

|

|

Volume 4: No.
4, October 2007
ORIGINAL RESEARCH
Church-Based Breast Cancer Screening Education: Impact of Two Approaches on Latinas Enrolled in Public and Private Health Insurance Plans
Angela Sauaia, MD, PhD, Sung-joon Min, PhD, David Lack, Cecilia Apodaca, Diego Osuna, MD, Angela Stowe, Gretchen F. McGinnis, Lisa M. Latts, MD, MSPH, MBA, Tim Byers, MD, MPH
Suggested citation for this article: Sauaia A, Min S, Lack D, Apodaca C, Osuna D, Stowe A, et al. Church-based breast cancer screening education: impact of two approaches on Latinas enrolled in public and private health insurance plans. Prev Chronic Dis 2007;4(4).
http://www.cdc.gov/pcd/issues/2007/
oct/06_0150.htm.
Accessed [date].
PEER REVIEWED
Abstract
Introduction
The Tepeyac Project is a church-based health promotion project that was conducted from 1999 through 2005 to increase breast cancer screening rates among Latinas in Colorado. Previous reports evaluated the project among Medicare and Medicaid enrollees in the state. In this report, we evaluate the program among enrollees in the state’s five major insurance plans.
Methods
We compared the Tepeyac Project’s two interventions: the Printed Intervention and the Promotora Intervention. In the first, we mailed culturally tailored education packages to 209 Colorado Catholic churches for their use. In the second, promotoras (peer counselors) in four Catholic churches delivered breast-health education messages personally. We compared biennial
mammogram claims from the five insurance plans in the analysis at baseline (1998–1999) and during follow-up (2000–2001) for Latinas who had received the interventions. We used generalized estimating equations (GEE) analysis to adjust rates for confounders.
Results
The mammogram rate for Latinas in the Printed Intervention remained the same from baseline to follow-up (58%
[2979/5130] vs 58% [3338/5708]). In the Promotora Intervention, the rate was 59% (316/536) at baseline and 61% (359/590) at follow-up. Rates increased modestly over time and varied widely by insurance type. After adjusting for age, income, urban versus rural location,
disability, and insurance type, we found that women exposed to the Promotora Intervention had a significantly higher increase in biennial mammograms than did women exposed to the Printed Intervention (GEE parameter estimate = .24
[±.11], P = .03).
Conclusion
For insured Latinas, personally delivering church-based education through peer counselors appears to be a better breast-health promotion method than mailing printed educational materials to churches.
Back to top
Introduction
Disparities in breast cancer screening rates among Latinas have persisted for the past decade (1-4). Difficulty in accessing preventive care is highly prevalent among Latinas, but studies show that even insured Latinas, who have access, resist screening mammography because of cultural barriers such as fear, embarrassment, and a sense of fatalism (5-7). Culturally sensitive, church-based health
promotion and programs using peer counselors have shown promising results among Latinos (8-14) and may be helpful in increasing breast cancer screening among Latinas.
This report is the third in a series that examines the impact of the Tepeyac Project, a 6-year health quality improvement project that began in 1999 with the aim of increasing breast cancer screening awareness among Latinas in Colorado. The project, which compares the effectiveness of printed breast-health education with personally delivered education, takes its name from Tepeyac, Mexico, the
site revered by Latinos as the place where Our Lady of Guadalupe appeared to Saint Juan Diego, and from the community-based clinic that was a close partner in the project, Clínica Tepeyac.
The project’s first report focused on Medicare enrollees receiving the interventions; the second addressed Medicaid enrollees (15,16). In both insurance groups, personally delivered education seemed to be more effective than printed educational materials (15,16). Our report expands the evaluation to include enrollees in Colorado’s five major private and public insurance plans. This
comprehensive analysis allowed us to compare the effectiveness of the two interventions among the majority of insured Colorado Latinas.
