Organizational Characteristics of Local Health Departments and Environmental Health Services and Activities
Download the printable version of this article pdf icon[PDF – 596 KB]
Shailendra N. Banerjee, PhD
Division of Emergency and Environmental Health Services, National Center for Environmental Health, Centers for Disease Control and Prevention
Justin A. Gerding, MPH, REHS
John Sarisky, MPH, REHS
Environmental Health Services Branch, Division of Emergency and Environmental Health Services, National Center for Environmental Health, Centers for Disease Control and Prevention
Published in the Journal of Environmental Health. 2018;80(8):20–9.
Abstract
The main objective of this research was to ascertain the association between organizational characteristics of local health departments (LHDs) and environmental health services rendered in the community. Data used for the analysis were collected from LHDs by the National Association of County and City Health Officials for its 2013 national profile study of LHDs. We analyzed the data during 2016. Apart from understanding basic characteristics of LHDs in the nation, we introduced new measures of these characteristics, including “environmental health full-time equivalents” (EH FTE) per 100,000 population and “other revenue” (revenues from fees and fines) per capita.
The association of these and other organizational characteristics with EH services were measured using likelihood ratio χ2 and t-tests. Out of 34 EH services considered, LHDs directly provided an average of 12 different services. As many as 41% of the 34 EH services were not available in more than 10% of the communities served by LHDs. About 70% of communities received some services from organizations other than LHDs. All the available organizational characteristics of LHDs had association with some of the EH services. Although we might assume an increase in per capita expenditure could result in an increase in LHDs’ direct involvement in providing EH services, we found it to be true only for five (15%) of the EH services. The variation of EH services provided in communities could be explained by a combination of factors such as fee generation, community needs, type of governance, and population size.
Introduction
In 2012, the Institute of Medicine recommended a minimum package of public health services related to communicable and noncommunicable disease control, emergency preparedness and disaster response, and environmental health protections, among others (Leider, et al., 2015). This minimum package is termed the “foundational public health services” framework. Environmental public health, as a part of the framework, includes the provision of critical services in cities, counties, and states to protect and promote a safe and healthy environment for the public. This is accomplished through an array of environment health (EH) services aimed at preventing exposure to adverse environmental conditions in food, water, air, and other media.
Adverse environmental conditions are potential causes of illness, infections, and death in communities. An example of these adverse conditions was seen in exposures to lake water contamination in Tarrant County, Texas, in 2008 (Cantey et al., 2012). Cryptosporidium in the lake water led to an outbreak of gastrointestinal illness among persons who swallowed contaminated water while playing in the lake. Another example from Texas is food source contamination that caused a Salmonella outbreak among patrons of restaurants in 2008 (Mody et al., 2011). The patrons had eaten contaminated jalapeño peppers, which resulted in Salmonella enterica serotype Saintpaul infections.
The system and delivery of EH services vary across the nation. In Maryland, for example, EH services were conducted by the Maryland Department of Health and Mental Hygiene and the Maryland Department of the Environment at the state level (Resnick, Zablotsky, Nachman, & Burke, 2008). Most EH services were provided at the local level by county-based or city-based EH divisions housed within local health departments. In contrast, depending on the county, EH services in Iowa were administered by different offices, not all of which were part of the local public health department (Ramaswamy et al., 2012).
Studies of EH service delivery systems have noted variation in services and activities provided at local (e.g., county and city) and state levels. These studies indicated that EH services might correspond to local need and revenue generated by fees for service (Dyjack, Case, Marlow, Soret, & Montgomery, 2007; Resnick et al., 2008). EH services may also be intertwined with the delivery of other public health services, which vary across the nation and are affected by factors such as size of the jurisdiction and area served, governance structure, finances, and workforce structure (Mays et al., 2009).
Organizational capacity, such as fiscal resources and workforce, has been identified as an important construct in public health services and systems research, with emphasis placed on understanding its relationship with public health performance and outcomes (Meyer, Davis, & Mays, 2012; Scutchfield, Marks, Perez, & Mays, 2007). In this study, we sought to expand on this research by identifying aspects of local health departments’ (LHDs) organizational capacity associated with EH services. The primary objective was to test the association between organizational characteristics and EH services to identify those characteristics that might be most associated with the provision of specific EH services.
Methods
Data for this study were collected by the National Association of County and City Health Officials (NACCHO) from LHDs in 2013 (NACCHO, 2013). We used these data to study local level public health infrastructure and EH practice; we analyzed the data during 2016. Among approximately 2,800 LHDs in the U.S., 2,532 were included in the study population. All LHDs in the study population were asked to complete questionnaires seeking information about organizational capacity such as funding, workforce, jurisdiction, governance, and activities or services provided. These were core questions. Weights were developed by NACCHO based on answers for the items from the core questionnaire to obtain national estimates. We used these weights for our analysis. NACCHO’s profile report provides more details regarding the survey methodology (NACCHO, 2014). Overall, 2,000 LHDs completed the 2013 profile study survey, for a response rate of 79%.
