COVID-19 Science Update released: October 1, 2021 Edition 107

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
Efficacy of the mRNA-1273 SARS-CoV-2 vaccine at completion of blinded phaseexternal icon. El Sahly et al. NEJM (September 22, 2021).
Key findings:
- Vaccine efficacy (VE) for preventing:
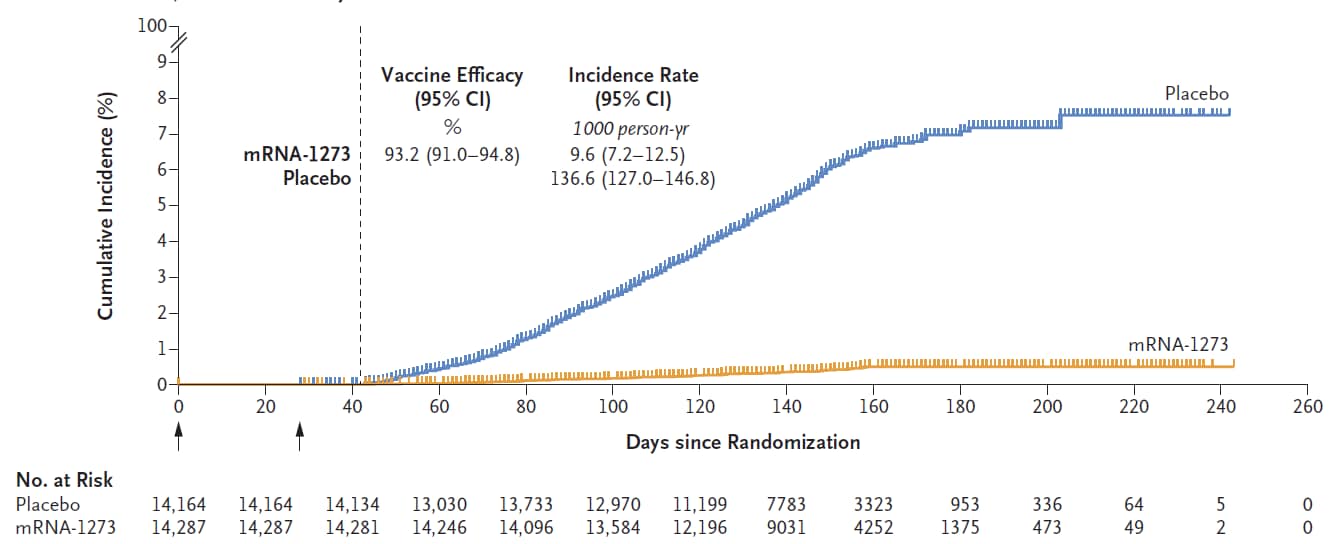
- COVID-19 was 93.2% (95% CI 91.0-94.8) (Figure).
- Severe disease was 98.2% (95% CI 92.8-99.6).
- VE for preventing COVID-19 ≥4 months after the 2nd injection was 92.4% (95% CI 84.3-96.8).
Methods: Clinical trial conducted among adults randomized to receive 2 doses of the mRNA-1273 (Moderna) vaccine (N = 15,209) or placebo (N = 15,206). Outcomes of COVID-19, severe COVID-19 illness, and SARS-CoV-2 infection were assessed ≥14 days after the 2nd dose, as of March 26, 2021; median follow-up time was 5.3 months. Limitations: Key populations (e.g., pregnant women, children, immunocompromised patients) not included; low circulation of Delta variant during trial.
Implications: A 2-dose regimen of mRNA-1273 conferred substantial protection against symptomatic SARS-CoV-2 infection and severe COVID-19 illness in adults for at least 4 months.
Figure:
Note: Adapted from El Sahly et al. Cumulative COVID-19 incidence among participants who received placebo or mRNA-1273. The dashed vertical line depicts the beginning of the adjudicated assessment of outcomes. From the New England Journal of Medicine, El Sahly et al., Efficacy of the mRNA-1273 SARS-CoV-2 vaccine at completion of blinded phase. September 22, 2021, online ahead of print. Copyright © 2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Effectiveness of mRNA COVID-19 vaccine among U.S. health care personnelexternal icon. Pilishvili et al. NEJM (September 22, 2021).
Key findings:
- Among fully vaccinated healthcare personnel, adjusted vaccine effectiveness (VE) was 90.4% (95% CI 69.6%-92.9%) and did not vary by which mRNA vaccine was received.
- Severe symptoms or hospitalization were more likely among unvaccinated case participants than among partially or fully vaccinated case participants.
- VE was comparable across race and ethnicity, comorbidities, and age.
Methods: Case-control study conducted among 1,482 cases (had SARS-CoV-2 infection) and 3,449 controls (did not have SARS-CoV-2 infection, matched on test date and site) selected from healthcare personnel in acute care hospitals and long-term care facilities in 25 U.S. states, December 2020–May 2021. VE for the BNT162b2 (Comirnaty, Pfizer/BioNTech) and mRNA-1273 (Moderna) vaccines was calculated as 1–(matched OR). Limitations: COVID-19 testing practices varied across sites; vaccinated personnel may have accessed testing differentially than unvaccinated, potentially underestimating VE; persons with unknown prior COVID-19 could not be excluded.
Implications: BNT162b2 and mRNA-1273 vaccines prevented symptomatic COVID-19 among frontline healthcare personnel, regardless of demographic characteristics or underlying risk.
