

|

|

Volume 2: No. 3, July 2005
ORIGINAL RESEARCH
Are Older Adults Up-to-Date With Cancer Screening and Vaccinations?
Douglas Shenson, MD, MPH, MS, Julie Bolen, PhD, MPH, Mary Adams, MPH, Laura Seeff,
MD, Donald Blackman, PhD
Suggested citation for this article: Shenson D, Bolen J, Adams M, Seeff
L, Blackman D. Are older adults up-to-date with cancer screening and vaccinations? Prev Chronic Dis [serial online] 2005 Jul [date cited]. Available from: URL:
http://www.cdc.gov/pcd/issues/2005/
jul/05_0021.htm.
PEER REVIEWED
Abstract
Introduction
Public health organizations in the United States emphasize the importance of
providing routine screening for breast cancer, cervical cancer, and colorectal
cancer, as well as vaccinations against influenza and pneumococcal disease among
older adults. We report a composite measure of adults aged 50 years and older
who receive recommended cancer screening services and vaccinations.
Methods
We analyzed state data from the 2002 Behavioral Risk Factor Surveillance System, which included 105,860 respondents aged 50 and older. We created a composite measure that included colonoscopy or sigmoidoscopy
within 10 years or a fecal occult blood test in the past year, an influenza
vaccination in the past year, a Papanicolaou test within 3 years for women with an intact cervix,
a mammogram, and for adults aged 65 and older, a pneumonia vaccination during their lifetime. We performed separate analyses for four age and sex groups: men aged 50 to 64, women aged 50 to 64, men aged 65 and older, and women aged 65 and older.
Results
The percentage of each age and sex group that was up-to-date according to our composite measure ranged from 21.1% of women aged 50 to 64 (four tests) to 39.6% of men aged 65 and older (three tests). For each group, results varied by income, education, race/ethnicity, insurance status, and whether the respondent had a personal physician.
Conclusion
These results suggest the need to improve the delivery of cancer screenings and vaccinations among adults aged 50 and older. We propose continued efforts to measure use of clinical preventive services.
Back to top
Introduction
Healthy People 2010 is a national initiative that has set specific health and health care objectives (1). These performance targets include the delivery of adult clinical preventive services such as cancer screening and vaccinations. Studies of the effectiveness of these services have been reviewed by the U.S. Preventive Services Task Force (USPSTF) (2), and recommendations for
providing the services have been developed by the Guide to Community Preventive Services (3). Both efforts emphasize the importance of providing routine screening for breast cancer, cervical cancer, and colorectal cancer as well as vaccinations against influenza and pneumococcal disease.
The delivery rates of cancer screenings and adult vaccinations have typically been measured separately through population-based surveys, including the Behavioral Risk Factor Surveillance
System (BRFSS) and the National Health Interview Survey (NHIS). Although this approach is well suited for assessing progress toward Healthy People 2010 objectives, it does not measure the extent to
which individuals receive the full complement of recommended clinical preventive services.
There is currently no index that combines data on the use of all recommended
clinical preventive services among adults. In this article, we present a
composite measure of cancer screening services and vaccinations obtained by
adults aged 50 years and older as a first step toward assessing overall clinical preventive service delivery. We chose to begin our assessment by combining these two sets
of interventions because they are universally recommended and data on their use in all 50 states and the District of Columbia are available through the 2002 BRFSS. Composite indices have long been used for the surveillance of childhood vaccinations (4).
Our approach aims to provide a more meaningful and practical measure of the state of clinical preventive service delivery. Such a comprehensive measure could also enhance the ability of health departments and community groups to assess disparities in delivering preventive services, to better gauge progress toward measurable objectives, and to identify best practices for achieving prevention
goals.
Back to top
Methods
Data
We used data from the 2002 BRFSS; the BRFSS is an ongoing state-based telephone survey of randomly selected adults and is coordinated by the Centers for Disease Control and Prevention (CDC). The survey collects data from noninstitutionalized adults
aged 18 and older on health practices that are related to the leading causes of death and disability (5). We limited our analysis to data from
adults aged 50 and older, including 105,860 respondents in 49 states and the District of Columbia. Illinois data are not reported because approximately half of the female respondents in that state were not asked questions about breast and cervical cancer screening. All results are based on weighted data that account for different probabilities of selection and are adjusted to the total adult
population in each state by age and sex or age, race, and sex.
