COVID-19 Science Update released: June 25, 2021 Edition 95

The COVID-19 Science Update summarizes new and emerging scientific data for public health professionals to meet the challenges of this fast-moving pandemic. Weekly, staff from the CDC COVID-19 Response and the CDC Library systematically review literature in the WHO COVID-19 databaseexternal icon, and select publications and preprints for public health priority topics in the CDC Science Agenda for COVID-19 and CDC COVID-19 Response Health Equity Strategy.
Section headings in the COVID-19 Science Update align with the CDC Science Agenda for COVID-19.
Section headings in the COVID-19 Science Update have been changed to align
with the CDC Science Agenda for COVID-19.
Here you can find all previous COVID-19 Science Updates.
PEER-REVIEWED
BNT162b2-elicited neutralization of B.1.617 and other SARS-CoV-2 variants.external icon Liu et al. Nature. (June 10, 2021).
Key findings:
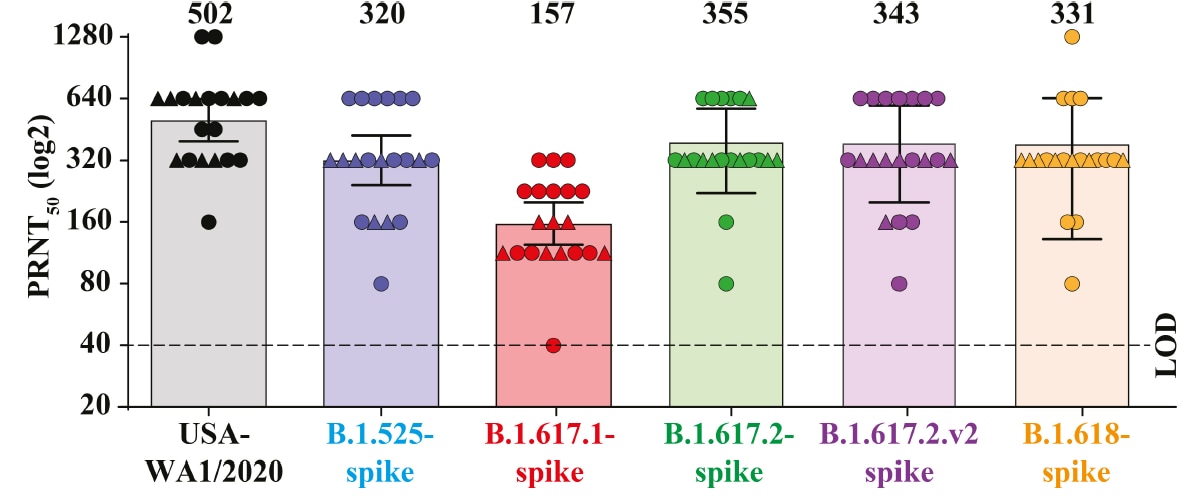
- All sera samples neutralized the SARS-CoV-2 wild-type (WA1/2020) virus and variant viruses B.1.525, B.1.617.1, B.1.617.2, and B.1.618 (Figure).
- Neutralization of all variants, except B.1.617.1, was only modestly reduced relative to the wild-type virus.
- Neutralization of B.1.617.1 was reduced to 0.31 times that of the wild-type virus.
Methods: Neutralizing antibody responses to SARS-CoV-2 wild-type virus and spike protein variants B.1.617.1, B.1.617.2, B.1.618 (all first identified in India) and B.1.525 (first identified in Nigeria) were examined in human sera (n = 20) 2 or 4 weeks after 2nd dose of BNT162b2 (Pfizer/BioNTech). Limitations: Potential for mutations to alter neutralization by affecting spike protein function rather than antigenicity; only examined effect of spike protein mutations on neutralization.
Implications: To date, there is no evidence that SARS-CoV-2 variants have escaped BNT162b2-mediated protection from COVID-19.
Figure:
Note: Adapted from Liu et al. Neutralization of SARS-CoV-2 wild-type (USA-WA1/2020) and variants B.1.525, B.1.617.1, B.1.617.2, B.1.617.2.v2 (B.1.617.2-spike plus an additional E156G substitution and F157-R158 deletion) and B.1.618 by BNT162b2 vaccine-elicited sera. Each data point represents the geometric mean neutralization titer (PRNT50) against the indicated virus obtained from a serum sample obtained 2 weeks (circles) or 4 weeks (triangles) after the 2nd dose of vaccine. The heights of bars and the numbers over the bars indicate geometric mean titers. The horizontal bars indicate 95% confidence intervals. The dashed line indicates the limit of detection (LOD) at 1:40. Reprinted by permission from Springer Nature Customer Service Centre GmbH: Springer Nature. Nature, BNT162b2-elicited neutralization of B.1.617 and other SARS-CoV-2 variants. Liu et al. COPYRIGHT 2021.
Characterising the background incidence rates of adverse events of special interest for COVID-19 vaccines in eight countries: multinational network cohort study.external icon Li et al. BMJ (June 14, 2021).