We used available data to construct the following new variables representing organizational characteristics: per capita expenditure, per capita total income, per capita other revenue (revenues from fees and fines), and per capita environmental health full-time equivalents (EH FTE). These variables were derived for per unit population of LHDs for expenditure and income and per 100,000 population for EH FTE. Other variables representing organizational characteristics included population size served, governance type, jurisdiction, and region. Each of these organizational characteristics was used with a sufficient number of observations in appropriately constructed categories subdivided into two groups for services to test association (Table 1). These categories included services provided by the LHD directly or contracted out and services provided by others; we show only the proportion in the first category in the table.
The profile data included a list of 13 select EH services provided by LHDs, plus 21 regulation, inspection, or licensing services, such as those covering food service establishments and public swimming pools, which are commonly provided as EH services. This gave us a total of 34 EH services for this study.
Variables for each of these services were combined to discern if a particular service was provided by the LHD directly, by others in the community independent of LHD funding, or contracted out by the LHD (Table 2). Some services were not available in all communities, or a provider was not specified (“not known”).
To establish associations with organizational characteristics, we chose to consider services most commonly provided by LHDs (i.e., 19 EH services provided by ≥30% of LHDs) (Table 1). Table 1 shows the percentages of LHDs providing these services directly or through contract for the categories of the organizational characteristics. Values are shown only for services with significant association (p ≤ .05). The other category of “provided by others” is not shown in the table.
Data were analyzed using statistical software (SAS version 9.3). We estimated the mean number of EH services directly provided by LHDs for some of the organizational characteristics. The significant differences of these means within each of the characteristics were tested using PROC ANOVA (Table 3). Individual means were compared using t-tests. We assessed the association of each organizational characteristics of an LHD with activities and services provided in the community by using likelihood ratio χ2 tests.
Results
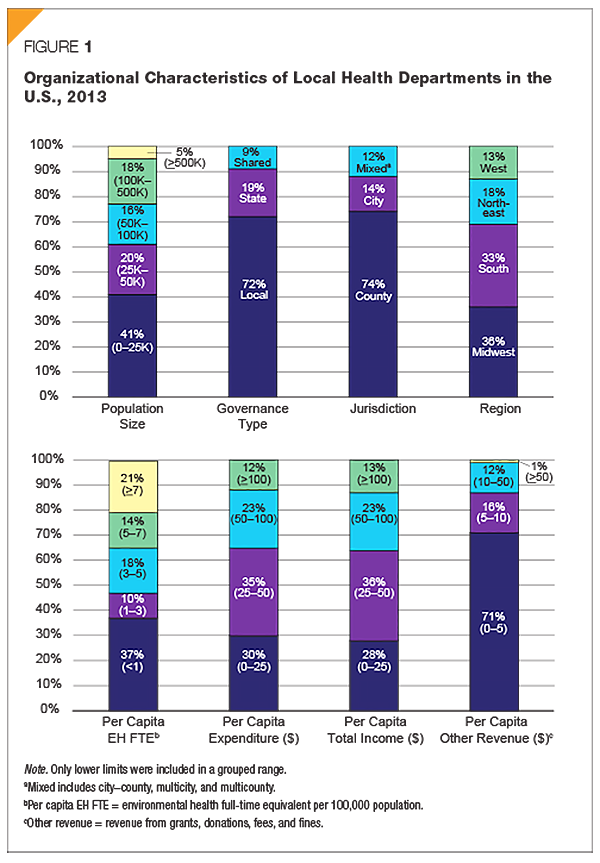
Figure 1 shows eight important LHD organizational characteristics: population size, governance type, jurisdiction, region, per capita EH FTE, per capita expenditure, per capita total income, and per capita revenues from fees and fines (other revenues). Among these, “other revenues” was not specifically described in the NACCHO profile report.
Most of the LHDs were under local governance (72%) and run by county government (74%). The largest portion (41%) of LHDs served populations <25,000, and 77% catered to populations <100,000. We found that 37% of LHDs had <1 EH FTE per 100,000 population, and 65% had <5 EH FTEs per 100,000 population.
Moreover, total revenues and expenditures of LHDs were closely aligned. Nearly one quarter (30% and 28%, respectively) had per capita expenditure and total income <$25, and only about one tenth (12% and 13% respectively) had per capita expenditure and total income ≥$100. Median revenue and expenditure of LHDs were similar (about $1.5 million). “Other revenues” was comprised of grants, donations, fees, and fines potentially generated by EH services such as food service inspections and permits. Only 13% of LHDs, however, earned ≥$1 million from these other sources, and 44% earned <$50,000, with a median of $84,000.
