Clinical and Laboratory Diagnosis
Rickettsial Disease Diagnostic Testing and Interpretation for Healthcare Providers
This video provides information on rickettsial disease diagnostic methods for healthcare providers, including what tests are available and when it is most appropriate to collect samples. This video focuses on the use of polymerase chain reaction (or PCR) tests, and the indirect immunofluorescence antibody (IFA) assay for rickettsial disease diagnosis.
Clinical Diagnosis
- Early recognition and treatment is key.
- Ehrlichiosis can be difficult to diagnose, particularly in the early stages of illness; early recognition and treatment based on clinical suspicion are important to prevent severe illness.
- Maintain a high level of clinical suspicion for ehrlichiosis or other tickborne diseases in cases of non-specific febrile illness of unknown origin, particularly during spring and summer months when ticks are most active.
- Always take a thorough patient history, including:
- History of a recent tick bite. NOTE: Tick bites are often painless. Many people do not remember being bitten. Do not rule out a tickborne infection if your patient does not remember a tick bite.
- Exposure to areas where ticks are commonly found, including wooded areas or brushy areas with high grasses and leaf litter.
- Travel history (domestic and international) to areas where ehrlichiosis is endemic.
- Advanced ehrlichiosis may also be confused clinically with non-tickborne illnesses such as meningoencephalitis, sepsis, toxic shock syndrome, gastroenteritis, hepatitis, and blood malignancies.
- Laboratory confirmation is helpful for disease surveillance and understanding burden of ehrlichiosis infection in the United States.
The diagnosis of ehrlichiosis is often made based on clinical signs and symptoms, and can later be confirmed using specialized laboratory tests. Treatment should not be delayed pending the receipt of laboratory test results or withheld based on an initial negative laboratory result.
Laboratory Diagnosis
- Diagnostic tests should be performed on those with illness clinically compatible with ehrlichiosis.
- The optimal diagnostic test may depend on the timing relative to symptom onset and the type of specimen(s) available for testing.
- Testing for ehrlichiosis should be considered for any person with a compatible illness and known risk factors, such as history of a tick bite.
- Ehrlichiosis is a nationally notifiable condition. Correct testing and reporting of ehrlichiosis are important to improve our understanding of how common this disease is, where it occurs, and how disease trends change over time.
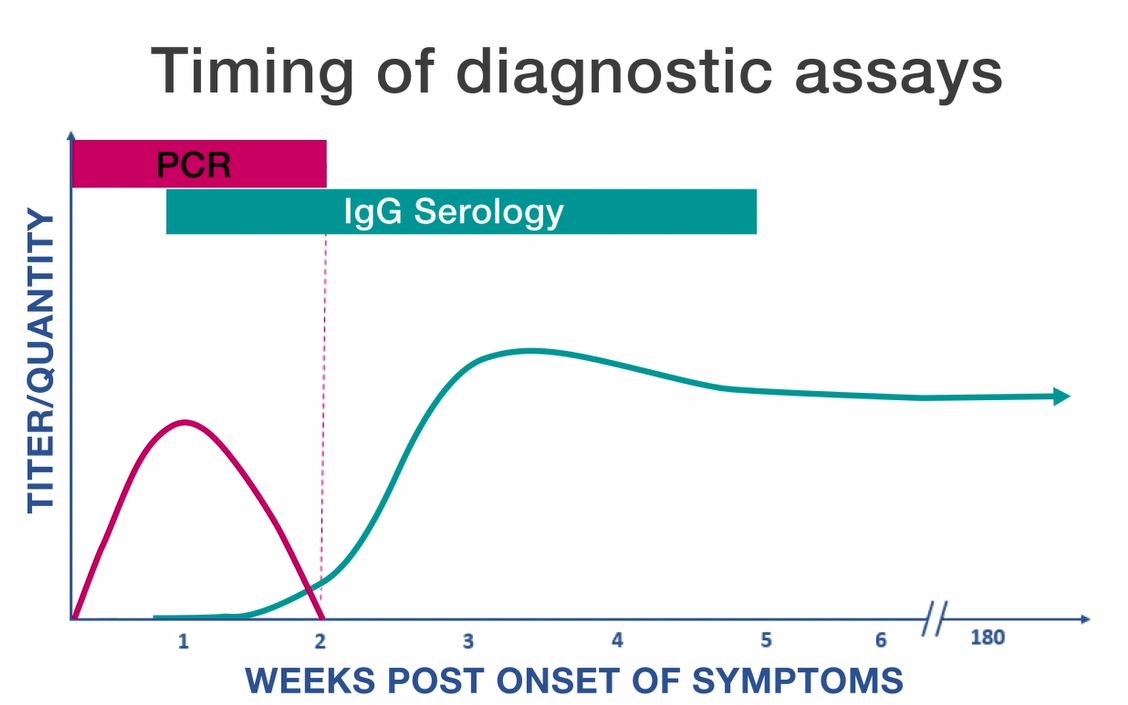
PCR
- Polymerase chain reaction (PCR) amplification is performed on whole blood specimens.
