Healthcare Response Activities
If there is ever an emergency caused by the release of B. mallei, hospitals and other healthcare facilities will be called upon to diagnose, treat, and care for patients with glanders.
Treat and Care for Patients
All patients with glanders will need to be treated with the appropriate antibiotic treatment regimen. Treatment consists of two rounds: an intravenous round and an oral eradication round. The first round of treatment usually lasts 10 to 14 days, but may last longer for patients with more severe disease. The follow-on eradication round lasts 3 to 6 months.
Read the full treatment recommendations for glanders in Emerging Infectious Diseases
Treatment recommendations for glanders are based upon the treatment recommendations of melioidosis. Melioidosis is caused by B. pseudomallei, which is similar to B. mallei. In an emergency, CDC will work with physicians treating patients with glanders to monitor the success of recommended treatments and modify these recommendations, if needed.
Some patients may require intensive care, including ventilator support. Depending upon the scale of the emergency event, your healthcare facility may have many patients requiring intensive care for several days or weeks.
In an emergency, healthcare professionals and facilities should communicate with their state public health department’s medical countermeasures coordinator to request additional supplies, such as ventilators, from the Strategic National Stockpile.
Identify Patients Requiring Treatment
Depending upon the circumstances of the emergency, some individuals who developed symptoms soon after coming into contact with B. mallei, but before the emergency was identified, may have been diagnosed as having illnesses other than glanders. Healthcare facilities may need to work with public health authorities to perform tasks such as chart reviews to identify and contact individuals who require further examination and treatment.
Infection Control
Healthcare workers should follow standard and airborne precautions when caring for patients with glanders. Person-to-person transmission of the disease is possible, though there have been only a few documented cases.
Environmental Control
Current practices to disinfect and sterilize patient-care equipment and environmental surfaces are sufficient for managing areas where glanders patients are evaluated, admitted, and treated.
Protect Laboratory Staff
Laboratory personnel who handle specimens from patients suspected of having glanders or cultures of B. mallei are at risk of laboratory-acquired glanders. In contrast to other healthcare personnel, laboratory personnel are at risk because some procedures required to prepare specimens for culture may aerosolize particles and release B. mallei into the air. Laboratory personnel who have been exposed to B. mallei should begin post-exposure prophylaxis immediately.
Laboratory personnel can reduce their risk of exposure by following good laboratory practices. Laboratory personnel should take precautions by:
- Performing work with clinical specimens using Biosafety Level 2 (BSL-2) practices*
- Always using appropriate personal protective equipment when working with the specimens or cultures
- Performing work with cultures or any tasks that generate aerosols or droplets in BSL-3 facilities
Respiratory protection is essential when centrifuging or performing any other tasks outside of a biological safety cabinet (BSC).
*Clinical diagnostic laboratories functioning at BSL-2 may isolate B. mallei from patient specimens. Once B. mallei is suspected, transfer work to BSL-3 facilities.
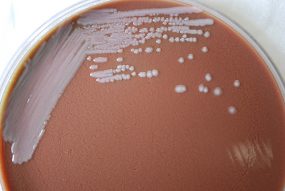
Colonial morphology displayed by gram-negative Burkholderia mallei bacteria, which were grown on a medium of chocolate agar for a 48 hour time period at a temperature of 37° Celsius.
Laboratory-related Exposure
If a laboratory worker is exposed to B. mallei, immediately wash and decontaminate the inoculation site (if there is one). Report the incident to the laboratory safety manager, and perform a risk assessment to determine whether the incident poses a low-risk or a high-risk.
Learn how to manage an accidental laboratory exposure to B. mallei
The type of exposure determines the course of post-exposure management, summarized here:
| Type of exposure | Post-exposure Management |
|---|---|
| High-risk incident | Begin post-exposure prophylaxis immediately Fever monitoring |
| Low-risk incident | Fever monitoring only |
Laboratory workers who have been exposed to B. mallei should record their temperatures twice a day for 21 days (fever monitoring). Workers who were exposed and develop any of the following symptoms should seek medical care immediately and inform their clinician about their exposure to B. mallei:
- Fever greater than 100.4°F (38°C)
- Cough
- Progressive inflammation at the site of known inoculation (if there is one)