Measures
We analyzed responses to the BRFSS core questions on the use of clinical preventive services recommended by the USPSTF for adults aged 50 and older: colorectal cancer screening, mammography, Papanicolaou (Pap) test, and influenza and pneumococcal vaccinations
(Table 1). These questions were asked in all states and territories that participated in the 2002 BRFSS survey. All measures of
preventive health services were dichotomized as yes or no based on receipt of the service according to schedules recommended by the USPSTF.
The USPSTF recommends influenza vaccination for adults aged 50 and older (6); other agencies support this recommendation (7). We used a 10-year interval for endoscopy (colonoscopy or sigmoidoscopy) because the BRFSS question did not distinguish
between the two interventions. The USPSTF does not recommend intervals for the use of sigmoidoscopy or colonoscopy; other national guidelines recommend a 5-year interval for sigmoidoscopy and a 10-year interval for colonoscopy (8-10). For all services, people who had never had the test or had the tests outside the designated schedule were included in the group who answered no. Our analysis
excluded respondents with missing values except for respondents missing one colorectal cancer screening value. Because colorectal cancer screening recommendations involve receiving either endoscopy or fecal occult blood testing (FOBT), we did not exclude respondents with missing values for one test if they had the other test within the recommended interval.
From the separate measures for cancer screenings and vaccinations, we created a variable to measure whether a person had received
all of these clinical preventive services as recommended by the USPSTF. Because the recommendations vary by age and sex, this measure, which we call being up-to-date, was determined separately for four age and sex groups. For men
aged 50 to 64, the up-to-date measure included men who met the recommendation for colon cancer screening and influenza vaccination (two services). For women aged 50 to 64, the up-to-date measure included women who met the recommendations for colon cancer screening, breast cancer screening, cervical cancer screening, and influenza vaccination (four services). The up-to-date measure includes women
with a hysterectomy among those who met recommendations for cervical cancer screening. Because a Pap test is not normally recommended for these women, it would be incorrect to classify them as not being up-to-date on cervical cancer screening. For adults aged 65 and older, the up-to-date measure included the cancer screening tests for their sex, plus an influenza vaccination and a
pneumococcal vaccination (three services for men and five services for women). The number of tests required for being up-to-date
was two for men aged 50 to 64, three for men aged 65 and older, four for women aged 50 to 64,
and five for women aged 65 and older (colorectal, breast, and cervical cancer screening
in addition to influenza and pneumonia vaccinations).
From responses to several questions on race and ethnicity that permitted respondents to indicate more than one race, we created five groups: white (limited to non-Hispanic whites), black (limited to non-Hispanic blacks), Hispanic of any race, Asian or Pacific Islander, and American Indian or Alaska Native. Level of education was recoded from multiple responses into four
categories: less than high school, high school graduate or general equivalency
diploma (GED), some college, and college graduate. Health insurance status was
determined by the response to a single question and coded yes or no. Data on household income were coded into four groups: less than $25,000, $25,000 to $49,999, $50,000 to $74,999, and $75,000 and above. Respondents were asked if they had a personal physician; those with
one or more were coded as yes. Health status was dichotomized into 1) fair or poor
or 2) good, very good, or excellent.
Statistical analysis
Stata, Version 8.0 (StataCorp, College Station, Tex), was used in all statistical analyses to account for the complex sample design of the BRFSS. Most analyses were performed on subpopulations representing four age and sex groups: men aged 50 to 64, women aged 50 to 64, men aged 65 and older, and women aged 65 and older. Pearson's chi-square tests were used to compare the percentage of adults who
were up-to-date on the recommended services for their age and sex group by demographic characteristics. For mapping purposes, we divided state results into quartiles and then combined the middle two quartiles.
Back to top
Results
The median state response rate for the 2002 BRFSS was 58.3% (range 42.2%–82.6%) (11). Results for the individual preventive health services for each of the age and sex groups are presented in
Appendix Tables A–D. All other results are for being up-to-date on cancer screening and vaccinations as defined above.