Back to top
Methods
The Tepeyac Project was conducted from 1999 through 2005 and used a community-participatory approach in which local Latinas identified four main themes that would affect the success of an effort to increase breast cancer screening in the community: the importance of family, Latinos’ sense of fatalism, the need for trust, and the need for personal delivery by a trusted messenger (15).
These issues guided development of the two interventions compared in the project. In the first, the Printed Intervention, we mailed culturally tailored breast-health promotion packages to Catholic churches across the state. In the second, the Promotora Intervention, we trained peer counselors (promotoras) to deliver the health promotion message personally, on a one-to-one basis.
We delivered the interventions through churches because they are an integral part of Latinos’ social network (17). Local Latinas assisted in choosing the program message and brochures and in developing messages addressing barriers to breast cancer screening for their church bulletins and for the project newsletter. Periodically, we shared evaluations of mammogram rates with participating
churches to keep the community informed, to encourage participation, and to allow people to monitor the intervention in their regions. The study was approved by the Colorado Multiple Institutional Board (Protocol number 02-973).
Implementation of interventions
Printed Intervention
The materials used in this intervention included 1) a letter describing the project, 2) bilingual printed materials from the National Cancer Institute that promote breast cancer screening and reflect a sense of family (“Do it for you. Do it for your family.”), 3) a display unit, 4) short bilingual messages suitable for delivery from the pulpit
and coordinating camera-ready copy for publication in church bulletins, and 5) a fax-back form asking at which level churches would participate (i.e., display materials, publish messages, deliver messages from pulpit).
The three Catholic archdioceses in Colorado approved the project and contacted the churches in their registries, encouraging their participation. We sent the printed intervention package to 209 churches in the registries. The first mailing occurred in March 2000, a second in October 2000, and a third in February 2001. The second and third mailings included issues of the project newsletter
containing updates and mammogram rates for the regions. We included all 209 churches that received the Printed Intervention in an intention-to-treat analysis.
Information about the level of church participation, evaluated by personal telephone calls and fax-back forms in 2001, was available for 150 (72%) churches in the Printed Intervention. Of these churches, 61 (41%) displayed the printed materials, 8 (5%) published messages in the bulletin, and 85 (57%) did both; 18 (12%) also made pulpit announcements. The participation level was undetermined in
47 churches, and 12 declined to participate. A second round of telephone contacts in 2004, during the second phase of the project, indicated that participation had increased by approximately 20%, with 177 churches reporting active participation.
Promotora Intervention
In the Promotora Intervention, women recruited and trained by project and Clínica Tepeyac staff delivered education about breast cancer screening in person. As the base for this intervention, Clínica Tepeyac staff chose four churches in the Denver area that had large Latino populations and were close to the clinic and to
the promotoras’ residences. The priests of these churches enthusiastically supported the intervention.
The promotoras reached their peers through meetings held at least bimonthly immediately after mass and through other church events. During the intervention, a respected leader chosen by the promotoras, Sister Lydia Peña, delivered homilies addressing women’s breast health at least twice in each of the four churches, in English or Spanish, depending on the language of
the mass. Promotoras also conducted one to three health groups per church. These groups were for women only and met at the home of one of the participants. The same newsletter used in the Printed Intervention was made available to these churches. The intervention began in 2000 and continued until 2005, when the second phase of the project ended.
Study population and insurance plans
We received data on enrollment and mammogram claims for women aged 50 to 69 years from Medicare Fee-for-Service (FFS), Medicaid FFS, and the following health maintenance organizations (HMOs): Kaiser Permanente of Colorado (a staff-model HMO
[i.e., HMO with its own clinic and staff]), Access (the major Medicaid HMO provider in Colorado), and Anthem Blue Cross and Blue Shield (all group-model HMOs
[i.e., HMO contracting with a group medical practice]). To merge administrative data from
these multiple payers, we used standardized variables and created specific record linkage variables to allow for cross-checking of Medicare FFS and Medicaid FFS datasets to identify dually eligible subjects (18,19). The HMO plans’ datasets included their Medicare and Medicaid enrollees. Medicaid FFS subjects enrolled in a primary care case management (PCCM) program, which is reimbursed by
Medicaid FFS, were included in the Medicaid FFS database.
