World NTD Day 2023: Following the diagnostic development pathway to better health

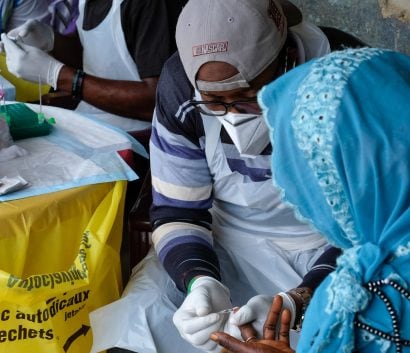
Scott Elder (center) training laboratory team members from the National Public Health Reference Laboratory – Ghana on a technique for detecting antibodies against Onchocerca volvulus. Credit: Andrew Abbott/CDC
On World NTD Day 2023, we highlight a group of diseases including trachoma, onchocerciasis, lymphatic filariasis (LF), schistosomiasis, and Guinea worm disease that collectively threaten more than a billion people across the world and undercut global health equity because of the way they affect the world’s poorest people. These neglected tropical diseases (NTDs) cause disability, derail school attendance, hinder care of families and neighbors, and make earning a living challenging. Across the globe, they deprive people of the opportunity to attain their highest level of health.
CDC works alongside global health partners including the World Health Organization (WHO), the U.S. Agency for International Development (USAID), the Bill and Melinda Gates Foundation, and the CDC Foundation to prevent and manage NTD infections in partner countries and in American territories. Together, we strive to restore the opportunity of living healthy lives. We carry out surveillance, mass drug administration campaigns, clinical management of cases, and development of new diagnostics.
In 2021, WHO published its plan for addressing NTDs around the world: Ending the neglect to attain Sustainable Development Goals: A road map for neglected tropical diseases 2021–2030. This plan sets ambitious milestones on the road towards eliminating or eradicating certain NTDs. CDC experts provided technical input towards the development of this plan and align their work with these targets.
Diagnostic tests to support surveillance are foundational to NTD control and elimination programs. Many traditional methods have relied on detection of parasite life cycle stages. As elimination efforts ramp up and infection rates decline, these traditional methods lack the sensitivity to confirm interruption of transmission. Thus, tests with greater precision are essential. Having tools that can accurately assess the level of NTD transmission in a community is the only way NTD control programs can know whether they have successfully achieved established targets.
Limitations of existing diagnostic tools undermine confidence that program milestones are being achieved and threaten measurement of progress toward the 2030 goals. Take onchocerciasis, for example. WHO guidelines dictate that countries cannot say that transmission has ceased unless they can demonstrate that fewer than 1 in 1,000 children have been exposed to the parasite that causes onchocerciasis. This is extremely difficult to measure, and current tests are unable to meet these standards. The key is having a test that can consistently detect infected people without misdiagnosing uninfected people.
“We need to be able to say we’ve achieved our goal,” says Dr. Evan Secor who leads the Parasitic Diseases Elimination and Control Lab Team within CDC’s Division of Parasitic Diseases and Malaria (DPDM). “New diagnostics are the only way to know when we’ve reached interruption of transmission.”
In addition to inadequate accuracy, the current generation of diagnostics can also be slow and enormously inconvenient to use. For example, one of the tests for onchocerciasis looks for parasites in someone’s skin, requiring a painful, hard-to-get skin sample. For LF, there is a diagnostic that requires a blood sample being taken in the middle of the night. And for schistosomiasis, diagnosis depends on detection of parasite eggs in stool or urine samples (which can be difficult to obtain). “Simply put, we need tests that are easier, more reliable, and as minimally invasive as possible,” says Secor.
Of course, developing new tests is no easy feat. “Diagnostic development is a pathway,” describes DPDM health scientist Dr. Kimberly Won. “First, there’s research to identify appropriate biomarkers [measurable substances that indicate the presence of infection]. Then, after new tests are developed, we validate them in a laboratory setting to determine how well they work before sending them out to the field for further trials in a real-world setting. After that, there’s WHO and regulatory review before the tests are ultimately ready for use… It’s an iterative process.”
