Fire Fighter Trainee Suffers Sudden Cardiac Death During Maze Training – Virginia
 Death in the Line of Duty…A summary of a NIOSH fire fighter fatality investigation
Death in the Line of Duty…A summary of a NIOSH fire fighter fatality investigation
F2009-02 Date Released: July 2009
SUMMARY
On November 9, 2008, a 42-year-old female volunteer fire fighter trainee participated in an entry-level fire fighter certification class. The training included turnout gear dressing drills, hose maze, self-contained breathing apparatus (SCBA) skill station/low profile, and maneuvering through a maze with no smoke or fire while wearing full turnout gear and SCBA.
After completing the hose maze evolution, the Trainee was tired and sweating heavily. After lunch, the Trainee began the maze portion and completed approximately half of the exercise when her SCBA low-air alarm sounded. The Trainee informed the instructor that she wanted to continue. After entering the next portion of the maze and crawling up a slight incline, she did not turn around and back down the decline as required. The Instructor saw that something was wrong and spoke to the Trainee but received no response. At this time, the Trainee’s personal alert safety system (PASS) alarm sounded. It took instructors about 10 minutes to remove the Trainee from the maze.
Once outside the maze, the Trainee was found to be unresponsive, not breathing, and without a pulse. An ambulance was requested, and cardiopulmonary resuscitation (CPR) was begun. The ambulance arrived about 7 minutes later, and paramedics began advanced life support. One defibrillation was administered without a change in heart rhythm. The Trainee was transported to the hospital’s emergency department, where CPR and advanced life support treatment continued. Approximately 59 minutes after her collapse, despite CPR and advanced life support, the Trainee died. The death certificate and the autopsy, completed by the Medical Examiner, listed “arrhythmogenic right ventricular cardiomyopathy/dysplasia” as the cause of death. NIOSH investigators conclude that the physical exertion involved in performing the fire fighter training exercises, coupled with the Trainee’s underlying cardiomyopathy/dysplasia and enlarged heart (cardiomegaly), triggered her sudden cardiac death.
NIOSH investigators offer the following recommendations to address general safety and health issues. Had these recommended measures been in place prior to the Trainee’s collapse, it is possible her sudden cardiac death may have been prevented.
- Provide preplacement and annual medical evaluations to fire fighters.
- Incorporate medical monitoring of trainees into rehabilitation programs.
- Educate fire fighters to report signs and symptoms consistent with a heart attack to appropriate authorities for prompt medical evaluation.
- Perform a preplacement and an annual physical performance (physical ability) evaluation.
- Ensure fire fighters are cleared for return to duty by a physician knowledgeable about the physical demands of fire fighting, the personal protective equipment used by fire fighters, and the various components of NFPA 1582.
- Phase in a comprehensive wellness and fitness program for fire fighters.
- Provide fire fighters with medical clearance to wear a self-contained breathing apparatus (SCBA) as part of the Fire Department’s medical evaluation program.
- Ensure that all SCBA training is conducted in accordance with NFPA 1404, Standard for Fire Service Respiratory Protection Training.
- Ensure that training maze props or trailers used in SCBA confidence training have adequate safety features such as emergency egress panels, emergency lighting, ventilation, and a temperature monitoring system to measure the ambient temperature inside the maze.
INTRODUCTION & METHODS
On November 9, 2008, a 42-year-old female volunteer fire fighter trainee suffered sudden cardiac death during fire fighter training. Despite CPR and advanced life support, the Trainee died. NIOSH was notified of this fatality on November 10, 2008, by the U.S. Fire Administration. NIOSH contacted the affected Fire Department on November 12, 2008, to gather additional information, and on December 4, 2008, to initiate the investigation. On January 26, 2009, two safety and occupational health specialists from the NIOSH Fire Fighter Fatality Investigation Team traveled to Virginia to conduct an on-site investigation of the incident.
During the investigation, NIOSH personnel interviewed the following people:
- County Environmental Health and Safety Manager
- Battalion Chief of the career County Fire Department
- Battalion Chief of the volunteer Fire Department
- Coordinator of the Fire Training Center
- Trainee’s spouse
NIOSH personnel reviewed the following documents:
- Fire Department policies and operating guidelines
- Fire Department training records
- Fire Department annual report for 2008
- Witness statements
- Dispatch report
- Emergency medical service (ambulance) incident report
- Hospital emergency department records
- Death certificate
- Autopsy report
- Primary care provider medical records
RESULTS OF INVESTIGATION
Background
Public Safety Training Center. The County’s Public Safety Training Center (PSTC), a combined Police and Fire and Rescue Academy, is responsible for fire, rescue, and emergency medical service (EMS) training for both career and volunteer members. The PSTC is authorized to teach Firefighter I & II, Driver Operator, Instructor 1 & 2, Officer 1 & 2, Emergency Medical Technician-Basic (EMT-B), Emergency Medical Technician-Intermediate (EMT-I), Advanced Life Support and Basic Life Support protocols, CPR, and other courses. These fire and rescue courses are taught by an instructor cadre group that mainly instructs the fire fighting class, and an outside contractor that conducts the EMT-B and EMT refresher classes.
