Lifesaving Naloxone

What is naloxone?
Naloxone is a life-saving medication that can reverse an overdose from opioids—including heroin, fentanyl, and prescription opioid medications—when given in time.1 Naloxone is easy to use and small to carry. There are two forms of naloxone that anyone can use without medical training or authorization: prefilled nasal spray and injectable.

Prefilled devices that spray medication into the nose.
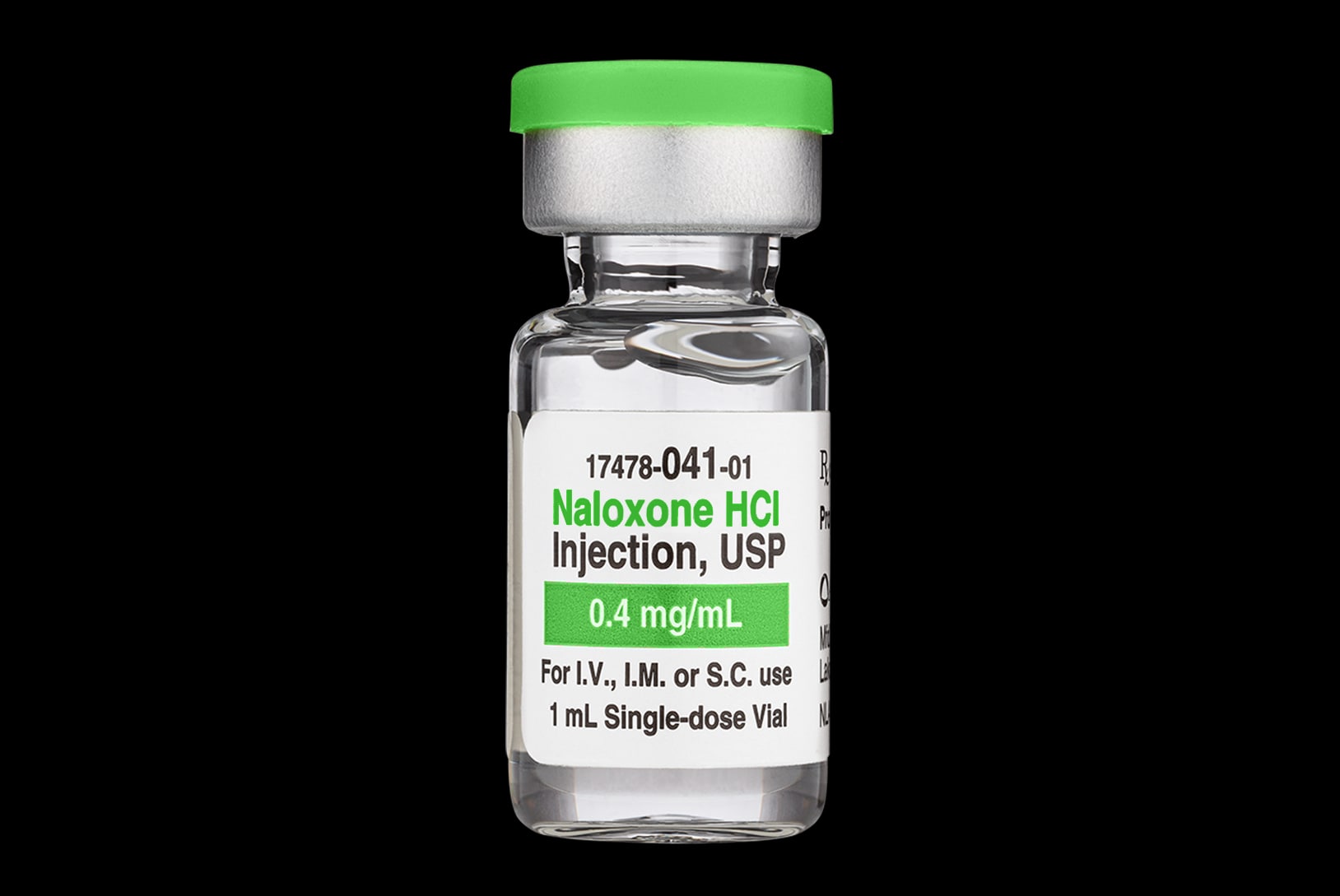
Medication (solution) given by injection into a muscle or under the skin.
The decision on which form of naloxone to use or carry can depend many factors such as cost, availability, and comfort level. Both are safe, effective, and can help save a life.
How does naloxone work and how do you use it?
Naloxone quickly reverses an overdose by blocking the effects of opioids. It can restore normal breathing within 2 to 3 minutes in a person whose breath has slowed, or even stopped, as a result of opioid overdose. More than one dose of naloxone may be required when stronger opioids like fentanyl are involved.2
Naloxone won’t harm someone2 if they’re overdosing on drugs other than opioids, so it’s always best to use it if you think someone is overdosing.
If you give someone naloxone, stay with them until emergency help arrives or for at least four hours to make sure their breathing returns to normal.2
Good Samaritan laws are in place in most states to protect those who are overdosing and anyone assisting them in an emergency from arrest, charges, or a combination of these.
Why carry naloxone?
Naloxone saves lives
Nearly 50,000 people died from an opioid-involved overdose in 2019.3 One study found that bystanders were present in more than one in three overdoses involving opioids.3 With the right tools, bystanders can act to prevent overdose deaths. Anyone can carry naloxone, give it to someone experiencing an overdose, and potentially save a life.
Who should carry naloxone?
If you or someone you know is at increased risk for opioid overdose, especially those struggling with opioid use disorder (OUD), you should carry naloxone and keep it at home. People who are taking high-dose opioid medications (greater or equal to 50 morphine milligram equivalents per day) prescribed by a doctor, people who use opioids and benzodiazepines together, and people who use illicit opioids like heroin should all carry naloxone. Because you can’t use naloxone on yourself, let others know you have it in case you experience an opioid overdose.
Carrying naloxone is no different than carrying an epinephrine auto-injector (commonly known by the brand name EpiPen) for someone with allergies. It simply provides an extra layer of protection for those at a higher risk for overdose.
In nearly 40% of overdose deaths, someone else was present.4 Having naloxone available allows bystanders to help a fatal overdose and save lives.

