FIGURE. Number and percentage of adults aged ≥18 years who had hypertension, who had controlled or uncontrolled hypertension, and who were aware and/or pharmacologically treated for hypertension among those with uncontrolled hypertension — National Health and Nutrition Examination Survey (NHANES), United States, 2003–2010*
Vital Signs: Awareness and Treatment of Uncontrolled Hypertension Among Adults — United States, 2003–2010
Abstract
Background: Hypertension is a leading risk factor for cardiovascular disease and a significant cause of morbidity and mortality. This report uses data from the National Health and Nutrition Examination Survey (NHANES) to examine awareness and pharmacologic treatment of uncontrolled hypertension among U.S. adults with hypertension and focuses on three groups: those who are unaware of their hypertension, those who are aware but not treated with medication, and those who are aware and pharmacologically treated with medication but still have uncontrolled hypertension.
Methods: CDC analyzed data from the NHANES 2003–2010 to estimate the prevalence of hypertension awareness and treatment among adults with uncontrolled hypertension. Hypertension was defined as an average systolic blood pressure (SBP) ≥140 mmHg or an average diastolic blood pressure (DBP) ≥90 mmHg, or currently using blood pressure (BP)–lowering medication. Uncontrolled hypertension was defined as an average SBP ≥140 mmHg or an average DBP ≥90 mmHg, among those with hypertension.
Results: The overall prevalence of hypertension among U.S. adults aged ≥18 years in 2003−2010 was 30.4% or an estimated 66.9 million. Among those with hypertension, an estimated 35.8 million (53.5%) did not have their hypertension controlled. Among these, an estimated 14.1 million (39.4%) were not aware of their hypertension, an estimated 5.7 million (15.8%) were aware of their hypertension but were not receiving pharmacologic treatment, and an estimated 16.0 million (44.8%) were aware of their hypertension and were being treated with medication. Of the 35.8 million U.S. adults with uncontrolled hypertension, 89.4% reported having a usual source of health care, and 85.2% reported having health insurance.
Implications for Public Health Practice: Nearly 90% of U.S. adults with uncontrolled hypertension have a usual source of health care and insurance, representing a missed opportunity for hypertension control. Improved hypertension control will require an expanded effort and an increased focus on BP from health-care systems, clinicians, and individuals.
Introduction
Hypertension is a leading risk factor for cardiovascular disease, a major cause of morbidity and mortality, and costs $131 billion annually in health-care expenditures (1–3). A previous report documented that during 2005–2008, nearly one third of U.S. adults had hypertension, and less than half had it under control (4). Uncontrolled hypertension among adults with hypertension is associated with increased mortality (5). Adequate hypertension treatment and control can reduce the incidence of first and recurrent heart attacks and strokes, heart failure, and chronic kidney disease, and can save lives (1,2,5,6). This report uses data from the National Health and Nutrition Examination Survey (NHANES) to examine awareness and treatment among U.S. adults with uncontrolled hypertension. This report focuses on three groups of adults with uncontrolled hypertension: those who are unaware of their hypertension, those who are aware but not treated with medication, and those who are aware and treated with medication but still have uncontrolled hypertension. The findings in this report can be used to target populations to improve hypertension control in the United States.
