

|

|

Volume
3:
No. 2, April 2006
ORIGINAL RESEARCH
Diffusing a Research-based Physical Activity Promotion Program for Seniors
Into Diverse Communities: CHAMPS III
Anita L. Stewart, PhD, Dawn Gillis, MS, Melanie Grossman, PhD, Martha Castrillo, Leslie Pruitt, PhD, Barbara McLellan,
MPH, Nina Sperber, MA
Suggested citation for this article: Stewart AL, Gillis D, Grossman M, Castrillo M, Pruitt L, McLellan B, et al. Diffusing a research-based physical activity promotion program for seniors
into diverse communities: CHAMPS III. Prev Chronic Dis [serial online] 2006 Apr [date cited]. Available from: URL: http://www.cdc.gov/pcd/issues/2006/
apr/05_0091.htm.
PEER REVIEWED
Abstract
Introduction
Increasing the physical activity levels of older adults through diffusion of
successful research-based programs into community settings is challenging because of differences between research and real-world settings. This project diffused
the Community Healthy Activities Model Program for Seniors (CHAMPS) II, an individual-level research-based physical activity promotion program, through
three community organizations to reach lower-income and minority (primarily
Hispanic or Latino and African American) seniors.
Methods
Through an academic–community partnership, university staff worked with each organization to adapt the program to be appealing and
effective, enable
their staff and volunteers to provide the program, increase participants’ physical activity, and leave
sustainable programs in place. Evaluation was based on methods recommended by the Centers for Disease Control and Prevention.
Results
The adapted programs, referred to as CHAMPS III, differed from the original program and among organizations. Group-based components and resource guides were included and new features were added; however, individualized components were not offered because of limited resources. A total of 321 people enrolled among three organizations; there was a trend toward increased physical activity at two
organizations (an estimated increase of 481 kcal/week [P = .08] and 437 kcal/week [P = .06] expended in physical activity). Evaluation revealed challenges and unexpected community-level benefits. All organizations are continuing efforts to promote physical activity for older adults.
Conclusion
This project enabled community organizations to implement physical activity promotion programs. The overarching challenge was to retain original program features within each organization’s resources yet be sustainable. Although the programs differed from the original research program, they were a catalyst for numerous community-level changes. Our findings can guide similar projects to
reach underserved older adults.
Back to top
Introduction
To address the current public health problem of widespread sedentary behavior among older adults in the United States, numerous initiatives have emerged to promote increased physical activity (PA) (1,2). These are based on substantial evidence of physical and mental health benefits of regular PA for older adults (1,3,4), including walking (5,6).
Evidence for the effectiveness of community-level interventions to increase adult PA was reviewed by the Task Force on Community Preventive Services (7). Two “strong” recommendations were individually adapted health behavior-change programs and creating or improving access to places for PA, particularly in neighborhoods with the least resources, combined with informational
outreach. Individually tailored PA programs and interventions that include principles of behavior change were also featured in the recent Best Practices Statement for promoting PA in older adults developed by a coalition of national organizations led by The American College of Sports Medicine (8).
Many initiatives emphasize the need to increase PA in underserved populations, such
as racial and ethnic minorities or people with low socioeconomic status (SES) (1,9), primarily because these groups are at higher risk of poor health (10-14) and have lower levels of PA than their counterparts (15,16). For example, among adults aged 65 and older who participated in the National
Health Interview Survey, 2001–2002, only 13% of non-Hispanic blacks and 13.6% of Hispanics
or Latinos reported regular leisure-time PA, compared with 22.8%
of non-Hispanic whites (17).
One promising approach to increasing PA among older people in underserved populations is to diffuse
into the community successful research-based PA-promotion programs that are consistent with the recommendations of the Task Force on Community Preventive Services and the
Best Practices Statement (8). However, there are few methods or guidelines for adapting and
diffusing such programs (18). In addition, results from ethnically inclusive studies are often not disseminated widely (19). Closing statements from The Cooper Institute conference in 2004, “Increasing Physical Activity in World Populations: Understanding Diffusion and Dissemination,” suggested that diffusion and dissemination are areas that are still developing (20).
This article reports on a project to diffuse a research-based PA-promotion program, the Community Healthy Activities Model Program for Seniors (CHAMPS) (21), into three community organizations to reach primarily lower-income, racial and ethnic minority older adults. CHAMPS successfully increased PA in adults aged 65 and older in two research studies funded by the National
Institute on Aging: CHAMPS I was conducted in congregate housing settings (22), and CHAMPS II was a randomized controlled trial of sedentary or underactive members of Medicare health maintenance organizations (23).
