 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Giardiasis Surveillance --- United States, 2003--2005Please note: An erratum has been published for this article. To view the erratum, please click here. Jonathan S. Yoder, MSW, MPH Corresponding author: Jonathan S. Yoder, MSW, MPH, Division of Parasitic Diseases, National Center for Zoonotic, Vector-Borne, and Enteric Diseases, CDC, 1600 Clifton Rd., N.E., MS F-22, Atlanta, GA 30333. Telephone: 770-488-3602; Fax: 770-488-7761; E-mail: jey9@cdc.gov. AbstractProblem/Condition: Giardiasis, a gastrointestinal illness, is caused by the protozoan parasite Giardia intestinalis. Reporting Period: 2003--2005. Description of System: State, commonwealth, territorial, and two metropolitan health departments voluntarily reported cases of giardiasis through CDC's National Notifiable Disease Surveillance System. Results: During 2003--2005, the total number of reported cases of giardiasis remained relatively stable. Reporting increased from 20,084 for 2003 to 20,962 for 2004 and then decreased to 20,075 for 2005. A total of 49 jurisdictions reported giardiasis cases; the number of areas reporting >15 cases per 100,000 population increased from four areas in 2003 to seven in 2005. Compared with other age groups, a greater number of case reports were received for children aged 1--9 years and for adults aged 30--39 years. Incidence of giardiasis was highest in northern states. Peak onset of illness occurred annually during early summer through early fall. Interpretation: Transmission of giardiasis occurs throughout the United States, with increased diagnosis or reporting occurring in northern states. State incidence figures should be compared with caution because individual state surveillance systems have varying capabilities to detect cases. The seasonal peak in age-specific case reports coincides with the summer recreational water season and might reflect increased outdoor activity and exposures such as use of communal swimming venues (e.g., lakes, rivers, swimming pools, and water parks) by young children. Public Health Action: Giardiasis surveillance provides data to educate public health practitioners and health-care providers about the epidemiologic characteristics and the disease burden of giardiasis in the United States. These data are used to improve reporting of cases, plan prevention efforts, and establish research priorities. IntroductionGiardia intestinalis (also known as G. lamblia and G. duodenalis) is the most common intestinal parasite identified by public health laboratories in the United States (1). This flagellated protozoan causes a generally self-limited clinical illness (i.e., giardiasis) typically characterized by diarrhea, abdominal cramps, bloating, weight loss, and malabsorption; asymptomatic infection also occurs frequently (2--4). Case reports indicate that giardiasis also might be associated with the development of reactive arthritis (5). In addition, giardiasis affects domestic and wild mammals (e.g., cats, dogs, cattle, deer, and beavers) (2). Giardia infection is transmitted by the fecal-oral route and results from the ingestion of Giardia cysts through the consumption of fecally contaminated food or water or through person-to-person (or, to a lesser extent, animal-to-person) transmission. The cysts are infectious immediately upon being excreted in feces. The infectious dose is low; ingestion of 10 cysts has been reported to cause infection (6). Infected persons have been reported to shed <108--109 cysts in their stool per day and to excrete cysts for months (6--8). Effective treatment alternatives are available for patients with symptomatic giardiasis, including metronidazole, nitazoxanide, tinidazole, paromomycin, furazolidone, and quinacrine. Persons at increased risk for