratory and neurologic complications.
Complications during pregnancy. Measles may cause pregnant women who have not had the MMR vaccine to give birth prematurely, or have a low-birth-weight baby.
Related page: The Measles chapter of the Epidemiology and Prevention of Vaccine Preventable Diseases (Pink Book) describes measles complications in more depth.
Long-term complications
Subacute sclerosing panencephalitis (SSPE) is a very rare, but fatal disease of the central nervous system that results from a measles virus infection acquired earlier in life.
- SSPE generally develops 7 to 10 years after a person has measles, even though the person seems to have fully recovered from the illness.
- Since measles was eliminated in 2000, SSPE is rarely reported in the United States.
- Among people who contracted measles during the resurgence in the United States in 1989 to 1991, 7 to 11 out of every 100,000 were estimated to be at risk for developing SSPE.
- The risk of developing SSPE may be higher for a person who gets measles before they are 2 years of age.
- To learn more, visit the Subacute sclerosing panencephalitis (SSPE) MedlinePlus Medical Encyclopedia.