The goal of CHAMPS III was to evaluate the efficacy of diffusing CHAMPS II by implementing it in three community organizations, adapted to their context and clientele. Specific objectives were the following: 1) to work with staff from participating organizations and community members to adapt CHAMPS II to be appealing, feasible, and
sustainable; 2) to diffuse the modified programs by enabling their staff and volunteers to conduct the programs, with training and assistance; 3) to evaluate implementation processes; 4) to increase participants’ PA levels; and 5) to leave programs in place at each organization. We describe these processes and challenges as well as ideas for improving translation and diffusion processes
in other settings. Our results contribute to a small body of literature on diffusing PA-promotion programs
to reach underserved populations.
Back to top
Methods
Research basis
CHAMPS is a lifestyle PA-promotion program for older adults. The choice-based individually tailored program provides information, skills training, support, and problem solving through a personal planning session, regular telephone follow-up, group workshops, newsletters, activity diaries, and functional fitness assessments. Using principles of social-cognitive theory,
trained staff members assist participants to develop and maintain a PA regimen of their choice, based on their health, preferences, readiness to increase activity, ability, and resources. Participants are encouraged to join existing community-based PA classes and programs, develop a regimen on their own (with guidance), or both. They learn how to motivate themselves, overcome barriers, exercise
safely, develop a balanced program (endurance, strength training, flexibility, balance, and coordination), and progress slowly.
Community–campus partnerships
For CHAMPS III, the University of California, San Francisco (UCSF) partnered with three San Francisco Bay
Area community organizations differing in purpose, size, infrastructure, and clientele. The organizations were as follows:
- Network for Elders (“Network”) in Bayview Hunters Point, San Francisco, provides case management and referral for about 500 frail elders and their families to help elders remain in their homes and reduce isolation. An affiliated interfaith volunteer program provides many services. The
city of San Francisco has designated the region as a low-income concentration
area and an area of concentration for African Americans and Asian/Pacific Islanders.
- On Lok’s 30th Street Senior Center (“30th Street”) in the Mission
District of San Francisco provides approximately 250 seniors per day with a range of activities and services to maintain or improve their well-being. Volunteers offer many of the services. The
city of San Francisco has designated the region as a low-income concentration area and an area of
concentration for Latinos.
- Sequoia Hospital Health & Wellness Services, a hospital-affiliated outpatient center in Redwood City, serves parts of San Mateo County. It provides wellness programs to promote the independence and well-being of adults, in partnership with physicians. Although its clientele tends to be nonminority (its service area was 38% nonwhite in 2003), it aimed to recruit
lower-income, minority older adults for this project.
The organizations were selected to represent different organizational models for program diffusion to reach underserved populations. Selection was also based on a history of collaboration with UCSF faculty working in minority health research.
Because extensive time is needed to establish an effective relationship with community-based organizations (24,25),
this history helped to provide a foundation of trust. We
aimed for each organization to provide the program to community members, with UCSF serving
in a background role.
The UCSF team had expertise in social work, exercise physiology, health education, and community work. UCSF’s role was to 1) help adapt the program to be as similar as possible to the original, 2) develop new program materials, 3) translate materials into Spanish as needed, 4) provide training, 5) monitor implementation, and 6) conduct program evaluation.
Program evaluation framework
The California Endowment funded the project in November 1999 through its CommunitiesFirst initiative (26). This initiative was not intended to support research, so the goal of CHAMPS III was to develop sustainable programs
that met the needs of the communities and organizations. The evaluation was designed to reflect the entire process — from adaptation through implementation. The desire
of our three organizations to minimize the burden of assessment (i.e.,
paperwork) for participants and staff guided many of our choices. We reviewed several program evaluation approaches (27) and selected the Centers for Disease Control and Prevention’s Physical Activity Evaluation Handbook (28), which conceptualizes a project as a sequence of steps leading to a specified goal. A logic model describes influential factors, inputs, activities, and
initial, intermediate, and long-term outcomes, including links among them. Each step is evaluated, and a feedback loop is included. The logic model is intended as a flexible framework that can be interpreted to fit specific project needs. The Figure presents
our interpretation of the logic model for CHAMPS III.
Inputs and planning activities
The project included 1 year for planning and adaptation (November 1999
through October 2000) and 2 years for implementation and evaluation (November
2000 through October 2002). Planning and adaptation activities included
community focus groups on PA attitudes, preferences, and barriers (29,30); planning meetings; and advisory groups (Figure).
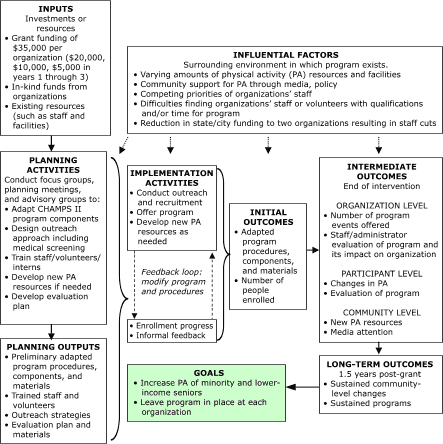
Figure. Logic model for evaluating diffusion of the Community Healthy Activities Model Program for Seniors (CHAMPS) II to reach racial and ethnic minority and lower-income seniors (CHAMPS III).