Methods
NHANES is a complex, multistage probability sample of the U.S civilian, noninstitutionalized population (7). The survey includes a household interview and a detailed physical examination. To obtain statistically stable estimates, data were analyzed from the most recent four 2-year survey cycles (2003–2010) in which a total of 22,992 participants aged ≥18 years were interviewed and examined.* Excluded from this analysis were pregnant women (n = 732), those missing blood pressure (BP) measurements or missing information on self-reported current use of hypertension medication (n = 1,318), and participants missing data on covariates of interest (n = 183). Some participants were excluded based on more than one criterion, yielding an eligible sample of 20,811. Hypertension was defined as an average systolic BP (SBP) ≥140 mmHg or an average diastolic BP (DBP) ≥90 mmHg, based on the average of up to three BP measurements† (7), or currently using BP-lowering medication. Uncontrolled hypertension was defined as an average SBP ≥140 mmHg or an average DBP ≥90 mmHg, among those with hypertension. Participants with uncontrolled hypertension were considered aware of their condition if they responded "yes" to the question "Have you ever been told by a doctor or other health professional that you had hypertension, also called high blood pressure?" Participants were classified as being treated for their hypertension if they answered "yes" to both of the following questions: "Because of your high blood pressure/hypertension, have you ever been told to take prescribed medicine?" and "Are you currently taking medication to lower your blood pressure?" Health insurance coverage referred to coverage at the time of interview; public insurance includes Medicaid, Children's Health Insurance Program (CHIP), state-sponsored or other government-sponsored health plan, Medicare, or military health plan (e.g., TRICARE, VA, or CHAMP-VA). The prevalence of uncontrolled hypertension was examined among those with hypertension, as well as the prevalence of awareness and treatment among those with uncontrolled hypertension. In addition, the prevalence of stage 2 hypertension (SBP ≥160 mmHg or DBP ≥100 mmHg) was estimated among those with uncontrolled hypertension (1).
All analyses were conducted using statistical software to account for sampling weights and to adjust variance estimates for the multistage, clustered sample design. Because trends over time were not examined and multiple cycles of the survey were collapsed, prevalence estimates were not age adjusted. Population counts were calculated using the Current Population Surveys provided by NHANES, by averaging the population for the four cycles examined.§
Results
The overall prevalence of hypertension among U.S. adults aged ≥18 years during 2003−2010 was 30.4%, representing an estimated 66.9 million persons, of whom an estimated 35.8 million (53.5%) had uncontrolled hypertension (Figure). The prevalence of uncontrolled hypertension among adults with hypertension was highest among those who reported receiving no medical care in the previous year (93.3%), those without a usual source of health care (87.4%), and those without health insurance (71.8%) (Table 1). Among the 35.8 million persons with uncontrolled hypertension, 32.0 million (89.4%) reported having a usual source of health care, 31.4 million (87.7%) received medical care in the previous year, and 30.5 million (85.2%) had health insurance. More than half (51.8%), an estimated 14.1 million, of Medicare beneficiaries with hypertension had uncontrolled hypertension. Approximately 9.1 million adults had stage 2 hypertension, representing 13.6% of all adults with hypertension and 25.4% of those with uncontrolled hypertension.
Among adults with uncontrolled hypertension, an estimated 14.1 million (39.4%) were unaware of their hypertension (Table 2); the prevalence of being unaware was highest among those who reported not receiving health care in the previous year (71.5%), those without a usual source of health care (64.3%), adults aged 18–44 years (56.6%), and those without health insurance (51.9%). An estimated 5.7 million adults (15.8%) were aware but not pharmacologically treated for hypertension; the prevalence of being aware yet untreated for hypertension was highest among those without a usual source of health care (25.6%), adults aged 18–44 years (25.4%), those of Hispanic ethnicity other than Mexican-Americans (24.8%), and those without health insurance (23.5%). An estimated 16.0 million (44.8%) were aware of their hypertension and pharmacologically treated; the prevalence of being aware and treated with medication was highest among Medicare beneficiaries (60.6%), those aged ≥65 years (59.9%), and those who reported receiving medical care two or more times in the previous year (55.3%).
Conclusion and Comment
The results of this analysis indicate that more than half (53.5%) of the estimated 66.9 million U.S. adults with hypertension had uncontrolled hypertension during the period 2003–2010. Nearly 90% of the 35.8 million U.S. adults with uncontrolled hypertension had a usual source of health care, had health insurance coverage, and received health care in the previous year, all of which indicate potential missed opportunities by individuals, health-care providers, and health-care systems to improve hypertension control. Improved hypertension control will require an expanded effort and increased focus on hypertension from patients, health-care systems, and clinicians.