The study included a total of 34 EH services that LHDs provided (Table 2). Nine (26%) of these services, however, were provided by <20% of LHDs. Organizations other than LHDs provided a large proportion of communities with services such as hazardous materials response (73%), hazardous materials disposal (70%), collection of unused pharmaceuticals (66%), and land use planning (68%) . As many as 14 (41%) of the 34 EH services were not available in >10% of the communities served by LHDs. These included services related to indoor air quality (18%), radiation control (19%), noise pollution (16%), mobile homes (20%), and milk processing (17%), among others. Although the majority of EH services were most frequently provided by LHDs directly or by other organizations serving the community, some were contracted out by LHDs. They varied from <1% (noise pollution and land use planning) to 6% (lead inspection). On average, LHDs directly provided 12 different EH services.
Table 3 shows the mean number of EH services LHDs performed, by population size, per capita other revenue, and per capita expenditure. The mean number of EH services provided by LHDs significantly increased with gains in population size and per capita other revenue, although it decreased for the highest group (>$50) of per capita other revenue, this dip could be an artifact of the small number of observations in this group. Per capita expenditure, however, did not follow this increasing pattern of mean number of EH services performed by LHDs. The mean was the same (13) in the lowest and highest group, indicating that the number of EH services performed by LHDs might not necessarily depend on expenditure only.
In general, as the per capita LHD expenditure increased, the proportion of LHDs directly providing services in the community also increased (Table 1). We found, however, that this increasing association was statistically significant (p ≤ .05) for only 5 of the 19 services: food safety education, body art (tattoo), lead inspection, food service establishments, and health-related facilities. For food processing, the proportion of LHDs providing service decreased as per capita expenditure increased. No association was observed between per capita expenditure and any of the other services.
A similar increasing association was observed with per capita total income and eight services: indoor air quality, septic systems, children’s camps, body art (tattoo), lead inspection, public drinking water, private drinking water, and health-related facilities. This significant association was observed also for per capita other revenues with all the services except for vector control, hotel/motel, lead inspection, and food processing.
We found a significant positive association between EH FTEs per 100,000 population and LHDs directly providing each of the 19 services (Table 1). Regional differences in LHD participation for providing services was also significant for all the services, with Northeast and South regions, in general, having the two highest percentages of participation by LHDs directly . The same type of relationship was observed with the governance and jurisdiction characteristics for most of the services, with local government and city jurisdiction having the highest percentages of participation by LHD directly for more than half of these services. The percentage of LHDs directly providing services significantly increased with population size for 12 of the 19 services.
Discussion
The NACCHO profile study identified 87 public health services provided by LHDs, of which 34 were EH related (NACCHO, 2014). On average, LHDs directly provided a total of 12 services, and as many as 14 of the 34 EH-related services were not available in >10% of the communities. Among the LHDs, 37% had <1 EH FTE per 100,000 population, and 65% had <5 EH FTE per 100,000 population. Many of the EH services were more commonly provided by agencies other than the LHDs (as much as ≥70%). This finding highlights the complex and varied EH service delivery system, which includes multiple EH partners and stakeholders.
All eight LHD organizational characteristics showed association with at least some of the 19 EH services reviewed. Of all the characteristics, per capita expenditures and total income were associated with the fewest number of services. Per capita other revenue, however, showed statistically significant relationships with most of the EH services (Table 1). Other revenues included funds potentially generated by licensing and permitting fees. Thus, the relationship of other revenues and EH services could affect the provision of EH services.
Food safety education was provided directly by 77.1% of LHDs with per capita expenditures of <$25. That percentage increased to 87.6% for LHDs with per capita expenditure ≥$100, showing a significantly increasing association with per capita expenditure (p < .01) (Table 1). This associated increase would seem to reflect a natural assumption that with increases in per capita expenditure, the direct involvement of LHDs in providing health services will increase. We did not find this to be true, however, for all of the EH services, except for body art (tattoo), lead inspection, food processing, food service establishments, and health-related facilities. We did find the association to be more pervasive for per capita total income, population size, per capita other revenues, and per capita EH FTE. LHDs were certainly more likely to provide services with increases in income, expenditure, population, or EH FTE, but this pattern probably was also influenced by the importance or need for the service in the community.
Governance and jurisdiction showed association with most of the services. A higher percentage of LHDs at the city level were providing each of these services. The number of EH FTE per 100,000 population, and regional locations of LHDs showed the highest number of significant relationships, identified among all 19 EH services selected. One might expect that higher percentages of LHDs would be providing services as the number of EH FTE per 100,000 population increases. But, the relationship between regional locations and LHD provision of EH services might be an indication of services being based on needs of a particular geographic area.