The PSTC is a 30-acre facility comprised of a backdraft simulator, a flashover simulator, a 5-story burn building/tower, and a maze. One medic unit, three engines, and one ladder truck service the PSTC with 18 full-time personnel. Advanced life support equipment is available on site at all times; paramedics, part of the time. The practical drill maze was built in 2007 from a metal sea shipping container (see Sketch 1 and Photograph 1). It tests students for claustrophobia, Fire Fighter I critical performance standards, and obstacle negotiation as required in NFPA 1001, Standard for Fire Fighter Professional Qualifications [NFPA 2008a].
Training Class. The training being conducted during this incident consisted of classroom, personal protective equipment (PPE) dressing drills, hose maze, SCBA skill station/low profile, and practical maze drill described in Appendix A.
Incident. On Sunday, November 9, 2008, 12 students, including the Trainee, met at the PSTC to complete their fire fighter certification training. The class began at 0800 hours. Weather conditions included a temperature of 43 degrees Fahrenheit (°F) and 76% relative humidity [NOAA 2008]. The lead instructor discussed the training components, rehabilitation, PPE, building description, and emergency evacuation procedures. The Trainee successfully completed the classroom and PPE dressing drills.
After a short break, the group was split into two groups of six students to perform the SCBA skill station/low profile and hose maze training. Donning her SCBA over her turnout gear, she completed the low profile station without any problems or health complaints. However, during the hose maze (crawling along a hose to locate the exit with a covered SCBA facepiece) the Trainee became disoriented and proceeded back to the entrance as her SCBA cylinder’s low air alarm sounded. After resting a few minutes and getting another air cylinder, she successfully completed the evolution. At this point, however, she seemed to be more short of breath, sweatier and more tired than the other trainees. She confided to one trainee that she did not feel well (tired and dizzy), but she did not mention this to the instructor. The class took a 30-minute lunch break during which time the Trainee drank some water, rested, and ate some food.
The class reassembled at 1315 hours for the practical maze drill. At this time weather conditions included a temperature of 59°F and 33% relative humidity [NOAA 2008]. Instructors briefed the students and asked if anyone was claustrophobic. The Trainee stated that she was claustrophobic but wanted to continue with the drill anyway. Wearing full turnout gear and SCBA, the Trainee began breathing SCBA air and entered the maze at approximately 1417 hours. Her SCBA was a Mine Safety Appliance (MSA) Firehawk® 4500 with integrated Personal Alert Safety System (PASS). Her SCBA was essentially full (4,260 pounds per square inch [psi] of air [4,500 psi full capacity]). While she moved through the maze, the instructors remained in voice contact with her from just outside the maze wall. As she entered the “big room” portion of the maze, her SCBA low air alarm sounded (sounds when 25% of the tank’s air remains). Instructors asked if she wanted to continue or stop. The Trainee said, “I made it this far, keep going.”
The Trainee entered the incline/turnaround/decline section of the maze (see Photographs 2 and 3). She crawled to the top of the incline, but failed to turn around. Instructors then noticed her boots had fallen off. At this time the Trainee stopped breathing air from her SCBA (1438 hours) even though 1,000 psi of air remained, and her PASS alarm activated (1439 hours). Sensing something was wrong, the two instructors entered the maze. When the instructors reached the Trainee, she was unresponsive. A third instructor was directed to notify the lead instructor and to call 911. A fourth instructor called 911 (1445 hours) and advised a staff member to retrieve the ambulance at the nearby PSTC.
At approximately 1449 hours the Trainee was removed from the maze; instructors had to move the Trainee back up the incline section to get her out. Assessment revealed the Trainee was unresponsive, not breathing, and had no pulse; CPR was begun and an oral airway was placed. An off-site ambulance was first to arrive on scene (1452 hours). A cardiac monitor/automated external defibrillator (AED) did not advise a defibrillation (shock), and CPR continued. The on-site PSTC ambulance arrived shortly thereafter (about 1453 hours). The first paramedic unit (Medic 525) arrived on scene at 1500 hours and began advanced life support, which included placing an intravenous line and intubation. Tube placement was confirmed by auscultation and visualization. Secondary confirmation using a technology test [AHA 2000] could not be performed due to excessive secretions in the tube. A cardiac monitor was placed, revealing asystole (no heart rhythm).
Medic 525 departed the scene at 1502 hours en route to the hospital’s emergency department. En route, the Trainee was re-intubated due to suspected dislodgement. Again, tube placement was confirmed by auscultation and visualization but not a secondary technology test as recommended by the AHA [AHA 2000]. Her heart rhythm changed to ventricular fibrillation, and one defibrillation attempt (shock) was administered with no positive change in the Trainee’s heart rhythm or her condition during transport. The ambulance arrived at the hospital at 1522 hours. Inside the emergency department, advanced life support treatment continued for another 15 minutes with no change in her clinical condition. At 1537 hours, the trainee was pronounced dead by the attending physician.