Key findings:
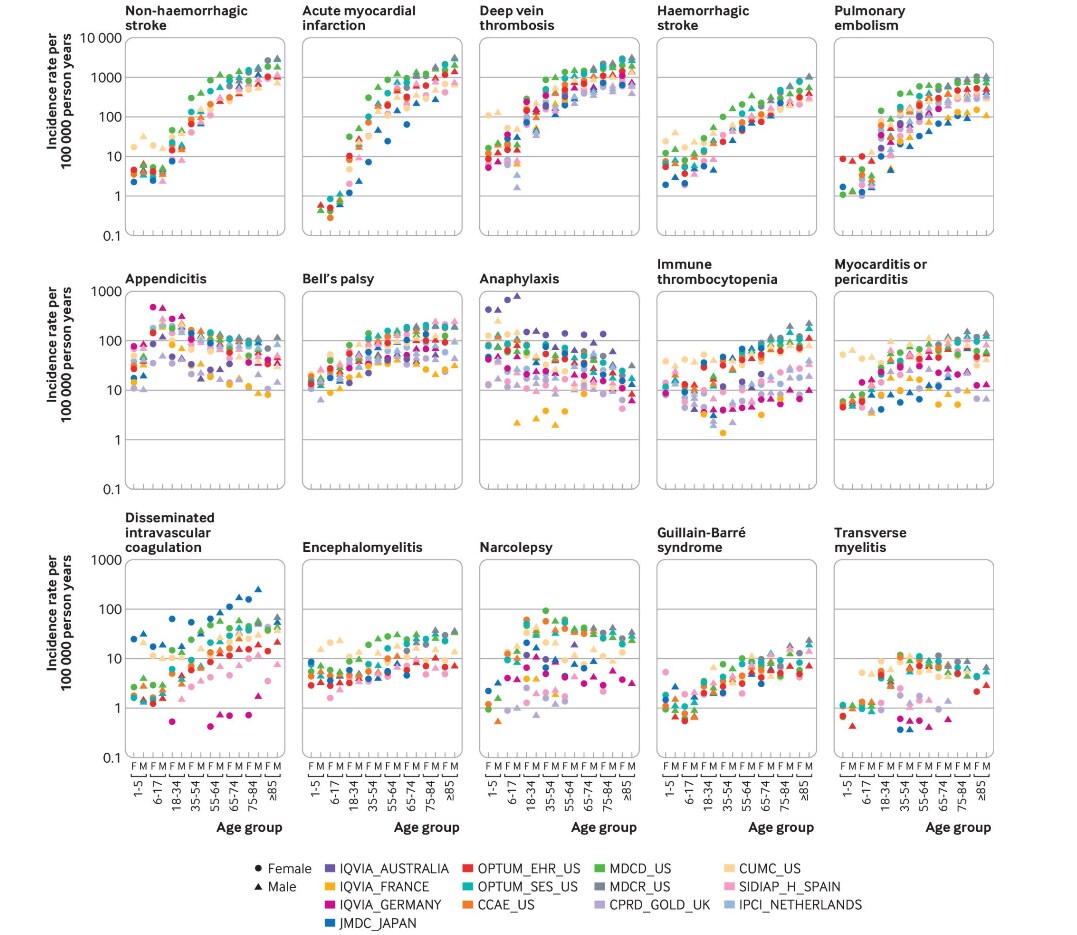
- While background incidence rates varied greatly across databases, similar age and sex trends were observed for each adverse event of special interest (AESI) (Figure).
- Rates of deep vein thrombosis, acute myocardial infarction, hemorrhagic and non-hemorrhagic stroke, pulmonary embolism, Bell’s palsy, immune thrombocytopenia, Guillain-Barré syndrome, and disseminated intravascular coagulation increased with age (Figure).
Methods: Retrospective study using data from 13 electronic health record databases in 8 countries to determine background incidence rates of 15 AESIs potentially associated with COVID-19 vaccines. AESI data were collected from 126,661,070 individuals enrolled between January 1, 2017 and December 31, 2019. Age and sex-specific background incidence rates were calculated across databases and pooled. Limitations: Observational study.
Implications: Due to large variation in AESI rates between databases, the same data source should be used to compare post-COVID-19 vaccination (observed) and background (expected) AESI rates for vaccine safety monitoring.
Figure:
Note: Adapted from Li et al. Age and sex (females: circles, males: triangles) stratified incidence rates (per 100,000 person years) for 15 adverse events of special interest by database. Abbreviated name of electronic health record database is shown before each country name in the legend. Licensed under CC BY 4.0.
SARS-CoV-2 Delta VOC in Scotland: demographics, risk of hospital admission, and vaccine effectiveness.external icon Sheikh et al. Lancet (June 14, 2021).