Hypertension control can be challenging to achieve, with barriers to hypertension control attributed to patients, health-care providers, and health-care systems, and the silent nature of the disease (8). Moreover, even modest elevations in BP increase the risk for cardiovascular disease and mortality. For every 20-mmHg increase in SBP beginning at 115 mmHg, or 10-mmHg increase in DBP beginning at 75 mmHg, mortality from ischemic heart disease and stroke are doubled (1). Furthermore, nearly 30% of adults with uncontrolled hypertension who are aware of their hypertension and pharmacologically treated have stage 2 hypertension (SBP ≥160 mmHg or DBP ≥100 mmHg); these patients have significantly elevated BP and are at high risk for adverse cardiovascular events (1). Increased focus on BP from clinicians and health-care systems is essential for improving hypertension control, with all health-care providers participating, not just primary-care providers. Clinical strategies to improve hypertension control include using evidence-based practice guidelines, innovative health-care delivery models, such as team-based care, patient-centered medical homes, and interventions to promote medication adherence (Box). Team-based care, recommended by the Community Preventive Services Task Force, promotes improved communication with patients and other health-care providers and adherence to evidence-based guidelines, such as BP guidelines from the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (1,9,10). In addition, individuals also can play an important role in achieving greater hypertension control by improving medication adherence, measuring their own BP, and eating a lower-sodium diet.
BP screening, measurement, and control are key performance measures for several quality-improvement and reporting initiatives from the Centers for Medicare & Medicaid Services and other health-improvement initiatives and are based on National Quality Forum and Healthcare Effectiveness Data and Information Set hypertension-control measures. A number of programs contain quality reporting measures addressing hypertension control.¶ BP measures are key components of most electronic health records (EHRs). Health information technology, including EHRs, registries, and clinical decision support, helps clinicians improve care and target interventions to patients needing intensified care (9). A recent study indicated that hypertension was underdiagnosed in EHRs in outpatient clinics in the San Francisco Bay area, which serves approximately 600,000 patients (11). For patients with two or more BP readings of ≥140/90 or an antihypertensive medication prescription, only 63% had an appropriate hypertension diagnosis noted in the EHR. A study from the Geisinger Health System had a similar finding in which 30% of patients in their outpatient clinics had blood pressure measurements recorded in the EHR that met the definition for hypertension, yet were not documented as having hypertension and were not prescribed BP-lowering medications (Nirav Shah, New York State Department of Health, personal communication, 2012).
Health-care systems can adopt system-wide approaches facilitating increased hypertension identification and drug and lifestyle treatment strategies when indicated. Hypertension control rates improved from 45.7% in 2000 to 76.3% in 2010 in 15 Veterans Affairs medical centers with the implementation of system-wide strategies, including a BP-control performance measure, automatic notification of health-care providers regarding a patient's previously elevated BP readings, electronic reminders of treatment guidelines, and systematic scheduling of follow-up visits (12). In South Carolina, the Outpatient Quality Improvement Network improved hypertension control from 49% in 2000 to 66% in 2005 among a cohort of 208,547 patients with hypertension after implementation of a hypertension initiative, including education of health-care providers regarding hypertension and the use of evidence-based guidelines, participation in a central database, and receipt of quarterly feedback reports (13).
Million Hearts, a U.S. Department of Health and Human Services initiative co-led by CDC and the Centers for Medicare & Medicaid Services, is focusing efforts on a common goal of preventing 1 million heart attacks and strokes by 2017 (9).** Focused clinical and policy strategies and more effective application of health information technology are being used to improve the clinical management of hypertension, along with interventions such as aspirin therapy, cholesterol management, and smoking cessation (9). With respect to hypertension, this initiative has the goal of increasing by 10 million the number of persons in the United States whose hypertension is under control, which will help reach the objective of preventing 1 million heart attacks and strokes by 2017.
The findings in this report are subject to at least three limitations. First, NHANES surveys only the noninstitutionalized U.S. population. Military personnel and persons residing in nursing homes and other institutions are not included, which might result in underestimation of hypertension prevalence, given that older nursing home residents might have a higher prevalence of age-related hypertension. Moreover, the exclusion of military personnel might result in overestimation of the prevalence of hypertension because they might be younger, more physically fit, and have a lower prevalence of hypertension. Second, self-reported data on hypertension awareness and medication use might be subject to recall bias. Finally, this report examined hypertension treatment based only on medication use, not accounting for those using lifestyle or dietary approaches to reducing BP.
