CDC’s Public Health Laboratory Electronic Test Orders and Results Initiative
Public health laboratories and partners can request technical assistance (TA) with implementing electronic test orders and results through the Association of Public Health Laboratories’ (APHL) Technical Assistance Form or by emailing DLS_Informatics@cdc.gov.
CDC is collaborating with the nation’s public health laboratories (PHLs) and other partners to modernize data systems. CDC and its collaborators are building the technical infrastructure to facilitate the exchange of electronic test orders and results between healthcare facilities and PHLs, an activity abbreviated as “ETOR.” This multidirectional platform will streamline channels of data transmission and improve interoperability between partners. This exchange will decrease the use of paper-based test orders and reports, reducing the risk of errors in manual data entry and result reporting, and ensuring that accurate testing information is captured and transmitted to a patient’s medical record in a timely manner.
Implementing ETOR will also strengthen public health surveillance and emergency response by linking laboratory data with patient information through standardized data elements included in the test order.
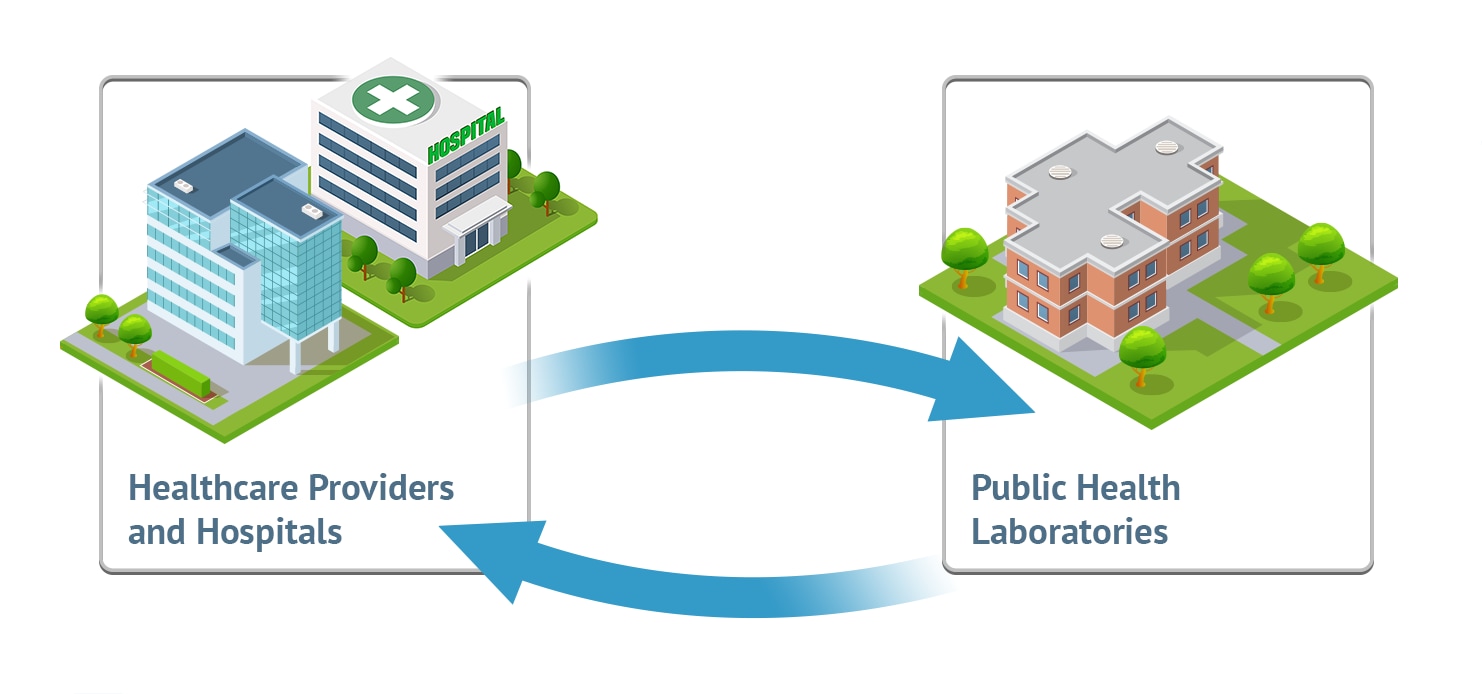
ETOR connects healthcare facilities and public health laboratories.