The results of this study showed that the providers of EH services in communities can vary widely. Although LHDs are the common providers of the services, other organizations or agencies also contribute to service delivery. This supports claims about varied EH structure and consequent delivery systems. Organizational characteristics and their relationships with LHD EH services further demonstrate that variables such as finance, population, geographic location, and workforce are related to LHD provision of EH services. EH services provided in U.S. communities vary considerably, which might be the result of factors such as fee generation, specific community needs, type of governance, or simply population size.
Programs and activities specific to a health department or a community’s needs were also one of the considerations of a Public Health Leadership Forum convened in 2013. The findings from our study might present implications for the description of environmental public health activities developed by this forum (Public Health Leadership Forum, 2014).
Further research into the structure and delivery of EH services could help build a better understanding of how and why certain services are provided in a community and others are not. This knowledge might be used to help ensure that communities receive necessary EH services.
Finally, our study contributes to public health services research by testing the association between organizational characteristics of LHDs and EH services rendered. Shah and coauthors (2014) showed differences in performed services for some of the characteristics. We showed this relationship to be true, however, for the available and derived organizational characteristics based on standard statistical procedure.
This study is subject to several limitations. The study imparts general information about whether or not an LHD provides a specific service, without going into much detail about its scope and level. The study is based also on self-reported information, without any verification for reliability, giving the possibility of biased results.
Acknowledgements: Data to support this research were provided by NACCHO through funding from the Robert Wood Johnson Foundation and the Centers for Disease Control and Prevention.
Corresponding Author: Shailendra N. Banerjee, Division of Emergency and Environmental Health Services, National Center for Environmental Health, Centers for Disease Control and Prevention, Atlanta, GA 30341. E-mail: snb1@cdc.gov.
References
Cantey, P.T., Kurian, A.K., Jefferson. D., Moerbe, M.M., Marshall, K., Blankenship, W.R., . . . Hlavsa, M.C. (2012). Outbreak of cryptosporidiosis associated with a man-made chlorinated lake—Tarrant County, Texas, 2008. Journal of Environmental Health, 75(4), 14–19.
Dyjack, D.T., Case, P., Marlow, H.J., Soret, S., & Montgomery, S. (2007). California’s county and city environmental health services delivery system. Journal of Environmental Health, 69(8), 35–43.
Leider, J.P., Juliano, C., Castrucci, B.C., Beitsch, L.M., Dilley, A., Nelson, R., . . . Sprague, J.B. (2015). Practitioner perspectives on foundational capabilities. Journal of Public Health Management and Practice, 21(4), 325–335.
Mays, G.P., Smith, S.A., Ingram, R.C., Racster, L.J., Lamberth, C.D., & Lovely, E.S. (2009). Public health delivery systems: Evidence, uncertainty, and emerging research needs. American Journal of Preventive Medicine, 36(3), 256–265.
Meyer, A.M., Davis, M., & Mays, G.P. (2012). Defining organizational capacity for public health services and systems research. Journal of Public Health Management and Practice, 18(6), 535–544.
Mody, R.K., Greene, S.A., Gaul, L., Sever, A., Pichette, S., Zambrana, I., . . . Swerdlow, D.L. (2011). National outbreak of Salmonella serotype Saintpaul infections: Importance of Texas restaurant investigations in implicating jalapeño peppers. PLOS ONE, 6(2), e16579.
National Association of County and City Health Officials. (2014). 2013 national profile of local health departments. Retrieved from http://archived.naccho.org/topics/infrastructure/profile/upload/2013-National-Profile-of-Local-Health-Departments-report.pdf.pdf iconexternal icon
Public Health Leadership Forum. (2014). Defining and constituting foundational “capabilities” and “areas” version 1 (V-1). Retrieved from https://www.resolve.ngo/docs/articulation-of-foundational-capabilities-and-foundational-areas.v1.may_.pdfpdf iconexternal icon
Ramaswamy, R., Segal, S., Harris, J., Randolph, G.D., Cornett, A., Harrison, L.M., & Lea, C.S. (2012). Standardizing environmental health processes at the Iowa Department of Public Health. Journal of Public Health Management and Practice, 18(1), 27–35.
Resnick, B., Zablotsky, J., Nachman, K., & Burke, T. (2008). Examining the front lines of local environmental public health practice: A Maryland case study. Journal of Public Health Management and Practice, 14(1), 42–50.
Scutchfield, F.D., Marks, J.S., Perez, D.J., & Mays, G.P. (2007). Public health services and systems research. American Journal of Preventive Medicine, 33(2), 169–171.
Shah, G.H., Luo, H., & Sotnikov, S. (2014). Public health services most commonly provided by local health departments in the United States. Frontiers in Public Health Services & Systems Research, 3(1), 1–7.