Medical Findings. The death certificate and the autopsy, completed by a pathologist in the Office of the Chief Medical Examiner, listed “arrhythmogenic right ventricular cardiomyopathy/dysplasia” as the cause of death. Key findings from the autopsy included no coronary artery disease, enlarged right and left ventricles, and cardiomegaly. Histologic (microscopic) examination revealed fibrotic and fatty tissue infiltrating the right greater than the left ventricles. Specific findings from the autopsy report are listed in Appendix B.
The Trainee was 65 inches tall and weighed 241 pounds, giving her a body mass index (BMI) of 40.1 kilograms per meters squared (kg/m2). A BMI >30.0 is considered obese [CDC 2009]. In 2003, she was diagnosed with high blood pressure (hypertension) but was not prescribed a blood pressure-lowering medication until 2007. Her blood pressure was well controlled with this medication. An echocardiogram performed in 2005 for a heart murmur revealed a normal left ventricular ejection fraction (60%) but right ventricular enlargement (34 millimeters [mm]; normal is < 27mm), left atrial enlargement (42mm [normal is < 40mm]), and mild tricuspid valve regurgitation. Repeat echocardiograms in 2006 and 2007 revealed similar findings, with no changes in these cardiac dimensions. Her last visit to her primary care provider was for follow-up of her high blood pressure 6 days before she died. She did not report heart-related symptoms (chest pain, chest pressure, angina, shortness of breath on exertion, etc.) at this time to her physicians, her family, the Fire Department, or the PSTC.
DESCRIPTION OF THE FIRE DEPARTMENT
At the time of the NIOSH investigation, the volunteer Fire Department consisted of four fire stations with 190 uniformed personnel that served 30,000 residents in a geographic area of 27.7 square miles. It is one of 11 volunteer fire and rescue departments in the county. The career County fire department provides administration, operational, logistical, and coordination for these 11 volunteer fire and rescue departments. In 2008, the volunteer Fire Department responded to 16,826 calls and 7,981 incidents.
Membership and Training. The Fire Department requires new fire fighter applicants to complete an application, pass a driver’s license check, pass a criminal background check, and be approved by the membership committee. The new member is placed into one of three categories: (1) associate member who performs no emergency responses, (2) emergency medical service member who performs medical responses only, or (3) fire fighter who responds to fire calls and medical calls. New volunteer members must attend the 150-hour Fire Fighter I (FFI) training course to become certified as a fire fighter. The Trainee was attending the PSTC for FFI certification. The Trainee had previously taken the Emergency Medical Technician, Hazardous Materials Awareness, and the Emergency Vehicle Operators Course. She had 8 years of emergency medical experience prior to her month as a fire fighter trainee.
Preplacement and Periodic Medical Evaluations. In 2003, the Fire Department began requiring preplacement medical evaluations. The evaluations are performed by a contract physician. At the time of this report NIOSH was unable to review this medical record, or even confirm that a preplacement medical evaluation had taken place. After this incident, the PSTC now requires a medical evaluation and SCBA medical clearance for each trainee. The medical clearance form, which includes a description of fire fighting duties as described in NFPA 1582, is given to trainees to provide to their primary care physician, who performs the medical evaluation. The medical clearance is then given to the county Health and Safety Officer who makes the final determination to clear the trainee to attend training.
Prior to this incident neither annual medical evaluations nor SCBA medical clearance were required. The Fire Department is planning to implement annual programs in 2009. An annual SCBA facepiece fit test is required by the Fire Department for interior structural fire fighters. Members injured on duty must be evaluated by their primary care physician who makes a recommendation regarding return to duty. The final decision regarding return to duty is made by the Fire Department’s Board of Directors.
Health and Wellness Programs. The Fire Department does not have a formal wellness/fitness program, but exercise (strength only) equipment is available in the four fire stations operated by this Fire Department, and employee assistance programs, if requested, are available from the County.
DISCUSSION
Arrhythmogenic Right Ventricular Cardiomyopathy/Dysplasia (ARVCM/D). ARVCM/D is a cardiomyopathy, most commonly inherited, characterized by progressive replacement of the muscle of the heart’s right ventricle with fibrous and fatty tissue. This process also occurs in the heart’s left ventricle although to a much lesser extent [Gemayel et al. 2001; Thiene et al. 2007; Wynne and Braunwald 2008]. Patients typically present in their 20s with symptoms and signs of right ventricular failure (swollen ankles, enlarged liver). When the disease involves the ventricular septum and the left ventricle, symptoms and signs of left ventricular failure appear (shortness of breath, particularly upon exertion) [Thiene et al. 2007]. At all ages, patients with ARVCM/D are at risk for ventricular tachyarrhythmias and sudden cardiac death [Gemayel et al. 2001; Wynne and Braunwald 2008]. In the United States, ARVCM/D accounts for approximately 5% of sudden cardiac deaths in individuals under the age of 65, and about 4% of deaths associated with physical activity in young athletes [Gemayel et al. 2001].
