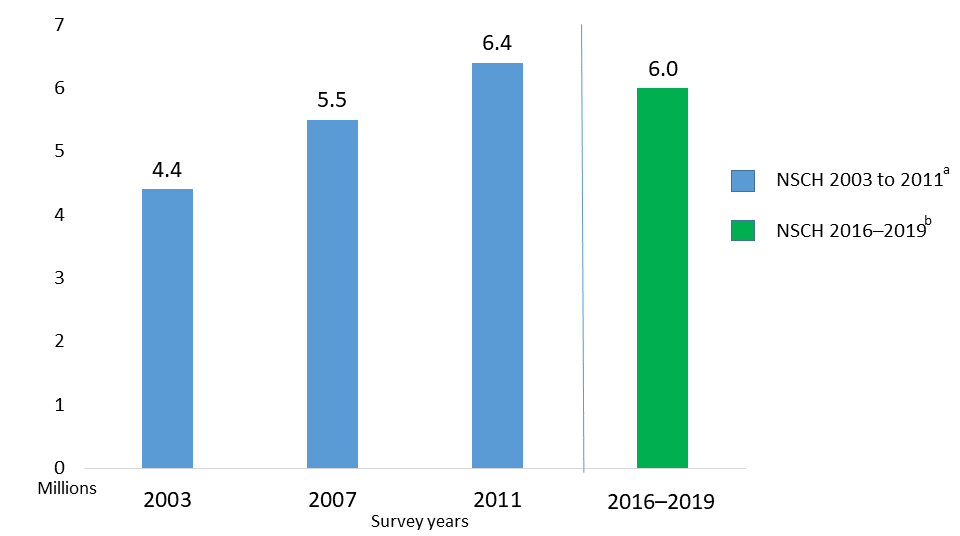Data and Statistics About ADHD
CDC uses datasets from parent surveys and healthcare claims to understand diagnosis and treatment patterns for attention-deficit/hyperactivity disorder (ADHD). Estimates for diagnosis and treatment can vary depending on the source. This page includes ADHD data from different sources.
Facts about ADHD
Millions of US children have been diagnosed with ADHD
- The estimated number of children aged 3–17 years ever diagnosed with ADHD, according to a national survey of parents,1 is 6 million (9.8%) using data from 2016-2019. This number includes
- 3–5 years: 265,000 (2%)
- 6–11 years 2.4 million (10%)
- 12–17 years: 3.3 million (13%).
- Boys (13%) are more likely to be diagnosed with ADHD than girls (6%).1
- Black, non-Hispanic children and White, non-Hispanic children are more often diagnosed with ADHD (12% and 10%, respectively), than Hispanic children (8%) or Asian, non-Hispanic children (3%).1
- Estimates for ADHD vary by state:2
- ADHD diagnosis among children aged 3–17 years: State estimates vary from 6% to 16%.
- Any ADHD treatment among children with current ADHD: State estimates vary from 58% to 92%
- ADHD medication: State estimates vary from 38% to 81%
- ADHD behavior treatment: State estimates vary from 39% to 62%
- Learn about ADHD diagnosis and treatment estimates by state.
The number of US children ever diagnosed with ADHD has changed over time
Estimated number of U.S. children ages 3–17 years who ever had a diagnosis of ADHD,1 in millions
About this chart:
a NSCH 2003 to 2011: National Survey of Children’s Health (NSCH), telephone survey data, information collected every 4 years.
b NSCH 2016 to 2019: Redesigned as an online and mail survey, information collected annually.
Beginning in 2016, the National Survey of Children’s Health used different methods than in previous survey years. Therefore, estimates from 2016 to 2019 are not directly comparable with estimates based on previous National Survey of Children’s Health data. For the information presented on this page, data from survey years 2016 to 2019 were combined to allow for more precise estimates.
For more information, see ADHD diagnosis throughout the years
For more information:
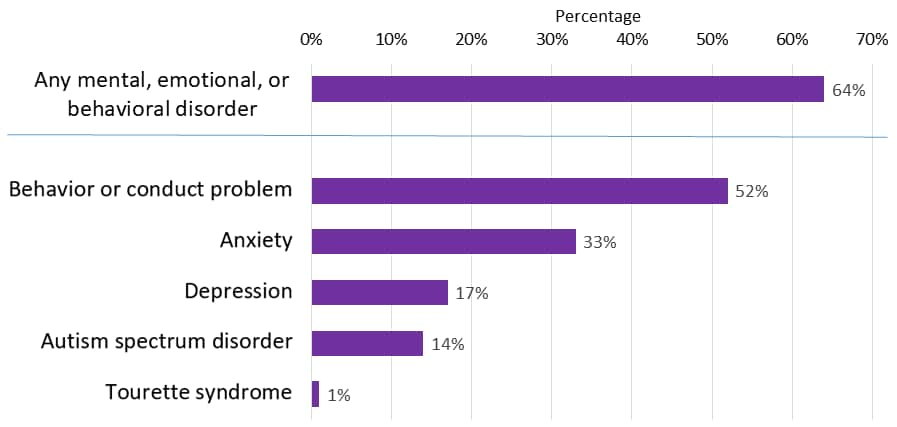
Many children with ADHD also have other disorders
According to a national 2016 parent survey,3 6 in 10 children with ADHD had at least one other mental, emotional, or behavioral disorder:
- About half of the children with ADHD had a behavior or conduct problem.