We combined data for 49 states and the District of Columbia to examine the percentage of adults who were up-to-date among demographic and risk-factor subgroups
(Table 2). Black, Hispanic,
and Asian older adults were significantly less likely than whites to be
up-to-date in at least two of the four age and sex groups. On the other hand,
although they did not reach statistical significance, rates for American Indians were
consistently close to rates for whites in three of the four groups.
Among both men and women in all age groups, having more education was strongly related to being up-to-date. Respondents with less than a high school education were much less likely to be up-to-date (range 12.4%–29.5%) than those with a college degree (range 25.4%–43.8%). Similarly, higher income was associated with being up-to-date on cancer screening and vaccinations.
Adults with health insurance were about twice as likely to almost three times as likely to be up-to-date as adults with no insurance. The same was true for adults with a personal physician compared with those without one. Overall, people who reported fair or poor health were more likely to be up-to-date than those
who reported good, very good, or excellent health.
State-specific prevalence estimates for each of the age and sex groups were divided into quartiles and mapped (Figure 1). States in the western and southeastern United States were among
those with the lowest percentage of men aged 50 to 64 who were up-to-date on cancer screening and vaccinations (California, Idaho, Nevada, Utah, and Wyoming in the West; Arkansas, Florida, Georgia, Louisiana,
and Mississippi in the Southeast). There was a similar but less pronounced pattern for women aged 50 to 64 (Idaho, Nevada, and Wyoming in the West; Arkansas, Florida, Georgia, Louisiana, and Mississippi in the Southeast). The percentage of men and women aged 65 and older who were up-to-date was low in Indiana, Louisiana, Mississippi, Nebraska, and Texas. Arizona, California, Minnesota,
North Dakota, Connecticut, Rhode Island, Wisconsin, Massachusetts, and Maine had higher percentages of people aged 65 and older who were up-to-date than most of the other states. Minnesota had the highest percentage of
up-to-date adults in each of the four age and sex groups.
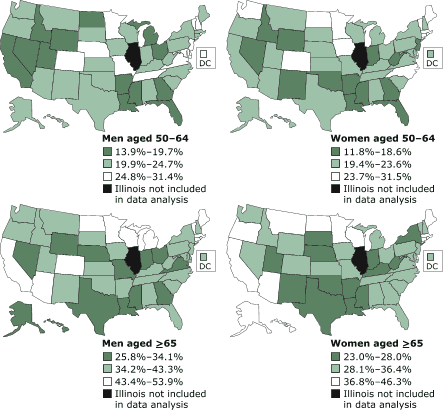
Figure 1. Prevalence estimates of adults aged ≥50
years who were up-to-date for cancer screening and vaccinations by age group, sex, and
state, Behavioral Risk Factor Surveillance System (BRFSS), 2002. Data from 49 states and
the District of Columbia. Results were divided into quartiles, and the middle
two quartiles were combined. Illinois data are not included because the state
used a split sample for some preventive service questions. [A
text description of these maps is also available.]
The percentage of each age and sex group that was up-to-date is presented by state in
Table 3. The state medians for the percentage of
respondents who were up-to-date were consistently less than 40% (with a range of
22.1% for women aged 50 to 64 to 38.2% for men aged 65 and older) (Figure 2). Median state values were similar to results for all adults reported in Table 2.
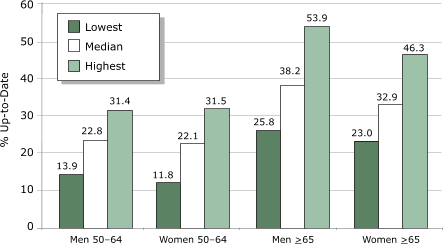
Figure 2. Median and range of state-specific results for percentage of adults
aged ≥50 years who were up-to-date
for cancer screening and immunizations, Behavioral Risk Factor Surveillance
System (BRFSS), 2002. Data from 49 states and the District of Columbia. Illinois data
are not included because the state used a split sample for some preventive
service questions. [A
text description of this graph is also available.]
Table 4 shows the
percentage of adults who had zero, one, two, three, four, or five cancer
screenings or vaccinations. Most adults had one or more preventive services, with
the percentage of adults who received none of the services ranging from 3.6% for
women aged 65 and older to 38.3% for men aged 50 to 64. Thus, the results
indicated that at least 61.7% of older men and more than 95% of older women have had
some contact with the health care system within the past few years.
