Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Prevalence of Autism Spectrum Disorders --- Autism and Developmental Disabilities Monitoring Network, United States, 2006
Please note: An erratum has been published for this article. To view the erratum, please click here.
Abstract
Problem/Condition: Autism spectrum disorders (ASDs) are a group of developmental disabilities characterized by atypical development in socialization, communication, and behavior. ASDs typically are apparent before age 3 years, with associated impairments affecting multiple areas of a person's life. Because no biologic marker exists for ASDs, identification is made by professionals who evaluate a child's developmental progress to identify the presence of developmental disorders.
Reporting Period: 2006.
Methods: Earlier surveillance efforts indicated that age 8 years is a reasonable index age at which to monitor peak prevalence. The identified prevalence of ASDs in U.S. children aged 8 years was estimated through a systematic retrospective review of evaluation records in multiple sites participating in the Autism and Developmental Disabilities Monitoring (ADDM) Network. Data were collected from existing records in 11 ADDM Network sites (areas of Alabama, Arizona, Colorado, Florida, Georgia, Maryland, Missouri, North Carolina, Pennsylvania, South Carolina, and Wisconsin) for 2006. To analyze changes in identified ASD prevalence, CDC compared the 2006 data with data collected from 10 sites (all sites noted above except Florida) in 2002. Children aged 8 years with a notation of an ASD or descriptions consistent with an ASD were identified through screening and abstraction of existing health and education records containing professional assessments of the child's developmental progress at health-care or education facilities. Children aged 8 years whose parent(s) or legal guardian(s) resided in the respective areas in 2006 met the case definition for an ASD if their records documented behaviors consistent with the Diagnostic and Statistical Manual of Mental Disorders, 4th edition, text revision (DSM-IV-TR) criteria for autistic disorder, pervasive developmental disorder--not otherwise specified (PDD NOS), or Asperger disorder. Presence of an identified ASD was determined through a review of data abstracted from developmental evaluation records by trained clinician reviewers.
Results: For the 2006 surveillance year, 2,757 (0.9%) of 307,790 children aged 8 years residing in the 11 ADDM sites were identified as having an ASD, indicating an overall average prevalence of 9.0 per 1,000 population (95% confidence interval [CI] = 8.6--9.3). ASD prevalence per 1,000 children aged 8 years ranged from 4.2 in Florida to 12.1 in Arizona and Missouri, with prevalence for the majority of sites ranging between 7.6 and 10.4. For 2006, ASD prevalence was significantly lower in Florida (p<0.001) and Alabama (p<0.05) and higher in Arizona and Missouri (p<0.05) than in all other sites. The ratio of males to females ranged from 3.2:1 in Alabama to 7.6:1 in Florida. ASD prevalence varied by type of ascertainment source, with higher average prevalence in sites with access to health and education records (10.0) compared with sites with health records only (7.5). Although parental or professional concerns regarding development before age 36 months were noted in the evaluation records of the majority of children who were identified as having an ASD, the median age of earliest documented ASD diagnosis was much later (range: 41 months [Florida]--60 months [Colorado]). Of 10 sites that collected data for both the 2002 and 2006 surveillance years, nine observed an increase in ASD prevalence (range: 27%--95% increase; p<0.01), with increases among males in all sites and among females in four of 11 sites, and variation among other subgroups.
Interpretation: In 2006, on average, approximately 1% or one child in every 110 in the 11 ADDM sites was classified as having an ASD (approximate range: 1:80--1:240 children [males: 1:70; females: 1:315]). The average prevalence of ASDs identified among children aged 8 years increased 57% in 10 sites from the 2002 to the 2006 ADDM surveillance year. Although improved ascertainment accounts for some of the prevalence increases documented in the ADDM sites, a true increase in the risk for children to develop ASD symptoms cannot be ruled out. On average, although delays in identification persisted, ASDs were being diagnosed by community professionals at earlier ages in 2006 than in 2002.
Public Health Actions: These results indicate an increased prevalence of identified ASDs among U.S. children aged 8 years and underscore the need to regard ASDs as an urgent public health concern. Continued monitoring is needed to document and understand changes over time, including the multiple ascertainment and potential risk factors likely to be contributing. Research is needed to ascertain the factors that put certain persons at risk, and concerted efforts are essential to provide support for persons with ASDs, their families, and communities to improve long-term outcome.
Introduction
Autism spectrum disorders (ASDs) are a group of developmental disabilities characterized by atypical development in socialization, communication, and behavior. The symptoms of ASDs typically are present before age 3 years and often are accompanied by abnormalities in cognitive functioning, learning, attention, and sensory processing (1). The term "spectrum disorders" is used to indicate that ASDs encompass a range of behaviorally defined conditions, which are diagnosed through clinical observation of development. These conditions include autistic disorder (i.e., autism), Asperger disorder, and pervasive developmental disorder--not otherwise specified (PDD-NOS) (2--4). Persons with Asperger disorder or PDD-NOS have fewer diagnostic symptoms of ASDs compared with autism, and the symptoms often are indicative of more mild impairment. The complex nature of these disorders, the current lack of consistent and reliable genetic or biologic diagnostic markers, and changes in how these conditions are defined and identified make evaluating ASD prevalence over time challenging.
Since the early 1990s, the number of persons receiving services for ASDs has increased substantially (5--11). However, identifying children for services for autism might not be equivalent to using consistent diagnostic standards to identify persons in the population because services within communities are not available uniformly to all persons with ASDs. For this reason, studies that rely exclusively on single-source administrative datasets (e.g., disability service records or annual reports of special education counts) most likely underestimate ASD prevalence and might not adequately capture changes in the ASD population over time (8,12--14).