We identified Latinas in the enrollment databases of the insurance groups through the race and ethnicity data field of the two insurance groups for which these data were available (Medicaid FFS, Medicare FFS) combined with the Passel-Word
Spanish Surname List (20). In Colorado, this list has a 12% ±.3% commission rate and a 22% ±.4% omission rate, both comparable to rates for the
United States as a whole. To be included, women had to 1) be aged 50 to 69 years (the group with the strongest evidence of benefit from screening mammograms [21]), 2) be continuously enrolled in the plan for longer than 23 months with a gap in coverage of no longer than 30 days (to obtain completely independent records by excluding individuals who might have appeared in more than one enrollment
dataset), and 3) have survived the entire baseline or follow-up period (but not necessarily both).
We used zip codes to determine exposure to the interventions. Study subjects living in the zip codes of the churches visited by the promotoras during 2000 and 2001, the time of the first phase of the interventions and the follow-up period for our analysis, were considered exposed to the Promotora Intervention; subjects living in the remaining zip codes
were considered exposed to the Printed Intervention.
Reasons for enrollment in Medicaid were 1) receipt of a pension (for people aged 60 to 64 years); 2) disability or blindness (a small number of refugees were included in this group because of similar mammogram screening rates); and 3) receipt of benefits from Aid to Families with Dependent Children. Reasons for enrollment in Medicare were being aged 65 years or older, having end-stage renal
disease (ESRD), and having a disability. In Colorado in 2000, approximately 70% of Medicare enrollees were enrolled in FFS
plans; the remaining 30% were in Medicare HMO plans (22,23). Eighty-eight
percent of Medicaid enrollees were enrolled in managed care, with the remainder
enrolled in Medicaid's FFS plans (24,25).
Mammogram rates
We considered claims with any of the following codes to represent mammogram use: International Classification of Diseases, Ninth Revision, Clinical Modification
(ICD-9-CM) (www.cdc.gov/nchs/icd9.htm) procedure codes 87.36, 87.37, or diagnostic code V76.1x; Healthcare Common Procedure Coding System codes GO202, GO203, GO204, GO205, GO206, or GO207; Current Procedural
Terminology (www.ama-assn.org *) codes 76085, 76090, 76091, or 76092; and revenue center codes 0401, 0403, 0320, or 0400 in conjunction with breast-related ICD-9-CM diagnostic codes 174.x, 198.81, 217, 233.0, 238.3, 239.3, 610.0, 610.1, 611.72, 793.8, V10.3, V76.1x.
Statistical analysis
We compared the rates of mammogram screening obtained for the baseline period before the intervention (January 1998 through December 1999) with those for the follow-up period used in our analysis (January 2000 through December 2001) for Latinas living in each of the intervention areas.
The outcome variable was the biennial mammography screening status in each study period, as determined by the codes cited above. The main effect variable was the intervention, and the covariates were age, insurance type, two measures of income (median family income from United States Census 2000
[www.census.gov] and Medicare-Medicaid dual eligibility status), urban versus rural
residence, and disability. We included disability as a variable because the Medicare FFS dataset contained a large proportion (49%) of Latinas aged 50 to 64 years with disability and ESRD as reasons for coverage. To determine rural or urban residence, we linked the patient’s zip code to the Rural Urban Commuting Area (RUCA) codes using the
RUCA Zip Code Approximation, and the
suggested binary categorization (categorization C) (26).
We used the chi-square test and the Fisher exact test (for cells with expected values <5) to compare categorical variables and analysis of variance (ANOVA) for continuous variables (with the Welch modification when the assumption of similar variances did not hold) (27). For multivariate modeling, we used generalized estimating equations (GEE) analysis, a statistical technique appropriate
for binary variables that allows for testing several covariance structures. GEE analysis accounts for correlations between baseline and follow-up samples (as a consequence of having some subjects present in both time periods), while accommodating unequal group sizes, as was the case in this project (28,29).