Tables
Table 1 Part 1. Local Health Departments’ Organizational Characteristics and Environmental Health Services Provided in U.S. Communities, 2013
Table 1 Part 2 shows nine additional environmental health services.
| Organizational Characteristics | Body Art (Tattoo) | Campgrounds & Recreational Vehicles | Children’s Camps | Food Processing | Food Safety Education | Food Service Establishments | Groundwater Protection | Health-Related Facilities | Hotel / Motel | Indoor Air Quality |
|---|---|---|---|---|---|---|---|---|---|---|
| Per capita expenditure ($): 0–25 | 73.3 | 44.3 | 77.1 | 83.2 | 34.9 | |||||
| Per capita expenditure ($): 25–50 | 72.0 | 36.7 | 79.6 | 82.9 | 33.9 | |||||
| Per capita expenditure ($): 50–100 | 74.2 | 36.5 | 80.0 | 78.5 | 42.0 | |||||
| Per capita expenditure ($): ≥100 | 82.6 | 40.2 | 87.6 | 87.1 | 44.0 | |||||
| Per capita expenditure ($): χ2 | 8.4 | 7.6 | 11.7 | 8.3 | 10.9 | |||||
| Per capita expenditure ($): p-value | .03 | .05 | <.01 | .04 | <.01 | |||||
| Per capita income ($): 0–25 | 72.2 | 63.5 | 33.0 | 50.6 | ||||||
| Per capita income ($): 25–50 | 71.9 | 63.2 | 32.7 | 43.0 | ||||||
| Per capita income ($): 50–100 | 76.7 | 76.0 | 43.5 | 57.2 | ||||||
| Per capita income ($): ≥100 | 83.1 | 69.5 | 45.0 | 48.9 | ||||||
| Per capita income ($): χ2 | 10.1 | 15.9 | 17.2 | 12.9 | ||||||
| Per capita income ($): p-value | .02 | <.01 | <.01 | <.01 | ||||||
| Per capita other revenue ($): 0–5 | 70.1 | 57.7 | 64.7 | 77.5 | 79.8 | 47.1 | 34.3 | 47.7 | ||
| Per capita other revenue ($): 5–10 | 81.8 | 71.7 | 73.0 | 87.9 | 91.8 | 57.0 | 44.1 | 58.4 | ||
| Per capita other revenue ($): 10–50 | 82.6 | 78.0 | 75.9 | 86.2 | 87.6 | 57.7 | 41.5 | 51.0 | ||
| Per capita other revenue ($): ≥50 | 68.9 | 56.7 | 78.4 | 88.2 | 71.3 | 41.5 | 40.1 | 27.0 | ||
| Per capita other revenue ($): χ2 | 22.4 | 33.0 | 11.8 | 21.2 | 30.0 | 13.5 | 9.7 | 8.6 | ||
| Per capita other revenue ($): p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | .02 | .04 | ||
| Full-time equivalents (per 100,000): 0–1 | 52.4 | 44.0 | 54.9 | 35.8 | 59.9 | 61.0 | 32.7 | 28.9 | 50.1 | 38.3 |
| Full-time equivalents (per 100,000): 1–3 | 74.5 | 65.2 | 72.5 | 40.9 | 88.7 | 91.4 | 43.9 | 42.5 | 72.3 | 32.8 |
| Full-time equivalents (per 100,000): 3–5 | 78.9 | 66.8 | 71.2 | 48.1 | 90.5 | 94.2 | 45.4 | 39.2 | 73.9 | 50.7 |
| Full-time equivalents (per 100,000): 5–7 | 86.0 | 68.5 | 74.5 | 42.0 | 91.3 | 95.2 | 58.7 | 44.9 | 69.4 | 61.4 |
| Full-time equivalents (per 100,000): ≥7 | 88.1 | 76.2 | 80.8 | 48.4 | 91.7 | 97.4 | 68.4 | 50.6 | 73.3 | 57.2 |
| Full-time equivalents (per 100,000): χ2 | 213.0 | 116.5 | 687.0 | 23.2 | 301.2 | 456.1 | 169.4 | 61.5 | 96.4 | 70.3 |
| Full-time equivalents (per 100,000): p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 |
| Population size: 0–50,000 | 57.2 | 46.4 | 80.1 | 43.1 | 65.4 | 76.9 | ||||
| Population size: 50,000–150,000 | 68.1 | 39.7 | 88.2 | 50.8 | 67.8 | 86.0 | ||||
| Population size: ≥150,000 | 64.2 | 34.4 | 86.8 | 59.2 | 59.6 | 83.0 | ||||