The diagnosis of ARVCM/D is suspected by an echocardiogram that reveals right ventricular enlargement, right ventricular wall motion abnormalities, and less commonly right ventricular apical aneurysm formation [Wynne and Braunwald 2008]. A definitive diagnosis of ARVCM/D, however, requires the microscopic finding of transmural fibrofatty replacement of the right ventricular myocardium [Gemayel et al. 2001]. In this case, the Trainee did not have a family history of ARVCM/D, nor did she report symptoms of right or left ventricular failure prior to the training. She did have echocardiograms for a heart murmur in 2005, 2006, and 2007 that showed her right ventricular enlargement. It is unclear why further medical evaluation of this finding was not undertaken.
The Trainee had performed maze training while wearing full turnout gear and SCBA. During the training, she expressed symptoms consistent with mild left ventricular failure. The training she undertook is considered heavy physical activity [AIHA 1971; Gledhill and Jamnik 1992]. Given the Trainee’s underlying ARVCM/D, her sudden cardiac death was probably triggered by the physical stress of the fire fighter training in full turnout gear and SCBA.
Occupational Medical Standards for Structural Fire Fighters. To reduce the risk of sudden cardiac arrest or other incapacitating medical conditions among fire fighters, the NFPA developed NFPA 1582, Standard on Comprehensive Occupational Medical Program for Fire Departments [NFPA 2007a]. This voluntary industry standard provides (1) the components of a preplacement and annual medical evaluation and (2) medical fitness for duty criteria. ARVCM/D is not specifically mentioned in NFPA 1582. However, it is one type of cardiomyopathy, a Category A condition for candidates that “precludes a person from performing as a member in a training or emergency operational environment by presenting a significant risk to the safety and health of the person or others” [NFPA 2007a]. Had a preplacement medical evaluation been performed consistent with NFPA 1582, including a workup for her documented right ventricular enlargement, perhaps a definitive diagnosis of ARVCM/D could have been made. With this diagnosis, perhaps the Trainee would have been precluded from performing fire fighter training and would not have suffered sudden cardiac death at this time.
RECOMMENDATIONS
NIOSH investigators offer the following recommendations to address general safety and health issues. Had these recommended measures been in place prior to the Trainee’s collapse, it is possible her sudden cardiac death may have been prevented.
Recommendation #1: Provide preplacement and annual medical evaluations to fire fighters.
Guidance regarding the content and frequency of these medical evaluations can be found in NFPA 1582 and in the International Association of Fire Fighters (IAFF)/International Association of Fire Chiefs (IAFC) Fire Service Joint Labor Management Wellness/Fitness Initiative [IAFF, IAFC 2000; NFPA 2007a]. These evaluations are performed to determine fire fighters’ medical ability to perform duties without presenting a significant risk to the safety and health of themselves or others. However, the Fire Department and the Training Center are not legally required to follow this standard or this initiative. Applying this recommendation involves economic repercussions and may be particularly difficult for small volunteer fire departments to implement.
To overcome the financial obstacle of medical evaluations, the Fire Department could urge current members to get annual medical clearances from their private physicians. Another option is having the annual medical evaluations completed by paramedics and emergency medical technicians (EMTs) from the local EMS (vital signs, height, weight, visual acuity, and electrocardiogram [EKG]). This information could then be provided to a community physician (perhaps volunteering his or her time), who could review the data and provide medical clearance (or further evaluation, if needed). The more extensive portions of the medical evaluations could be performed by a private physician at the fire fighter’s expense (personal or through insurance), provided by a physician volunteer, or paid for by the Fire Department, City, or State. Sharing the financial responsibility for these evaluations between fire fighters, the Fire Department, the City, the State, and physician volunteers may reduce the negative financial impact on recruiting and retaining needed fire fighters.
Recommendation #2: Incorporate medical monitoring of trainees into rehabilitation programs.
A model rehabilitation program can be found in NFPA 1584, Standard on the Rehabilitation Process for Members During Emergency Operations and Training Exercises [NFPA 2008b]. Medical monitoring should be part of any rehabilitation program. This would consist of evaluating the symptoms, signs, and vital signs of personnel upon entry to, and discharge from, the rehabilitation program. These findings should be recorded and maintained. Symptomatic members or members with abnormal findings should receive additional monitoring and be evaluated for potential transport to the emergency department. If medical care is given, a medical report should be completed and maintained. In this incident, all participants should have been assigned to rehabilitation after the hose maze drill. Perhaps if the Trainee had gone to rehabilitation and her vital signs (including pulse oximetry) were checked, an abnormality might have been detected. This may have led to the Trainee being referred for further medical diagnosis/treatment.
Recommendation #3: Educate fire fighters to report signs and symptoms consistent with a heart attack to appropriate authorities for prompt medical evaluation.
