Muscular Dystrophy Diagnostic Tools
Why Diagnostic Tools are Important
CDC supports early identification and evaluation of motor development in children. Motor development is how a child’s brain and muscles become able to move parts of the body like arms, fingers, legs, and head, and to work together so the child can get around, such as in walking, running, and climbing.
Early screening and identification can reduce the “diagnostic odyssey” that families of children with motor delays may face as they spend years visiting different doctors and undergoing many tests to reach a correct diagnosis. Early screening enables a faster referral to a specialist and early identification can mean quicker access to early intervention programs or special education resources.
CDC has collaborated with partners to design these diagnostic tools for families and healthcare professionals.
Web-based Tool for Families
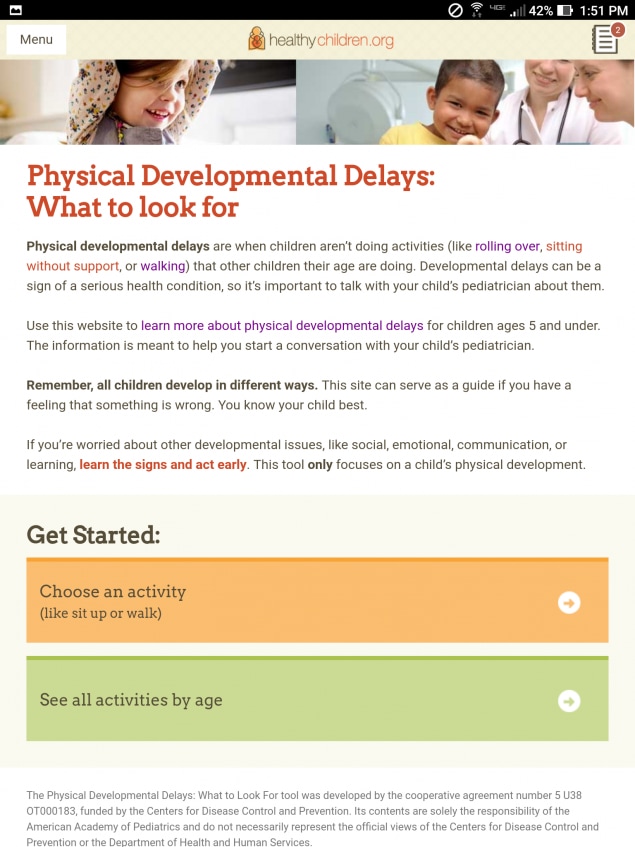
Physical Developmental Delays: What to look forParents know their child best. This online quiz is for parents who are concerned about the physical development of their child. Parents can identify “red flags” they see when their child stands, walks, climbs stairs, holds toys, and other activities. The quiz also helps parents prepare to talk to their child’s doctor.
Web-based Tool for Health Professionals
Child Muscle Weakness This web-based tool may help primary care clinicians, therapists, and other specialists diagnose child muscle weakness. This tool can decrease the time between initial signs and first diagnosis, and improve early intervention and access to care.
Links to Other Websites
Learn the Signs. Act Early. Milestones Tracker App
Bright Futures Program (American Academy of Pediatrics)