[A text description of the logic model is also
available.]
Planning outputs
We adapted the program for each organization to maximize safety, feasibility, sustainability, and effectiveness. The original model was not feasible for any of the three organizations selected for this study; thus, during adaptation, we identified the purpose of each component of the original program (e.g., education, motivation) and determined whether it could be achieved in a different way.
For example, although grant funding was available, 30th Street did not hire an exercise specialist because it was not sustainable. (Volunteers
provide many of their programs.) Adaptations continued during implementation based on participant and staff feedback. Planning outputs for each organization are summarized in
Table 1.
One challenge was determining appropriate medical screening procedures based on staffing differences and a reduced capacity for providing individual guidance compared with CHAMPS II. Unique situations also had to be considered; for example, most PA classes at 30th Street were historically available without medical screening or consent. Balancing the need for participant safety with the need to
reduce barriers to participation also influenced CHAMPS III procedures.
The evaluation plan was similar among organizations and included process evaluation to understand adaptation and implementation (31). Every 6 to 12 months, the principal investigator conducted informal, semistructured interviews with staff, volunteers, and directors to obtain their perspective on
the successes and challenges of the program and suggestions for improvement. Depending on the project phase, we
included additional questions on topics such as collaboration, sustainability, and the program’s effect on the organization and community at large.
To measure individual outcomes, interviewers administered the CHAMPS Physical Activity Questionnaire (21,32-34) in English or Spanish
at enrollment and 6 months. From these data, we estimated for each cohort the mean number of calories per week expended and hours per week spent in PA. We compared baseline and 6-month data
using paired t tests to determine the
significance of the changes. Staff also obtained informal input from participants throughout the project, and the Network director conducted a discussion group at the end of the first cohort. The UCSF Institutional Review Board approved
a waiver of consent for all evaluation procedures.
Back to top
Results
We report on the implementation of CHAMPS III as well as initial, intermediate, and long-term outcomes. Initial outcomes include differences between CHAMPS II and the programs offered by each of the three organizations in CHAMPS III and the sociodemographic characteristics of the participants at each organization. Intermediate outcomes were measured at the end of the intervention and
included data on participant levels of PA and organization- and community-level changes. Long-term outcomes were measured
1.5 years after funding for CHAMPS III ended.
Implementation activities
Each organization offered a 6-month program, enrolling two to seven cohorts. During implementation, Network and 30th Street required substantial assistance from UCSF staff, whereas Sequoia conducted its entire program using its own resources. Because PA resources were almost nonexistent in Network’s community, developing new resources became an essential part of
its program.
Feedback from participants and staff and other factors such as community interest resulted in
some early recruitment and program modifications. For example, at Network and 30th Street, the initial recruitment plan was adapted to provide “rolling”
or ongoing enrollment to accommodate individuals who wanted to join after the program was underway.
Initial outcomes
Table 2 shows how each program in CHAMPS III differed from CHAMPS II in
several areas, including staffing, duration, and components offered, and the manner in which the components were provided. The lack of an exercise specialist and other health professionals to offer the one-on-one program components at 30th Street and Network represented a major change from CHAMPS II to CHAMPS III, and the
program was shortened from 1 year to 6 months. Of the components offered in CHAMPS II, the following three were included at all CHAMPS III organizations: functional fitness testing, group workshops, and PA resource directories. Functional fitness assessments were conducted at two sites by volunteers or other participants for educational, planning, and motivational purposes only.
Only Network provided newsletters but in a modified form. 30th Street created a program bulletin board to display announcements and information. The personal planning session and ongoing telephone support were not offered by any organization because of staffing and budget constraints. In CHAMPS II, these two components enabled personal attention and individualized guidance
through discussion of topics such as readiness to change, exercise safety,
barriers to PA, resources, and goal setting. Even Sequoia found these components too labor-intensive despite having appropriate staff.
Elements from these components were included in CHAMPS III group workshops whenever possible. All organizations used occasional reminder telephone calls; Network also provided check-in calls when participants missed activities. New features were added to some programs, such as a weekly program-based
exercise class at Network. This class provided informal support activities, such as sending get-well cards to fellow participants.
Table 3 summarizes the
characteristics of participants at the three organizations, which enrolled a
total of 321 people; most (76% to 97%) were women. A broad age range was
represented: 24% to 52% were aged 75 years and older. Each organization had a
different ethnic mix: of Network’s enrollees, 90% were African American; of 30th
Street’s enrollees, 84% were Latino. Sequoia had difficulty recruiting
lower-income and minority groups; however, of its enrollees, 33% were nonwhite. Participants at 30th Street had low educational levels; more
than half had less than a high school education. At Sequoia, just over 10% had less than a high school education; education was not assessed at Network because community input indicated that the question was too sensitive. Each
organization promoted some events to the community at large (or the entire senior center); therefore, the reach of each program sometimes extended beyond the people who formally joined.