Key findings:
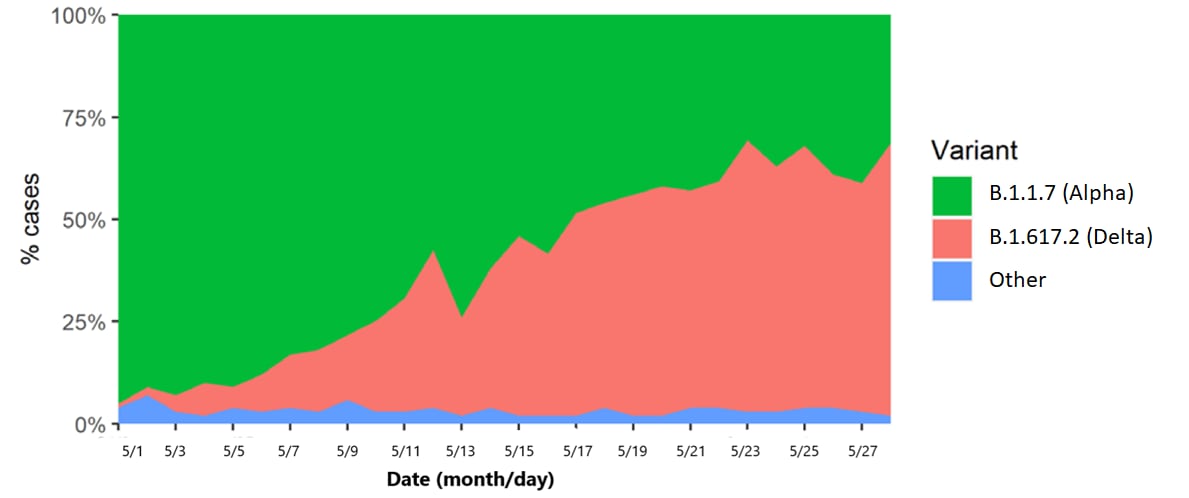
- In May 2021, the B.1.617.2 (Delta) variant became the dominant SARS-CoV-2 strain in Scotland (Figure).
- B.1.617.2 made up 97% of S-gene positive cases, which comprises 40% (7,723/19,543) of all cases and 36% (134/377) of hospitalizations.
- S-gene positive cases were associated with increased hospitalization risk (aHR 1.85, 95% CI 1.39-2.47) compared to S-gene negative cases.
- Both BNT1682b (Pfizer/BioNTech) and ChAdOx1 (Oxford/AstraZeneca) vaccines were effective in preventing hospitalization regardless of S-gene status.
Methods: S-gene positive and S-gene negative (i.e., B.1.1.7, Alpha variant) infections and genomic sequencing obtained from multi-target SARS-CoV-2 PCR tests. Hospitalization risk for S-gene positive cases and estimated BNT1682b and ChAdOx1 vaccine effectiveness in preventing hospitalizations ≥14 days after 2nd dose determined from surveillance data (n = 19,543) collected between April 1 and June 6, 2021. Limitations: Observational study.
Implications: The SARS-CoV-2 B.1.617.2 variant rapidly replaced B.1.1.7 in Scotland and was associated with increased hospitalization risk. However, COVID-19 vaccines appear effective in preventing hospitalization from B.1.617.2.
Figure:
Note: Adapted from Sheikh et al. Changing proportions of infections due to SARS-CoV-2 B.1.1.7 (Alpha), B.1.617.2 (Delta), and other variant viruses in Scotland over time. All dates are from 2021. Reprinted from The Lancet, online June 14, 2021, Sheikh et al., SARS-CoV-2 Delta VOC in Scotland: demographics, risk of hospital admission, and vaccine effectiveness. Copyright 2021, with permission from Elsevier.
First-dose ChAdOx1 and BNT162b2 COVID-19 vaccines and thrombocytopenic, thromboembolic and hemorrhagic events in Scotland.external icon Simpson et al. Nature Medicine (June 9, 2021).
Key findings:
- Within 0-27 days after the 1st dose, ChAdOx1 (Oxford/AstraZeneca) vaccination was associated with rare but higher occurrences of:
- Idiopathic thrombocytopenic purpura (ITP) (aRR 5.77, 95% CI 2.41-13.83), representing 1.13 (95% CI 0.62-1.63) incident cases per 100,000 doses (Figure).
- Arterial thromboembolic events (aRR 1.22, 1.12-1.34).
- Hemorrhagic events (aRR 1.48 95% CI 1.12-1.96).
- No positive associations were seen between BNT162b2 (Pfizer/BioNTech) and thrombocytopenic, thromboembolic, or hemorrhagic events.
Methods: Assessment of hematological and vascular adverse events after the 1st dose of ChAdOx1 (n = 1.7 million) or BNT162b2 (n = 0.82 million) using an incident-matched case-control study design among individuals aged 16+ in Scotland between December 2020 and April 2021. Limitations: 2nd dose analysis not performed; results may be overestimated based on unknown confounders.
Implications: The ChAdOx1 vaccine might be associated with a very small increased incidence of ITP, which was not seen with BNT162b2. This very small risk needs to be considered within the context of the clear benefits of the vaccine.
Figure:
Note: Adapted from Simpson et al. Date of 1st vaccine dose and vaccine type for individuals with an idiopathic thrombocytopenic purpura event. AZ: ChAdOx1; PB: BNT162b2. Licensed under CC BY 4.0.
Safety and immunogenicity of a third dose of SARS-CoV-2 vaccine in solid organ transplant recipients: a case series.external icon Werbel et al. Annals of Internal Medicine (June 15, 2021).
Key findings:
- At a median of 14 days after the 3rd dose:
- All 6 patients with low-positive antibody titers before the 3rd dose had high-positive antibody titers.
- Of 24 patients with negative titers before the 3rd dose, 6 had high-positive antibody titers, 2 had low-positive antibody titles, and 16 remained negative.
- Most frequently reported vaccine reactions after the 3rd dose included mild or moderate local reactions (15 participants) and fatigue (14 participants).