* Based on a CDC Vital Signs report.
Naloxone is available in your state.
Naloxone is available in all 50 states. If you have been prescribed high-dose opioids, talk to your doctor about co-prescribing naloxone. However, in most states, you can get naloxone at your local pharmacy without a prescription.1 You can also get naloxone from community-based naloxone programs and most syringe services programs.

Recognizing the signs of opioid overdose can save a life. Here are some things to look for:
- Small, constricted “pinpoint pupils”
- Falling asleep or losing consciousness
- Slow, weak, or no breathing
- Choking or gurgling sounds
- Limp body
- Cold and/or clammy skin
- Discolored skin (especially in lips and nails)
It may be hard to tell whether a person is high or experiencing an overdose. If you aren’t sure, treat it like an overdose—you could save a life.
Call 911 Immediately.*

Administer naloxone, if available.

Try to keep the person awake and breathing.

Lay the person on their side to prevent choking.

Stay with the person until emergency assistance arrives.
*Most states have laws that may protect a person who is overdosing or the person who called for help from legal trouble.
- CDC Podcast – Lifesaving Naloxone [MP3 – 17 MB]
- Reversing Opioid Overdoses with Lifesaving Naloxone [PDF – 8 MB]
- Reverse Overdose to Prevent Death
- Overdose Deaths and the Involvement of Illicit Drugs
- Life-Saving Naloxone from Pharmacies
- Increase in Fatal Drug Overdoses Across the United States Driven by Synthetic Opioids Before and During the COVID-19 Pandemic
- Life-Saving Naloxone from Pharmacies. (2019). Centers for Disease Control and Prevention. https://www.cdc.gov/vitalsigns/naloxone/index.html
- Opioid Overdose Prevention Toolkit. (2018). Substance Abuse and Mental Health Services. https://store.samhsa.gov/sites/default/files/d7/priv/sma18-4742.pdf
- National Institutes on Health: National Institute on Drug Abuse: Overdose Death Rates
https://www.drugabuse.gov/drug-topics/trends-statistics/overdose-death-rates - O’Donnell J, Gladden RM, Mattson CL, Hunter CT, Davis NL. Vital Signs: Characteristics of Drug Overdose Deaths Involving Opioids and Stimulants — 24 States and the District of Columbia, January–June 2019. MMWR Morb Mortal Wkly Rep 2020;69:1189–1197. DOI: http://dx.doi.org/10.15585/mmwr.mm6935a1