Intermediate outcomes
Intermediate outcomes were measured at the organizational, participant, and community levels immediately after the intervention was completed.
Organization-level outcomes
Each program was unique, and offerings changed as the program evolved and new cohorts were enrolled; thus, the number of activities that were offered varied. Network’s cohorts could attend seven or eight exercise- and health-related workshops and a weekly exercise class. Functional fitness tests were offered two times per cohort. Special events like potluck luncheons
were held occasionally. 30th Street offered to each cohort six exercise-related workshops, two to three additional exercise- and health-related presentations, five to seven The Doctor
Is In sessions (a question-and-answer forum with a physician about exercise and various medical conditions), and one to four special events such as celebrations of participants’ program completion.
Participants could complete fitness testing one or two times. Sequoia’s program at each senior center consisted of eight workshops, including two functional fitness testing sessions and a celebration at completion of the program.
We obtained input on intermediate organization-level outcomes from staff and administrators through process evaluation. A Network administrator noted that although the organization primarily focused on frail elders, CHAMPS III
provided an opportunity to reach seniors who were not homebound or as frail as
its typical client. The project also brought together public and nonprofit community organizations.
30th Street administrators reported positive organization-level changes such as enhanced awareness among staff, volunteers, and seniors of the benefits of PA as well as increased participation in their ongoing exercise classes (open to all 30th Street attendees). The emphasis on increasing PA also attracted younger seniors to the center. Some local physicians referred
patients to 30th Street because of increased program awareness. Because of low participation among men, 30th Street hosted a men’s conference on the benefits of PA and sought information on what might help them become more active. Efforts were then initiated through the city’s recreation and parks department to develop activities suggested by the men. New partnerships provided a channel for sharing information on topics such as potential funding or community resources. Both 30th Street and Network gained access to several academic programs that provided student interns.
Sequoia’s new approach of offering programs at community senior centers (rather than at its own site) led to increased community awareness and appreciation. Sequoia created new partnerships
and strengthened existing ones with several senior centers; they are committed to working together to help maintain seniors’ independence.
Participant-level outcomes
Of the 321 participants enrolled in the three programs, 207 completed baseline and 6-month follow-up questionnaires. Six-month changes
in PA are shown in
Table 4, indicated by changes in estimated caloric
expenditure per week and hours spent per week in PA. A trend toward increased PA was observed at Network (+481 kcal/week, P = .08; +1.9 hrs/week, P = .10) and Sequoia (+437 kcal/week,
P = .06; +2.0 hrs/week, P = .08). No statistically significant change in caloric expenditure was observed at 30th Street, but there was a trend toward decreased duration (−1.4 hrs/week, P = .09). For the total sample among organizations (n = 207), there was a trend toward increased caloric expenditure (+213 kcal/week, P = .10). The overall 6-month response rate at
Sequoia was low (52%), with 83 of 160 participants completing the follow-up questionnaire; thus, results may not represent all people participating in the Sequoia program. The response rate at Network was 85% (53/62), and the response rate at 30th Street was 72% (71/99).
Network obtained an informal evaluation by participants through a one-time discussion group after
being in the program for about 6 months. Most of the feedback was positive. For example, the participants particularly liked the group exercise, fellowship, and a chance to meet new people. They felt that the program “helped them help themselves” and perceived both physical and mental benefits.
Constructive criticism was also provided; participants felt that the classes and workshops were too short, and they wanted more exercise equipment such as treadmills.
Community-level outcomes
At Network, new partnerships with other community organizations developed, enhancing PA resources for seniors. As noted previously, there were no exercise classes available in the Bayview Hunters Point community at the beginning of the program. By the end, there were six: three offered by the local community college, one beginner pool-exercise class, and one African American
line-dancing class, in addition to the program’s exercise class. One intern helped start a walking group that developed into a partnership between the program, the city’s recreation and parks department, and Network’s interfaith volunteer group. All of these exercise resources were formally or informally associated with Network’s program. Program participants regularly
attended the community college classes and helped keep enrollment high enough to sustain the classes. Seniors and staff in Network’s program successfully advocated for new chairs, improved lighting, and regular cleaning of the gymnasium where
some classes were held. Some enrollees became formally involved with the Trust for Public Land in developing a new community park. The Trust approached the
seniors to conduct programs in the park, plan clean-up and planting days, and promote
these activities in their community.