Methods: Case series describing 30 solid organ transplant patients determined to have a suboptimal antibody response to 2 doses of either BNT162b2 (Pfizer/BioNTech) or mRNA-1273 (Moderna) and subsequently received a 3rd vaccine dose (either Ad26.COV2.S (Johnson & Johnson/Janssen), BNT162b2, or mRNA-1273). Antibody testing was done at a median of 9 days before and at a median of 14 days after receiving the 3rd dose. Patients completed a vaccine reaction questionnaire 7 days after receiving the 3rd dose. Limitations: Small convenience sample; not representative of all solid organ transplant recipients. Included only those with a “suboptimal” response (not defined in the paper) to standard vaccination.
Implications: A 3rd dose of mRNA vaccine might offer increased protection against COVID-19 among solid organ transplant patients, with only mild to moderate reactions.
PREPRINTS (NOT PEER-REVIEWED)
Antibody responses to SARS-CoV-2 after infection or vaccination in children and young adults with inflammatory bowel disease.external icon Dailey et al. medRxiv (June 15, 2021). Published in Inflammatory Bowel Diseasesexternal icon (September 16, 2021).
Key findings:
- 44/436 of children and young adults being treated with infliximab or vedolizumab for inflammatory bowel disease (IBD) had SARS-CoV-2 spike protein receptor-binding domain (S-RBD) antibodies.
- 6 months post-infection these patients lacked neutralizing antibody.
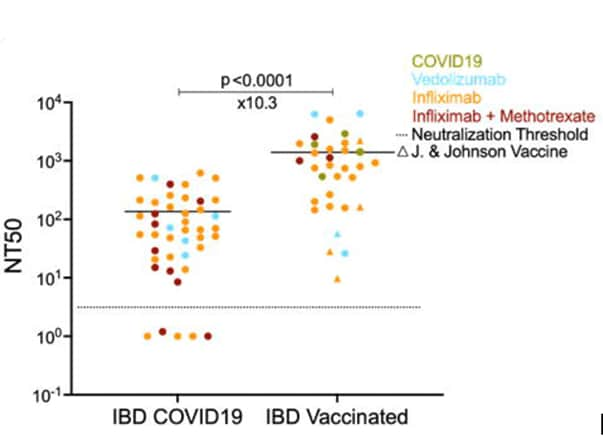
- Anti-S-RBD antibody levels and neutralization capacity were approximately 15 and 10 times higher, respectively, following COVID-19 vaccination compared to natural infection (Figure).
Methods: Single-center prospective study (May 2020–April 2021) evaluating SARS-CoV-2 S-RBD antibody positivity in 436 persons aged 2–26 years with IBD who were treated with infliximab or vedolizumab. Antibody response and neutralization capacity determined approximately 3 weeks after complete vaccination, [BNT1682b (Pfizer/BioNTech) = 21, mRNA-1273 (Moderna) = 7, Ad26.COV2.S (Johnson & Johnson/Janssen) = 5] and compared to that of natural infection. Limitations: No control data from IBD patients not receiving biologics; no longitudinal data on durability of post-vaccination antibody response.
Implications: Young persons with IBD who are treated with biologics could be at increased risk for SARS-CoV-2 reinfection due to the short durability of SARS-CoV-2 neutralizing antibody response after natural infection. However, at least initially, COVID-19 vaccination appears to provide robust protection.
Figure:
Note: Adapted from Dailey et al. Neutralization titers (NT50) in pediatric and young adult IBD patients who were COVID-19 seropositive (n = 44) or vaccinated with an mRNA vaccine (BNT1682b or mRNA1273) or Ad26.COV2.S (n = 33), by IBD treatment group: vedolizumab, infliximab, infliximab and methotrexate. Green dots represent COVID-19 seropositive patients among the vaccinated group. Circles indicate vaccination with an mRNA vaccine and triangles indicate vaccination with Ad26.COV2.S. Horizontal bars show the mean value. The x value under the significance bar represents the fold change between the mean values of groups. Dotted line indicates the neutralization threshold which was NT50 of 5. Used by permission of authors.
Casirivimab and imdevimab in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label, platform trial.external icon Horby et al. medRxiv (June 16, 2021). Published in The Lancetexternal icon (February 10, 2022).
Key findings:
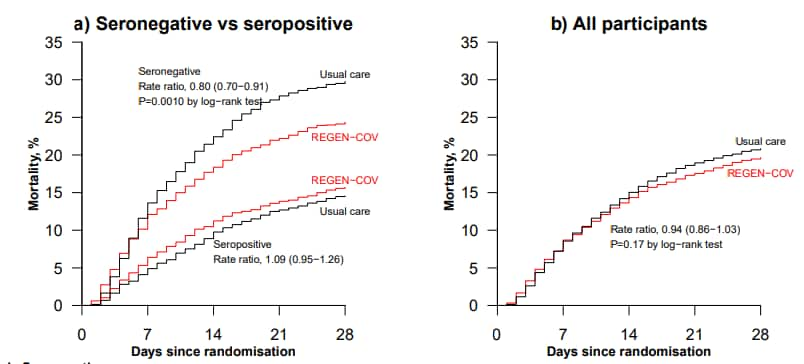
- Among patients seronegative at hospital admission, significantly fewer COVID-19 patients who received REGEN-COV antibody therapy died within 28 days than did patient controls (RR 0·80; 95% CI 0·70-0·91):
- 24% of patients receiving REGEN-COV vs. 30% of patient controls died (Figure, panel A).