Back to top
Discussion
This analysis of state BRFSS data indicates that among the four age and sex groups, the state medians for adults who are up-to-date with recommended cancer screenings and vaccinations range from 22.1% (women aged 50 to 64) to 38.2% (men aged 65 and older). Although the delivery rates of individual clinical preventive services may be relatively high — cervical cancer screening, for
example, is at a national median of 81.0% — overall levels of protection provided by cancer screenings and vaccinations are low.
This study did not include data on cholesterol screening or tetanus–diphtheria vaccination,
or data on clinical preventive services that are also recommended according to a
specific schedule. Other excluded measures included screening for abnormalities of blood pressure, height, weight, obesity, vision, and hearing; chemoprevention for cardiovascular disease (aspirin); and counseling on
calcium intake, folic acid, tobacco cessation, drug and alcohol use, sexually transmitted diseases, human immunodeficiency virus (HIV), nutrition, physical activity, sun exposure, oral health, injury prevention, and polypharmacy.
In addition to low absolute levels, the data indicate important differences among states. For each of the four age and sex groups, Minnesota consistently had the highest up-to-date percentages. Several factors may explain why this state has done so well in preventive service delivery: a high proportion of the population is enrolled in managed care; the state has a low uninsurance rate; and
state-sponsored outreach promotes colorectal cancer screening and adult vaccinations. Additional research is necessary to fully explore the reasons for success in Minnesota. Many of the lowest measurements were found in the southeastern and south-central United States; these states have low rates of health insurance among adults (12).
Each of the four age and sex groups has its own set of recommended clinical preventive services.
Figure 2 illustrates that men and women within each of the two age groups have similar proportions that are up-to-date, despite the fact that more tests are required of women. When compared
with women in the same age group, men are much more likely to have had none of the recommended
services. The reasons for these differences are not clear from the data and require further analysis.
There were significant differences in being up-to-date among racial and
ethnic categories. Based on consistency across age and sex groups, it appears that blacks, Hispanics, and Asians may be less likely than whites to be up-to-date for cancer screenings and adult vaccinations.
There may be higher rates of screening among American Indians because many American Indians receive health care through the Indian Health Service, which emphasizes preventive health practices. Further investigation of these racial and ethnic disparities is warranted.
Not only are reasons for racial and ethnic disparities not clear from the data but these disparities
also are confounded by disparities in being up-to-date according to educational, socioeconomic, and insurance status. Respondents who have a college degree are 1.5 to 2 times more likely to be up-to-date than respondents who do not have a high school degree. Receipt of clinical
preventive services is also consistently associated with higher income level for each of
the four age and sex groups. Large differences exist between people who have medical insurance and people who do not. People with health insurance or personal physicians have approximately two to three times the rate of clinical preventive service delivery as people without
either of them. According to the U.S. Census,
11.1% of whites, 19.6% of blacks, 18.8% of Asians, and 32.7% of Hispanics lacked insurance in 2003 (13). These findings are consistent with those of other studies that have found significant disparities in the delivery of cancer screening (14-16) and adult vaccinations (17,18) when measured by race/ethnic group, education, and income.
More than 95% of adults aged 65 and older have health insurance through
Medicare, which pays for cancer screening and vaccinations (19). Nonetheless,
fewer than 40% of this age group are up-to-date on all of the recommended cancer screening and vaccinations. Having health insurance (and a personal physician) —
although necessary — is not in itself sufficient for achieving high
levels of being up-to-date with cancer screenings and vaccinations.
Our results suggest that most respondents have received at least one cancer screening or vaccination. Therefore, most adults aged 50 and older have
had some contact with the health care system within the past few years, but they do not receive the preventive services recommended for their age and sex group. At the same time, the analysis indicates that up-to-date rates are not low because adults lack only a single
service.
This work builds on the analysis of others (20). The BRFSS has followed state rates for clinical preventive service delivery for more than 20 years, and a recent study has provided a comprehensive overview of trends (21). Combined measurements of mammography, clinical breast exam, and Pap testing have been made using
data from the 1990 NHIS of Health Promotion and Disease Prevention (22). A methodology for building a prevention index has also been developed using electronic medical records. This index can serve as a combined quality assessment measure and be compared with consensus measures or with selected Health Plan Employer Data and Information Set (HEDIS) scores for health management organizations (23).