At 30th Street, a new tai chi class was offered twice weekly and became affiliated with the program, with an average attendance of nearly 40. During the project, Sequoia’s staff learned from participants that there was a need for fall prevention; some participants dropped out because they were afraid of falling. Sequoia developed and started teaching fall-prevention
and strength-training classes at three senior centers. The new program attracted new clients. One senior center organized a fitness advisory board to determine
which fitness and health classes should be offered.
Each program received news media attention that helped expand its reach into the community, although most
attention was for Network. A local community newspaper published four articles about PA and Network’s program, and the program was featured on KQED (National Public Radio) in a prime-time report. The line-dancing
class was featured by the San Francisco Chronicle. For 30th
Street, a local Spanish-language newspaper included an article about PA for seniors and the 30th Street program.
Long-term outcomes
Long-term outcomes are defined as those that were measured 1.5 years after the funding for CHAMPS III ended. Ultimately, the success of diffusion programs is
determined by their sustained availability to community members; all organizations
in CHAMPS III are continuing efforts to promote PA for older adults, despite
funding challenges.
At Network, five community dance and exercise classes have continued. In addition, Senior Strutters, a performance group that evolved from the African American line-dancing class, often performs at community events. Because of the increased number of seniors at the city recreation and parks department’s facility where the program class is held, the department provided a staff member to help with set-up and registration, and an employee now teaches the class, which may help the
class continue. Network staff maintains the monthly PA resource calendar discussed previously.
These are substantial accomplishments, because the entire program is run by the
seniors who volunteer their time to promote and coordinate the program and
sustain the exercise classes created in their community; no staff is currently paid to
coordinate the program.
30th Street obtained funding for 2 years to continue and expand its program. The grant supported
a bilingual Wellness Services Coordinator dedicated to the program and provided
for two treadmills. In the new program, physician consent was obtained using a new form that enables physicians to indicate
which classes offered at 30th Street are appropriate for each individual. This allows the coordinator,
without being a trained exercise professional, to tailor the program
to some extent for each participant. In addition, 30th Street’s tai chi class has continued, and a second advanced class has been added.
At Sequoia, efforts have shifted to providing the Mature & Secure From Falls program. Sequoia Hospital offers these programs at no charge. The program has developed into a 6-week community-based class series and has been presented at more than 20 sites in San Mateo County. Sequoia also convened the San Mateo County Fall Prevention Task Force, where 27
organizations providing services to seniors are working to increase awareness about the need for fall prevention and to develop related resources.
Back to top
Discussion
CHAMPS III provided insight into the process of translating and diffusing a research-based program into diverse community-based organizations to reach underserved older adults. We are aware of only a few studies that have diffused research-based PA programs
to reach minority and lower SES subgroups of older adults. The California Active Aging Program was a large-scale effort to
reach seniors through a variety of community settings; although not focused on underserved people, it reached a diverse sample (36). Active for Life is a program to establish research-based PA programs in community settings for adults aged 50 and older; 2 of the 10 settings focus on minority and lower SES individuals (37). Our study differs from the California Active
Aging Program in that, together with our community partners, we obtained community input in our planning year and throughout the project (as part of the participatory research model) to develop adapted programs. Further, we provide more extensive process evaluation information, including challenges and solutions related to diffusion. Last,
we documented unintended community-level changes that
occurred in response to the program.
Our original intent was to diffuse CHAMPS II with some adaptations to meet the needs of the communities and organizations; however, it became apparent that the program would need to change substantially to be feasible and sustainable. The most substantial changes were the loss of the personal planning session and ongoing motivational telephone support at all three
organizations and the lack of a staff exercise specialist at two organizations. Without these components, the programs were not able to provide the ongoing, individual-level guidance and support available in CHAMPS II.
We speculated on why we did not observe more changes in PA levels. It is difficult to compare preintervention and postintervention PA changes between CHAMPS III and CHAMPS II because
CHAMPS II was a randomized controlled trial. Nevertheless, in CHAMPS II, the 1-year estimated increase of 687 kcal/week in PA among the intervention group (23) was
much greater than the estimated increase of 213
kcal/week achieved in the total CHAMPS III sample. Program adaptations likely contributed to these differences; whereas CHAMPS II offered most components recommended in the Best Practices Statement (8), many of these were lost with the adaptations. Other possible explanations are that CHAMPS II excluded people who were already physically active,
whereas physically active people were able to join CHAMPS
III. The baseline level of energy expended in PA among CHAMPS III participants was 2545 kcal/week; among CHAMPS II participants, the baseline level was 1052 kcal/week (23). The California Active Aging Program, using a pre–post design, demonstrated total estimated increases of 644 kcal/week (midpoint) and 707 kcal/week (endpoint) (36). However, that program included individuals aged 50 and
older, included more program components than CHAMPS III, and also excluded people who were already active.