- Among all patients, regardless of baseline antibody status, there was no significant difference in 28-day mortality between those who received REGEN-COV therapy and patient controls (RR 0·94; 95% CI 0·86-1·03; p = 0·17):
- 20% of patients receiving REGEN-COV vs. 21% of patient controls died (Figure, panel B).
Methods: In a randomized trial conducted at 127 UK hospitals (September 2020–May 2021), 9,785 patients were assigned to receive usual care (controls) or usual care plus REGEN-COV (casirivimab and imdevimab) monoclonal antibody therapy. Patients were grouped by anti-SARS-CoV-2 status at admission: 3,153 (32%) seronegative, 5,272 (54%) seropositive and 1,360 (14%) unknown. Vital status, the primary outcome, was determined on day 28 for 99% of the patients. Limitations: Information on other medical outcomes was not collected.
Implications: REGEN-COV monoclonal antibody therapy can reduce mortality among COVID-19 patients who are seronegative at the time of hospitalization; use in the hospital setting might ideally be restricted to these patients.
Figure:
Note: Adapted from Horby et al. Comparison of treatment (usual care or usual care plus REGEN-COV therapy) in a randomized trial of hospitalized COVID-19 patients (a) by antibody status; (b) regardless of antibody status. Licensed under CC BY 4.0.
PREPRINTS (NOT PEER-REVIEWED)
Benefits of surveillance testing and quarantine in a SARS-CoV-2 vaccinated population of students on a university campus.external icon Motta et al. medRxiv (June 18, 2021). Published in JAMA Health Forum as Assessment of simulated surveillance testing and quarantine in a SARS-CoV-2–vaccinated population of students on a university campusexternal icon (October 1, 2021).
Key findings:
- Regardless of outside community infection prevalence:
- At 90% vaccine effectiveness, weekly surveillance testing only marginally reduces viral transmission as compared to no testing (Figure).
- At 50%–75% vaccine effectiveness, weekly surveillance testing can provide over 10-fold reduction in the number of infections (Figure).
- A 10-day quarantine protocol for exposures has limited effect on infections until vaccine effectiveness drops to 50%.
- Testing of exposed students every 2 days is at least as effective as quarantine at limiting infections.
Methods: An agent-based model simulating SARS-CoV-2 spread over 90 days in a population of 5,000 students where vaccine effectiveness may be impacted by vaccine type, variants, and/or waning immunity. Limitations: Parameters in the model were fit to infection dynamics data collected by the surveillance program at Duke University during the 2020-2021 academic year, therefore outcomes may be context and resource-specific; the protection conferred by vaccination is the product of coverage and efficacy, and may not be generalizable to universities without mandatory vaccination.
Implications: On campuses with 100% of students vaccinated and 90% vaccine effectiveness, infections should remain low in the absence of surveillance testing. Increased testing of exposed students may be a viable alternative to quarantine on campuses.
Figure:
Note: Adapted from Motta et al. Daily infection prevalence, with and without surveillance testing. The medians (dark red and blue lines) and 2.75%-97.5% quantile ranges (light red and blue bands) of the daily infection prevalence in the modelled population of 5,000 individuals over 100 simulations, assuming an interaction multiplier of 10. The outside community infection prevalence was fixed at 0.1% (top row) or 1.0% (bottom row), with vaccine effectiveness chosen to be 90% (left), 75% (middle) or 50% (right). Licensed under CC BY 4.0.
PEER-REVIEWED
Naturally enhanced neutralizing breadth against SARS-CoV-2 one year after infection.external icon Wang et al. Nature (June 14, 2021).
Key findings:
- Among unvaccinated convalescent individuals, SARS-CoV-2 neutralizing activity after infection was not significantly different at 6 and 12 months.
- Among convalescent individuals 12 months after infection, neutralizing activity against SARS-CoV-2 variants was greater (21- to 71-fold) among mRNA-vaccinated compared with non-vaccinated individuals (Figure).
Methods: Cohort study examining humoral response in 63 COVID-19-convalescent adults after infection with Wuhan Hu-1. 41% of the adults also received at least 1 dose of a mRNA vaccine. Neutralizing antibodies and number of memory B-cells were assessed at 1.3, 6.2, and 12 months after infection. Neutralizing activity against SARS-CoV-2 variants B.1.351, B.1.1.7, B.1.526, and P.1 was assessed in a sub-group of 30 (15 convalescent-unvaccinated and 15 convalescent-vaccinated) individuals at the same timepoints. Limitations: Small sample sizes.
Implications: mRNA vaccination after SARS-CoV-2 produces antibodies and memory B cells that can protect against circulating SARS-CoV-2 variants for up to 12 months and should be protective against variants. In addition, immunity in convalescents may be long lasting.
Figure:
Note: Adapted from Wang et al. Plasma neutralizing activity (y-axis) against SARS-CoV-2 wild-type (Wuhan-Hu-1) and variants B.1.351, B.1.1.7, B.1.526, and P.1. Time points (x-axis) are in months. COVID-19 non-vaccinated convalescent and vaccinated convalescent (Vac) persons are shown separately at 12 months only. Red bars indicate medians, red numbers indicate the geometric mean neutralization (NT50) at indicated timepoints. Reprinted by permission from Springer Nature Customer Service Centre GmbH: Springer Nature. Nature, Naturally enhanced neutralizing breadth against SARS-CoV-2 one year after infection. Wang et al. COPYRIGHT 2021.