PREPRINTS (NOT PEER-REVIEWED)
Real-world serologic responses to extended-interval and heterologous COVID-19 mRNA vaccination in frail elderly – interim report from a prospective observational cohort studyexternal icon. Vinh et al. medRxiv (September 21, 2021). Published in The Lancet Healthy Longevity as Real-world serological responses to extended-interval and heterologous COVID-19 mRNA vaccination in frail, older people (UNCoVER): an interim report from a prospective observational cohort studyexternal icon (February 21, 2022).
Key findings:
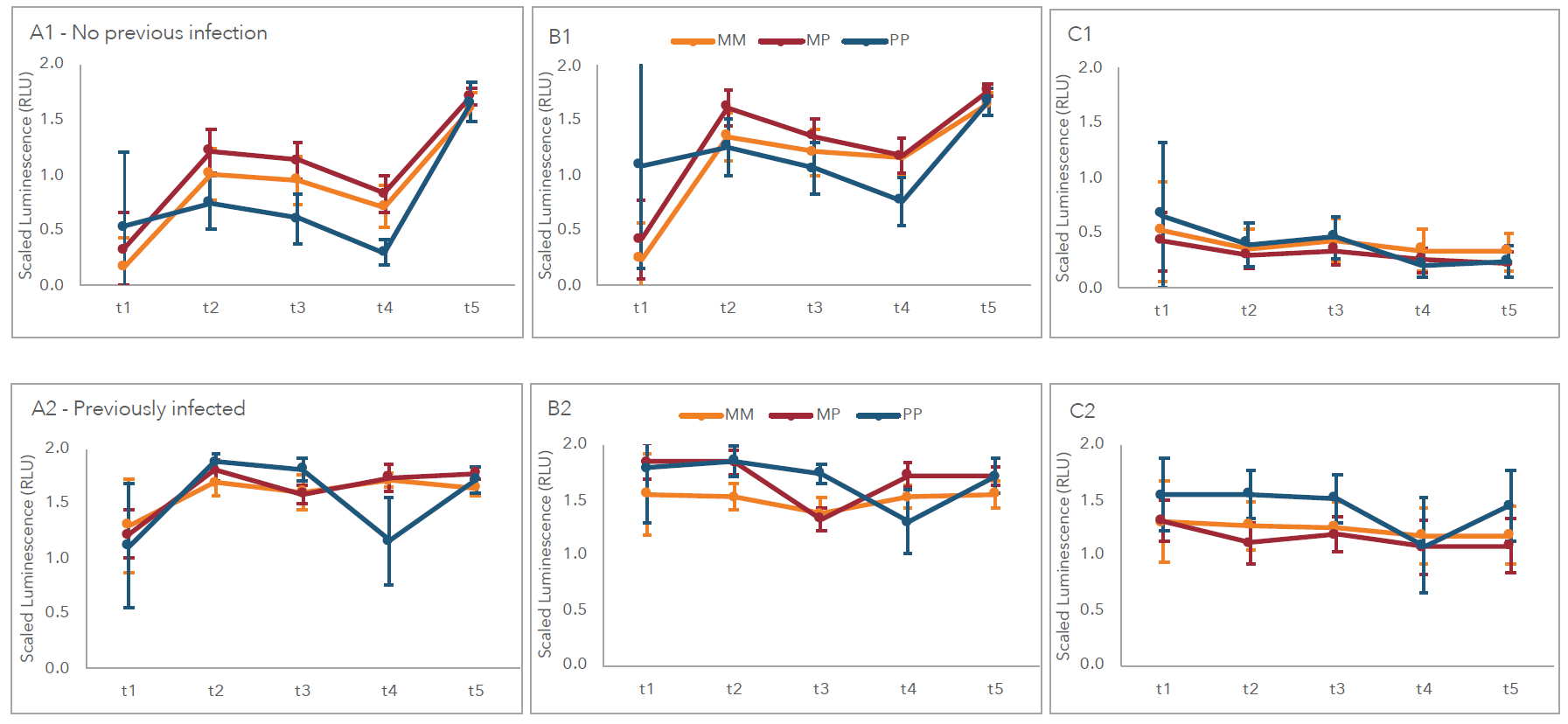
- Antibody levels at 4 weeks after 2nd dose did not differ between vaccine recipients of either heterologous or homologous vaccine regimens (Figure).
- Previously uninfected individuals exhibited lower antibody responses up to 16 weeks after the 1st dose
- Antibody levels by 4 weeks after 2nd dose were comparable to those of previously infected individuals and did not differ by age, sex, or presence of comorbidities.
Methods: Real-world study among elderly long-term care facility residents in Québec (n = 185) who received 2-dose mRNA vaccines with an extended (16 week) interval between doses. Participants received homologous vaccination (2 doses of either mRNA-1273 [Spikevax/Moderna] or BNT162b2 [Comirnaty, Pfizer/BioNTech]) or heterologous (1 mRNA-1273 dose then 1 BNT162b2 dose) based on availability. IgG responses were measured. Limitations: Clinical outcomes were not evaluated; cellular immune responses were not measured.
Implications: Based on antibody responses, heterologous vaccination might be as effective as homologous vaccination among elderly persons receiving mRNA vaccine.