CDC has cultivated unique expertise, honed over decades, to identify efficiencies and streamline the diagnostic development pathway. CDC experts also serve on WHO’s Diagnostic Technical Advisory Groups, which guide the creation and validation of new tests.
The diagnostic development pathway
- Biomarker discovery
- Assay development
- Laboratory validation
- Field validation
- WHO and regulatory review
- Epidemiologic and/or clinical use
Partners in Sierra Leone work in the field to evaluate LF diagnostics. Credit: Kimberly Won/CDC
Once new tests pass the hurdle of initial development and rigorous lab testing, they are sent out for field evaluations. “We have to make sure the test is actually effective in the exact context for which it is intended: in the field, in communities, directly from a finger stick,” explains Won. “Some of the tests we develop look great in the lab, but then fail in real field settings.”
DPDM biologist Scott Elder traveled with Dr. Won to Sierra Leone in 2022 to evaluate a new test for LF. “When we go out into the field, we ask ourselves ‘In real world settings, will this test perform the way we expect it to every single time? Can we really replicate the same outcomes we’ve seen in our lab in Atlanta?’”
Elder and Won worked with local teams for more than two weeks to see whether the new LF test could provide consistent, rapid, and actionable results. They were trying to determine if the new test can help with decisions about when preventive treatment for LF can stop. They then observed a team using these tools in villages which had previously found it challenging to meet certain milestones.
Data analysis from the Sierra Leone evaluation remains ongoing, though Elder and Won are hopeful about what new LF tools could potentially mean for LF control and elimination.
LF, also called elephantiasis, affects more than 120 million across 72 countries. Some people with LF develop lymphedema (fluid collection and swelling which most often affects the legs) or, in men, a swelling of the scrotum called hydrocele. It often leads to lifelong pain, disability, and stigma. “Being in the field allows you to see how meaningful this work really is to people,” adds Elder. “Sometimes, just looking at numbers and tests in the lab all day, you can lose sight of the devastating effect these diseases have on people.”
Once field evaluations sufficiently demonstrate the efficacy of a new test, CDC works to ensure that countries’ and territories’ NTD control programs are equipped to roll it out.
“We help countries take ownership of their testing. We don’t want the testing all being sent to CDC,” explains DPDM microbiologist Dr. Jessica Prince–Guerra. “Lab quality is a major focus of ours. We take what we’ve learned over the years and share knowledge with others. We strive to make sure that countries have a sustainable way forward, and that they are able to generate consistent laboratory data to support decision making.” Prince-Guerra and Elder went to Ghana in 2022 to help the national public health reference laboratory with rapid diagnostic testing and ELISA techniques for onchocerciasis. Following the training, the Ghanaian lab staff demonstrated proficiency in use of the new tests, paving the way for greater sustainability within their own, national lab.
Elimination of NTDs remains an achievable and undeniably worthwhile goal. Globally, 43 countries have already eliminated at least one NTD. In May 2022, WHO validated Togo as having eliminated trachoma as a public health problem. At the time, USAID’s Assistant Administrator for Global Health Dr. Atul Gawande wrote Togo is “crushing it, eliminating three neglected tropical diseases in 5 years.”1 We are also on the cusp of Guinea worm disease eradication. Just 13 human cases of Guinea worm disease were reported in 2022, down from approximately 3.5 million human cases in 1986.
Through a partnership between industry, technical agencies, academic institutions, donors, and national NTD programs, the global health community remains steadfast in its push against the torment of NTDs.
“There really is potential to reduce the global NTD burden and eliminate certain diseases,” says Won. “Being able to protect future generations is what drives us.”
Read more about how DPDM works to eliminate NTDs in its Strategic Priorities 2021—2025.
1 Atul Gawande on Twitter: “NEWS: @WHO certified that #Togo has become the 15th nation to eliminate blinding trachoma as a public health problem. @MSPS_Togo is crushing it, eliminating 3 neglected tropical diseases in 5 years. US is proud to have supported this incredible effort. https://t.co/6Pmhf0s8AI https://t.co/sTp7u6uu5H” / Twitter
- World Neglected Tropical Disease (NTD) Day 2023: A letter from CDC Director
- CDC: Neglected Tropical Diseases
- USAID: Neglected Tropical Diseases
- WHO: Neglected Tropical Diseases