| Population size: χ2 | 15.7 | 19.0 | 24.0 | 33.9 | 6.2 | 22.9 | ||||
| Population size: p-value | <.01 | <.01 | <.01 | <.01 | .04 | <.01 | ||||
| Governance type: Local | 62.9 | 40.3 | 79.0 | 81.3 | 51.5 | 37.9 | 60.4 | 53.4 | ||
| Governance type: Shared or state | 54.0 | 51.2 | 84.6 | 90.1 | 33.0 | 45.2 | 82.1 | 25.4 | ||
| Governance type: χ2 | 8.3 | 14.7 | 7.6 | 24.1 | 47.6 | 7.1 | 73.0 | 87.7 | ||
| Governance type: p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | ||
| Jurisdiction: City | 90.6 | 80.3 | 85.9 | 66.0 | 97.6 | 57.8 | 49.3 | 79.6 | 67.0 | |
| Jurisdiction: County | 70.4 | 58.1 | 64.4 | 39.1 | 81.0 | 44.6 | 37.8 | 63.2 | 42.9 | |
| Jurisdiction: Mixed | 69.4 | 65.0 | 70.1 | 36.7 | 78.5 | 55.0 | 37.5 | 61.1 | 50.2 | |
| Jurisdiction: χ2 | 56.3 | 34.2 | 56.9 | 69.5 | 84.9 | 24.9 | 13.2 | 28.5 | 51.7 | |
| Jurisdiction: p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | |
| Region: Northeast | 81.9 | 77.7 | 86.7 | 54.6 | 80.4 | 90.0 | 62.8 | 47.1 | 72.1 | 65.8 |
| Region: Midwest | 64.4 | 47.7 | 48.5 | 33.7 | 74.8 | 73.0 | 45.1 | 24.2 | 49.3 | 47.6 |
| Region: South | 83.0 | 69.0 | 76.1 | 44.0 | 88.5 | 93.6 | 42.8 | 53.5 | 78.5 | 37.9 |
| Region: East | 49.0 | 58.1 | 63.3 | 44.9 | 72.3 | 72.5 | 46.3 | 31.1 | 57.0 | 44.1 |
| Region: χ2 | 126.2 | 91.7 | 189.1 | 44.4 | 63.3 | 174.2 | 46.9 | 146.6 | 145.3 | 72.1 |
| Region: p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 |
Table 1 Part 2. Local Health Departments’ Organizational Characteristics and Environmental Health Services Provided in U.S. Communities, 2013
Table 1 Part 1 shows nine additional environmental health services.
| Organizational Characteristics | Lead Inspection | Private Drinking water | Public Drinking Water | Schools / Daycare | Septic Systems | Smoke-Free Ordinances | Surface Water Protection | Swimming Pools (Public) | Vector Control |
|---|---|---|---|---|---|---|---|---|---|
| Per capita expenditure ($): 0–25 | 66.9 | ||||||||
| Per capita expenditure ($): 25–50 | 61.2 | ||||||||
| Per capita expenditure ($): 50–100 | 69.8 | ||||||||
| Per capita expenditure ($): ≥100 | 68.6 | ||||||||
| Per capita expenditure ($): χ2 | 8.5 | ||||||||
| Per capita expenditure ($): p-value | .04 | ||||||||
| Per capita income ($): 0–25 | 64.0 | 65.3 | 33.1 | 74.3 | |||||
| Per capita income ($): 25–50 | 58.7 | 68.2 | 33.8 | 75.4 | |||||
| Per capita income ($): 50–100 | 72.5 | 71.5 | 42.3 | 81.3 | |||||
| Per capita income ($): ≥100 | 65.8 | 75.8 | 40.5 | 81.1 | |||||
| Per capita income ($): χ2 | 16.1 | 8.2 | 10.4 | 8.7 | |||||
| Per capita income ($): p-value | <.01 | .04 | .02 | .03 | |||||
| Per capita other revenue ($): 0–5 | 66.6 | 32.7 | 73.5 | 73.6 | 68.8 | 37.7 | 73.4 | ||
| Per capita other revenue ($): 5–10 | 76.9 | 46.9 | 81.4 | 86.9 | 76.9 | 46.8 | 88.7 | ||
| Per capita other revenue ($): 10–50 | 79.3 | 46.5 | 80.5 | 83.8 | 73.6 | 50.0 | 86.3 | ||
| Per capita other revenue ($): ≥50 | 73.1 | 37.4 | 61.7 | 71.3 | 86.8 | 31.3 | 57.6 | ||