Figure:
Note: Adapted from Vinh et al. Antibody responses to homologous (MM: Moderna/Moderna, PP: Pfizer/Pfizer) vs. heterologous (MP: Moderna/Pfizer) mRNA vaccines based on previous infection status. Top row (A1, B1, C1) no previous infection, bottom row (A2, B2, C2) previously infected. Antibody responses to receptor binding domain (A), S-protein (B), or N antigen (C). t1: baseline, t2: 4 weeks after 1st dose, t3: 6–10 weeks after 1st dose, t4: 16 weeks after 1st dose, t5: 4 weeks after 2nd dose. Licensed under CC-BY-NC-ND 4.0.
PREPRINTS (NOT PEER-REVIEWED)
COVID-19 in the Phase 3 trial of MRNA-1273 during the Delta-variant surgeexternal icon. Baden et al. medRxiv (September 22, 2021). Published in NEJM as Phase 3 trial of mRNA-1273 during the Delta-variant surgeexternal icon (December 23, 2021).
Key findings:
- During the Delta variant surge, rates of COVID-19 were reduced by 36.4% (95% CI 17.1-51.5) and severe illness by 46% (95% CI -52.4-83.2) among adults vaccinated with mRNA-1273 (Moderna) vaccine more recently, compared with those vaccinated earlier.
- Reductions in the rate of infection were more pronounced in persons aged <65 years, but reductions in the rate of severe illness were more pronounced among persons aged ≥65 years.
Methods: Using data from the randomized Coronavirus Efficacy (COVE) mRNA-1273 vaccine trial, rates of COVID-19 and severe COVID-19 illness were assessed during July 1–August 27, 2021 in an intention-to-treat analysis. Outcomes among adult participants vaccinated earlier (July–December 2020; N = 14,746) were compared to those vaccinated more recently (December 2020–April 2021; N = 11,431). Limitations: Short follow up time (2 months).
Implications: During the months when Delta was the dominant COVID-19 variant, rates of COVID-19 and severe illness were lower among persons who were more recently vaccinated. Reevaluation after longer follow-up is needed.
PEER-REVIEWED
Trajectory of COVID-19 vaccine hesitancy over time and association of initial vaccine hesitancy with subsequent vaccinationexternal icon. Siegler et al. JAMA Network Open (September 24, 2021).
Key findings:
- Among participants hesitant to vaccinate at baseline, 32% reported receiving 1 or more vaccine doses, 37% reported being likely to be vaccinated, and 32% remained unlikely to be vaccinated at follow-up.
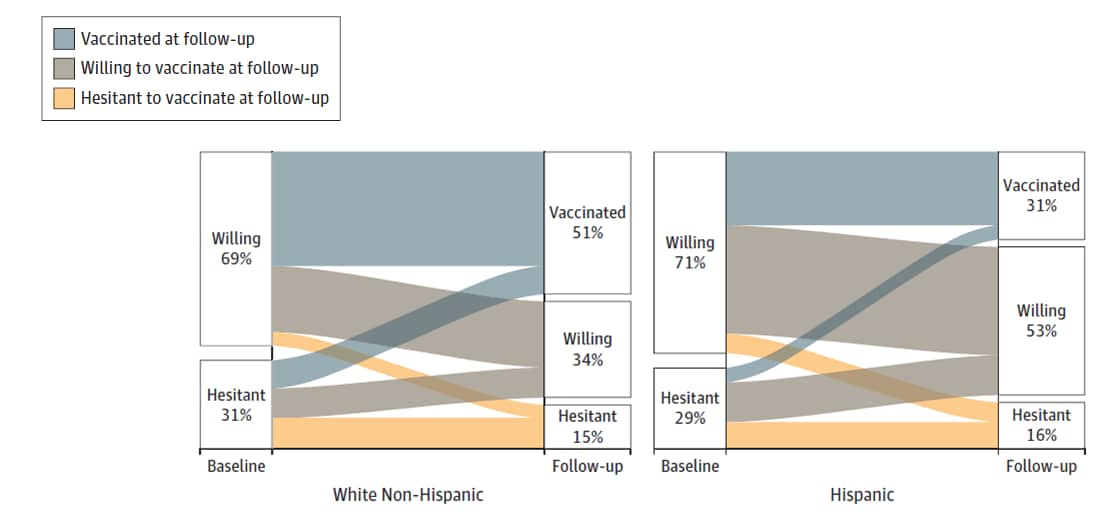
- Vaccine willingness at baseline was similar for Hispanic/Latino and non-Hispanic White participants (71% vs. 69%), but Hispanic/Latino participants had lower vaccination rates at follow-up (31% vs. 51%; Figure).
- Vaccination was confirmed with antibody test results (94.8% sensitivity; 99.1% specificity), suggesting self-reported vaccination status is a valid metric.
Methods: Cohort study of 3,439 U.S. respondents who completed surveys at baseline (August 9–December 8, 2020) and follow-up (March 2–April 21, 2021) to measure vaccine hesitancy, and who self-collected biological specimens to measure antibody response. Limitations: Follow-up period ended before vaccines were available to all respondents.
Implications: Vaccine hesitancy declined in this sample. However, differences in vaccination by socio-demographic characteristics pose challenges to overall vaccination coverage and achievement of health equity, and also suggest potential barriers to vaccination.
Figure:
Note: Adapted from Siegler et al. Alluvial plot paths from hesitancy at baseline (August 9–December 8, 2020) to vaccination status (vaccinated, willing, hesitant) at follow-up (March 2–April 21, 2021) among a national, weighted sample of 3,439 U.S. respondents by race and ethnicity. Licensed under CC BY.