Also of interest is why Network and Sequoia had trends toward increased levels of PA, but no change or
a trend
toward decreased PA (depending on the measure) was observed at 30th Street. Many seniors at 30th Street may have joined because they happened to be at the center at the time of enrollment and fitness testing, and they wanted to be part of what was happening that day. At Network, individuals had to go out of their
way to join and participate. Some participants at 30th Street did not feel comfortable joining existing classes because they were concerned about exercising with certain medical conditions or limitations;
they requested a weekly program class in which they could get guidance similar
to that given in the monthly workshops by the exercise physiologist. Network’s
class was taught by an exercise physiologist and provided social support. Scheduling conflicts related to
the participant’s transportation to the center,
volunteer duties, extended travel to their country of origin, and difficulties with keeping track of when program events were held (because they weren’t on a weekly schedule) seemed common at 30th Street and may have contributed to the PA findings.
Sequoia’s variability in PA changes among cohorts is more difficult to interpret. The variability highlights the unique challenges of collecting evaluation data for a program offered by community organizations (rather than universities such as UCSF). Because program funding was not focused on research, we had to limit paperwork, including questionnaires.
Sequoia’s lower response rates may have been partially responsible for the variability. Sequoia chose to collect data without assistance from UCSF, making quality control difficult. In fact, Sequoia’s staff reported that collecting data on PA was one of the main challenges of the project. At the other sites, extensive efforts were required to collect data; UCSF
staff worked closely
with organization staff to find participants and administer the questionnaires face-to-face. Overall, it was difficult to provide a practical community-based program while obtaining useful evaluation data. At times, the amount of missing or questionable data
precluded our reporting the findings (e.g., data related to participation in program events). Future programs should address these
issues in the grant-proposal stages. It would help to designate and fund university staff to collect all data.
Ideally, more funding should also be allocated toward a more extensive development phase for diffusion project proposals. Although we met with organization administrators before submitting our grant, it was only after the grant was funded and numerous planning meetings took place that both sides truly understood the other’s expectations and resources. It then became
apparent that UCSF staff would need to play more substantial roles than planned
at two sites. This shift raised sustainability concerns, but it was important to support the organizations in offering some version of CHAMPS and observe how it could be sustained. We also learned that some organizations would have preferred to be offered an existing program rather than developing it together; that is, they wanted
to get a program going quickly and respond to problems when they emerged. Because much literature emphasizes the need to involve the community in all aspects of planning (38,39), we were surprised by this feedback.
Based on our experiences, this project succeeded because of at least one enthusiastic staff member at each organization committed to helping seniors with this program. In addition, UCSF
staff characteristics that helped were being 1) culturally competent, 2)
interested in being involved in the community beyond project demands, 3)
creative and patient in overcoming barriers, and 4) able to adapt on a moment’s
notice. For future projects, it would be helpful to have university or
organization staff members serve as a liaison to make connections among resources. In a related study, we found that many community organizations are interested and willing to help in many capacities (e.g., developing new PA resources); however, someone needs to cultivate relationships and translate intentions into
action (40).
We consider the community-level changes effected through implementation of an individual-level program to be the most successful part of our project. This project enabled three organizations to adapt and implement a program to increase PA among minority and lower-income seniors. The three organizations are committed to retaining PA as part of their offerings; Network and
30th Street have sustained some program components, and Sequoia is promoting PA through
its new fall-prevention program.
The main caveat is that the project was only a first step toward a sustained effort. To adequately diffuse such a program into communities to serve lower income and minority older adults, settings are needed with more infrastructure and capacity, with staff experienced in reaching and working with culturally diverse groups, and with an exercise specialist
available to offer parts of the program. An
alternative model is to partner with public health departments offering chronic disease prevention programs, where health educators and public health nurses might provide program features with assistance and input from exercise specialists
(40). Public health departments already serve precisely the seniors we targeted; thus, they already have
established relationships in the community and mechanisms for conducting outreach.
This article provides an example of applying the program evaluation approach from the Physical Activity Evaluation Handbook (28) to a diffusion project. We have highlighted the complexities of evaluating community programs to reach minority and lower-income older adults. Our findings should facilitate the diffusion of
other programs such as CHAMPS into communities to reach
some of our nation’s more vulnerable older adults.
Back to top
Acknowledgments
This project was funded by grant #1998/296 from The California Endowment. A portion of the evaluation was funded by grant #44223 from The Robert Wood Johnson Foundation. The authors thank each of the organizations, their volunteers, participants, interns, and dedicated staff, especially Shireen McSpadden (now at San Francisco Department of Aging and Adult Services) and
Beverly Taylor at Network for Elders, Jorge Santis and Valorie Villela at On Lok’s
30th Street Senior Center, and Marie Violet and Kristin Lauria Gurley at Sequoia Hospital Health
& Wellness Services. We also thank their community partners, especially the Older Adults Department at City College of San Francisco and San Francisco Recreation & Park Department, Bayview Hunters
Point; Belle Haven Senior Center, Menlo Park; San Carlos Senior Center, San Carlos; Twin Pines Senior Center, Belmont; and Veterans Memorial Senior Center, Redwood City.