The Trainee was a certified Emergency Medical Technician. Her training included recognizing the signs and symptoms of heart attacks [American Red Cross 1997]. Recognizing these signs and symptoms in oneself is often difficult, particularly if the symptoms could have been easily attributed to heavy physical exertion during the training (shortness of breath, heavy sweating, and excess fatigue). However, as mentioned in Recommendation #2, if the Trainee was evaluated in rehabilitation after the hose maze drill, perhaps her symptoms would have resulted in further medical evaluation. This evaluation may have led to diagnosis of her condition and possibly treatment prior to her sudden cardiac death.
Recommendation #4: Perform a preplacement and an annual physical performance (physical ability) evaluation.
NFPA 1500, Standard on Fire Department Occupational Safety and Health Program, requires the fire department to develop physical performance requirements for candidates and members who engage in emergency operations [NFPA 2007b]. Members who engage in emergency operations must be annually qualified (physical ability test) as meeting these physical performance standards for structural fire fighters [NFPA 2007b]. Because this Trainee never completed a physical ability test, it is unclear if her fitness level was appropriate for unrestricted duty as a structural fire fighter.
Recommendation #5: Ensure that fire fighters are cleared for return to duty by a physician knowledgeable about the physical demands of fire fighting, the personal protective equipment used by fire fighters, and the various components of NFPA 1582.
Guidance regarding medical evaluations and examinations for structural fire fighters can be found in NFPA 1582 [NFPA 2007a] and in the IAFF/IAFC Fire Service Joint Labor Management Wellness/Fitness Initiative [IAFF, IAFC 2000]. According to these guidelines, the Fire Department should have an officially designated physician who is responsible for guiding, directing, and advising the members with regard to their health, fitness, and suitability for duty. The physician should review job descriptions and essential job tasks required for all Fire Department positions and ranks to understand the physiological and psychological demands of fire fighters and the environmental conditions under which they must perform, as well as the personal protective equipment they must wear during various types of emergency operations. This recommendation is made based on review of the Fire Department health and medical programs.
Recommendation #6: Phase in a comprehensive wellness and fitness program for fire fighters.
Guidance for fire department wellness/fitness programs to reduce risk factors for cardiovascular disease and improve cardiovascular capacity is found in NFPA 1583, Standard on Health-Related Fitness Programs for Fire Fighters, and the IAFF/IAFC Fire Service Joint Labor Management Wellness/Fitness Initiative [IAFF, IAFC 2000; NFPA 2008c]. Worksite health promotion programs have been shown to be cost effective by increasing productivity, reducing absenteeism, and reducing the number of work-related injuries and lost work days [Stein et al. 2000; Aldana 2001]. Fire service health promotion programs have been shown to reduce coronary artery disease risk factors and improve fitness levels, with mandatory programs showing the most benefit [Dempsey et al. 2002; Womack et al. 2005; Blevins et al. 2006]. A recent study conducted by the Oregon Health and Science University reported a savings of more than $1 million for each of four large fire departments implementing the IAFF/IAFC wellness/fitness program compared to four large fire departments not implementing a program. These savings were primarily due to a reduction of occupational injury/illness claims with additional savings expected from reduced future nonoccupational healthcare costs [Kuehl 2007].
The National Volunteer Fire Council (NVFC) and the U.S. Fire Administration (USFA) Health and Wellness Project Health and Wellness Guide, was developed to improve health and wellness within the volunteer fire service [USFA 2004]. Given the size of this volunteer Fire Department, this may be more relevant than the programs listed above.
Recommendation #7: Provide fire fighters with medical clearance to wear SCBA as part of the Fire Department’s medical evaluation program.
The Occupational Safety and Health Administration (OSHA) Revised Respiratory Protection Standard requires employers to provide medical evaluations and clearance for employees using respiratory protection [29 CFR1 1910.134]. These clearance evaluations are required for private industry employees and public employees in States operating OSHA-approved State plans. Virginia operates an OSHA-approved State plan; therefore the Fire Department should ensure all members have been medically cleared to wear an SCBA. In addition, the PSTC should ensure all trainees have been medically cleared to wear an SCBA. Medical records obtained by NIOSH did not indicate the Trainee’s clearance. The PSTC program has been implemented since the Trainee’s death.
Recommendation #8: Ensure that all SCBA training is conducted in accordance with NFPA 1404, Standard for Fire Service Respiratory Protection Training.
NFPA 1404 [NFPA 2006] covers the minimum requirements for the training component of the respiratory protection program found in NFPA 1500 [NFPA 2007b]. The purpose of NFPA 1404 is to specify the minimum requirements for respiratory protection training for the emergency response organization, including safety procedures for those involved in fire suppression, rescue, and other related activities in a toxic, contaminated, or oxygen deficient atmosphere or environment. Chapter 6 of NFPA 1404 provides guidance for recruit training in respiratory protection that describes the minimum requirements of instructors, record keeping, minimum performance, fit testing, and medical and physical fitness standards references as well as respiratory protection training safety.
Recommendation #9: Ensure that training maze props or trailers used in SCBA confidence training have adequate safety features such as emergency egress panels, emergency lighting, ventilation, and a temperature monitoring system to measure the ambient temperature inside the maze.