| Per capita other revenue ($): χ2 | 19.9 | 26.8 | 12.0 | 30.0 | 8.6 | 14.6 | 43.6 | ||
| Per capita other revenue ($): p-value | <.01 | <.01 | <.01 | <.01 | .03 | <.01 | <.01 | ||
| Full-time equivalents (per 100,000): 0–1 | 51.7 | 45.8 | 27.6 | 59.1 | 53.3 | 56.3 | 28.3 | 58.1 | 42.4 |
| Full-time equivalents (per 100,000): 1–3 | 64.4 | 58.9 | 38.4 | 84.8 | 60.4 | 74.4 | 34.5 | 86.1 | 55.8 |
| Full-time equivalents (per 100,000): 3–5 | 74.9 | 69.8 | 40.3 | 84.1 | 85.3 | 75.1 | 37.1 | 91.0 | 69.3 |
| Full-time equivalents (per 100,000): 5–7 | 73.5 | 80.2 | 42.0 | 82.4 | 90.8 | 77.5 | 49.6 | 87.8 | 77.6 |
| Full-time equivalents (per 100,000): ≥7 | 75.7 | 87.4 | 50.0 | 86.5 | 92.2 | 84.0 | 55.5 | 92.0 | 73.6 |
| Full-time equivalents (per 100,000): χ2 | 100.8 | 284.4 | 71.2 | 186.0 | 388.6 | 125.5 | 106.4 | 298.0 | 177.1 |
| Full-time equivalents (per 100,000): p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 |
| Population size: 0–50,000 | 63.4 | 33.8 | 71.0 | 68.4 | 36.4 | 74.4 | |||
| Population size: 50,000–150,000 | 68.6 | 41.1 | 77.8 | 71.3 | 41.6 | 83.9 | |||
| Population size: ≥150,000 | 69.4 | 47.8 | 77.7 | 76.8 | 47.6 | 86.3 | |||
| Population size: χ2 | 7.1 | 26.6 | 13.3 | 10.8 | 16.8 | 38.2 | |||
| Population size: p-value | .03 | <.01 | <.01 | <.01 | <.01 | <.01 | |||
| Governance type: Local | 69.1 | 68.3 | 73.6 | 76.8 | 71.7 | 43.5 | 77.0 | 64.6 | |
| Governance type: Shared or state | 50.9 | 53.7 | 83.1 | 60.7 | 66.6 | 23.6 | 86.0 | 46.6 | |
| Governance type: χ2 | 42.4 | 30.0 | 19.5 | 46.7 | 4.0 | 56.01 | 18.7 | 42.0 | |
| Governance type: p-value | <.01 | <.01 | <.01 | <.01 | .04 | <.01 | <.01 | <.01 | |
| Jurisdiction: City | 80.6 | 31.6 | 83.6 | 90.5 | 81.8 | 50.1 | 94.2 | 79.4 | |
| Jurisdiction: County | 61.8 | 38.6 | 74.8 | 70.3 | 68.9 | 36.3 | 76.1 | 57.5 | |
| Jurisdiction: Mixed | 70.6 | 40.5 | 70.8 | 76.0 | 68.3 | 46.6 | 76.4 | 61.2 | |
| Jurisdiction: χ2 | 45.7 | 6.6 | 16.2 | 64.9 | 23.4 | 26.7 | 66.8 | 51.8 | |
| Jurisdiction: p-value | <.01 | .04 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | |
| Region: Northeast | 81.5 | 70.5 | 42.4 | 78.2 | 87.0 | 74.8 | 51.7 | 89.3 | 72.3 |
| Region: Midwest | 61.9 | 64.0 | 30.6 | 64.3 | 66.7 | 64.4 | 38.6 | 61.2 | 65.0 |
| Region: South | 63.7 | 69.6 | 38.4 | 89.1 | 78.7 | 75.5 | 30.8 | 92.7 | 54.5 |
| Region: East | 56.4 | 51.5 | 50.3 | 65.6 | 61.3 | 69.5 | 39.5 | 72.1 | 51.5 |
| Region: χ2 | 63.2 | 30.6 | 41.1 | 163.5 | 95.3 | 25.5 | 74.3 | 272.3 | 47.2 |
| Region: p-value | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 | <.01 |
Note: Table includes environmental health services provided by ≥30% of local health departments (LHDs). The table shows the percentages of LHDs providing these services directly or through contract. Only lower limits were included in a grouped range. The percentages are shown only for services with significant association with organizational characteristics. Mixed jurisdiction includes city-county, multicity, and multicounty. Numbers in bold indicate statistical significance (p<.05).
