A Cautionary Tale: Pregnancy, Travel and Malaria

Street scene in Freetown, the capital of Sierra Leone. Travelers to Sierra Leone and other malaria-endemic areas should take precautions against acquiring this dangerous mosquito-borne disease. (Courtesy Doug Brooks)
In June 2005, Mariama Jones* was living in a comfortable house in Lawrenceville, Georgia, near Atlanta, with her husband Samuel, 10-year-old son Ahmed, and 2-year-old daughter Sonya. Ms. Jones had moved to Atlanta from her native Sierra Leone when she was 20, and in the 16 years that followed, she had built a productive and happy life for herself and her loved ones.
Ms. Jones, a nursing assistant at a local health-care facility, was 19 weeks pregnant. At her most recent check-up, her obstetrician had told her that the pregnancy was progressing well and that the baby was showing normal movements.
A Sudden Trip Abroad
Shortly after that promising report, a family crisis required Ms. Jones to travel to Sierra Leone as soon as possible. As a health-care provider and a native of Sierra Leone, she knew that this travel would expose her to malaria, a dangerous disease prevalent in most of Africa. Indeed, during a previous trip to Sierra Leone in 2001, Ms. Jones had taken antimalarial pills to protect herself against the disease.
In preparation for the 2005 trip, Ms. Jones visited a health-care provider to ask what precautions she should take for this trip, given her pregnancy. According to Ms. Jones, the health-care provider told her that because she was pregnant, there was no safe medication she could take to prevent malaria. Ms. Jones had her doubts about this, but with only three days left before her departure, and many other concerns on her mind, she failed to get a second opinion.
Ms. Jones was in Sierra Leone from June 9 to July 12, spending time in Freetown, the capital, and a smaller town called Small Makeni. During the trip she took no special precautions against malaria.
Back Home, Illness Sets In
Upon her return to Atlanta, Ms. Jones visited her obstetrician who examined her and said that everything was fine with the pregnancy. Ms. Jones went back to work, but after a couple of days, she felt tired and weak and noticed a changed taste in her mouth.
Within a week of her return from Africa, she developed a fever and chills and could not go to work. She suspected malaria and went to see her family doctor, who drew blood for a malaria test and prescribed an antibiotic while waiting for the lab results. During the next two days, her condition worsened. She lost her appetite but was extremely thirsty. She suffered from headaches and body aches and could no longer walk. It was then that she decided that she must go to a hospital.
Battling Malaria
In the emergency room, the doctors noted that Ms. Jones had a fever and a cough with some difficulty breathing, as well as nausea and vomiting. She was also weak and sleepy. Ms. Jones recalls that in the emergency room she passed dark red urine. Reassuringly, the doctors found good fetal heart tones.
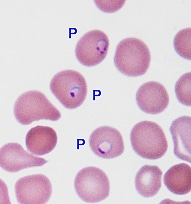
Blood smear taken from Ms. Jones in the emergency room and examined under the microscope, showing that many of the red blood cells are infected ("P") with the malaria parasite Plasmodium falciparum. (Copyrighted image used with permission)
Because of her symptoms and the history of recent travel to Africa, the doctors suspected malaria and ordered the necessary tests. Examination of Ms. Jones’ blood under the microscope (a “blood smear“) indeed confirmed their suspicion and Ms. Jones’ fears: she had malaria. The infection was due to Plasmodium falciparum, the malaria parasite most prevalent in Africa and one that can cause severe, even fatal disease. On the blood smear, up to 6 percent of her red blood cells were infected, indicating a rather severe episode.
Ms. Jones was admitted to the hospital and the doctors started treatment for malaria. They administered a combination of drugs used for malaria and known to be safe in pregnancy.
The doctors told her that they were concerned about the baby, because malaria can have harmful effects on pregnancies. During the next few days Ms. Jones remained very ill and weak, and her husband recalls that during that time she had periods of hallucinations. Three days after being admitted to the hospital, Ms. Jones was in the restroom when she passed out. Soon after, she had a miscarriage. Four days later, Ms. Jones’ condition had improved enough for the doctors to discharge her from the hospital.
Recovery and Reflection
Ms. Jones has now recovered her physical health. As part of her emotional recovery, she wishes to share her experience so that other people will not have to endure the same ordeal. “I want travelers to avoid malaria, especially if they are pregnant women!” she says earnestly.
Her concern is shared by Dr. Carlos Franco-Paredes, co-director of the TravelWell Clinic of Emory University in Atlanta.
“Travelers to malaria-endemic areas should take all necessary precautions,” says Dr. Franco-Paredes, who adds: “Pregnant women in particular are more susceptible than others to malaria. Malaria can increase the risk of negative outcomes such as premature delivery, miscarriage, and stillbirth. We recommend that pregnant women not travel to malaria-endemic areas. But if they must go, they absolutely should take antimalarial pills (mefloquine being the best choice currently) and avoid mosquito bites.”
Protect yourself against malaria
- All travelers to malaria-endemic areas should take precautions against this dangerous mosquito-borne disease.
- Pregnant women are at especially high risk; they should avoid traveling to malaria-endemic areas if at all possible.
- If a pregnant woman must travel to a malaria-endemic area, she should make sure to take all necessary precautions against malaria.
Footnotes
* The names of the patient and her family members have been changed. All other details are directly derived from interviews with actual persons and from review of medical records.

Dr. Carlos Franco-Paredes (TravelWell Clinic, Emory University) recommends extreme caution whenever pregnant women consider travel to a malaria-endemic area. (CDC photo)