Some training props (such as an SCBA training maze) contain confined space areas for skill building of fire fighters by restricting the maneuvering/working area of the fire fighter. Combined with reduced visibility and other conditions designed to simulate fireground conditions, these props challenge the fire fighters and improve their skills and confidence in using SCBA. Many of these training mazes are designed and constructed by fire departments and may not possess all of the necessary safety features to provide for emergency medical conditions of users. Although no fire or smoke conditions are introduced into these training maze props, fire fighters have experienced serious medical conditions while inside the props and have had to be extricated before treatment could be rendered. Extricating a fire fighter who has suffered a debilitating medical condition inside a severely restricted space is difficult and can be time consuming and labor intensive. Emergency egress panels that would allow for easy removal of fire fighters experiencing a medical event should be located inside the confined space areas. Emergency lighting should be provided for users and rescuers. The fire fighters often have PPE, SCBA, and other equipment that may have to be disentangled in order to remove them, and emergency lighting will aid in the extrication and removal. Many training mazes are outdoor semipermanent trailer designs that are exposed to temperature extremes. A temperature monitoring system inside the training maze would allow the instructors to monitor temperature extremes and adjust the training accordingly. Ventilation of training mazes should be considered to control the temperatures. Additional information concerning training props can be found in NFPA 1402, Guide to Building Fire Service Training Centers [NFPA 2007c].
In this incident, the victim experienced a medical condition inside the training maze and had to be removed before medical assistance could be provided. When she experienced the medical condition, she was in a portion of the training maze that was not immediately accessible to the instructors. The instructors had to enter the training maze and physically remove her back up the incline (see Photograph 2) with all of her gear including her SCBA.
1Code of Federal Regulations. See CFR in references.
REFERENCES
AHA [2000]. Advanced cardiovascular life support: section 3: adjuncts for oxygenation, ventilation, and airway control. Circ 102(8)(Suppl):I-95 – I-104.
AIHA [1971]. Ergonomics guide to assessment of metabolic and cardiac costs of physical work. Am Ind Hyg Assoc J 32(8):560–564.
Aldana SG [2001]. Financial impact of health promotion programs: a comprehensive review of the literature. Am J Health Promot 15(5):296–320.
American Red Cross [1997]. Emergency response. St. Louis, MO: Mosby Lifeline.
Blevins JS, Bounds R, Armstrong E, Coast JR [2006]. Health and fitness programming for fire fighters: does it produce results? Med Sci Sports Exerc 38(5):S454.
CDC (Centers for Disease Control and Prevention) [2009]. BMI – Body Mass Index. [www.cdc.gov/healthyweight/assessing/bmi/adult_bmi/english_bmi_calculator/bmi_calculator.html]. Date accessed: June 2009.
CFR. Code of Federal Regulations. Washington, DC: U.S. Government Printing Office, Office of the Federal Register.
Dempsey WL, Stevens SR, Snell CR [2002]. Changes in physical performance and medical measures following a mandatory firefighter wellness program. Med Sci Sports Exerc 34(5):S258.
Gemayel C, Pelliccia A, Thompson PD [2001]. Arrhythmogenic right ventricular cardiomyopathy. J Am Coll Cardiol 38(7):1773–1781.
Gledhill N, Jamnik VK [1992]. Characterization of the physical demands of firefighting. Can J Spt Sci 17(3):207–213.
IAFF, IAFC [2000]. The fire service joint labor management wellness/fitness initiative. 2nd ed. Washington, DC: International Association of Fire Fighters, International Association of Fire Chiefs.
Kuehl K [2007]. Economic impact of the wellness fitness initiative. Presentation at the 2007 John P. Redmond Symposium in Chicago, IL on October 23, 2007.
NFPA [2006]. Standard for fire service respiratory protection training. Quincy, MA: National Fire Protection Association. NFPA 1404.
NFPA [2007a]. Standard on comprehensive occupational medical program for fire departments. Quincy, MA: National Fire Protection Association. NFPA 1582.
NFPA [2007b]. Standard on fire department occupational safety and health program. Quincy, MA: National Fire Protection Association. NFPA 1500.
NFPA [2007c]. Guide to building fire service training centers. Quincy, MA: National Fire Protection Association. NFPA 1402.
NFPA [2008a]. Standard for fire fighter professional qualifications. Quincy, MA: National Fire Protection Association. NFPA 1001.
NFPA [2008b]. Standard on the rehabilitation process for members during emergency operations and training exercises. Quincy, MA: National Fire Protection Association. NFPA 1584.
NFPA [2008c]. Standard on health-related fitness programs for fire fighters. Quincy, MA: National Fire Protection Association. NFPA 1583.
NOAA [2008]. Quality controlled local climatological data.external icon National Oceanic and Atmospheric Administration. [http://cdo.ncdc.noaa.gov/qclcd/QCLCD]. Date accessed: June 2009.