PREPRINTS (NOT PEER-REVIEWED)
SARS-CoV-2-antibody response in health care workers after vaccination or natural infection in a longitudinal observational study.external iconHerzberg et al. medRxiv (June 13, 2021).Published in Vaccineexternal icon (January 8, 2022).
Key findings:
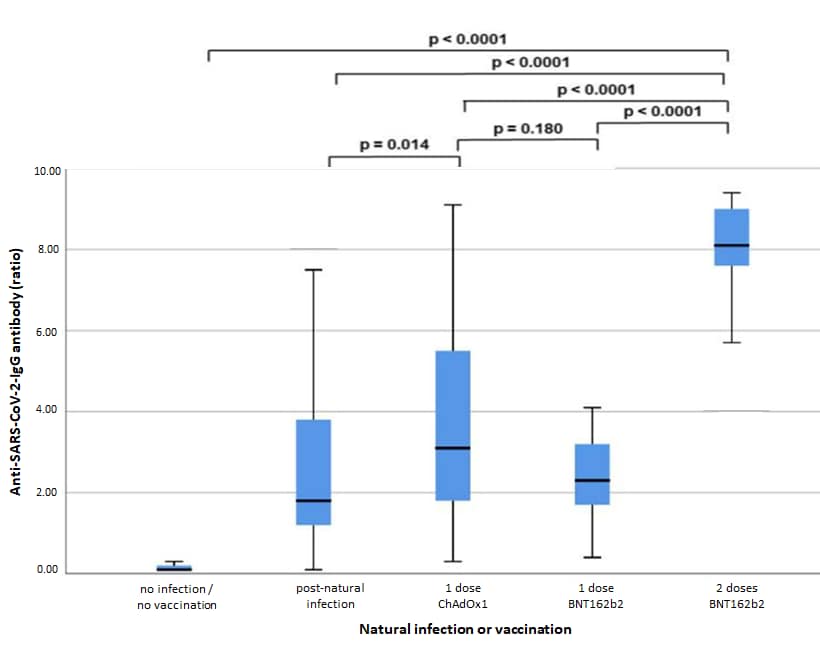
- 2 doses of BNT162b2 (Pfizer/BioNTech) vaccine elicited significantly higher antibody levels compared to:
- A single dose of either BNT162b2 or ChAdOx1 (AstraZeneca) vaccines (Figure).
- Immunity obtained from previous PCR-confirmed SARS-CoV-2 infection (Figure).
Methods: Longitudinal study in Germany, April 2021, comparing anti-SARS-CoV-2 immunoglobulin G (IgG) antibody responses among hospital employees who had received 1 or both doses of BNT162b2 (n = 324) or 1 dose of ChAdOx1 (n = 117), had tested positive for SARS-CoV-2 and had not been vaccinated (n = 52), or who were neither vaccinated nor previously infected (n = 69). Limitations: Single-center study, small sample size (n = 9) in single-dose BNT162b2 group, time frame between vaccination and blood sampling differed between groups of participants.
Implications: 2 doses of BNT162b2 elicit greater antibody response than prior PCR-confirmed SARS-CoV-2 infection or a single dose of BNT162b2 or ChAdOx1 vaccine.
Figure:
Note: Adapted from Herzberg et al. Anti-SARS-CoV-2-IgG antibody ratio by previous infection or vaccination status. According to assay manufacturer, a ratio <0.8 should be interpreted as negative, a ratio ≥0.8 to <1.1 should be considered equivocal, and a ratio ≥1.1 should be interpreted as positive. Solid lines indicate median IgG ratio, outlier values are not shown. Licensed under CC-BY-NC-ND 4.0.
