Symptoms of Hand, Foot, and Mouth Disease
Symptoms of hand, foot, and mouth disease (HFMD) usually include fever, mouth sores, and skin rash. The rash is commonly found on the hands and feet.
Hand, foot, and mouth disease is common in infants and children younger than 5 years old. Most children have mild symptoms for 7 to 10 days.
Symptoms include

Children often get a fever and other flu-like symptoms 3 to 5 days after they catch the virus. These can include:
- Fever
- Eating or drinking less
- Sore throat
- Feeling unwell

Your child can get painful mouth sores. These sores usually start as small red spots, often on the tongue and insides of the mouth, that blister and can become painful.
Signs that swallowing might be painful for your child:
- Not eating or drinking
- Drooling more than usual
- Only wanting to drink cold fluids
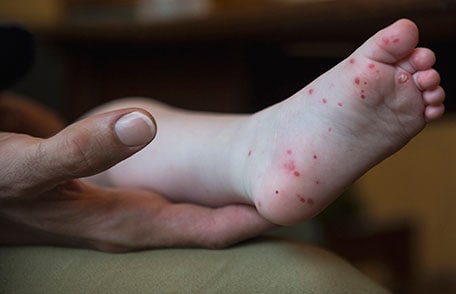
Your child can get a skin rash on the palms of the hands and soles of the feet. It can also show up on the buttocks, legs, and arms.
The rash usually is not itchy and looks like flat or slightly raised red spots, sometimes with blisters that have an area of redness at their base. Fluid in the blister can contain the virus that causes HFMD.
Keep blisters clean and avoid touching them.
Treat symptoms at home
Often a HFMD infection is mild, and symptoms can be treated at home.
Treat Hand, Foot, and Mouth DiseaseWhen to see a healthcare provider
- Your child is not able to drink normally and you’re worried they might be getting dehydrated.
- Your child’s fever lasts longer than 3 days.
- Symptoms do not improve after 10 days.
- Your child has a weakened immune system (body’s ability to fight germs and sickness).
- Symptoms are severe.
- Your child is very young, especially younger than 6 months.
Healthcare providers can usually tell if someone has HFMD by examining the patient and the rash appearance while considering the patient’s age and other symptoms.
Sometimes, healthcare providers might collect samples from the patient’s throat or feces (poop) and send them to a laboratory to test for the virus. However, these tests are rarely done.

Wash your hands often for at least 20 seconds to stop germs from spreading.