Uncontrolled hypertension affects nearly 36 million adults in the United States, yet 32 million of these adults have a usual source of health care, and 30 million have health insurance, representing a missed opportunity for hypertension control. The findings in this report can be used to target populations and refine interventions to improve hypertension control. Improved hypertension control will require an expanded effort from patients, health-care providers, and health-care systems.
Reported by
Amy L. Valderrama, PhD, Cathleen Gillespie, MS, Sallyann Coleman King, MD, Mary G. George, MD, Yuling Hong, MD, PhD, Div for Heart Disease and Stroke Prevention; Edward Gregg, PhD, Div of Diabetes Translation, National Center for Chronic Disease Prevention and Health Promotion, CDC. Corresponding contributor: Amy L. Valderrama, avalderrama@cdc.gov, 770-488-8218.
Acknowledgment
Robert Merritt, MA, Div for Heart Disease and Stroke Prevention, National Center for Chronic Disease Prevention and Health Promotion, CDC.
References
- Chobanian AV, Bakris GL, Black HR, et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003;42:1206–52.
- Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease and stroke statistics—2012 update: a report from the American Heart Association. Circulation 2012;125:e2–e220.
- Heidenreich PA, Trogdon JG, Khavjou OA, et al. Forecasting the future of cardiovascular disease in the United States: a policy statement from the American Heart Association. Circulation 2011;123:933–44.
- CDC. Vital signs: prevalence, treatment, and control of hypertension—United States, 1999–2002 and 2005–2008. MMWR 2011;60:103–8.
- Gu Q, Dillon CF, Burt VL, Gillum RF. Association of hypertension treatment and control with all-cause and cardiovascular disease mortality among US adults with hypertension. Am J Hypertens 2010;23:38–45.
- Farley TA, Dalal MA, Mostashari F, Frieden TR. Deaths preventable in the U.S. by improvements in use of clinical preventive services. Am J Prev Med 2010;38:600–9.
- CDC. National Health and Nutrition Examination Survey: surveys and data collection systems (2010 data). Atlanta, GA: US Department of Health and Human Services, CDC, National Center for Health Statistics; 2012. Available at http://www.cdc.gov/nchs/nhanes.htm. Accessed July 26, 2012.
- Wofford MR, Minor DS. Hypertension: issues in control and resistance. Curr Hypertens Rep 2009;11:323–8.
- Frieden TR, Berwick DM. The "Million Hearts" initiative—preventing heart attacks and strokes. N Engl J Med 2011;365:e27.
- Community Preventive Services Task Force. Guide to community preventive services—cardiovascular disease prevention and control: team-based care to improve blood pressure control. Atlanta, GA: US Department of Health and Human Services, CDC; 2012. Available at http://www.thecommunityguide.org/cvd/teambasedcare.html. Accessed July 26, 2012.
- Banerjee D, Chung S, Wong EC, Wang EJ, Stafford RS, Palaniappan LP. Underdiagnosis of hypertension using electronic health records. Am J Hypertens 2012;25:97–102.
- Fletcher RD, Amdur RL, Kolodner R, et al. Blood pressure control among US veterans: a large multiyear analysis of blood pressure data from the Veterans Administration Health Data Repository. Circulation 2012;125:2462–8.
- Egan BM, Laken MA, Wagner CS, et al. Impacting population cardiovascular health through a community-based practice network: update on an ASH-supported collaborative. J Clin Hypertens (Greenwich) 2011;13:543–50.
* Mobile examination center response rates for NHANES ranged from 75% to 77% during the study period.
† This study used the average of up to three BP measurements, obtained under standardized conditions during a single physical examination at the mobile examination center. Approximately 95% of participants had two or three complete BP measurements during the study period. For participants with only one BP measurement, that single measurement was used.