infection include 1) travelers to disease-endemic areas, 2) children in child care settings, 3) close contacts of infected persons (e.g., those in the same family or household or in the child care setting), 4) persons who ingest contaminated drinking water, 5) persons who swallow contaminated recreational water (e.g., water in lakes, rivers, and pools), 6) persons taking part in outdoor activities (e.g., backpacking or camping) who consume unfiltered, untreated water or who fail to practice good hygienic behaviors (e.g., hand washing), 7) persons who have contact with infected animals, and 8) men who have sex with men (2,9--13), although giardiasis does not appear to be opportunistic in persons infected with human immunodeficiency virus. The relative contribution of person-to-person, animal-to-person, foodborne, and waterborne transmission to sporadic human giardiasis in the United States is unknown. Although giardiasis cases occur sporadically, outbreaks are well documented. During 1995--2004, Giardia was identified as a causal agent of five (3.7%) of 136 reported cases of recreational water-associated gastroenteritis outbreaks and of 14 (13%) of 108 reported cases of drinking water-associated gastroenteritis outbreaks (14--20). In addition, foodborne outbreaks of giardiasis linked to infected foodhandlers and to uninfected foodhandlers who diapered infected children prior to handling food have been reported (21). Outbreaks resulting from person-to-person transmission in child care centers also have been reported (22). Communitywide outbreaks might be waterborne initially but spread subsequently through the community by person-to-person transmission (23). Few direct animal-to-human outbreaks have been documented although linkages have been identified between canine and human transmission (24). In addition, animal contamination of water (e.g., an infected dead beaver in a water system intake) has been associated with drinking water outbreaks (25). However, the zoonotic transmission of giardiasis is not believed to play a major role in human disease (26). In 1992, the Council of State and Territorial Epidemiologists assigned an event code for giardiasis (code 11570) to facilitate transmission of reported giardiasis data to CDC. Surveillance data for 1992--2002 have been published previously (27,28). Reporting of giardiasis as a nationally notifiable disease began in 2002. This report summarizes national giardiasis surveillance data for 2003--2005. MethodsA confirmed case of giardiasis in humans is one that has a positive laboratory finding. Confirmed and probable cases of giardiasis are reported voluntarily to CDC. Confirmed giardiasis is defined as the detection (in symptomatic or asymptomatic persons) of Giardia intestinalis
A probable case of giardiasis is a clinically compatible case that is linked epidemiologically to a confirmed case (29). Because Giardia cysts can be excreted intermittently, multiple stool collections (i.e., three stool specimens collected every other day) increase test sensitivity (30). The use of concentration methods and trichrome staining might not be sufficient to demonstrate Giardia because variability in the concentration of organisms in the stool can make this infection difficult to diagnose. For that reason, fecal immunoassays with greater sensitivities and specificities are available. DFA is extremely sensitive and specific (31). Rapid immunochromatographic cartridge assays also are available and are useful for diagnosing Giardia infections, but they do not take the place of routine ova and parasite examination. Health departments in the 50 states, the District of Columbia (DC), New York City (NYC), the Commonwealth of Puerto Rico, and Guam voluntarily report laboratory-confirmed and probable cases of giardiasis to CDC