Back to top
Author Information
Corresponding Author: Anita L. Stewart, PhD, Institute for Health & Aging, University of California, San Francisco, 3333 California St, Suite 340, San Francisco, CA 94118. Telephone: 415-502-5207. E-mail:
Anita.Stewart@ucsf.edu.
Author Affiliations: Dawn Gillis, MS, Melanie Grossman, PhD, Martha Castrillo, Barbara McLellan, MPH, Nina Sperber, MA, Institute for Health & Aging, University of California, San Francisco, San Francisco, Calif; Leslie Pruitt, PhD, Institute for Health
& Aging, University of California, San Francisco, San Francisco, Calif, Stanford Prevention Research Center, Stanford
University School of Medicine, Stanford, Calif.
Back to top
References
- U.S. Department of Health and Human Services. Healthy people 2010. Washington
(DC): U.S. Department of Health and Human Services, U.S. Government Printing Office; 2000.
- National blueprint: increasing physical activity among adults age 50 and older. J Aging Physical Activity 2001;9(Supplement):1-28.
- U.S. Department of Health and Human Services. Physical activity and health:
a report of the Surgeon General. Atlanta (GA): U.S. Department of Health and
Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion; 1996.
- American College of Sports Medicine Position Stand.
Exercise and physical activity for older adults. Med Sci Sports Exerc 1998;30(6):992-1008.
- Moreau KL, Degarmo R, Langley J, McMahon C, Howley ET, Bassett DR, et al.
Increasing daily walking lowers blood pressure in postmenopausal women. Med Sci Sports Exerc 2001;33(11):1825-31.
- Pate RR, Pratt M, Blair SN, Haskell WL, Macera CA, Bouchard C, et al.
Physical activity and public health. A recommendation from the Centers for Disease Control and Prevention and the American College of Sports Medicine. JAMA 1995;273(5):402-7.
- Centers for Disease Control and Prevention.
Increasing physical activity. A report on recommendations of the Task Force on Community Preventive Services.
MMWR Recomm Rep 2001;50(RR-18):1-14.
- American College of Sports Medicine.
Physical activity programs and behavior counseling in older adult populations. Med Sci Sports Exerc 2004;36(11):1997-2003.
- The Prevention Institute. Health for all: California’s strategic approach
to eliminating racial and ethnic health disparities [Internet]. Washington (DC): The American Public Health Association;
2003 Nov. Available from: URL: http://www.preventioninstitute.org/pdf/ H4A_MAIN_1Scites_021304.pdf*.
- Hummer RA, Benjamins MR, Rogers RG. Racial and ethnic disparities in health and mortality among the U.S. elderly population. In: Anderson NB, Bulatao RA, Cohen B, editors. Critical perspectives on racial and ethnic differences in health in late life. Washington
(DC): The National Academies Press; 2004. p. 53-94.
- Pappas G, Queen S, Hadden W, Fisher G.
The increasing disparity in mortality between socioeconomic groups in the United States,
1960 and 1986. N Engl J Med 1993;329(2):103-9.
- National Center for Health Statistics. Health, United States 2003. Hyattsville
(MD): U.S. Department of Health and Human Services; 2003.
- Centers for Disease Control and Prevention.
Recent trends in mortality rates for four major cancers, by sex and race/ethnicity — United States, 1990-1998.
MMWR Morb Mortal Wkly Rep 2002;51(3):49-53.
- Pamuk E, Makuc D, Heck K, Reuben C, Lochner K. Socioeconomic status and health chartbook. Health United States, 1998. Hyattsville
(MD): National Center for Health Statistics; 1998.
- Liao Y, Tucker P, Okoro CA, Giles WH, Mokdad AH, Harris VB.
REACH 2010 surveillance for health status in minority communities — United States, 2001-2002.
MMWR Surveill Summ 2004;53(6):1-36.
- Centers for Disease Control and Prevention. Behavioral Risk Factor Surveillance System
survey data. Atlanta (GA): U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; 2002.
- Federal Interagency Forum on Aging-Related Statistics. Older Americans 2004. Key indicators of well-being. Washington
(DC): Federal Interagency Forum on Aging-Related Statistics, U.S. Government Printing Office; 2004.
- Prohaska TR, Peters KE, Warren JS. Health behavior. From research to community practice. In: Albrecht GL, Fitzpatrick R, Scrimshaw SC, editors. The handbook of social studies in health & medicine. London:
SAGE Publications; 2000. p. 359-373.
- Yancey AK, Kumanyika SK, Ponce NA, McCarthy WJ, Fielding JE, Leslie JR, et al.