This study has a number of limitations. First, the BRFSS relies on self-reported data. Depending on the measure, self-reports can result in overestimates or underestimates compared with other data sources, such as health care records. Unfamiliarity with medical terms and telescoping (24) (recalling events more recently than they actually occurred) can affect the validity of self-reported
clinical preventive services and probably result in overestimates (20,25). A review article by Nelson
et al rates the validity of self-reports for mammography, Pap test, colorectal cancer screening, and pneumococcal vaccination as moderate and the validity for influenza vaccination as high (26). Second, households without telephones, which are more likely to have adults with low
socioeconomic status, were excluded from the survey. This omission may have resulted in an overestimation of delivery rates (27). Third, the survey excludes people who rely only on cellular telephones for their telephone service. Finally, the BRFSS questions limited our ability to adequately determine compliance with Pap test recommendations for women aged 65 and older. The USPSTF recommends
against routine screening for cervical cancer for women in this age group if they have had sufficient recent Pap tests with no abnormal results and are not otherwise at increased risk for cervical cancer (28). Without Pap test histories, we could not ascertain which of these older women might not need further Pap testing, and thus we were unable to determine how this anomaly in the recommendations
might have affected our estimates of being up-to-date on the Pap test among women aged 65 and older.
The results of this study suggest several potential next steps. From a surveillance perspective, we recommend that state-based surveys such as the BRFSS consider periodically collecting in the same year information about clinical preventive services with specific schedules (i.e., the services analyzed in this study as well as cholesterol screening and tetanus–diphtheria vaccination). In this way, a more complete measure of delivered adult clinical preventive services recommended by age and sex can be calculated. One of the strengths of a composite measure of clinical preventive services is that it emphasizes the overall protection of individuals by combining measurements across disease categories. We also recommend that surveys such as the BRFSS examine the
feasibility and implications of routinely reporting a composite measure such as the one suggested by this study.
The building blocks of composite measures will change as recommendations for individual interventions evolve. For example, colorectal cancer screening guidelines for Healthy People
2010 objectives have not yet been updated to match USPSTF recommendations. (Healthy
People 2010 objectives for Pap test, mammography, and adult vaccinations are consistent with USPSTF recommendations for women aged 50 and older.)
The results of this study also suggest that the delivery of clinical preventive services in physicians’ offices needs continued attention. Among respondents who indicated having a personal physician, the group with the highest proportion
of up-to-date was men aged 65 and older at only 41.5%; the group with the lowest proportion was women aged 50 to 64 at 22.8%. Despite important initiatives designed
to improve the provision of clinical preventive services in physicians’ offices, such as the Agency for Healthcare Research and Quality’s Put Prevention
Into Practice (PPIP) (29), more work is necessary to enhance chart-flagging systems and improve reminder protocols aimed at patients. Physicians have begun to systematically consider various approaches to addressing multiple behavioral
risk factors in primary care (30), and we hope that this commitment can be extended to providing multiple clinical preventive services.
From a public health standpoint, new kinds of programs are needed to address the shortfall identified by this study. Access to each of the recommended clinical preventive services can be facilitated inside and outside of the clinical setting.
New initiatives must focus on populations, not patient panels. A community-wide strategy has been developed by the Sickness Prevention
Achieved through Regional Collaboration (SPARC) program in Connecticut, Massachusetts, and New York, and has achieved promising results (31,32) by expanding delivery at clinical sites and creating new points of access in nonclinical settings. A similar approach has been taken by New York State’s Healthy Women Partnerships, which facilitates the delivery of multiple cancer screenings for
underserved populations. Community-wide assurance of clinical preventive services has been a priority for the Group Health Cooperative, a nonprofit health care system based in Seattle, Wash, which covers a large proportion of its region’s residents (33).
Additional analytic work is necessary. An examination of data from states that collect information on cholesterol screening and tetanus–diphtheria vaccinations will yield a more complete — and perhaps lower — composite measure of up-to-date use of recommended services. A multivariable regression analysis will provide a fuller understanding of factors that are most strongly and
independently associated with failure to be up-to-date, and a longitudinal analysis of trends in the composite measure will yield useful information for targeting state preventive health efforts.
