Detailed FAQs
On This Page
- Introduction
- How do people get Chagas disease?
- If I have Chagas disease, should my family members be tested for the infection?
- In what parts of the world is Chagas disease found?
- What are the signs and symptoms of Chagas disease?
- What should I do if I think I have Chagas disease?
- How is Chagas disease treated?
- I plan to travel to a rural area of Latin America that might have Chagas disease. How can I prevent infection?
What is Chagas disease?
Chagas disease is caused by the parasite Trypanosoma cruzi, which is transmitted to animals and people by insect vectors and is found only in the Americas (mainly, in rural areas of Latin America where poverty is widespread). Chagas disease (T. cruzi infection) is also referred to as American trypanosomiasis.
It is estimated that as many as 8 million people in Mexico, Central America, and South America have Chagas disease, most of whom do not know they are infected. If untreated, infection is lifelong and can be life threatening.
The impact of Chagas disease is not limited to only rural areas of Latin America in which vectorborne transmission (diseases transmitted by insects) occurs. Large-scale population movements from rural to urban areas of Latin America and to other regions of the world have increased the geographic distribution and changed the epidemiology of Chagas disease. In the United States and in other regions where Chagas disease is now found but is not endemic, control strategies should focus on preventing transmission from blood transfusion, organ transplantation, and mother-to-baby (congenital transmission).
How do people get Chagas disease?
People can become infected in several ways. In areas where Chagas disease is common, the main way is through vectorborne transmission. The insect vectors are called triatomine bugs. These blood-sucking bugs get infected with T. cruzi by biting an infected animal or person. Once infected, the bugs pass the parasites in their feces. The bugs are found in houses made from materials such as mud, adobe, straw, and palm thatch. During the day, the bugs hide in crevices in the walls and roofs. During the night, when the inhabitants are sleeping, the bugs emerge. Because they tend to bite people’s faces, triatomine bugs are also known as “kissing bugs”. After they bite and ingest blood, they defecate (poop) on the person. The person can become infected if T. cruzi parasites in the bug feces enter the body through mucous membranes or breaks in the skin. The unsuspecting, sleeping person may accidentally scratch or rub the feces into the bite wound, eyes, or mouth.
People also can become infected through
- Congenital transmission (from a pregnant woman to her baby);
- Blood transfusions;
- Organ transplantation;
- Consumption of uncooked food that is contaminated with feces (poop) from infected triatomine bugs; and
- Accidental laboratory exposure.
It is generally considered safe to breastfeed even if the mother has Chagas disease. However, if the mother has cracked nipples or blood in the breast milk, she should pump and discard the milk until the nipples heal and the bleeding resolves.
Chagas disease is not transmitted from person-to-person like a cold or the flu or through casual contact with infected people or animals.
If I have Chagas disease, should my family members be tested for the infection?
Possibly. They should be tested if they:
- Could have become infected the same way that you did, for example, by vectorborne transmission;
- Are your children and were born after you were infected; or if
- There are other reasons to think that they might have Chagas disease.
In what parts of the world is Chagas disease found?
People who have Chagas disease can be found anywhere in the world. However, transmission of the disease by kissing bugs (vectorborne transmission), only occurs in the Americas. Most people with Chagas disease became infected in rural areas of Mexico, Central America, and South America. In some regions of Latin America, efforts to eliminate kissing bugs, called vector control programs, have succeeded in stopping this type of disease spread. Vectorborne transmission does not occur in the Caribbean (for example, in Puerto Rico or Cuba). Rare vectorborne cases of Chagas disease have been noted in the southern United States.
What are the signs and symptoms of Chagas disease?
Much of the clinical information about Chagas disease comes from experience with people who became infected as children through contact with triatomines. The severity and course of an individual infection can vary based on a number of factors, including the age at which a person became infected, the way in which a person acquired the infection, or the particular strain of the T. cruzi parasite.
There are two phases of Chagas disease: the acute phase and the chronic phase. Both phases can be symptom free or life threatening.