Population-based interventions engaging communities of color in healthy eating and active living: a review. Prev Chronic Dis [serial online] 2004
Jan.
- The Cooper Institute. Increasing physical activity in world populations: understanding
diffusion and dissemination. The Cooper Institute Conference Series
[Internet]. Dallas (TX): The Cooper Institute; 2004 Oct 21–23. Available from:
URL: http://www.cooperinst.org/conf2004prg.asp*.
- Institute for Health & Aging. CHAMPS: Community Healthy Activities Model Program for Seniors [Internet].
San Francisco (CA): University of California, San Francisco, Institute for
Health & Aging. Available from: URL: http://www.ucsf.edu/champs/*.
- Stewart AL, Mills KM, Sepsis PG, King AC, McLellan B, Roitz K, et al.
Evaluation of CHAMPS, a physical activity promotion program for older adults. Ann Behav Med 1997;19(4):353-61.
- Stewart AL, Verboncoeur CJ, McLellan BY, Gillis DE, Rush S, Mills K, et al.
Physical activity outcomes of CHAMPS II:
a physical activity promotion program. J Gerontol A Biol Sci Med Sci 2001;56(8):465-70.
- Israel BA, Schulz AJ, Parker EA, Becker AB.
Review of community-based research:
assessing partnership approaches to improve public health. Annu Rev Public Health 1998;19:173-202.
- Lasker RD, Weiss ES, Miller R.
Partnership synergy:
a practical framework for studying and strengthening the collaborative
advantage. Milbank Q 2001;79(2):179-205, III-IV.
- The California Endowment. CommunitiesFirst initiative [Internet]. Thousand Oaks
(CA): The California Endowment [cited 2005 Jul 15]. Available from: URL:
http://calendow.org/opportunities/communitiesfirst.stm*.
- Linnan L, Steckler A. Process evaluation for public health interventions and research: an overview. In: Steckler A, Linnan L, editors. Process evaluation for public health interventions and research. San Francisco
(CA): Jossey-Bass; 2002. p. 1-23.
- U.S. Department of Health and Human Services. Physical activity evaluation handbook. Atlanta
(GA): U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; 2002.
- Grossman MD, Pruitt L, Gillis D, McLellan B, Castrillo M, Stewart AL, et al. Physical activity perceptions, preferences and barriers in older African Americans. Ann Behav Med 2001;23(Suppl):S109.
- Grossman M, Pruitt L, Castrillo M, Gillis D, McLellan B, Stewart A. Physical activity preferences, facilitators and barriers in older African Americans and Hispanics. Gerontologist 2002;42(Special Issue):96.
- U.S. Department of Health and Human Services. Promoting physical activity.
A guide for community action. Atlanta (GA): U.S. Department of Health and
Human Services, Centers for Disease Control and Prevention, National Center
for Chronic Disease Prevention and Health Promotion, Division of Nutrition
and Physical Activity; 1999.
- Stewart AL, Mills KM, King AC, Haskell WL, Gillis D, Ritter PL.
CHAMPS
physical activity questionnaire for older adults. Outcomes for interventions. Med Sci Sports Exerc 2001;33(7):1126-41.
- Harada ND, Chiu V, King AC, Stewart AL.
An evaluation of three self-report physical activity instruments for older adults. Med Sci Sports Exerc 2001;33(6):962-70.
- Resnicow K, MCCarty F, Blissett D, Wang T, Heitzler C, Lee RE.
Validity of a modified
CHAMPS physical activity questionnaire among African Americans. Med Sci Sports Exerc 2003;35(9):1537-45.
- Rikli RE, Jones CJ. Development and validation of a functional fitness test for community-residing older adults. J Aging Physical Activity 1999;7(2):129-61.
- Hooker SP, Seavey W, Weidmer CE, Harvey DJ, Stewart AL, Gillis DE, et al.
The California Active Aging Community Grant Program: translating science into practice to promote physical activity in older adults. Ann Behav Med 2005;29(3):155-65.
- Texas A&M University. Active for life [Internet]. College Park (TX): Texas A&M University System, School of Rural Public Health. Available from: URL: http://www.activeforlife.info*.
- Gonzalez VM, Gonzalez JT, Freeman V, Howard-Pitney B. Health promotion in diverse cultural communities. Palo Alto
(CA): Health Promotion Resource Center, Stanford Center for Research in Disease Prevention; 1991.
- Green LW, Mercer SL.
Can public health researchers and agencies reconcile the push from funding bodies and the pull from communities? Am J Public Health 2001;91(12):1926-9.
- Stewart Al, Grossman M, Bera N, Gillis DE, Sperber N, Castrillo M, et
al. Multi-level perspectives on diffusing a physical activity promotion
program to reach diverse older adults. J Aging Phys Act. Forthcoming.
Back to top
|
|