Stein AD, Shakour SK, Zuidema RA [2000]. Financial incentives, participation in employer sponsored health promotion, and changes in employee health and productivity: HealthPlus health quotient program. J Occup Environ Med 42(12):1148–1155.
Thiene G, Corrado D, Basso C [2007]. Arrhythmogenic right ventricular cardiomyopathy/ dysplasia. Orph J Rare Dis 2:45.
USFA [2004]. Health and wellness guide. Emmitsburg, MD: Federal Emergency Management Agency; United States Fire Administration. Publication No. FA-267.
Womack JW, Humbarger CD, Green JS, Crouse SF [2005]. Coronary artery disease risk factors in firefighters: effectiveness of a one-year voluntary health and wellness program. Med Sci Sports Exerc 37(5):S385.
Wynne J, Braunwald E [2008]. Cardiomyopathy and myocarditis. In: Fauci AS, Braunwald E, Kasper DL, Hauser SL, Longo DL, Jameson JL, Loscalzo J, eds. Harrison’s principles of internal medicine. 17th ed. New York: McGraw-Hill, pp. 1481–1488.
INVESTIGATOR INFORMATION
This incident was jointly investigated by the NIOSH Fire Fighter Fatality Investigation and Prevention Program, Cardiovascular Disease Component in Cincinnati, Ohio and the Traumatic Injury Component in Morgantown, West Virginia. Mr. Tommy Baldwin (MS) led the investigation and co-authored the report. Mr. Baldwin is a Safety and Occupational Health Specialist, a National Association of Fire Investigators (NAFI) Certified Fire and Explosion Investigator, an International Fire Service Accreditation Congress (IFSAC) Certified Fire Officer I, and a former Fire Chief and Emergency Medical Technician. Mr. Stephen Miles is a Safety and Occupational Health Specialist and a retired Battalion Chief of Safety with the Virginia Beach Fire Department. Dr. Thomas Hales (MD, MPH) provided medical consultation and co-authored the report. Dr. Hales is a member of the NFPA Technical Committee on Occupational Safety and Heath, and Vice-Chair of the Public Safety Medicine Section of the American College of Occupational and Environmental Medicine (ACOEM).
Practical Maze Drill
The maze trailer is specifically designed to simulate emergency scene situations. It is a metal sea shipping container with a maze built within (see Photographs 1–3 and Sketch 1 ). Students are instructed on the proper techniques to overcome obstacles and enter the maze using full PPE and SCBA while breathing tank air. Personnel must complete one trip through the maze without depleting a full 2216-pounds-per-square-inch or comparable SCBA. If students are unsuccessful on their first attempt, they receive immediate remedial training and are given a second chance to complete the evolution. Students are allowed two evolution attempts. Unsuccessful students are removed from the training program.

Photo1. Maze practical drill trailer built inside a metal sea shipping container

Photo 2. Inside the practical drill maze; incline slope

Photo 3. Inside the practical drill maze; decline slope
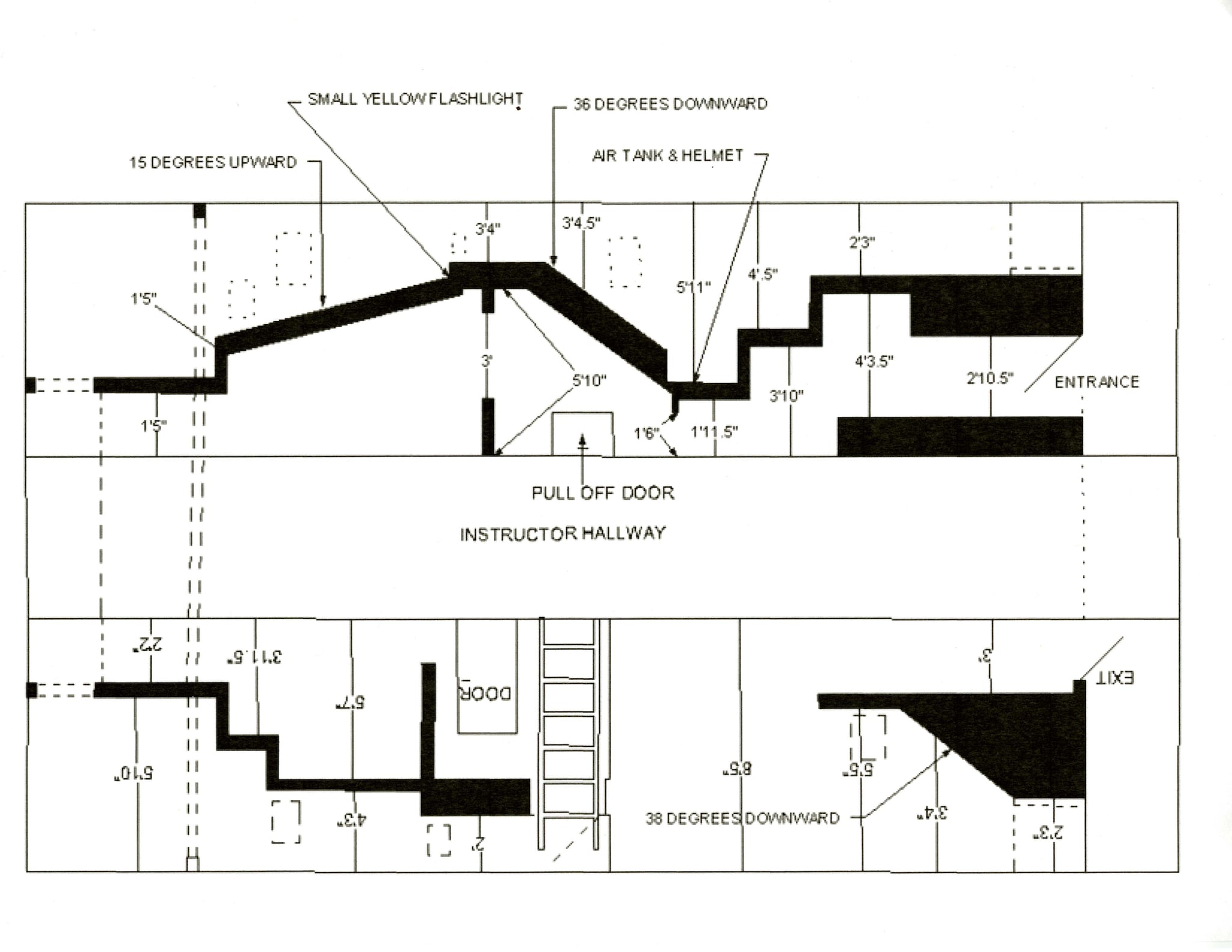
Sketch 1. Sketch of maze practical drill trailer with Trainee’s location identified
Autopsy Findings
- Arrhythmogenic right ventricular cardiomyopathy/dysplasia
- Fibrosis of the right greater than the left ventricle with multifocal replacement of the right wall with fibrofatty tissue.
