ILO Classification for B Readers
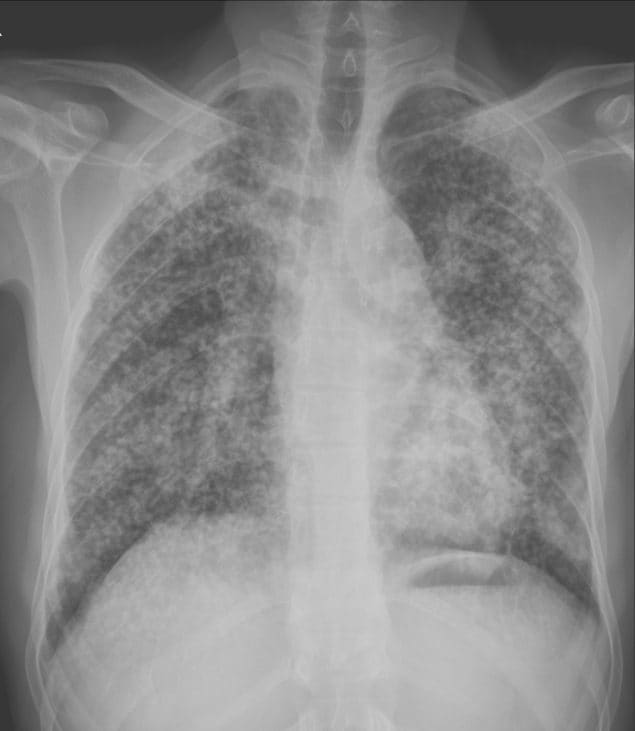
Photo by NIOSH
The International Labour Organization (ILO) is a tripartite U.N. agency that brings together governments, employers, and workers to set labor standards, develop policies and devise programs that promote honest work for women and men. The ILO International Classification of Radiographs of Pneumoconioses is a global tool used to:
- Improve surveillance of worker health
- Conduct epidemiological research
- Make comparisons of statistical data
Classification Scheme
The Classification System includes the Guidelines and two sets of standard images. The standard images represent different types and severity of lung abnormalities and are used to compare a person’s images during the classification process. The system is oriented towards describing the nature and extent of features associated with the different pneumoconioses, such as:
- Coal workers’ pneumoconiosis
- Silicosis
- Asbestosis
It deals with:
- Parenchymal abnormalities (small and large opacities).
- Pleural changes.
Other findings
In the ILO system, the reader is asked to:
- Grade radiograph quality.
- Categorize small opacities according to shape and size profusion.
- The size of small round opacities is characterized as:
- p (up to 1.5 mm)
- q (1.5-3 mm)
- r (3-10 mm)
- Irregular small opacities are classified by their short axis width as s, t, or u (same sizes as for small, rounded opacities).
- Profusion (frequency) of small opacities is classified on a 4-point major category scale (0 – 3), with each major category divided into three, giving a 12-point scale between 0/- and 3/+.
- Large opacities are defined as any opacity greater than 1 cm that is present in the image. These are classified as:
- Category A (for one or more large opacities whose combined dimension does not exceed 5 cm
- Category B (for one or more large opacities whose combined dimension exceeds 5 cm but does not exceed the equivalent area of the right upper lung zone)
- Category C (size is greater than the equivalent area of the right upper lung zone)
- Pleural abnormalities are also classified with respect to location, width, extent, and degree of calcification.
- Other abnormal features of chest radiographs can be commented upon (ILO 2022).
- The size of small round opacities is characterized as:
See the Guidelines for the Use of the ILO International Classification of Radiographs of Pneumoconioses for a full description and exact definition of terms and entities.
The Chest Radiograph Classification Form is used by the NIOSH Coal Workers’ Health Surveillance Program to record characteristics of the radiograph and abnormalities.
Classification Considerations
Accuracy and precision are important considerations when radiographic classifications made .
- Accuracy is defined as the ability for a measurement to reflect the true degree of underlying abnormality.
- Precision reflects the extent a measurement is consistent across repeated determinations.
- A measurement technique can be precise but inaccurate or can be accurate and imprecise. It is preferable for a measurement to be both accurate and precise to optimize validity.
References
Fletcher CM, Oldham PD. The problem of consistent radiological diagnosis in coalminers’ pneumoconiosis. An experimental study. Br J Ind Med 1949; 6:168-183.
Bohlig H, Bristol LJ, Cartier PH, et al. UICC/Cincinnati classification of the radiographic appearances of pneumoconiosis. Chest 1970; 58:57-67.
Jacobsen M. Part 5. Radiologic Abnormalities: Epidemiologic Utilization: The International Labour Office Classification: Use and Misuse. Ann NY Acad Sci 1991; 643:100-107.
Friedman LS, De S, Almberg KS, Cohen RA. Association Between Financial Conflicts of Interest and ILO Classifications for Black Lung Disease. Ann Am Thorac Soc 2021; doi:10.1513/AnnalsATS.202010-1350OC.
Fay JWJ, Rae S. The Pneumoconiosis Field Research of the National Coal Board. Ann Occup Hyg 1959; 1:149-61.
Hurley JF, Burns J, Copland L, et al. Coalworkers’ simple pneumoconiosis and exposure to dust at 10 British coalmines. Br J Ind Med 1982; 39:120-7.
Reger RB, Amandus HE, Morgan WKC. On the diagnosis of coalworkers’ pneumoconiosis – Anglo-American disharmony. Am Rev Respir Dis 1973; 108:1186-91
Weill H, Jones R. The chest roentgenogram as an epidemiologic tool. Report of a workshop. Arch Environ Health 1975; 30:435-9.
Sheers G, Rossiter CE, Gilson JC, et al. UK naval dockyards asbestos study: radiological methods in the surveillance of workers exposed to asbestos. Br J Ind Med 1978; 35:195-203.