through the Nationally Notifiable Disease Surveillance System (NNDSS). Reports include the patient's place of residence (i.e., state and county), age, sex, race, ethnicity (i.e., Hispanic or non-Hispanic), and date of illness onset and indicate whether the case is linked epidemiologically to a known outbreak. An outbreak-related case is a case that is linked epidemiologically to at least one laboratory-confirmed case. Before analysis, data were verified for accuracy by the reporting jurisdiction and finalized as of February 16, 2007. For this reason, the number of cases provided in this report might differ slightly from the number published in CDC's annual Summary of Notifiable Diseases. Analysis of the national giardiasis surveillance data for 2003--2005 was conducted using SAS® v.9.1 (SAS Institute, Inc.; Cary, North Carolina) and the Food Safety Information Link (FSI Link). FSI Link is an intranet-based tool available to CDC staff that provides access to NNDSS data and is used to monitor trends in and investigate outbreaks of reportable foodborne and waterborne diseases. Population data from the U.S. Census Bureau were used to calculate incidence rates. ResultsDuring 2003--2005, the total number of reported cases of giardiasis remained relatively stable. Case reports increased 4.4% from 20,084 for 2003 to 20,962 for 2004 and then decreased 4.2% to 20,075 for 2005 (Table 1). Cases reported to be outbreak related made up 1.1%--2.6% of the total number of cases reported annually for 2003--2005. During this period, 49 jurisdictions reported giardiasis cases; the number of jurisdictions reporting >15 cases per 100,000 population increased from four in 2003 to seven in 2005. For 2005, among jurisdictions reporting outbreaks, incidence of giardiasis per 100,000 population ranged from 1.4 cases in Louisiana to 30 cases in Vermont. Two states (Vermont and Minnesota) reported the greatest number of cases per 100,000 population for each of the 3 years of the reporting period. Northern states reported more cases annually per 100,000 population than southern states (Figure 1; Table 1). These surveillance data display a bimodal age distribution, with the greatest number of reported cases occurring among children aged 1--4 and 5--9 years and adults aged 35--44 years (Figure 2). When reports for which a patient's sex was missing or unknown are excluded, the percentage of cases reported to have occurred among males varied annually from 55.0% (9,694 of 17,624) for 2003 to 55.9% (11,542 of 20,641) for 2004. A twofold increase in reported giardiasis cases by onset of illness occurred during June--October compared with January--March (Figure 3). Age-specific analysis indicated a twofold increase in onset of illness during June--October among all age groups. The highest numbers of giardiasis cases were reported among children aged 1--4 and 5--9 years and adults aged 35--39 years (Figure 4). The majority of cases for which data on race were available for 2003--2005 occurred among whites, followed by blacks, Asians/Pacific Islanders, and Native Americans/Alaska Natives (Table 2). However, data on race were not included for 40.1%-- 48.7% of total annual case reports. Although 13.7%--15.0% of patients for whom data on ethnicity were reported were identified as Hispanic, data on ethnicity were lacking for 47.8%--57.2% of total annual case reports. DiscussionNational giardiasis surveillance data are used to assess the epidemiologic characteristics and disease burden of giardiasis in the United States. During 2003--2005, the total number of cases reported remained relatively stable, with a slight increase during 2003--2004 and a slight decrease during 2004--2005. However, following a gradual decline in case reports during 1996--2001 (27,28), the number of case reports