- Cardiomegaly (enlarged heart)(heart weighed 440 grams [g]; predicted normal weight is 339 g [ranges between 232 g and 497 g as a function of sex, age, and body weight]) [Silver and Silver 2001]
- Left ventricular hypertrophy (1.2 centimeters [cm])
- Normal at autopsy is 0.76–0.88 cm [Colucci and Braunwald 1997]
- Normal by echocardiographic measurement is 0.6–1.1 cm [Armstrong and Feigenbaum 2001]
- Left wall has perivascular and interstitial fibrosis
- Normal cardiac valves
- No focal narrowing of the coronary arteries
- No evidence of a coronary artery thrombus (blood clot)
- No evidence of a pulmonary embolus (blood clot in the lung arteries)
- Blood tests for volatiles (ethanol, acetaldehyde, 1-propanol, 2-propanol, acetone) and cyanide were negative
- Blood test for carbon monoxide revealed a carboxyhemoglobin level of <10% (reported as normal from this laboratory)
REFERENCES
Armstrong WF, Feigenbaum H [2001]. Echocardiography. In: Braunwald E, Zipes DP, Libby P, eds. Heart disease: a text of cardiovascular medicine. 6th ed. Vol. 1. Philadelphia, PA: W.B. Saunders Company, p. 167.
Colucci WS, Braunwald E [1997]. Pathophysiology of heart failure. In: Braunwald, ed. Heart disease. 5th ed. Philadelphia, PA: W.B. Saunders Company, p. 401.
Silver MM and Silver MD [2001]. Examination of the heart and of cardiovascular specimens in surgical pathology. In: Silver MD, Gotleib AI, Schoen FJ, eds. Cardiovascular pathology. 3rd ed. Philadelphia, PA: Churchill Livingstone, pp. 8–9.
|
The National Institute for Occupational Safety and Health (NIOSH), an institute within the Centers for Disease Control and Prevention (CDC), is the federal agency responsible for conducting research and making recommendations for the prevention of work-related injury and illness. In fiscal year 1998, the Congress appropriated funds to NIOSH to conduct a fire fighter initiative. NIOSH initiated the Fire Fighter Fatality Investigation and Prevention Program to examine deaths of fire fighters in the line of duty so that fire departments, fire fighters, fire service organizations, safety experts and researchers could learn from these incidents. The primary goal of these investigations is for NIOSH to make recommendations to prevent similar occurrences. These NIOSH investigations are intended to reduce or prevent future fire fighter deaths and are completely separate from the rulemaking, enforcement and inspection activities of any other federal or state agency. Under its program, NIOSH investigators interview persons with knowledge of the incident and review available records to develop a description of the conditions and circumstances leading to the deaths in order to provide a context for the agency’s recommendations. The NIOSH summary of these conditions and circumstances in its reports is not intended as a legal statement of facts. This summary, as well as the conclusions and recommendations made by NIOSH, should not be used for the purpose of litigation or the adjudication of any claim. For further information, visit the program website at www.cdc.gov/niosh/fire or call toll free 1-800-CDC-INFO (1-800-232-4636).
|
This page was last updated on 09/18/09.