This study reports low composite rates of adult clinical preventive service delivery based on 2002 BRFSS data for adults aged 50 and older and highlights significant disparities among groups. We
must redouble our efforts to develop more effective approaches to delivering these basic adult clinical preventive services.
Back to top
Acknowledgments
The authors thank Michael Alderman, MD, and David Nelson, MD, MPH, for their review of earlier drafts of this article.
Back to top
Author Information
Corresponding Author: Douglas Shenson, MD, MPH, MS, 76 Prince St, Newton, MA 02465. The author is affiliated with Sickness Prevention Achieved through Regional Collaboration (SPARC), Lakeville, Conn. Telephone: 617-796-7966. E-mail: dshenson@sparc-health.org.
Author Affiliations: Julie Bolen, PhD, MPH, Laura Seeff, MD, Donald Blackman,
PhD, Centers for Disease Control and Prevention, Atlanta, Ga; Mary Adams, MPH, On Target Health Data LLC, Hartford, Conn.
Back to top
References
- U.S. Department of Health and Human Services. Healthy People 2010: understanding and
improving health. 2nd ed. Washington (DC): U.S. Government Printing Office; 2000
Nov.
- U.S. Department of Health and Human Services. Guide to clinical preventive
services. U.S. Preventive Services Task Force. 3rd ed. Washington (DC): U.S.
Government Printing Office; 2004
Apr.
- Zaza S, Briss PA, Harris KW, editors. The guide to community preventive services:
what works to promote health? Task Force on Community Preventive Services. New
York (NY): Oxford University Press; 2005.
- Barker L, Santoli J, McCauley M. National, state, and urban area vaccination coverage among children aged 19-35 months — U.S. 2003. MMWR 2004;53(29):658-61.
-
Bolen JC, Rhodes L, Powell‑Griner E, Bland SD, Holtzman D.
State‑specific prevalence of selected health behaviors, by race and ethnicity
— Behavioral
Risk Factor Surveillance System 1997. MMWR CDC Surveill Summ 2000;49(2):1-60.
- Clinical Preventive Services for Normal-Risk Adults Recommended by the
U.S. Preventive Services Task Force. Put Prevention into Practice.
Agency for Healthcare Research and Quality. Rockville (MD);2004 Jan. Available from:
URL: http://www.ahrq.gov/ppip/adulttm.htm.
- Centers for Disease Control and Prevention.
Prevention and control of influenza:
recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 2000;49(RR-3):1-38.
-
Pignone M, Rich M, Teutsch SM, Berg AO, Lohr KN.
Screening for colorectal cancer in adults at average risk: a summary of the evidence
for the U.S. Preventive Services Task Force. Ann Intern Med 2002;137(2):132-41.
-
Winawer S, Fletcher R, Rex D, Bond J, Burt R, Ferrucci J, et al.
Colorectal cancer screening and surveillance: clinical guidelines and rationale-update
based on new evidence. Gastrointestinal Consortium Panel. Gastroenterology 2003;124(2):544–60.
- Smith RA, von Eschenbach AC, Wender R, Levin B, Byers T, Rothenberger D,
et al.
American Cancer Society guidelines for the early detection of cancer: update of early detection guidelines for prostate, colorectal, and endometrial cancers. CA Cancer J Clin 2001;51(1):38-75.
-
Centers for Disease Control and Prevention. 2002 Behavioral Risk Factor
Surveillance System summary data quality report. Atlanta (GA): Centers for
Disease Control and Prevention. Available from: URL: http://www.cdc.gov/brfss/technical_infodata/pdf/
2002SummaryDataQualityReport.pdf.
- Mills RJ, Bhandari S. Health insurance coverage in the United States, 2002.
Current Population Reports, P60-223. Washington (DC): U.S. Census Bureau; 2003.
p.1-24.
- DeNavas-Walt C, Proctor BD, Mills RJ. Income, poverty, and health
insurance coverage in the United States, 2003. Current Population Reports, P60-226.
Washington (DC): U.S. Census Bureau; 2004.
- Bradley CJ, Given CW, Roberts C.
Health care disparities and cervical cancer. Am J Public Health 2004;94(12):2098-103.
