Key Facts about Human Infections with Variant Viruses
- What is swine flu?
- What is a variant flu virus?
- How do people get infected with variant flu and who is at increased risk of getting variant flu?
- Can variant flu viruses spread from person to person?
- Can people catch variant flu from eating properly handled and prepared pork?
- What signs and symptoms do people have when they are infected with variant flu viruses?
- How common is it for people to be infected with variant flu?
- Why did the number of reported variant flu infections increased after 2012?
- Who is at higher risk of serious variant flu illness?
- Why are human infections with variant viruses of concern?
- Does getting a seasonal flu vaccine protect people against variant flu?
- How can human infections with variant flu viruses be diagnosed?
- What medications are available to treat variant flu infections in people?
- How did the H3N2v virus emerge and when did the largest outbreaks of H3N2v occur?
Questions & Answers
This page contains information about variant virus infections, which are human infections with flu viruses that normally spread in swine (pigs).
What is swine flu?
Swine flu is a respiratory disease of pigs caused by type A flu viruses that regularly cause outbreaks of flu in pigs (not people). Swine flu viruses can cause high levels of illness in swine herds, but usually cause few deaths. Common signs of illness in pigs include fever, depression, coughing (barking), runny nose or eyes, sneezing, breathing problems, eye redness or inflammation, and not eating. However, infected pigs also may not show signs or only be mildly sick. Swine flu viruses may spread among pigs throughout the year, but most outbreaks happen during the late fall and winter months, similar to outbreaks of seasonal flu in people.
What is a variant flu virus?
When a flu virus that normally spreads in pigs but not people is found in a person, it is called a “variant flu virus.” For example, if a swine flu A(H3N2) virus is found in a person, that virus will be called an “H3N2 variant” virus (abbreviated as “H3N2v” virus). This naming convention was first announced in a January 6, 2012, Morbidity and Mortality Weekly Report (MMWR) titled Update: Influenza A (H3N2)v Transmission and Guidelines — Five States, 2011. (Reference)
How do people get infected with variant flu and who is at increased risk of getting variant flu?
Human infections with variant flu viruses most commonly happen in people with exposure to infected pigs (e.g., children near pigs at an agricultural fair, people who raise pigs, or workers in the swine industry). This is thought to happen mainly when an infected pig coughs or sneezes and droplets with flu virus in them spread through the air. If these droplets land in the nose or mouth, or are inhaled, a person can be infected. There also is some evidence that people can get infected by touching something that has virus on it and then touching their own mouth or nose. Scientists are not sure which of these ways of spreading is most common.
Can variant flu viruses spread from person to person?
Yes. There have been multiple documented cases of people becoming sick after exposure to one or more infected pigs and also cases of limited spread of variant flu viruses from person-to-person. The vast majority of human infections with variant flu viruses do not result in person-to-person spread. However, each case of human infection with a swine flu virus should be fully investigated to be sure that such viruses are not spreading in an efficient and ongoing way in people and to limit further exposure of people to infected animals if infected animals are identified.
Can people catch variant flu from eating properly handled and prepared pork?
No. Variant flu has not been shown to spread through eating properly handled and prepared pork (pig meat) or other pig products. For more information about the proper handling and preparation of pork, visit the USDA website fact sheet Fresh Pork from Farm to Table.
What signs and symptoms do people have when they are infected with variant flu viruses?
Illness from variant virus infections has been mostly mild with symptoms similar to human seasonal flu. These include fever, lethargy (tiredness), lack of appetite and coughing. Some people also have reported runny nose, sore throat, eye irritation, nausea, vomiting and diarrhea. Like seasonal flu, however, serious illness resulting in hospitalization and death is possible.
How common is it for people to be infected with variant flu?
Flu viruses from swine (pigs) do not normally infect people; however, sporadic variant flu infections occur among people each year. Most commonly, variant flu infections happen in people exposed to infected pigs. Past variant flu infections have occurred among children and adults exposed to infected pigs at agricultural fairs, among people who raise pigs, and among swine workers. There have been documented cases of multiple people becoming sick after exposure to one or more sick pigs. Also, instances of limited person-to-person spread of variant viruses have occurred.
Prior to 2012, CDC received reports of approximately one variant flu virus infection every one to two years, but beginning in 2012, there was a jump in the number of variant flu cases. Human infections with variant flu are reported in FluView, and case counts are available at Novel Influenza A Virus Infections (cdc.gov) in FluView Interactive.
Why did the number of reported variant flu infections increased after 2012?
The increased detection and reporting of these cases could have occurred for a number of reasons, including:
- pandemic preparedness efforts have improved state level surveillance and laboratory capacity to detect novel flu viruses in the United States;
- in 2005, novel flu virus infections were made internationally reportable; and in 2007, they were made domestically reportable; and,
- it’s also possible that there has been a true increase in the number of these cases, following exposure to infected swine.
Who is at higher risk of serious variant flu illness?
The groups of people at higher risk of developing serious variant flu complications are thought to be the same groups at higher risk for serious seasonal flu complications. These groups include: children younger than 5 years, people 65 years and older, pregnant people, and people with certain chronic health conditions (like asthma, diabetes, heart disease, weakened immune systems, and neurological or neurodevelopmental conditions).
