Urban-Rural Differences in Chronic Obstructive Pulmonary Disease (COPD)
Updated April 21, 2023
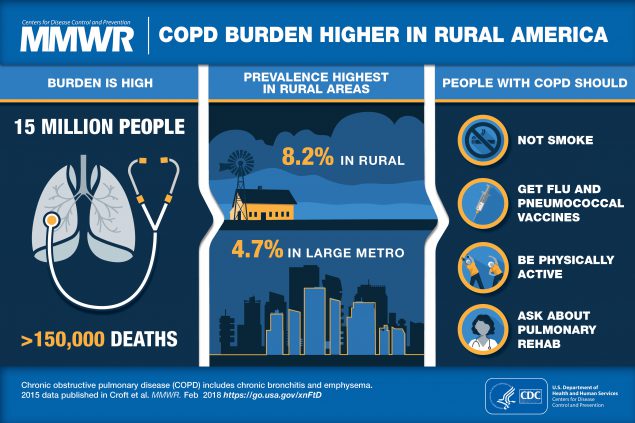
COPD is a group of respiratory conditions, including chronic bronchitis and emphysema, which makes breathing difficult for millions of Americans. COPD comprises the majority of deaths from chronic lower respiratory diseases, which was the fourth leading cause of death in the United States in 2016.1
Rural populations may have more COPD-related issues due to more people smoking,3 increased exposure to secondhand smoke, and less access to smoking cessation programs compared with people living in more urban areas.4 Rural residents are also more likely to be uninsured and have higher poverty levels, which may lead to less access to early diagnosis and treatment.5
There need to be additional efforts to prevent and reduce risk factors and overcome barriers to early diagnosis and appropriate treatment and management of COPD in rural areas.
Improving access to such health care may improve quality of life, reduce hospital readmissions among COPD patients, and reduce COPD-related deaths. There is a continued need for tobacco cessation programs and policies to prevent COPD and improve pulmonary function among adults with COPD in rural areas in particular. Additionally, there is a need for more widespread treatment, including pulmonary rehabilitation and oxygen therapy, and comprehensive chronic disease-self-management programs.
Health care providers and community partners that serve rural residents can help adults with COPD increase access to and participation in these health care interventions.
Educational resources for pulmonary rehabilitation, self-management, and patient support groups
TOOLS
Resources to help you best manage
your COPD.
SELF-MANAGEMENT PROGRAM
Educational resources from CDC
Better PROGRAM
COPD program from National Heart, Lung, and Blood Institute (NHLBI)
External Link IconPersonalized treatment program that teaches you how to manage your COPD symptoms to improve your quality of life.
External Link IconThe state and insurance costs, earnings lost,
and projections
- Heron M. Deaths: Leading causes for 2016. National Vital Statistics Reports; vol 67 no 6 [PDF – 87 KB]. Hyattsville, MD: National Center for Health Statistics. 2018.
- Croft JB, Wheaton AG, Liu Y, et al. Urban-Rural County and State Differences in Chronic Obstructive Pulmonary Disease — United States, 2015. MMWR Morb Mortal Wkly Rep 2018;67:205–211.
- Matthews KA, Croft JB, Liu Y, et al. Health-related behaviors by urban-rural county classification—United States, 2013. MMWR Surveill Summ 2017;66(No. SS-5).
- American Lung Association. Cutting tobacco’s rural roots: Tobacco use in rural communities. ALA, Washington, DC; 2012.
- University of Wisconsin Population Health Institute. County Health Rankings Key Findings 2016.