The hypothesis for the GEE model was that among Latinas, the Promotora Intervention was associated with a larger increase in mammogram rates over time than was the Printed Intervention, irrespective of insurance group. We used the following GEE statistical model to test this hypothesis:
Logit P = α + β1time (follow-up vs baseline) + β2intervention (PI vs PSI) + β3(time*intervention) + β4…n(covariates),
where P is the probability of having a mammogram, α is the intercept, β1 is the parameter estimate for time (baseline vs follow-up), β2 is the parameter estimate for the intervention (Promotora Intervention vs Printed Intervention), β3 is the parameter estimate for the interaction between time and intervention, and β4 is the parameter estimate(s) for the
covariates.
We also analyzed the subgroup of 4739 Latinas (56% of the total of 8439 individuals, with 11,964 observations included in the GEE analysis) who were present during both baseline and follow-up.
Back to top
Results
Study subjects
Latinas represented approximately 11% of the total population of eligible women (Latinas can be of any race; 90% were white). The distribution of insurance type was significantly different between Latinas in the Promotora Intervention and
in the Printed Intervention during baseline and follow-up
(Table 1). The staff-model HMO had the largest population, serving half of the Latinas receiving the
Promotora Intervention and about one-third of those receiving the Printed Intervention. Over time, the distribution of insurance type remained stable among women receiving the Promotora Intervention. Among women receiving the Printed Intervention, however, the proportion of enrollees in HMO plans increased and the proportion in public FFS plans decreased. Latinas receiving the
Promotora Intervention were younger and poorer than those receiving the Printed Intervention, and these differences were stable over time.
Mammogram rates
Overall, unadjusted mammogram rates did not change significantly in either intervention group (Promotora Intervention, unadjusted GEE, P = .15; Printed Intervention, unadjusted GEE, P = .68) (Figure). We used the GEE model to adjust the effect of the intervention on mammogram rates among Latinas by insurance group, age, income, rural
versus urban location, and disability. The significant positive interaction term between time and intervention suggests that the Promotora Intervention was more effective than the Printed Intervention in increasing mammogram screening among Latinas from baseline to follow-up and that this effect was independent of age, income, urban location, and insurance group
(Table 2).
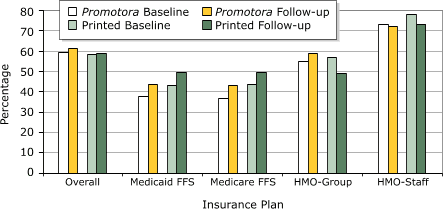
Figure. Biennial mammogram rates of Latinas exposed to the Printed Intervention or the Promotora Intervention during baseline (1998–1999) and follow-up (2000–2001), by insurance plan, Tepeyac Project, Colorado, 1999–2005.
(FFS indicates fee-for-service; HMO-Group, health maintenance organization
contracting with a group medical practice; HMO-Staff, health maintenance
organization with its own clinic and staff.) [A tabular version of this graph is also available.]
Other factors associated with not obtaining mammograms were being age 65 years or older (marginally significant),
having lower income, and having disability (Table 2). After adjustment for other variables, insurance type was a significant factor, with Latinas enrolled in Medicare FFS being less likely to obtain mammograms than were their HMO counterparts and more likely than were Latinas with Medicaid FFS. The
adjusted differences in mammogram rates between HMOs and Medicare FFS decreased significantly over time, as indicated by the significant negative interaction between time and insurance type.
The GEE model including only enrollees who were present in both periods of time produced very similar results (data not shown in table), with a significant positive interaction term between time and intervention (GEE parameter estimate = .2911
[± .1218], P = .02), suggesting that in this subset of women, the Promotora Intervention was also associated with a larger increase over
time in mammogram rates than was the Printed Intervention, independent of age, income, rural location, disability, and insurance group.