- About 3 in 10 children with ADHD had anxiety.
Other conditions affecting children with ADHD: depression, autism spectrum disorder, and Tourette syndrome.
Treatment for ADHD
Treatment for ADHD can include behavior therapy and medication. For children 6 years of age and older, the American Academy of Pediatrics (AAP) recommends behavior therapy and medication, preferably both together. For children under 6 years of age behavior therapy is recommended as the first line of treatment.
About 3 in 4 US children with current ADHD receive treatment
A national parent survey from 20163 reported on medication and behavior treatment for children 2–17 years of age with current ADHD:
- 62% were taking ADHD medication
- Ages 2–5: 18%
- Ages 6–11: 69%
- Ages 12–17: 62%
- 47% received behavior treatment
- Ages 2–5: 60%
- Ages 6–11: 51%
- Ages 12–17: 42%
- Altogether, 77% were receiving treatment. Of these children:
- About 30% were treated with medication alone.
- About 15% received behavior treatment alone.
- About 32% children with ADHD received both medication treatment and behavior treatment.
- About 23% children with ADHD were receiving neither medication treatment nor behavior treatment.
Note: Parents were not asked to specify what type of behavior treatment or medication their children received.
Read more about these findings
Most children with ADHD receive some types of services
A more in-depth national survey4 from 2014 reported on treatment and services that children with ADHD had received at some point prior to the survey. This survey was conducted with parents of children 4–17 years of age who had ever been diagnosed with ADHD.
- Almost 9 out of 10 children had received school support, which includes school accommodations and help in the classroom.
- About 6 out of 10 children had received some type of behavioral treatment or skills training:
- 3 out of 10 received parent-delivered behavior therapy.
- 4 out of 10 received social skills training.
- 3 out of 10 received peer interventions.
- 2 out of 10 received cognitive behavior therapy.
Read more about these findings
Read more about different types of therapy
Recommendations for treatment of ADHD
Healthcare claims data show treatment gaps
In addition to parent-reported data, healthcare claims from Medicaid or employer-sponsored insurance provide another way to understand treatment patterns. A study5 looking at the healthcare claims data for young US children found:
- During 2008–2011, children ages 2–5 years covered by Medicaid were twice as likely to receive clinical care for ADHD compared with similar-aged children covered by commercial employer-sponsored insurance.
- About 3 in 4 children ages 2–5 years who had clinical care for ADHD recorded in their healthcare claims from 2008–2014 received ADHD medication, and fewer than half received any form of psychological services.
Note: It is not known what types of psychological services these children received, or whether these children received behavior treatments that were not entered into the healthcare claims data.
References
- Bitsko RH, Claussen AH, Lichstein J, et al. Mental health surveillance among children—United States, 2013–2019. MMWR Suppl. 2022;71(2):1-48.
- Danielson ML, Holbrook JR, Newsome K., Charania SN, McCord RF, Kogan MD, Blumberg SJ. State-level estimates of the prevalence of parent-reported ADHD diagnosis and treatment among U.S. children and adolescents, 2016–2019. Journal of Attention Disorders, published online May 22, 2022.
- Danielson ML, Bitsko RH, Ghandour RM, Holbrook JR, Kogan MD, Blumberg SJ. Prevalence of Parent-Reported ADHD Diagnosis and Treatment Among U.S. Children and Adolescents, 2016. Journal of Child and Adolescent Psychology. 2018; 47(2), 199-212.
- Danielson ML, Visser SN, Chronis-Tuscano A, DuPaul GJ. A National Description of Treatment among United States Children and Adolescents with Attention-Deficit/Hyperactivity Disorder. The Journal of Pediatrics. 2018 Jan;192:240-246.e1.
- Visser, SN Danielson ML, Wolraich ML, Fox M, Grosse SD, Valle LA, Holbrook JR, Claussen AH, Peacock, P. Vital signs: National and state-specific patterns of attention deficit/hyperactivity disorder treatment among insured children aged 2–5 years — United States, 2008–2014. Morbidity and Mortality Weekly Report (MMWR); 2016,65, 443–450.