Two articles this week describe disparities in vaccination rates in Illinois communities. One article assesses the role of income and race/ethnicity in vaccination coverage; the other examines the impact of vaccination inequality on COVID-19 severity.
PEER-REVIEWED
A. Social and economic inequality in coronavirus disease 2019 vaccination coverage across Illinois countiesexternal icon. Liao. Scientific Reports (September 16, 2021).
Key findings:
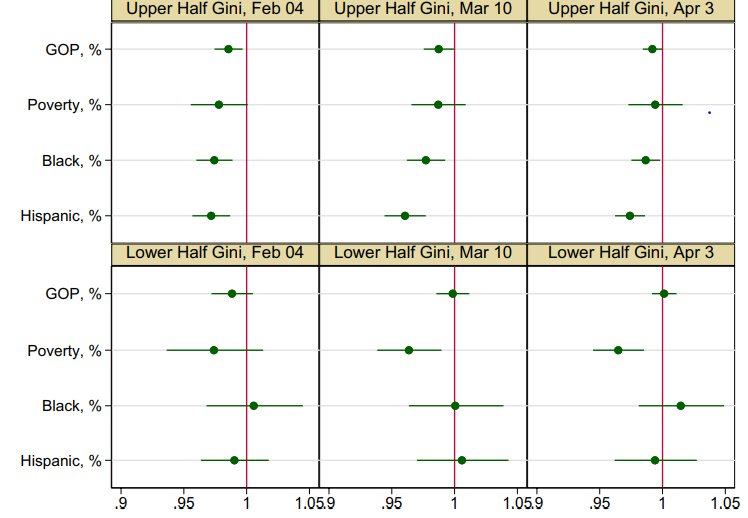
- Among Illinois counties with higher income inequality, higher percentages of either Black or Hispanic/Latino populations were consistently associated with lower odds of full vaccination in the county (Figure).
- Among Illinois counties with lower income inequality, greater poverty among county residents was associated with lower odds of full vaccination in the county during March–April 2021 (Figure).
Methods: Ecological county-level analysis of socioeconomic factors and vaccination coverage in 51 Illinois counties in 3 waves on February 4, March 10, and April 3, 2021; data were stratified by county income inequality as calculated by median Gini index. Limitations: Study conducted during early phases of vaccination distribution; findings may not be generalizable to communities in other U.S. states.
Figure:
Note: Adapted from Liao. Odds ratios (95% CI) of a county being fully vaccinated by county-level political affiliation, poverty, and race and ethnic composition, stratified by income inequality (upper half Gini indicates higher income inequality, lower half Gini indicates lower income inequality). Estimates adjusted for county population density, percent population aged ≥65 years, percent male, and percent uninsured. GOP = Republican. Licensed under CC BY 4.0
PREPRINTS (NOT PEER-REVIEWED)
B. Consequences of COVID-19 vaccine allocation inequity in Chicagoexternal icon. Zeng et al. medRxiv (September 23, 2021).
Key findings:
- The percentage of Chicago residents identifying as non-Hispanic/Latino Black was 80% in the least vaccinated ZIP codes and 8% in ZIP codes with highest vaccination coverage.
- Lower ZIP-code level vaccination coverage was significantly correlated with greater COVID-19 deaths.
- 72% of deaths among Chicago residents in ZIP codes with the lowest quartile of vaccination coverage could have been prevented if vaccination coverage was similar to vaccine coverage in the highest quartile ZIP codes.
Methods: Ecological ZIP code-level analysis of COVID-19-associated cases, deaths, and 1st-dose vaccination coverage (as of March 28, 2021) in Chicago, August 2020—June 2021. ZIP codes were grouped by (1) lowest quartile of vaccine coverage, (2) middle 2 quartiles, and (3) highest quartile. Limitations: Population characteristics of ZIP codes can be heterogenous; ecological design limits controlling for individual-level factors.
Implications for Liao and Zeng et al.: Communities in Chicago and other Illinois counties experienced unequal COVID-19 vaccine coverage. Reducing disproportionate morbidity and mortality from COVID-19 may require vaccination strategies that are informed by community social and economic needs.
PEER-REVIEWED
Prior infection and age impacts antibody persistence after SARS-CoV-2 mRNA vaccine.external icon Fraley et al. Clinical Infectious Diseases (September 22, 2021).
