Mpox Vaccination Basics
Here’s what you need to know at this time:
- If you have certain risk factors that make you able to get the mpox vaccine and you’ve never had mpox—or you haven’t gotten the mpox vaccine—get both recommended doses of JYNNEOS vaccine at least 28 days apart.
- If you only received one dose, it’s never too late to get the second dose.
- If you have recovered from mpox, you do not need any mpox vaccine doses.
- Right now, getting more than 2 mpox vaccine doses (a “booster”) isn’t recommended.
- Whether or not you’ve been vaccinated, continue to reduce your risk of getting mpox.
Find mpox vaccines near you with our updated vaccine finder!
- Are a gay, bisexual, or other same-gender loving man who has sex with men or are transgender, gender non-binary, or gender-diverse AND in the last 6 months you have had, or expect to have
- One or more sexually transmitted infections
- More than one sexual partner, or anonymous sexual or intimate contact
- Sex at a commercial sex venue
- Sex in association with a large public event in a geographic area where mpox transmission is occurring
- Have had sexual or intimate contact with a person who is at risk of mpox as described above
- Have had sexual or intimate contact with someone who may have mpox. Get vaccinated as soon as possible after exposure, regardless of your sexual or gender identity.
Unless there is a medical reason you cannot get the vaccine, like a severe allergic reaction (such as anaphylaxis) after a previous dose or a severe allergic reaction to a vaccine component.
Mpox vaccines are effective at protecting you from mpox.
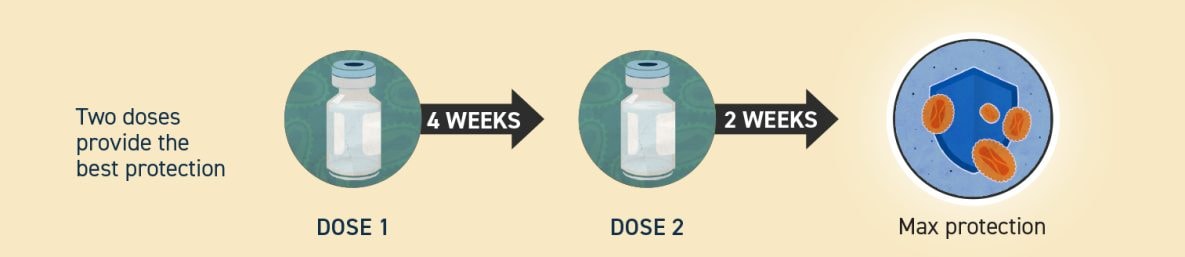
Two doses provide the best protection. Get dose 1, wait 4 weeks, and then get dose 2. If you can’t get your second dose on time, you should get it as soon as possible to complete the series. You will have maximum protection two weeks after your second dose.
Read more about the vaccine, how it’s given, side effects, and where to get it at Mpox Vaccine Recommendations.