- This method is most sensitive in the first week of illness and decreases in sensitivity following the administration of appropriate antibiotics (within 48 hours).
- Although a positive PCR result is helpful, a negative result does not rule out the diagnosis, and treatment should not be withheld due to a negative result.
- PCR might also be used to amplify DNA in solid tissue and bone marrow specimens.
Serology
- The reference standard serologic test for diagnosis of ehrlichiosis is the indirect immunofluorescence antibody (IFA) assay for immunoglobulin G (IgG).
- IgG IFA assays should be performed on paired acute and convalescent serum samples collected 2–4 weeks apart to demonstrate evidence of a fourfold seroconversion.
- Antibody titers are frequently negative in the first week of illness. Ehrlichiosis cannot be confirmed using single acute antibody results.
- Immunoglobulin M (IgM) IFA assays may also be offered by reference laboratories, however, are not necessarily indicators of acute infection and might be less specific than IgG antibodies.
- Antibodies, particularly IgM antibodies, might remain elevated in patients for whom no other supportive evidence of a recent rickettsiosis infection exists. For these reasons, IgM antibody titers alone should not be used for laboratory diagnosis.
Persistent Antibodies
- Antibodies against Ehrlichia species might remain elevated for many months after disease has resolved.
- Comparison of paired, and appropriately timed, serologic assays provides the best evidence of recent infection.
- Single or inappropriately timed serologic tests, in relation to clinical illness, can lead to misinterpretation of results.
Cross Reactivity
- Closely related organisms, including those in the Ehrlichia and Anaplasma genera, share similar antigens such that antibodies directed to one of these antigens can cross-react.
- Most commercial labs are unable to differentiate between Ehrlichia species.
- In areas endemic for Ehrlichiosis and Anaplasmosis, IFA using antigen from both Ehrlichia and Anaplasma species should be run side-by-side.
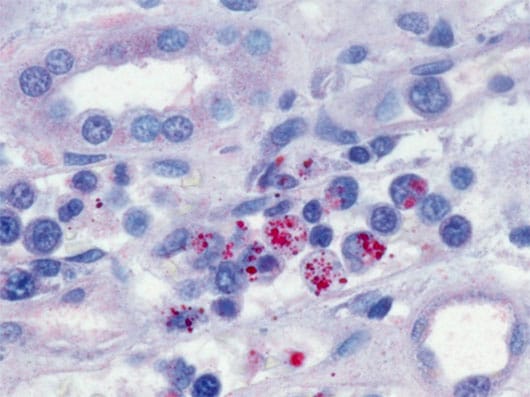
Immunohistochemical stain demonstrating Ehrlichia chaffeensis morulae (red) within monocytes in the kidney of a patient with ehrlichiosis
IHC and Culture
- Culture isolation and immunohistochemical (IHC) assays of Ehrlichia species are only available at specialized laboratories; routine hospital blood cultures cannot detect the organism.
- PCR, culture, and IHC assays can also be applied to post-mortem specimens.
- If a bone marrow biopsy is performed as part of the investigation of cytopenias, immunostaining of the bone marrow biopsy specimen can diagnose ehrlichiosis.
Blood-smear Microscopy
- During the first week of illness, a microscopic examination of a peripheral blood smear might reveal morulae (microcolonies of Ehrlichiae) in the cytoplasm of white blood cells and is highly suggestive of a diagnosis.
- E. chaffeensis most commonly infects monocytes.
- E. ewingii more commonly infects granulocytes.
- No target cell has been identified for E. muris eauclairensis.
- Blood smear examination is relatively insensitive and should not be relied upon solely to diagnose ehrlichiosis.
- The observance of morulae in a particular cell type cannot conclusively differentiate among Ehrlichia species or between Ehrlichia and Anaplasma
For more in-depth information about diagnosing ehrlichioses, see: Diagnosis and Management of Tickborne Rickettsial Diseases: Rocky Mountain Spotted Fever and Other Spotted Fever Group Rickettsioses, Ehrlichioses, and Anaplasmosis — United States: A Practical Guide for Health Care and Public Health Professionals (2016) pdf icon[PDF – 48 pages]