Detection, Burden, and Impact
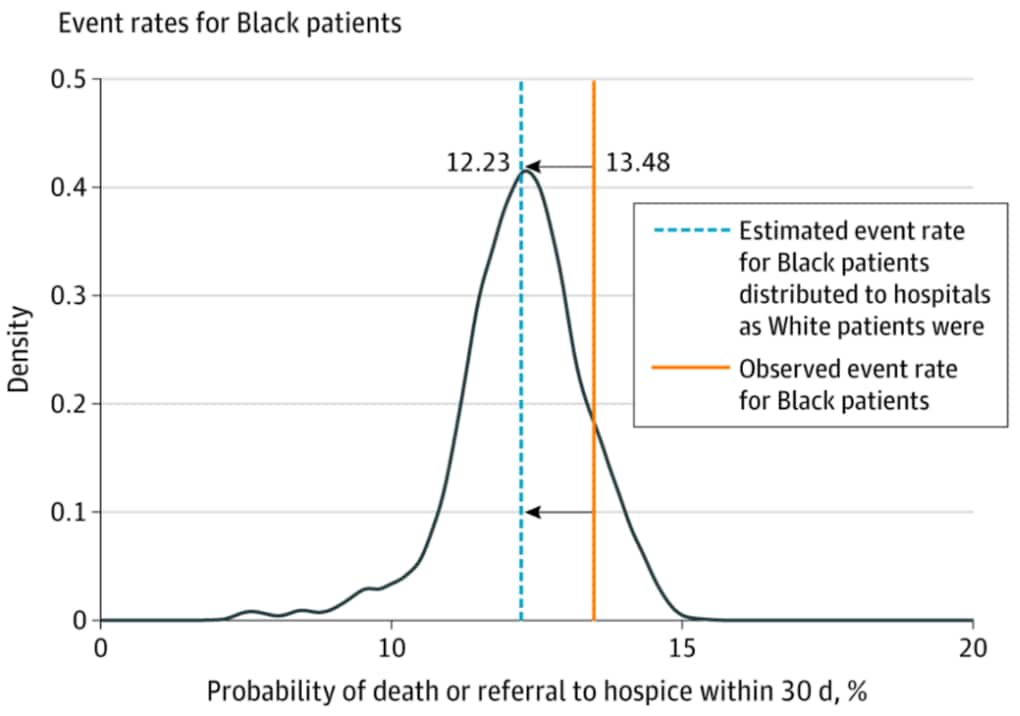
- Asch et al. Patient and hospital factors associated with differences in mortality rates among black and white US Medicare beneficiaries hospitalized with COVID-19 infection.external icon JAMA Network Open (June 17, 2021). After adjustment for clinical and sociodemographic patient characteristics, Black COVID-19 patients admitted to 1,188 hospitals (January–September 2020) were more likely than White patients to die or be discharged to hospice within 30 days of admission (adjusted odds ratio (aOR) 1.11; 95% CI 1.03-1.19). After additional adjustment for hospital fixed effects there was no difference in mortality between Black and White patients (aOR 1.02; 95% CI 0.94-1.10), suggesting higher mortality of Black patients was associated with the hospitals at which they disproportionately received care.
Note: Adapted from Asch et al. A simulation of the probability of death or referral to hospice if Black patients were admitted to the same hospitals as White patients. Solid line is observed rate of mortality or discharge to hospice for Black patients; dashed blue line is rate of mortality or discharge to hospice from simulation. Licensed under CC BY.
- Misra et al. Serological prevalence of SARS-CoV-2 antibody among children and young age (between age 2-17 years) group in India: An interim result from a large multi-centric population-based seroepidemiological study.external icon medRxiv (Preprint; June 16, 2021). Between March 15 and June 10, 2021, SARS-CoV-2 seroprevalence rates were 55.7% in 3,809 adults and 63.5% in 700 children in 4 Indian states. There was no statistically significant difference in seroprevalence between adults (> 18 years) and children aged 2–17 years.
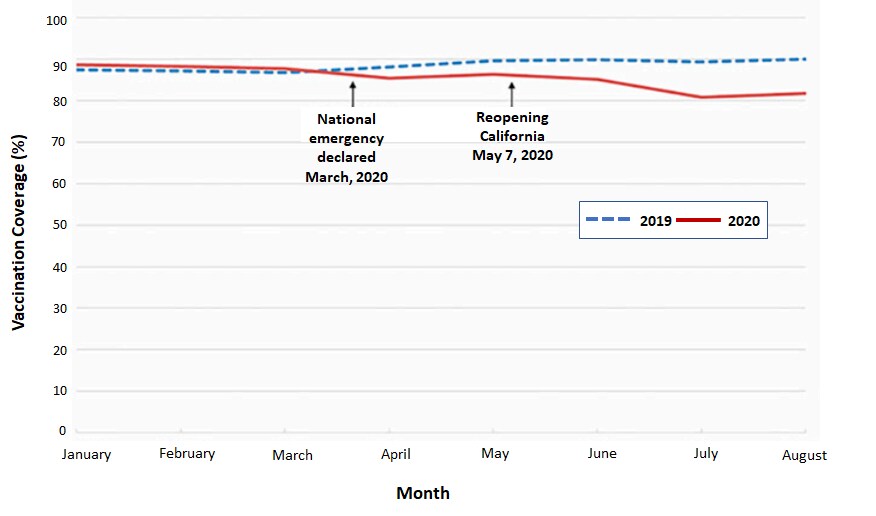
- Ackerson et al. Pediatric vaccination during the COVID-19 pandemic.external icon Pediatrics (June 17, 2021). Compared to January–August 2019, complete childhood vaccination coverage among children aged 0–18 years in an integrated healthcare system in Southern California (n >980,000) declined during the same period in 2020. At age 16 months, measles vaccination coverage in July 2020 was 81% compared to 89% in 2019.
Note: Adapted from Ackerson et al. Measles vaccination coverage at age 16 months in the Kaiser Permanente Southern California (KPSC) integrated healthcare system, January to August 2019 and 2020. Reproduced with permission from Journal Pediatrics, online June 17, 2021, Copyright © 2021 by the AAP.
Natural History of SARS-CoV-2 Infection
- Findings from 2 large multicenter studies released June 16 evaluating specific immunomodulatory therapies for multisystem inflammatory disease in children (MIS-C) appear to conflict. While Son et al., in Multisystem inflammatory syndrome in children – initial therapy and outcomesexternal icon, NEJM, determined that initial treatment with IVIG plus glucocorticoids lowered risk of cardiovascular dysfunction, McArdle et al., in Treatment of multisystem inflammatory syndrome in childrenexternal icon, NEJM, found no significant improvement with IVIG alone, IVIG and glucocorticoids, or glucocorticoids alone. An editorial by DeBiasi, Immunotherapy for MIS-C — IVIG, glucocorticoids, and biologicsexternal icon, NEJM, outlines several possible explanations for these disparate results.