§ Additional information is available at http://www.cdc.gov/nchs/nhanes/response_rates_cps.htm
¶ Information about the Physician Quality Reporting System, for example, is available at https://www.cms.gov/medicare/quality-initiatives-patient-assessment-instruments/pqrs/downloads//2012pqrs_medicareehr-incentpilot_final508_1-13-2012.pdf. Information about Meaningful Use Stage 1 and 2 Clinical Quality Measures is available at http://www.hrsa.gov/healthit/meaningfuluse/mu%20stage1%20cqm/mucqm_.html and http://www.gpo.gov/fdsys/pkg/FR-2012-03-07/pdf/2012-4443.pdf, respectively. Information about the Million Hearts initiative is available at http://millionhearts.hhs.gov/aboutmh/achieving-goals.html. Information about the Healthcare Effectiveness Data and Information Set is available at http://www.ncqa.org/LinkClick.aspx?fileticket=J8kEuhuPqxk%3d&tabid=836. Information about the National Committee for Quality Assurance's recognition program for patient-centered medical homes is available at http://www.ncqa.org/tabid/631/default.aspx. Information about Accountable Care Organizations is available at http://www.cms.gov/medicare/medicare-fee-for-service-payment/sharedsavingsprogram/downloads/aco_qualitymeasures.pdf. Finally, information about Healthy People 2020 is available at http://www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicid=21.
** Additional information is available at http://millionhearts.hhs.gov/index.html.
|
Key Points |
|
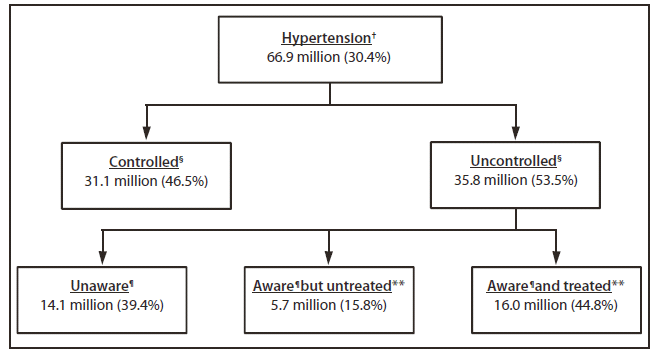
* Weighted population counts based on the Current Population Survey totals averaged across the four NHANES cycles (2003–2004, 2005–2006, 2007–2008, and 2009–2010).
† Hypertension is defined as an average systolic blood pressure ≥140 mmHg, an average diastolic blood pressure ≥90 mmHg, or reported current use of blood pressure–lowering medication.
§ Uncontrolled hypertension is defined as an average systolic blood pressure ≥140 mmHg or an average diastolic blood pressure ≥90 mmHg, among those with hypertension.
¶ Unaware defined as a "no" answer to the question, "Have you ever been told by a doctor or other health professional that you had hypertension, also called high blood pressure?" Aware defined as a "yes" answer to that question. Calculated among those with uncontrolled hypertension.
** Treated defined as an answer of "yes" to both of the following questions: "Because of your high blood pressure/hypertension, have you ever been told to take prescribed medicine?" and "Are you currently taking medication to lower your blood pressure?" Untreated defined as an answer of "no" to either of these questions. Calculated among those with uncontrolled hypertension.
Alternate Text: The figure above shows the number and percentage of adults aged ≥18 years who had hypertension, who had controlled or uncontrolled hypertension, and who were aware and/or pharmacologically treated for hypertension among those with uncontrolled hypertension, in the United States during 2003-2010. The overall prevalence of hypertension among U.S. adults aged ≥18 years during 2003−2010 was 30.4%, representing an estimated 66.9 million persons, of whom an estimated 35.8 million (53.5%) had uncontrolled hypertension.
|
BOX. Strategies to improve hypertension control in the clinical setting |
Sources: Glynn LG, Murphy AW, Smith SM, Schroeder K, Fahey T. Interventions used to improve control of blood pressure in patients with hypertension. Cochrane Database Syst Rev 2010;(3):CD005182. Institute of Medicine. A population-based policy and systems change approach to prevent and control hypertension. Washington, DC: The National Academies Press; 2010. Available at http://www.nap.edu/catalog.php?record_id=12819. |
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services. |
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