Healthcare providers: Learn more about how you, your practice, and your patients will benefit from ETOR in this report from CDC’s Division of Laboratory Systems, Public Health Electronic Test Orders and Results (ETOR) Initiative.
CDC is helping to establish direct data exchange between every state PHL and hospital systems in their jurisdiction through the activities listed here.
Characterizing Issues
• Gaining a better understanding of the national ETOR landscape and options for nationwide implementation
• Identifying hospitals and other clinical partners who could benefit from implementing ETOR with their PHL
Expanding Laboratories’ Use of Portals
Assisting PHLs in setting up web portals for ETOR, an easy-to-implement solution to connect low-volume submitters and to quickly respond to data needs for public health emergencies.
Enhancing Intermediaries
Frequently, one system is limited by the format of data it can send or accept, requiring an intermediary to facilitate communication between systems. CDC is working to enhance two cloud-based intermediaries, APHL Informatics Messaging Services (AIMS) and CDC’s ReportStream, to centralize, standardize, and translate messages (orders and results) between healthcare providers and PHLs.
Funding Activities
• Funding contractors to provide requested TA to clinical partners
• Funding APHL to provide TA to PHLs
• Funding APHL to enhance and build services within AIMS to support ETOR
• Providing funds to the Epidemiology and Laboratory Capacity for Prevention and Control of Emerging and Infectious Diseases cooperative agreement to support ETOR implementation
Partnering to Align ETOR Strategies
• Partnering with vendors of electronic health records (EHR) systems and laboratory information management systems (LIMS) vendors, healthcare systems, and standards organizations to align them with CDC’s ETOR strategy
• Partnering with healthcare providers to understand their challenges implementing ETOR with PHLs
• Working with the Office of the National Coordinator and the Centers for Medicare & Medicaid Services to explore regulatory incentives for use of standards and implementation of ETOR
The ultimate goal is integrated solutions that enable clinical EHR systems to directly communicate with PHL LIMS.
When healthcare facilities in medically underserved areas do not have ETOR systems in place, they may not be able to efficiently exchange laboratory testing data with PHLs. Our initial goal is to ensure that 30% of newly established ETOR connections benefit healthcare systems that serve patients in these communities.
Approximately four million babies are born in the United States every year, and nearly every one of them is screened at birth for dozens of potentially fatal or disabling health conditions that are treatable if detected as early as possible. These screenings identify infants that need immediate follow-up testing and lead to the diagnosis of one or more serious conditions in over 12,000 newborns each year. Many healthcare providers still submit newborn screening orders through the mail and receive their results by fax. These modes of transmission require additional manual data entry, increase the risk of human error, and can often result in missing data or samples and delayed or missed diagnoses. Strengthening ETOR will allow PHLs to plan for and track incoming specimens and immediately report test results with comprehensive data back to the provider, bolstering the peace of mind of new parents and ensuring that thousands of babies receive the prompt care they need.

Recent public health emergencies from Zika virus to SARS-COV-2 and mpox have demonstrated the urgent need for improved interoperability between PHLs and healthcare facilities. Existing manual processes for receiving test orders, accessioning and testing specimens, and reporting results back have proven insufficient for both providers and public health agencies who need patient demographic data to aid the emergency response. CDC’s ETOR solution will address these concerns by streamlining the transmission of test orders to allow PHLs to adequately anticipate incoming requests and facilitating a more immediate and comprehensive exchange of data when reporting results.
- • Data Modernization Implementation Support | DMI Support | CDC
• Expanding Laboratory Data Exchange | DMI Support | CDC
• Public Health Surveillance and Data | CDC
• INFO-2020-ETOR from the Association of Public Health Laboratories (APHL)
• INFO-2019-May-ETOR-high-level from APHL