Back to top
Discussion
Culturally appropriate health promotion specific to the needs and barriers affecting Latinas is necessary if health disparities are to be eliminated. The Tepeyac Project was based in churches because studies show that they represent a safe and convenient place for Latinas to gather for health education (9,13-17,30-33). Our question was whether receiving culturally tailored information through
this trusted environment was sufficient or whether a personal connection was necessary to move Latinas into action. The promotoras, well-trusted women in their communities, provided this personal component by engaging women on a one-on-one basis, tailoring the education to the individual needs and learning styles of each woman.
The previous evaluations on Medicare FFS and Medicaid FFS suggested that the personally delivered education was more effective than the mailed intervention package (Printed Intervention) (15,16). The present analysis expanded the evaluation to the most important insurance types in Colorado (public and private). The Promotora Intervention seemed to be more effective than the Printed
Intervention, independent of insurance type, age, location (urban vs rural), and income.
Overall, the changes in mammogram rates were quite modest. One explanation
might be that our interventions did not fully address the cultural factors involved in lower screening rates among Latinas or that the process requires more time to determine a behavioral change. Alternatively, the cultural components that our interventions try to address
may represent only a small fraction of the
causes of lower screening rates. Our experience working closely with the communities we were serving indicated that factors such as financial constraints that limit the ability to afford time off work, transportation, child care, copayments, and other issues involved in obtaining mammograms may play a more important role than education.
Merging administrative data from different insurance plans to provide objective outcomes for evaluation gave a comprehensive portrait of mammography rates among insured Latinas in the state and was a strength of this study. The
National Institutes of Health and the Agency for Healthcare Research and
Quality recognize the need for datasets from multiple payers in cancer research (34). This
approach presents challenges, however. Competing payers must collaborate in providing their claims and enrollment data.
Combining their individual datasets into one dataset without including duplicate patient records requires verification of data integrity, standardization of variables across plans, and the creation of record linkage variables to cross-check datasets for
duplicates and to identify individuals who were dually eligible for Medicare and Medicaid.
Working with nontraditional partners, such as churches and community-based clinics, and using a community-participatory approach were
somewhat new to the state’s Health Care Quality Improvement Program and represented another challenge. The Promotora Intervention requires that project staff stay in close personal contact with the community, partners, and the promotoras
to forge a trusting relationship. These partners, for whom health promotion is not the primary mission, however, have their own timing and priorities, all of which must be respected.
Another issue is that mammogram rates calculated from claims data seem to be consistently lower than those calculated from self-reported data. Widely cited self-reported data from the Behavioral Risk Factor Surveillance System and the National Health Interview Study suggest that 70% to 80% of women aged 65 to 69 years receive at least biennial screening (1,3,4).
Several groups, however, suggest that studies based on self-reported data may
overstate screening rates (35). The Colorado Mammography Project reports that the sensitivity of Medicare FFS billing data for screening mammography in Colorado was 85% and varied substantially by age, race, and socioeconomic status (36). A further complicating factor that particularly affects
Latinas and Asian-American women in studies using billing data is the low sensitivity of these data in identifying ethnicity (35,37). Using linked data from the Medicare Current Beneficiary Survey, Arday et al (37) assessed the accuracy of racial and ethnic classifications in the Centers for Medicare and Medicaid Services enrollment database before and after the 1997 effort to update the database. After the update,
sensitivity was 97% for whites and 95% for blacks but less than 60% for all other categories. The positive predictive value was higher than 96% for whites, blacks, and Latinos but lower than 80% for all others.
A limitation of our study is that although the interventions were based in churches, outcomes were measured in neighborhoods, with the assumption that a church intervention will diffuse into the community. Using zip codes to determine exposure to the interventions admittedly makes the study vulnerable to ecological fallacy; however, most churches do not release parishioners’ individual data
because of trust issues. In fact, the promotoras were adamantly against even asking for zip codes because any information request could result in distrust of the intervention. Furthermore, data from parish registries are unreliable because Latinos are less likely than whites to register (38). According to the Archdiocese of Denver’s Hispanic Ministry, however, a large proportion of
Latinos now attend their neighborhood churches (i.e., in the zip codes where they live) because of a recent increase in the number of churches offering masses in Spanish.