Table 2. Environmental Health Services and Providers in U.S. Communities, 2013
| Environmental Health Service | LHDa (%) | Othersb (%) | LHD and Othersc (%) | Contractor (%) | Not Available (%) | Don’t Know (%) |
|---|---|---|---|---|---|---|
| Air pollution | 15.7 | 54.7 | 7.7 | 1.6 | 12.3 | 15.7 |
| Body art (tattoo) | 55.2 | 21.3 | 1.7 | 2.1 | 14.0 | 7.4 |
| Campgrounds and recreational vehicles | 39.6 | 26.4 | 2.6 | 2.1 | 17.1 | 14.8 |
| Children’s camps | 48.5 | 23.2 | 4.0 | 2.2 | 13.1 | 13.0 |
| Collection of unused pharmaceuticals | 16.5 | 65.8 | 9.4 | 1.2 | 6.3 | 10.2 |
| Cosmetology businesses | 12.2 | 55.4 | 1.4 | 1.6 | 14.9 | 15.9 |
| Food processing | 32.1 | 46.4 | 4.3 | 2.0 | 11.0 | 8.5 |
| Food safety education | 72.4 | 18.6 | 14.9 | 2.2 | 3.5 | 3.3 |
| Food service establishments | 77.9 | 16.5 | 3.8 | 2.8 | 1.6 | 1.2 |
| Groundwater protection | 40.5 | 45.9 | 16.8 | 1.7 | 4.0 | 7.9 |
| Hazardous waste disposal | 15.0 | 70.3 | 7.3 | 2.5 | 4.9 | 7.3 |
| Hazardous materials response | 17.3 | 73.1 | 10.4 | 1.5 | 3.4 | 4.7 |
| Health-related facilities | 31.4 | 50.9 | 3.8 | 1.7 | 6.7 | 9.3 |
| Hotel/motel | 49.6 | 28.0 | 3.8 | 2.3 | 11.3 | 8.8 |
| Housing (inspection) | 25.9 | 54.0 | 6.6 | 1.3 | 7.1 | 11.7 |
| Indoor air quality | 30.7 | 36.3 | 8.8 | 2.4 | 18.1 | 12.5 |
| Land use planning | 14.1 | 68.4 | 6.7 | 0.8 | 5.3 | 11.4 |
| Lead inspection | 48.6 | 28.1 | 6.6 | 5.7 | 9.7 | 7.9 |
| Milk processing | 12.3 | 56.8 | 1.2 | 1.4 | 17.3 | 12.2 |
| Mobile homes | 27.7 | 32.5 | 2.2 | 1.6 | 19.9 | 18.3 |
| Noise pollution | 12.3 | 50.3 | 4.0 | 0.8 | 15.9 | 20.7 |
| Pollution prevention | 21.5 | 51.3 | 11.7 | 1.1 | 10.5 | 15.6 |
| Private drinking water | 55.7 | 30.6 | 7.3 | 2.6 | 5.6 | 5.5 |
| Public drinking water | 33.0 | 57.7 | 9.0 | 2.3 | 3.0 | 4.0 |
| Radiation control | 12.9 | 47.8 | 3.6 | 1.7 | 18.8 | 18.8 |
| School/daycare | 68.7 | 23.3 | 10.5 | 2.9 | 1.8 | 3.3 |
| Septic systems | 66.5 | 24.9 | 2.8 | 3.1 | 2.9 | 2.6 |
| Smoke-free ordinances | 58.8 | 25.3 | 10.5 | 2.1 | 7.6 | 6.2 |
| Solid waste disposal sites | 27.8 | 53.9 | 2.8 | 2.1 | 7.3 | 8.9 |
| Solid waste haulers | 27.7 | 51.7 | 1.5 | 2.1 | 6.1 | 12.4 |
| Surface water protection | 32.9 | 51.9 | 13.8 | 1.3 | 4.1 | 9.8 |
| Swimming pools (public) | 68.0 | 19.0 | 2.5 | 2.4 | 5.9 | 4.7 |
| Tobacco retailers | 25.0 | 44.1 | 3.4 | 2.7 | 10.6 | 17.6 |
| Vector control | 48.1 | 32.0 | 12.8 | 2.3 | 8.1 | 9.5 |
Table 3. Mean Number of Environmental Health Services Provided by Local Health Departments, 2013
| Organizational Characteristics | Mean Number of Services | p-Valuea |
|---|---|---|
| Population Size: 0–50,000 | 11 | <.01 |
| Population Size: 50,000–150,000 | 14 | |
| Population Size: ≥150,000 | 14 | |
| Per capita other revenue ($): 0–5 | 12 | <.01 |
| Per capita other revenue ($): 5–10 | 14 | |
| Per capita other revenue ($): 10–50 | 13 | |
| Per capita other revenue ($): ≥50 | 10 | |
| Per capita expenditure ($): 0–25 | 13 | <.01 |
| Per capita expenditure ($): 25–50 | 11 | |
| Per capita expenditure ($): 50–100 | 12 | |
| Per capita expenditure ($): ≥100 | 13 |
Note: Only lower limits were included in a grouped range.
ap-value was obtained from the F-statistic using PROC ANOVA.