appears to have stabilized thereafter, coinciding with the disease becoming nationally notifiable in 2002 (Figure 5). The reason for this gradual decline is unknown. Giardiasis is widespread geographically in the United States. These data and data from previous national giardiasis surveillance summaries (27,28) indicate that the diagnosis or transmission of giardiasis might be higher in northern states (Figure 1). However, because differences in giardiasis surveillance systems among states can affect the capability to detect cases, whether this finding is of true biologic significance or is only the result of differences in case detection or reporting is difficult to determine. Although giardiasis affects persons in all age groups, the number of reported cases was highest among children aged 1--9 years and adults aged 35--44 years. These data for younger age groups are consistent with reports published previously of giardiasis incidence being higher among younger children as well as contributing to transmission to their caregivers (e.g., day care staff, family members, and other household contacts) (2,27,28,32,33). A multicenter study identified Giardia as the cause of diarrhea in 15% of nondysenteric children examined in outpatient clinics (34). Investigation of a giardiasis outbreak in a day care facility determined that 47% of ill children transmitted the infection to more than one household contact (35). A marked seasonality in the onset of illness occurs in early summer through early fall. A twofold increase in transmission of giardiasis occurred during the summer, coinciding with increased outdoor activities (e.g., swimming and camping). This increase might reflect increased use of community swimming (essentially communal bathing) venues by younger children. In addition to animal contamination of surface water, transmission through use of surface water (e.g., lakes and rivers) and disinfected venues (e.g., swimming pools and water parks) is facilitated by the substantial number of Giardia cysts that can be shed by a single person (7); the extended periods of time that cysts can be shed (8); the low infectious dose (6); the moderate resistance to chlorine of Giardia (36); the prevalence of improper pool maintenance (i.e., insufficient disinfection, filtration, and recirculation of water), particularly of children's wading pools (37); the prevalence of Giardia in fecal material in pools (38); and documented transmission of Giardia infection among diapered children (22,34,35,39) who use swimming venues regularly. This seasonal variation also has been noted in state, Canadian provincial, and previous U.S. national surveillance data for giardiasis and as for cryptosporidiosis (27,28,32,33). The importance of water and food in the transmission of Giardia is highlighted by recent giardiasis outbreaks. In 2003, a communitywide outbreak of giardiasis in Massachusetts was traced to use of a wading pool at a membership club (23). In addition to the 30 case-patients with primary exposures to the pool, an additional 105 cases were caused by secondary person-to-person transmission. Also in 2003, a communitywide outbreak in Iowa implicated a wading pool at a day care center that was filled with water from the municipal water supply (14). From the child care center, illness spread into the community via secondary transmission, sickening an estimated 100 persons with giardiasis, cryptosporidiosis, or both. In 2004, a drinking water-associated outbreak in Ohio that sickened 1,450 persons was caused by multiple pathogens, including Giardia (42). Contamination of noncommunity public and private wells with sewage led to this communitywide outbreak. Foodborne outbreaks associated with ice, vegetables, and chicken salad also were reported in 2004 and 2005 (43). Among