Because this was a pilot project, financial and feasibility constraints limited to four the number of churches in the Promotora Intervention. The fact that the churches were not randomly chosen, but were selected by our community-based partner and the promotoras, presents a potential selection bias. We do not, however, anticipate that the women exposed to the personal education
were inherently more likely to obtain mammograms than were parishioners of the other churches. Unfortunately, we had to exclude uninsured women because of the lack of a denominator for computation. Even so, the data clearly indicate that insured Latinas represent a large group still requiring much effort in breast-health promotion.
Our results suggest, rather than provide firm evidence, that the Promotora Intervention is more effective than the Printed Intervention in increasing breast cancer screening rates among Latinas. The scientific rigor needed to prove causation, however, may be difficult to achieve in this type of project. Using pure control groups poses an ethical dilemma for community-participatory
projects such as ours, in which the community’s will, although not necessarily in line with academic standards, is paramount. Methods to obtain more detailed data, such as surveys, require large samples of ethnic minorities and special resources (e.g., trained bilingual surveyors) and, thus, sizeable funding (39). Furthermore, surveys are subject to limitations and biases among Latinos,
whose addresses and telephone numbers often change and who may feel uncomfortable providing personal information, including race and ethnicity, to unfamiliar people (39). Although randomized clinical trials are the paradigm of scientific evidence, community-participatory research projects may require a scientific model of their own.
Back to top
Acknowledgments
Drs Sauaia and Min had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. The datasets used in the analysis were generously made available by the following institutions: Colorado Department of Health Care Policy and Financing (Medicaid FFS),
Colorado Access, Anthem Blue Cross Blue Shield of Colorado, Kaiser Permanente of
Colorado, and the Colorado Foundation for Medical Care. Dr Sauaia’s work was supported by a grant from the National Cancer Institute (1RO3CA110820-01).
The Medicare FFS analyses on which this publication is based were performed under Contract Nos. 500-99-CO-01 and 500-02-CO-01, entitled
“Utilization and Quality Control Quality Improvement Organization for the State of Colorado,” sponsored by the Centers for Medicare and Medicaid Services, Department of Health and Human Services. The content of this publication does not necessarily
reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products, or organizations imply endorsement by the U.S. Government. The
lead author assumes full responsibility for the accuracy and completeness of the ideas presented. This article is a direct result of the Health Care Quality Improvement Program initiated by the Centers for
Medicare and Medicaid Services, which has encouraged identification of quality improvement projects derived from analysis of patterns of care, and therefore required no special funding on the part of this
contractor. Ideas and contributions to the author concerning experience in engaging with issues presented are welcomed.
Back to top
Author Information
Corresponding Author: Angela Sauaia, MD, PhD, Associate Professor, Department of Medicine, Division of Health Care Policy and Research, University of Colorado Health Sciences Center, 13611 East Colfax Ave, Ste 100, Aurora, CO 80011. Telephone: 303-724-2498. E-mail: Angela.Sauaia@UCHSC.edu.
Author Affiliations: Sung-joon Min, Tim Byers, University of Colorado Health Sciences Center, Denver, Colorado; David Lack, Cecilia Apodaca, Clínica Tepeyac,
Denver, Colorado; Diego Osuna, Kaiser Permanente of Colorado, Arvada, Colorado, Aurora Centrepoint Medical Offices, Aurora, Colorado,
and University of Colorado Health Sciences Center, Denver, Colorado; Angela Stowe, Colorado Foundation for Medical Care, Englewood, Colorado; Gretchen F. McGinnis,
Colorado Access, Denver, Colorado; Lisa M. Latts, Anthem Blue Cross Blue Shield, Denver, Colorado.
Back to top
References
- National health care disparities report, 2004. Rockville (MD): U.S.