Key findings:
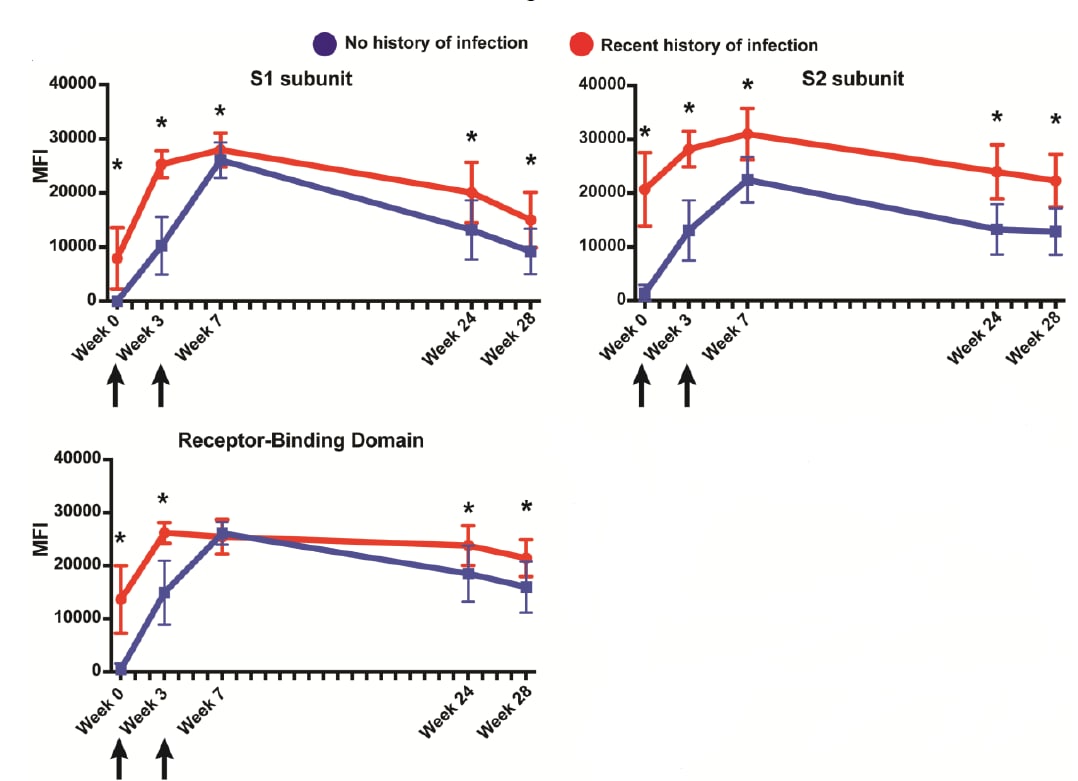
- Higher antibody levels were observed among vaccinated healthcare workers (HCWs) with recent SARS-CoV-2 infection compared with vaccinated HCWs without prior infection (Figure).
- Among HCWs without prior SARS-CoV-2 infection, persons aged 18–49 years had higher antibody response at week 3 (2nd vaccination dose) and week 28 (~7 months following 1st vaccination dose), compared with persons aged ≥50 years.
Methods: Among 188 HCWs fully vaccinated with BNT162b2 (Comirnaty, Pfizer/BioNTech), antibody levels up to 28 weeks after the 1st vaccine dose among HCWs with SARS-CoV-2 infection 30–60 days prior to vaccination were compared with levels among HCWs without prior infection. Limitations: Did not examine SARS-CoV-2 infection >60 days before vaccination.
Implications: Magnitude and duration of antibody response and protection from vaccination may be higher among those with prior SARS-CoV-2 infection and younger persons, which could inform ideal timing of booster vaccination.
Figure:
Note: Adapted from Fraley et al. Antibody levels for SARS-CoV-2 spike subunit 1 (S1), spike subunit 2 (S2), and receptor-binding domain over time among vaccinated HCWs with a recent SARS-CoV-2 infection and those without prior infection. Week 0 = 1st vaccination dose; week 3 = 2nd vaccination dose; MFI = Median Fluorescent Intensity; *indicates p <0.05. Used by permission of the Infectious Diseases Association of America and Oxford University Press.
PEER-REVIEWED
Assessment of a program for SARS-CoV-2 screening and environmental monitoring in an urban public school district.external icon Crowe et al. JAMA Network Open (September 22, 2021).
Key findings:
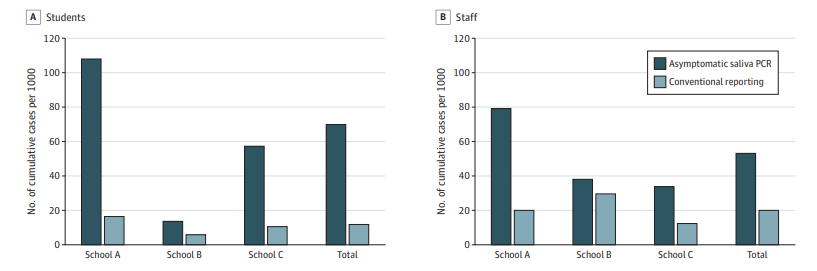
- Weekly SARS-CoV-2 saliva testing over 5 weeks resulted in higher cumulative case detection rates (per 1,000) among students (7.0%) and staff (5.3%) compared with conventional passive case reporting (1.2% and 2.1%, respectively) (Figure).
- 46 individuals were found to have SARS-CoV-2 and 2 clustering events were identified through genome sequencing.
- Participating schools detected SARS-CoV-2 RNA in wastewater samples.
Methods: Evaluation of a school-based weekly saliva PCR COVID-19 testing and environmental monitoring (wastewater, air, surface) pilot program in 3 Omaha, NE public schools (November 9–December 11, 2020); 773 in-person students and faculty were included. Genome sequencing conducted on positive saliva samples. Limitations: Findings may not be generalizable to other schools; incomplete testing among students may underestimate findings; conducted before vaccines were available.
Implications: Routine COVID-19 testing and environmental monitoring may be an effective school-based strategy to rapidly identify SARS-CoV-2 infections and enable implementation of risk-mitigation plans.
Figure:
Note: Adapted from Crowe et al. Cumulative SARS-CoV-2 case rates detected by weekly saliva PCR testing. Comparing in-person school pilot program (asymptomatic saliva PCR) and conventional reporting for A) students and B) staff. Licensed under CC BY.