patients for whom data on sex were reported, a majority of cases occurred among males. This sex-related difference might be attributable in part to sexual contact among men who have sex with men (11). However, the majority of cases occurred in males in nearly every age group (except those aged <1 year and >59 years), which suggests the influence of other factors (Table 2). Because data on race and ethnicity are incomplete, conclusions cannot be made regarding the differences noted in the epidemiology of giardiasis among members of different racial and ethnic populations. The data reported likely underestimate the giardiasis burden in the United States. Giardiasis is highly underreported because 1) not all infected persons are symptomatic, 2) those who are symptomatic do not always seek medical care (44,45), 3) health-care providers do not always include laboratory diagnostics in their evaluation of nonbloody diarrheal diseases (44), and 4) case reports are not always completed for positive laboratory results or forwarded to public health officials (46). Although the true burden of cryptosporidiosis in the United States is unknown, an estimated 2 million cases occur annually (46). Its low infectious dose, protracted communicability, and moderate chlorine resistance make Giardia ideally suited for transmission through drinking and recreational water, food, and person-to-person contact. Strategies to reduce the incidence of giardiasis have focused on reducing waterborne and person-to-person transmission. In response to parasitic drinking water outbreaks related to treated surface water, the Environmental Protection Agency (EPA) enacted the Surface Water Treatment Rule (SWTR) and the Interim Enhanced SWTR (15). These regulations have decreased the number of giardiasis outbreaks associated with community drinking water systems (15,17--20). In 2006, EPA finalized the Ground Water Rule to address contamination of public ground water (well) systems, which is likely to reduce the number of groundwater-associated outbreaks of giardiasis. Person-to-person transmission of Giardia is difficult to interrupt in a systematic fashion, particularly in day care settings (47). Adherence to appropriate infection control (e.g., hand washing, diaper changing, and separation of ill children) policies is recommended for controlling giardiasis, and other enteric pathogens, in group settings such as daycares (48). Prevention measures (Box 1) and measures to improve surveillance for giardiasis and increase understanding of its epidemiology and the associated disease burden (Box 2) have been recommended. General information about giardiasis is available from CDC at http://www.cdc.gov/ncidod/dpd/parasites/giardiasis/factsht_giardia.htm. Acknowledgments Giardiasis data were reported to CDC by jurisdiction surveillance coordinators. Ruth Ann Jajosky, DMD, and Roland Richard, MPH, National Center for Public Health Informatics, CDC, facilitated access to the data and assisted with the analysis. Technical assistance was provided by Michele Hlavsa, MPH, Stephanie Johnston, MS, and John Williamson, ScD, Division of Parasitic Diseases, National Center for Zoonotic, Vector-Borne, and Enteric Diseases, CDC. References
Table 1 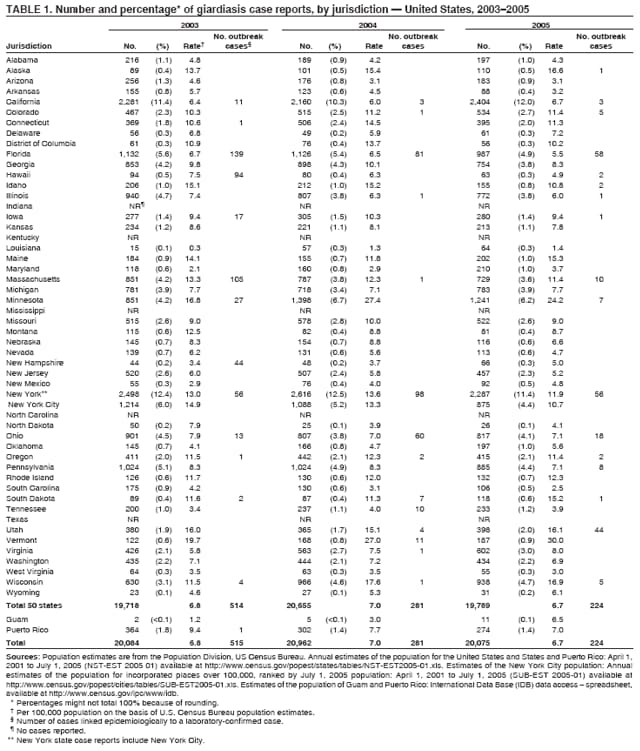 Return to top. Figure 1 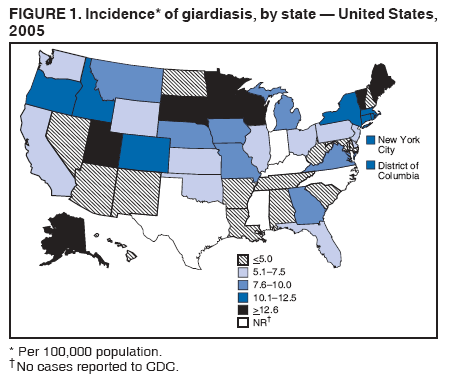 Return to top. Box 1  Return to top. Table 2 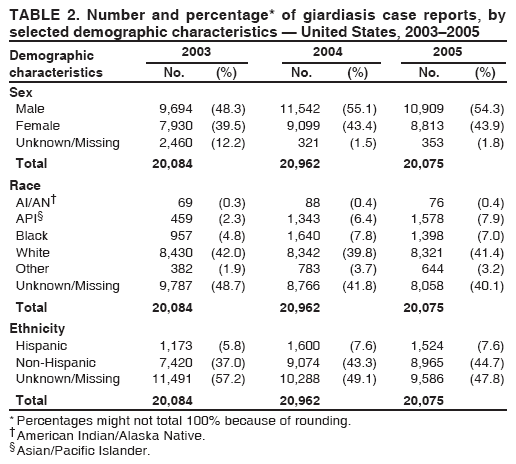 Return to top. Figure 2 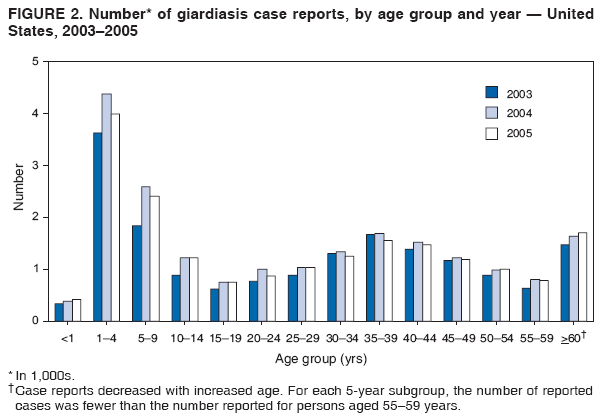 Return to top. Box 2  Return to top. Figure 3 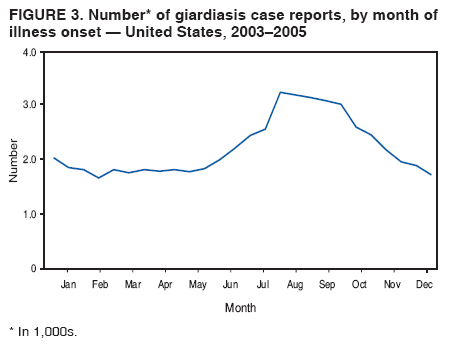 Return to top. Figure 4 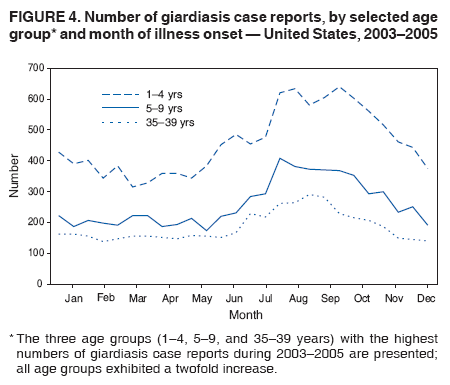 Return to top. Figure 5 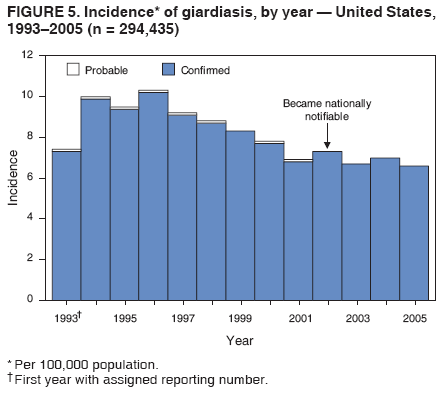 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Date last reviewed: 8/20/2007 |
|||||||||
|