Department of Health and Human Services, Agency for Healthcare Research and Quality; 2005. http://www.ahrq.gov/qual/nhdr04/nhdr04.htm
- Hsia J, Kemper E, Kiefe C, Zapka J, Sofaer S, Pettinger M, et al.
The importance of health insurance as a determinant of cancer screening: evidence from the Women's Health Initiative. Prev Med 2000;31(3):261-70.
- Behavioral Risk Factor Surveillance System survey data. Atlanta (GA): Centers for Disease Control and Prevention, U.S. Department of Health and Human Services;
1995-2001.
http://www.cdc.gov/brfss/technical_infodata/surveydata.htm
- Health: United States, 2002. With chartbook on trends in the health of Americans. Atlanta (GA): U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics; 2002. http://www.cdc.gov/nchs/data/hus/hus02.pdf
- Thompson B, Coronado GD, Solomon CC, McClerran DF, Neuhouser ML, Feng Z.
Cancer prevention behaviors and socioeconomic status among Hispanic and non-Hispanic whites in a rural population in the United States. Cancer Causes Control 2002;13(8):719-28.
- Austin LT, Ahmad F, McNally MJ, Stewart DE.
Breast and cervical cancer screening in Hispanic women: a literature review using the health belief model. Women’s Health Issues 2002;12(3):122-8.
- Ramirez AG, Suarez L, Laufman L, Barroso C, Chalela P.
Hispanic women’s breast and cervical cancer knowledge, attitudes, and screening behaviors. Am J Health Promot 2000;14(5):292-300.
- Suarez L, Roche RA, Pulley LV, Weiss NS, Goldman D, Simpson DM.
Why a peer intervention program for Mexican-American women failed to modify the secular trend in cancer screening. Am J Prev Med 1997;13(6):411-7.
- Peterson J, Atwood JR, Yates B.
Key elements for church-based health promotion programs: outcome-based literature review. Public Health Nurs 2002;19(6):401-11.
- Freeman HP.
Patient navigation: a community based strategy to reduce cancer disparities. J Urban Health 2006;83(2):139-41.
- DeHaven MJ, Hunter IB, Wilder L, Walton JW, Berry J.
Health programs in faith-based organizations: are they effective? Am J Public Health 2004;94(6):1030-6.
- Navarro AM, Senn KL, McNicholas LJ, Kaplan RM, Roppé B, Campo MC.
Por La Vida model intervention enhances use of cancer screening tests among Latinas. Am J Prev Med 1998;15(1):32-41.
- Duan N, Fox SA, Derose KP, Carson S.
Maintaining mammography adherence through telephone counseling in a church-based trial. Am J Public Health 2000;90(9):1468-71.
- Fox SA, Stein JA, Gonzalez RE, Farrenkopf M, Dellinger A.
A trial to increase mammography utilization among Los Angeles Hispanic women. J Health Care Poor Underserved 1998;9(3):309-21.
- Sauaia A, Dauchot CP, Borrayo EA, Leyba J, Gallo SM, Kramer A. The Tepeyac Project: a church-based approach to increase breast cancer screening among Latinas in Colorado. Conference proceeding from the 9th Biennial Symposium on Minorities, the Medically Underserved and Cancer, Intercultural Cancer Council. 2004 Mar 24-28; Washington, DC.
- Welsh AL, Sauaia A, Jacobellis J, Min S, Byers T. Effect of a church-based approach to increase breast cancer screening among Latinas on Medicaid. Prev Chronic Dis
2005;2(4).
http://www.cdc.gov/pcd/issues/2005/oct/04_0140.htm
- Castro FG, Elder J, Coe K, Tafoya-Barraza HM, Moratto S, Campbell N, et al.
Mobilizing churches for health promotion in Latino communities:
Compañeros en la Salud. J Natl Cancer Inst Monogr 1995;(18):127-35.
- Bailit HL.
Health services research. Adv Dent Res 2003;17(1):82-5.
