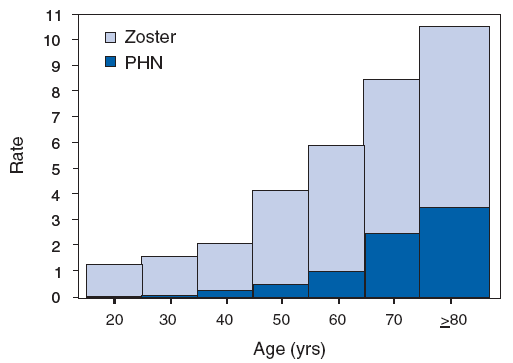Shingles Burden and Trends
About 1 in 3 people in the United States will develop shingles in their life. Your risk of having shingles increases as you get older or if you have a weakened immune system.
Most people who have shingles only have it one time. However, you can have shingles more than once.
The most common complication of shingles is severe pain in the area where the shingles rash occurred. This is known as postherpetic neuralgia, or PHN. Approximately 10% to 18% of people with herpes zoster will get PHN. The risk of PHN also increases with age.
Children can have shingles, but it is not common.
Hospitalizations and Deaths
Approximately 1% to 4% of people with shingles go to the hospital for complications. Older adults and people with weakened or suppressed immune systems are more likely to need to go to the hospital. About 30% of people in the hospital for shingles have a weakened or suppressed immune system.
Fewer than 100 people die from shingles each year. Almost all shingles deaths are in older adults or people with compromised immune systems.
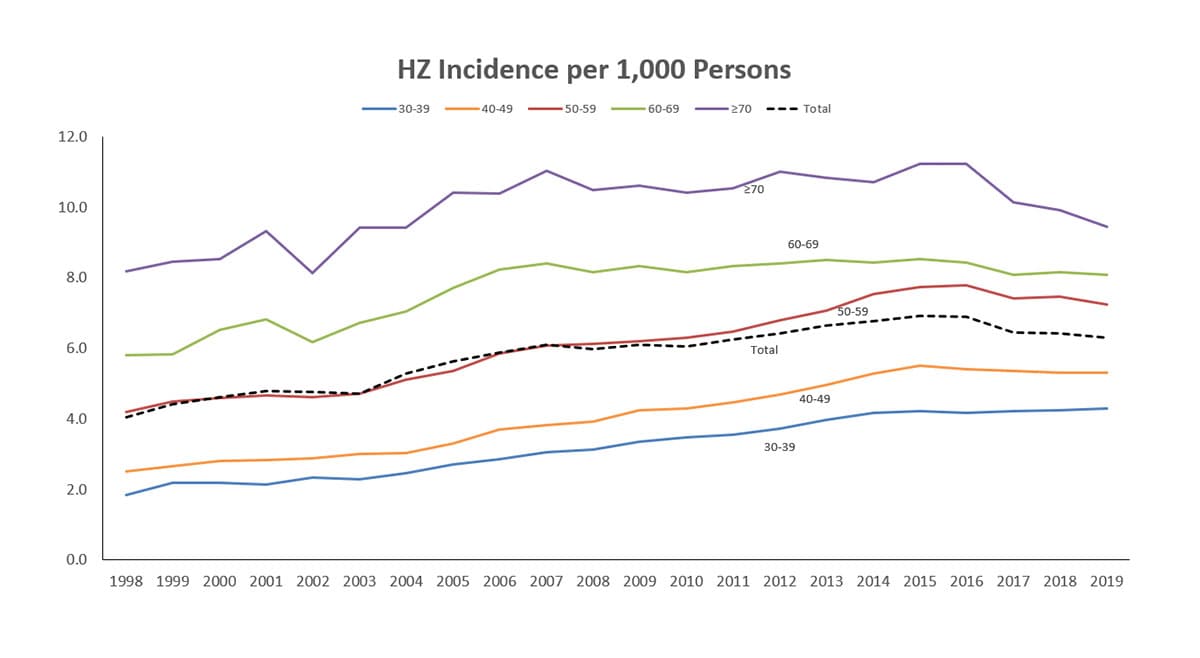
Trends
Herpes zoster rates among adults in the United States gradually increased over a long period of time. We do not know the reason for this increase. However, the rates across age groups have recently plateaued or declined.
*per 1,000 person-years.
† Defined as pain for 30 days or longer
Source: https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5705a1.htm