Prevention, Mitigation, and Intervention Strategies
- Lim et al. Antibody responses after SARS-CoV-2 vaccination in lymphoma.external icon. medRxiv (Preprint; June 12, 2021). Published in The Lancet Haematologyexternal icon (July 2, 2021). Among 129 lymphoma patients vaccinated with BNT162b2 (Pfizer/BioNTech) or ChAdOx1 (Oxford/AstraZeneca), antibody titers were lower among patients “on treatment” (ongoing treatment or completed ≤ 6 months before vaccination) compared to “no treatment” (treatment-naive or completed therapy > 6 months before 1st dose). Among those on treatment, 61% did not have detectable antibodies after 2 doses.
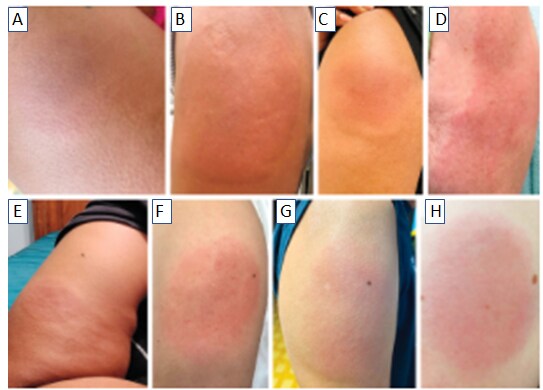
- Samarakoon et al. Delayed large local reactions to mRNA COVID-19 vaccines in Blacks, Indigenous Persons, and People of Color.external icon NEJM (June 9, 2021). Among 510 delayed large local reactions after mRNA vaccination reported to a COVID-19 vaccine allergy case registry between February 10 and April 23, 2021, 55 (11%) were in Black, Indigenous, or People of Color (BIPOC). Among BIPOC persons, mean time from vaccination until reaction was 8 days (range 4 to 14), and the majority of reactions occurred after 1st vaccine dose (53 [96%]) and after the mRNA-1273 (Moderna) vaccine (47 [85%]).
Note: Adapted from Samarakoon et al. Delayed large local reactions after 1st dose of the mRNA-1273 vaccine A) 41-year-old Black woman, B) 51-year-old Black woman, C) 44-year-old Black woman, D) 69-year-old woman of mixed race (Asian and White). Delayed large local reactions E) 41-year-old Black woman who had received the 1st dose of the BNT162b2 vaccine, F) 60-year-old Asian woman who had received the 1st dose of the mRNA-1273 vaccine, G) 73-year-old Asian man who had received the 2nd dose of the mRNA-1273 vaccine, H) 21-year-old Hispanic woman who had received the 1st dose of the mRNA-1273 vaccine. From the New England Journal of Medicine, Samarakoon et al., Delayed large local reactions to mRNA COVID-19 vaccines in Blacks, Indigenous Persons, and People of Color. June 9, 2021, online ahead of print. Copyright ©2021 Massachusetts Medical Society. Reprinted with permission from Massachusetts Medical Society.
- Stowe et al. Effectiveness of COVID-19 vaccines against hospital admission with the Delta (B.1.617.2) variant.external icon Knowledgehub (Preprint; June 14, 2021). Between April 12 and June 4, 2021 there were 14,019 symptomatic cases of SARS-CoV-2 B.1.617.2 variant with 166 hospitalizations in England. Vaccine effectiveness of 1 or 2 doses of BNT162b2 (Pfizer/BioNTech) or of 2 doses of ChAdOx1 (Oxford/AstraZeneca) against hospitalization with the B.1.617.2 variant was >90% and was comparable to effectiveness against hospitalization with the B.1.1.7 variant.
Social, Behavioral, and Communication Science
- Bothun et al. Poor readability of COVID-19 vaccine information for the general public: A lost opportunity.external icon medRxiv (Preprint; June 15, 2021). With 1 exception, the readability of EUA vaccine fact sheets (BNT162b2 (Pfizer/BionNTech), mRNA-1273 (Moderna), Ad26.COV2.S (Johnson & Johnson/Janssen)) and the CDC website on COVID-19 vaccines were judged as inadequately comprehensible to much of the US population. Only the V-Safe adverse event survey did not require comprehension at a 10th- to 12th-grade level when ranked by the Flesch Reading Ease Test, the Flesch-Kincaid Grade Level Test, and the Gunning-Fog Index. In 2003 nearly half US adults were estimated to read at <7th-grade level.
Disclaimer: The purpose of the CDC COVID-19 Science Update is to share public health articles with public health agencies and departments for informational and educational purposes. Materials listed in this Science Update are selected to provide awareness of relevant public health literature. A material’s inclusion and the material itself provided here in full or in part, does not necessarily represent the views of the U.S. Department of Health and Human Services or the CDC, nor does it necessarily imply endorsement of methods or findings. While much of the COVID-19 literature is open access or otherwise freely available, it is the responsibility of the third-party user to determine whether any intellectual property rights govern the use of materials in this Science Update prior to use or distribution. Findings are based on research available at the time of this publication and may be subject to change.