- Victor TW, Mera RM.
Record linkage of health care insurance claims. J Am Med Inform Assoc 2001;8(3):281-8.
- Perkins R. Evaluating the Passel-Word Spanish surname list: 1990 Decennial Census Post Enumeration Survey results. Washington (DC):
U.S. Census Bureau, Population Division; 1993.
- Humphrey LL, Helfand M, Chan BK, Woolf SH.
Breast cancer screening: a summary of the evidence for the U.S. Preventive Services Task Force. Ann Intern Med 2002;137(5 Part 1):347-60.
- Gluck ME, Hanson KW. Medicare chart book — Fall 2001. Menlo Park (CA): Henry J. Kaiser Family Foundation; 2001.
- Green LH, Cox DF, Langwell KM. Medicare state profiles. Menlo Park (CA): Henry J. Kaiser Family Foundation; 1999.
- Medicaid managed care penetration rates and expansion enrollment by state. Washington (DC):
U.S. Department of Health and Human Services, Centers for Medicare and Medicaid Services; 2006.
- A profile of Medicaid. 2000 chartbook. Washington (DC): U.S. Department of
Health and Human Services, Centers for Medicare and Medicaid Services; 2000.
- Rural urban commuting area zip code approximation. Washington (DC): Health Resources and Service Administration; Economic Research Service; WWAMI Rural Health Research Center; 2007.
- Ruxton GD. The unequal variance t-test is an underused alternative to Student’s
t-test and the Mann-Whitney U test. Behav Ecol 2006;17(4):688-90.
- Hanley JA, Negassa A, Edwardes MD, Forrester JE.
Statistical analysis of correlated data using generalized estimating equations: an orientation.
Am J Epidemiol 2003;157(4):364-75.
- Lipsitz SR, Fitzmaurice GM.
Estimating equations for measures of association between repeated binary responses.
Biometrics 1996;52(3):903-12.
- Davis DT, Bustamante A, Brown CP, Wolde-Tsadik G, Savage EW, Cheng X, et al.
The urban church and cancer control: a source of social influence in minority communities.
Public Health Rep 1994;109(4):500-6.
- Stockdale SE, Keeler E, Duan N, Derose KP, Fox SA.
Costs and cost-effectiveness of a church-based intervention to promote mammography screening.
Health Serv Res 2000;35(5 Pt 1):1037-57.
- Fox SA, Pitkin K, Paul C, Duan N.
Breast cancer screening adherence: does church attendance matter?
Health Educ Behav 1998;25(6):742-58.
- Derose KP, Hawes-Dawson J, Fox SA, Maldonado N, Tatum A, Kington R.
Dealing with diversity: recruiting churches and women for a randomized trial of mammography promotion.
Health Educ Behav 2000;27(5):632-48.
- Program announcement number PA-07-254: cancer surveillance using health claims-based data (R01). Washington (DC): National Institutes of Health, Agency for Healthcare
Research and Quality; 2007.
- Kagay CR, Quale C, Smith-Bindman R.
Screening mammography in the American elderly. Am J Prev Med 2006;31(2):142-9.
- Mouchawar J, Byers T, Warren M, Schluter WW.
The sensitivity of Medicare billing claims data for monitoring mammography use by elderly women. Med Care Res Rev 2004;61(1):116-27.
- Arday SL, Arday DR, Monroe S, Zhang J. HCFA’s racial and ethnic data: current accuracy and recent improvements. Health Care Financ Rev 2000;21(4):107-16.
- D’Antonio WV. Latino Catholics: how different? Kansas City (MO): The
National Catholic Reporter Publishing Company; 1999. http://www.natcath.com/NCR_Online/archives/102999/ 102999p.htm *
Accessed May 27, 2007.
- Panel on DHHS Collection of Race and Ethnicity Data; Ver Ploeg M, Perrin
E, eds. Eliminating health disparities: measurement and data needs. Washington (DC): The National Academies Press; 2004.
Back to top
|
|