Vaccines
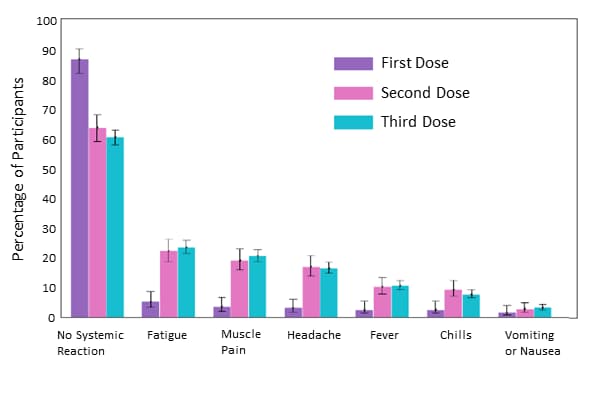
- Self-reported and physiological reactions to the third BNT162b2 mRNA COVID-19 (booster) vaccine doseexternal icon. Mofaz et al. medRxiv (Preprint; September 21, 2021). In a prospective observational study in Israel, self-reported reactions and biometrics were recorded for Israeli adults who received ≥1 of 3 doses of the BNT162b2 vaccine. Reactions were similar following the 2nd and 3rd doses, and were more frequent than after the 1st dose. Reactions after the 3rd dose were more common in participants who were aged <65 years, female, and had no underlying medical conditions.
Note: Adapted from Mofaz et al. Percentage of adults reporting symptoms following the first, second or third dose of Pfizer BNT162b2 vaccination. Used by permission of authors.
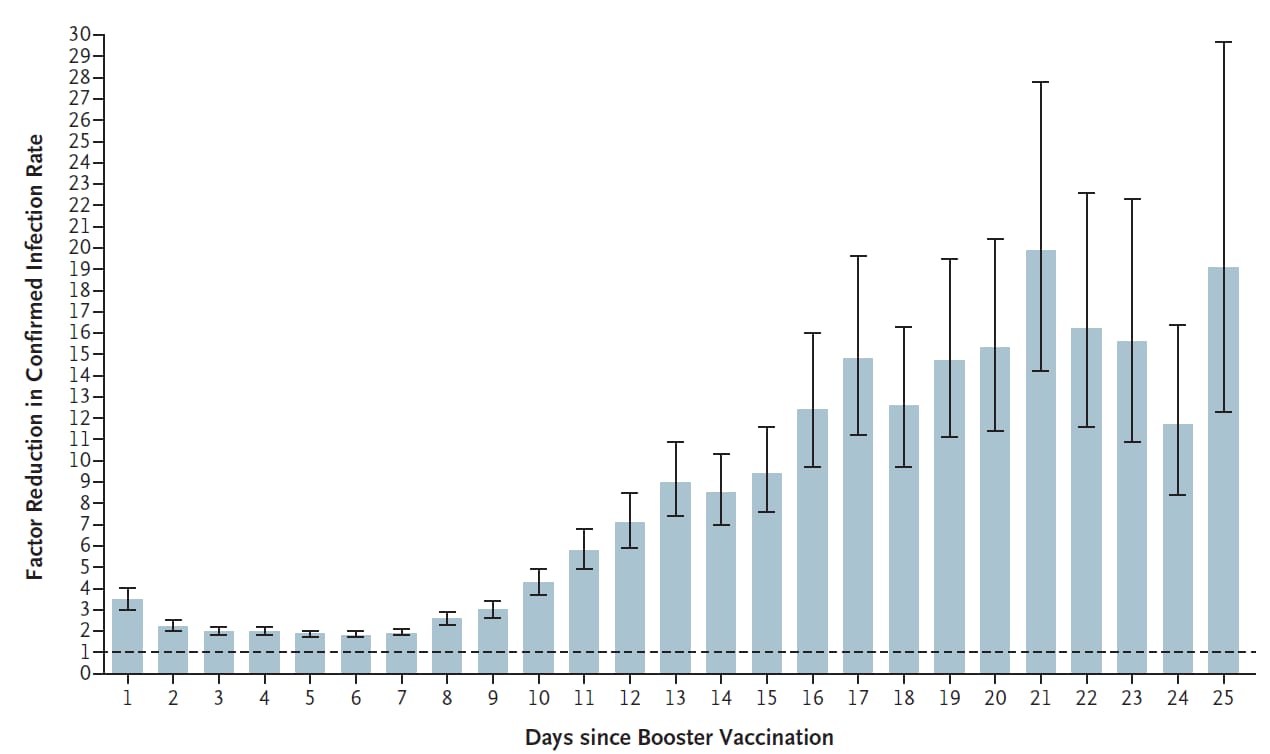
- Protection of BNT162b2 vaccine booster against COVID-19 in Israelexternal icon. Bar-On et al. NEJM (September 15, 2021). Among residents of Israel aged ≥60 years who had been vaccinated ≥5 months earlier (BNT162b2), a booster dose reduced the rate of SARS-CoV-2 infection by a factor of 11.3 (95% CI 10.4-12.3) and the rate of severe illness by a factor of 19.5 (95% CI 12.9-29.5), compared with persons who did not receive a booster dose. On each day between 12 and 25 days after receipt of the booster, the rate of confirmed infection was reduced by a factor of 7–20.