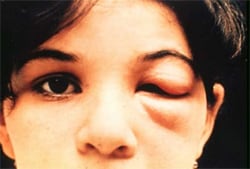
Romaña’s sign, the swelling of the child’s eyelid, is a marker of acute Chagas disease. Swelling is due to Trypanosoma cruzi infecting the eyelid when bug feces are accidentally rubbed into the eye, or because the bite wound was on the same side of the child’s face as the swelling. Credit: WHO/TDR
Acute phase: During this phase, which lasts for the first few weeks or months infection, a person may have no symptoms or mild ones, such as fever, fatigue, body aches, headache, rash, loss of appetite, diarrhea, and vomiting. Because these symptoms are similar to those of other illnesses, most people do not know their illness is from infection with the T. cruzi parasite.
However, a doctor may be able to pick up other signs of infection, including mild enlargement of the liver or spleen, swollen glands, or swelling at the site of the bite (called a chagoma), where the parasite entered the body. Some people with acute phase infection may have swelling of the eyelids on the side of the face near the bite wound or where the bug poop was accidentally rubbed into the eye, called Romaña’s sign. Even if a person develops symptoms during the acute phase, they usually feel well within a few weeks or months but if the person is not treated with antiparasitic medication, the infection remains in the body. Rarely, young children (less than 5%) die from severe inflammation and infection of the heart muscle (myocarditis) or brain (meningoencephalitis). The acute phase also can be severe in people with weakened immune systems, such as patients taking chemotherapy or those with advanced HIV infection.
Chronic phase: During this phase, which can last for decades or even for the entirety of someone’s lifetime, most people have no symptoms. Approximately 20–30 percent of infected people develop
- Cardiac complications, which can include an enlarged heart, heart failure, altered heart rate or rhythm, and cardiac arrest (sudden death); and/or
- Gastrointestinal complications, which can include an enlarged esophagus (megaesophagus) or colon (megacolon) and can lead to difficulties with eating or pooping.
What should I do if I think I have Chagas disease?
You should discuss your concerns with your healthcare provider, who will examine you and ask you questions (for example, about your health and where you have lived). Chagas disease is diagnosed by blood tests. If you have Chagas disease, you should have a heart tracing test (electrocardiogram), even if you feel fine. You might be referred to a specialist for more tests and treatment.
How is Chagas disease treated?
Two approaches to therapy, that can be life-saving include:
Antiparasitic treatment, to kill the parasite; and
Symptomatic treatment, to manage the symptoms and signs of infection.
Antiparasitic treatment is most effective early in the course of infection but is not limited to cases in the acute phase. In the United States, there are two types of treatments available. Benznidazole is approved by FDA for use in children 2–12 years of age and is commercially available at http://www.benznidazoletablets.comexternal icon. Lampit®external icon (nifurtimox) is FDA approved for treatment of children from birth to age younger than 18 years and is commercially available for pharmacies to purchase from several drug wholesalers. Your health-care provider can talk with CDC staff about whether and how you should be treated. Most people do not need to be hospitalized during treatment.
I plan to travel to a rural area of Latin America that might have Chagas disease. How can I protect myself from this infection?
No drugs or vaccines for preventing infection are currently available. Travelers who sleep indoors, in well-constructed facilities (for example, air-conditioned or screened hotel rooms), are at low risk for exposure to infected triatomine bugs that usually live in poor-quality dwellings and are most active at night. Preventive measures include spraying infested dwellings with long-lasting insecticides, using bed nets treated with long-lasting insecticides, wearing protective clothing, and applying insect repellent to exposed skin. Travelers should observe food and beverage precautions and avoid consuming salads, uncooked vegetables, unpeeled fruits, and unpasteurized fruit juices.
This information is not meant to be used for self-diagnosis or as a substitute for consultation with a healthcare provider. If you have any questions about the parasites described above or think that you may have a parasitic infection, consult a healthcare provider.