A full list of people at higher risk of flu related complications is available at People at Higher Risk of Developing Flu-Related Complications.
CDC has issued guidance for people attending fairs where swine might be present, including additional precautions for people who are at higher risk for serious flu complications.
Why are human infections with variant viruses of concern?
Variant flu infections are caused by flu viruses that normally spread in pigs (not people), and which are different from human seasonal flu viruses. Human seasonal flu vaccines are generally not expected to protect people from variant flu. Just like human seasonal flu viruses, infections with variant flu viruses can sometimes cause severe disease, even in healthy people. This can include complications which require hospitalization and sometimes result in death.
In addition, because pigs can be infected with avian (bird), human, and swine flu viruses, they have the potential to be infected with flu viruses from different species (e.g., ducks and humans) at the same time. If this happens, it is possible for the genes of these viruses to mix through a process called reassortment. This can result in the creation of a new flu virus. This type of major change in flu A viruses is known as antigenic shift. If this new virus causes illness in people and can spread easily from person-to-person, a flu pandemic can occur. This is what happened in 2009 when a flu A H1N1 virus with genes from swine, avian and human flu viruses emerged in the spring of 2009 and caused a pandemic. It is important to note that while variant flu virus infection has resulted in mostly mild disease in people, human infection with some avian flu viruses has resulted in quite severe illness. If reassortment were to result in a new flu virus with the severity of some avian flu viruses and the ability to spread easily from person-to-person, the possibility of a flu pandemic increases.
Does getting a seasonal flu vaccine protect people against variant flu?
Seasonal flu vaccines are not formulated to protect against variant flu viruses. Seasonal flu vaccines protect against seasonal flu viruses. CDC recommends that everyone 6 months and older get a seasonal flu vaccine each year. CDC also recommends that people who have contact with pigs get the seasonal flu vaccine to help prevent spreading human flu viruses to pigs.
How can human infections with variant flu viruses be diagnosed?
There is a test to diagnose variant flu A virus infection. Since the 2009 H1N1 pandemic, state health departments have the ability to test for novel (non-human) flu viruses. However, if a variant flu virus is suspected, a respiratory specimen is also sent to CDC for further testing.
What medications are available to treat variant flu infections in people?
There are four different antiviral drugs that are recommended for use in the United States for the treatment of flu: oseltamivir, peramivir, zanamivir, and baloxavir.
For information about seasonal flu, visit the CDC Seasonal Influenza (Flu) website.
How did the H3N2v virus emerge and when did the largest outbreaks of H3N2v occur?
Flu A H3N2 variant viruses, also known as “H3N2v” viruses, with the matrix (M) gene from the 2009 H1N1 pandemic virus were first detected in people in July 2011. The viruses were first identified in U.S. pigs in 2010. In 2011, 12 cases of H3N2v infection were detected in the United States (Indiana, Iowa, Maine, Pennsylvania, and West Virginia). The largest outbreaks of H3N2v occurred in 2012, when 309 cases of H3N2v infection across 12 states were detected. That year 16 people were hospitalized, and one died. Most cases of H3N2v infection have occurred in children.
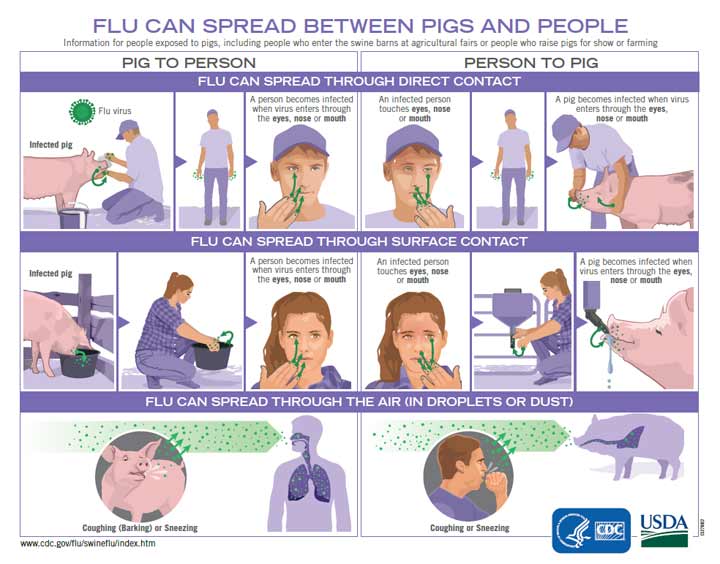
- Graphic: Flu Can Spread Between Pigs and People [1.2 MB, 2 pages] | Spanish [1.2 MB, 2 pages]
- Key Facts for People Exhibiting Pigs at Fairs [545 KB, 2 pages]
- Take Action to Prevent the Spread of Flu Between People and Pigs [1.3 MB, 2 pages]
- Educational Poster [389 KB, 1 page]
- Compendium of Measures to Prevent Disease Associated with Animals in Public Settings, 2017
- Reduce Your Risk (English) [22 KB, 1 page] | (Spanish) [22 KB, 1 page]
- Measures to Minimize Influenza Transmission at Swine Exhibitions, 2018 – NASAHO and NASPHV [97 KB, 8 pages]