- Peek ME, Han JH.
Disparities in screening mammography. Current status, interventions and implications. J Gen Intern Med 2004;19(2):184-94.
- Shapiro JA, Seeff LC, Nadel MR.
Colorectal cancer-screening tests and associated health behaviors. Am J Prev Med 2001;21(2):132-7.
- Centers for Disease Control and Prevention.
Racial/ethnic disparities in influenza and pneumococcal vaccination levels among persons aged
≥65 — United States, 1989-2001. MMWR 2003;52(40):958-62.
- Bonito AJ, Lenfestey NF, Eicheldinger C, Iannacchione VG, Campbell L.
Disparities in immunizations among elderly Medicare beneficiaries,
2000-2002. Am J Prev Med 2004;27(2):153-60.
- U.S. Department of Health and Human Services. The guide to medicare prevention
services: for physicians, providers, suppliers, and other health care
professionals. Center for Medicare and Medicaid Services. CMS-10110.
Washington (DC): U.S. Government Printing Office: 2004 Aug.
- Nelson DE, Bland S, Powell-Griner E, Klein R, Wells HE, Hogelin G, et al.
State trends in health risk factors and receipt of clinical preventive services among U.S. adults during the 1990s.
JAMA
2002;287(20):2659-67.
- Okoro CA, Strine TW, Young SL, Balluz LS, Mokdad AH.
Access to health care among older adults and receipt of preventive services. Behavioral Risk Factor Surveillance System
(BRFSS), 2002. Prev Med 2005;40(3):337-43.
- Pearlman DN, Rakowski W, Ehrich B.
Mammography, clinical breast exam, and
pap testing: correlates of combined screening. Am J Prev Med 1996;12(1):52-64.
- Vogt TM, Aickin M, Ahmed F, Schmidt M.
The
Prevention Index: using technology to improve quality assessment.
Health Serv Res 2004;39(3):511-30.
- Sudman SN, Bradburn NM. Effects of time and memory factors on response in surveys. J Am Stat Assoc 1973;68:805-15.
- Newell SA, Girgis A, Sanson-Fisher RW, Savolainen NJ.
The accuracy of self-reported health behaviors and risk factors relating to cancer and cardiovascular disease in the general population: a critical review.
Am J Prev Med 1999;17(3):211-29.
- Nelson DE, Holtzman D, Bolen J, Mack KA, Stanwyck CA.
Reliability and
validity of measures from the Behavioral Risk Factor Surveillance System
(BRFSS). Soz
Praventivmed 2001;46 (Suppl 1) p. S3-42.
- Thornberry OT, Massey JT. Trends in the United States telephone coverage across time and subgroup. In: Groves RM, Biemer PP, Lyberg LR, Massey JT, Nichols WL, editors. Telephone
survey methodology. New York (NY): John Wiley & Sons; 1988. p. 25-49.
- Smith RA, Cokkinides V, von Eschenbach AC, Levin B, Cohen C, Runowicz CD,
et al.
American Cancer Society
guidelines for the early detection of cancer. CA Cancer J Clin 2002;52(1):8-22.
- Agency for Healthcare Research and Quality. About PPIP: Put Prevention Into Practice, 2000.
Rockville (MD): Agency for Healthcare Research and Quality; 2000. Available from:
URL:
http://www.ahrq.gov/ppip/ppipabou.htm.
- Pronk NP, Peek CJ, Goldstein MG.
Addressing multiple behavioral risk factors in primary care.
Am J Prev Med 2004;27(2S):1-110.
- Shenson D, Cassarino L, DiMartino D, Marantz P, Bolen J, Good B, et al.
Improving access to mammography through community-based influenza clinics:
a quasi-experimental study. Am J Prev Med 2001;20(2):97-102.
- Shenson D, Quinley J, DiMartino D, Stumpf P, Caldwell M, Lee T.
Pneumococcal immunizations at flu clinics:
the impact of community-wide outreach. J Community Health 2001;26(3):191-01.
- Thompson RS, Taplin SH, McAfee TA, Mandelson MT, Smith AE.
Primary and secondary prevention services in clinical practice. Twenty years’ experience in development, implementation, and evaluation. JAMA 1995; 273(14):1130-5.
Back to top
|
|