Note: Adapted from Bar-On et al. Factor reduction in the rate of confirmed infection among participants who received a 3rd (booster) dose of the BNT162b2 vaccine as compared with those who did not receive a booster dose, by the number of days after the administration of the booster dose. The dashed horizontal line represents the level at which the booster dose provided no added protection. From the New England Journal of Medicine, Bar-On et al., Protection of BNT162b2 vaccine booster against COVID-19 in Israel. September 15, 2021, online ahead of print. Copyright © 2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
Variants
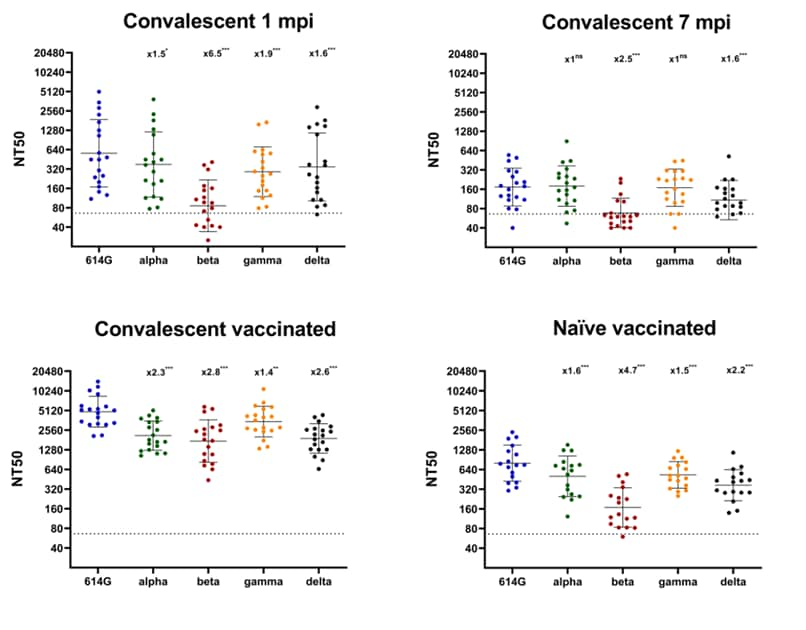
- Prime boost vaccination with BNT162b2 induces high neutralizing activity against SARS-CoV-2 variants in naïve and COVID-19 convalescent individualsexternal icon. Luczkowiak et al. Open Forum Infectious Diseases (September 24, 2021). In an analysis of COVID-19 naïve and infected healthcare workers during convalescence and post-BNT162b2 vaccination, sera from convalescent people showed decreased neutralizing activity against variants at 1 month post-infection, compared with the reference strain. Those fully vaccinated with BNT162b2 showed high levels of neutralizing antibodies to all variants, with convalescent people showing the highest neutralizing response.
Note: Adapted from Luczkowiak et al. Plasma neutralizing levels (NT50) against SARS-CoV-2: Reference S D614G and variants Alpha, Beta, Gamma, and Delta during COVID-19 convalescence and after BNT161b2 vaccination. Convalescent individuals (n = 19) tested 1-month post-infection (mpi), 7 mpi, and after BNT162b2; naïve group (n = 17) after BNT162b2. NT50 dilution values are presented as reciprocals. Solid lines: geometric mean; error bars: geometric SD. Dashed lines: cut-off titer (NT50 = 1/66). Fold-decrease in NT50 above scatter plot; *** statistically significant changes. Licensed under CC-BY-NC-ND.
Health Equity
- Outcome comparison of high-risk Native American patients who did or did not receive monoclonal antibody treatment for COVID-19external icon. Close et al. JAMA Network Open (September 21, 2021). Among Native American people eligible for monoclonal antibody (mAb) treatment (n = 481) at a rural acute care facility in Arizona, 201 COVID-19 patients received mAb and experienced lower odds of death (OR 0.44, 95% CI 0.29-0.66) than eligible patients who did not receive mAb.
- Understanding racial differences in attitudes about public health efforts during COVID-19 using an explanatory mixed methods designexternal icon. Nong et al. Social Science and Medicine (October 2021). In a study linking quantitative findings to explanatory qualitative interview questions (n = 1,000), Black or African American Michigan residents’ trust in public health agencies (adjusted beta coefficient [b] 0.07, p = 0.48) was not different from that of White residents (adjusted beta coefficient [b] 0.07, p = 0.48). An increased willingness to participate in public health interventions may be related to altruism and perceived risk of COVID-19 in the community.
- Identifying at-risk communities and key vulnerability indicators in the COVID-19 pandemicexternal icon. Thais et al. medRxiv (Preprint; September 22, 2021). In a validation study using open-source data to construct a model to describe communities at higher risk of COVID-19 and determine indicators for vulnerability during the COVID-19 pandemic, results suggest that prevalence of COVID-19 in a given area has more impact than prevalence of pre-existing co-morbidities. Childhood poverty, food insecurity, COVID-19 hospitalization rate, unemployment rate, and access to care were key indicators.
Natural History, Reinfection, and Health Impact
- The longitudinal kinetics of antibodies in COVID-19 recovered patients over 14 monthsexternal icon. Eyran et al. medRxiv (Preprint; September 21, 2021). Among 89 COVID-19 recovered patients and 17 infection-naïve BNT162b2 vaccinees followed over 14 months, antibody levels waned in 18% (IgG), 55% (IgM), and 62% (IgA) of persons to levels considered negative. Antibody decay rate in COVID-19-recovered patients was significantly slower compared with the decay in infection-naïve vaccinees.
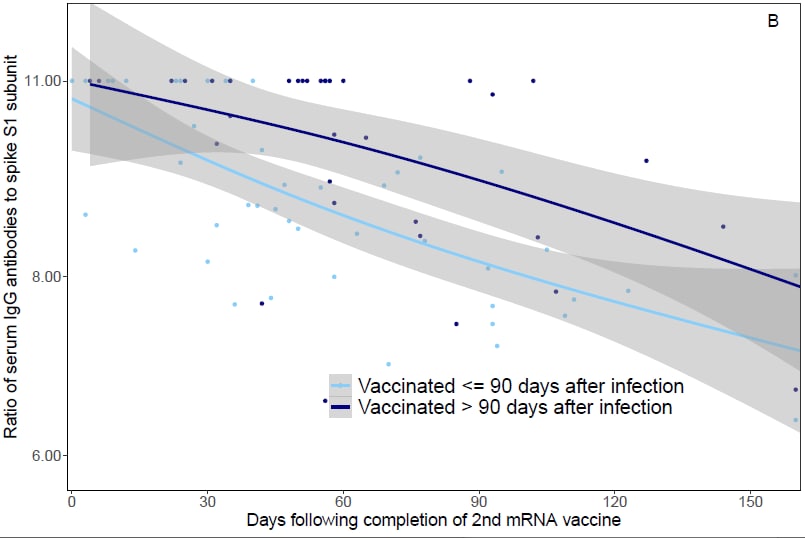
- Impact of prior SARS-CoV-2 infection on post-vaccination SARS-CoV-2 spike IgG antibodies in a longitudinal cohort of healthcare workersexternal icon. Zhong et al. medRxiv (Preprint; September 22, 2021). Published in JAMA as Durability of antibody levels after vaccination with mRNA SARS-CoV-2 vaccine in individuals with or without prior infectionexternal icon (November 1, 2021). From June–September 2021, healthcare workers (HCWs) who received 2 doses of an mRNA vaccine (n = 1,960) had higher serum spike IgG antibody levels than HCWs with natural infection (n = 98). Serum IgG antibody values were 14%, 19%, and 56% higher for those infected with SARS-CoV-2 prior to vaccination (n = 73) than naïve HCWs (n = 1,887) at 1, 3, and 6 months after vaccination, respectively. HCWs infected >90 days before vaccination (n = 32) had 10% higher IgG levels than those infected < 90 days before vaccination (n = 41).
Note: Adapted from Zhong et al. A) Serum spike S1 IgG antibody levels ≥14 days following 2 doses of SARS-CoV-2 mRNA vaccine in HCWs with prior SARS-CoV-2 infection, without prior SARS-CoV-2 infection, and in those following SARS-CoV-2 positive PCR test and before vaccination. B) Serum spike S1 IgG antibody mRNA vaccination among HCWs with SARS-CoV-2 infection ≤90 days before vaccination and >90 days before vaccination. The lines represent median IgG as a function of days following mRNA vaccination or natural infection, based on natural cubic splines (2 degrees of freedom) for each group. Shaded areas represent 95% confidence intervals. Licensed under CC-BY-NC-ND 4.0.
- Comparison of children and young people admitted with SARS-CoV-2 across the UK in the first and second pandemic waves: prospective multicentre observational cohort studyexternal icon. Swann et al. medRxiv (Preprint; September 17, 2021). Published in Pediatric Research as Comparison of UK paediatric SARS-CoV-2 admissions across the first and second pandemic wavesexternal icon (April 22, 2022). Compared with children and adolescents hospitalized with COVID-19 during Wave 1 (January–July 2020), children and adolescents hospitalized during Wave 2 (August 2020–January 2021) were more likely to be older (median age [years] 6.5 vs. 4.0), and less likely to be at risk for clinical deterioration at presentation (38% vs. 47%), be prescribed antibiotics (51% vs. 67%), and need respiratory/cardiovascular support. The percentage admitted to critical care did not differ between waves (12% vs. 13%).
- Childhood asthma and COVID-19: a nested case-control studyexternal icon. Gaietto et al. medRiv (Preprint; September 22, 2021). Published in Pediatric Allergy and Immunology as Asthma as a risk factor for hospitalization in children with COVID-19: A nested case-control studyexternal icon (November 14, 2021). In a nested case-control study using clinical registry data, asthma severity in children was not associated with a higher risk of SARS-CoV-2 infection. Children with COVID-19 and asthma were more than 4 times as likely to be hospitalized compared with children with COVID-19 and without asthma; however, there was no difference in hospital stay length or need for respiratory support.
From the Morbidity and Mortality Weekly Report (Month, day, year).
- Disparities in COVID-19 Vaccination Status, Intent, and Perceived Access for Noninstitutionalized Adults, by Disability Status — National Immunization Survey Adult COVID Module, United States, May 30–June 26, 2021
- Association Between K–12 School Mask Policies and School-Associated COVID-19 Outbreaks — Maricopa and Pima Counties, Arizona, July–August 2021
- COVID-19–Related School Closures and Learning Modality Changes — United States, August 1–September 17, 2021
- Pediatric COVID-19 Cases in Counties With and Without School Mask Requirements — United States, July 1–September 4, 2021
- Safety Monitoring of an Additional Dose of COVID-19 Vaccine — United States, August 12–September 19, 2021
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.