Before the 1980s, the term "autism" was used primarily to refer to autistic disorder and was thought to be rare, affecting approximately one in every 2,000 (0.5%) children (2,3). Autism now is considered to be one of three disorders classified together as ASDs (4). Using diagnostic criteria established in the early 1990s, which encompass a broad spectrum of disorders (15,16), the best estimate of ASD prevalence is that approximately six or seven of every 1,000 (0.6%--0.7%) children have an ASD. These estimates are approximately 10 times higher than estimates using earlier criteria (2--4,12). However, some recent population-based studies have documented even higher ASD prevalence estimates of >1% of children in areas of Japan, Sweden, the United Kingdom, and the United States (12,17--21), with ASD symptoms identified in 2.7% of children in one study from Norway (22).
Elevated public concern, continued increases in the number of children receiving services for ASDs, and reports of higher-than-expected ASD prevalence highlight the need for systematic public health monitoring of ASDs (23). For this reason, in 2000, CDC organized the Autism and Developmental Disabilities Monitoring (ADDM) Network to provide a better understanding of the prevalence, population characteristics, and public health impact of ASDs and other developmental disabilities in the United States (4,23). The ADDM Network employs a multisite, multiple-source, records-based surveillance methodology to conduct detailed retrospective screening and review of behavioral data from multiple education and health facilities. Administrative records of children who have been evaluated for a range of developmental conditions are reviewed, and standard criteria for case identification and confirmation are applied at each of the surveillance sites (1,24).
Two surveillance summaries presenting ADDM Network ASD prevalence data for 2000 and 2002 have been published previously (4,12). These first two ADDM prevalence reports served to establish baseline prevalence for ASDs among U.S. children aged 8 years. Prevalence for those reports was calculated by race/ethnicity, sex, and multiple ASD-associated characteristics (e.g., cognitive impairment) on the basis of data from six sites* in 2000 and from 14 sites† in 2002. Overall prevalence estimates for both surveillance years were comparable (6.7 and 6.6 cases per 1,000 children aged 8 years in 2000 and 2002, respectively). Among the participating sites, ASD prevalence in 2000 ranged from 4.5 cases per 1,000 children aged 8 years in West Virginia to 9.9 cases in New Jersey, compared with 3.3 cases in Alabama to 10.6 cases in New Jersey in 2002. From 2000 and 2002, prevalence of identified cases of ASDs was stable in four of the six sites (Arizona, Maryland, New Jersey, and South Carolina) that collected data in both years and increased in two sites (Georgia and West Virginia).
This report presents results for 2006 from 11 ADDM Network sites§ and describes updated ASD prevalence overall and by race or ethnicity, sex, level of cognitive functioning, ASD subtype, and multiple associated characteristics. Because 10 sites (Alabama, Arizona, Colorado, Georgia, Maryland, Missouri, North Carolina, Pennsylvania, South Carolina, and Wisconsin) also collected data on ASD prevalence in 2002 (12), changes in identified ASD prevalence in these sites are also reported. In addition, data for an additional surveillance year, 2004, were collected by eight sites.¶ The 2004 surveillance year represented an effort on a smaller scale that was conducted by sites with available resources to collect an additional surveillance year of data. Results for 2004 have been summarized (see Appendix).
Methods
Surveillance Methods
The ADDM Network's methodology (Figure 1) is modeled on that used by CDC's Metropolitan Atlanta Developmental Disabilities Surveillance Program (MADDSP), an active, population-based surveillance program that monitors the occurrence of developmental disabilities through retrospective record review among children aged 8 years in the metropolitan Atlanta area (1,25--27). Although ASD symptoms typically are present in the first 3 years of life, identification often is not made not until later; previous surveillance efforts have identified age 8 years as a reasonable index age at which to monitor peak prevalence for ASDs (1). The ADDM Network implemented the MADDSP methodology using a common case definition and standardized data abstraction, clinician review, and quality assurance procedures.
Study Sites
ADDM site project teams are located at state health departments or at universities working on behalf of their state health departments to collect or receive information used for protecting public health. Sites were selected through a competitive objective review process on the basis of their ability to conduct active ASD records-based surveillance; they were not selected to be a nationally representative sample. Each site met applicable local Institutional Review Board and/or other privacy and confidentiality requirements.
Study Sites and Population Characteristics
During 2006, CDC and 10 site project teams collaborated in monitoring reported occurrence of ASDs in selected areas of 11 states (Table 1). On the basis of postcensal estimates, the number of children aged 8 years in the 11 surveillance sites ranged from 7,184 in Colorado to 46,621 in Georgia (28). Distribution according to race/ethnicity among children aged 8 years varied across surveillance sites. The percentage of non-Hispanic white children residing in each surveillance area ranged from 23.3% in Maryland to 69.7% in Alabama; the percentage of non-Hispanic black children ranged from 5.4% in Arizona to 50.1% in Pennsylvania; the percentage of Hispanic children ranged from 2.9% in Missouri to 52.3% in Florida; the percentage of Asian/ Pacific Islander children ranged from 1.1% in Alabama to 5.8% in Georgia; and the percentage of American Indian/Alaska native children was ≤0.6% in all sites except Arizona (with 2.2%). The breakdown by sex was similar across sites, with approximately equal distribution of male and female children.
Case Definition
For surveillance purposes, children who were born in 1998 whose parent(s) or legal guardian(s) resided in the site's geographic region (Table 1) at any time in 2006 were classified as having an ASD if they displayed behaviors documented in evaluation records by a community professional that were consistent with the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision (DSM-IV-TR) criteria (15) for the subtypes of autistic disorder, PDD-NOS (including atypical autism), or Asperger disorder at any time through age 8 years. An evaluation record was defined as the documented record of an assessment conducted by a community professional to determine the need for special education services or the presence of a developmental disorder. The assessments could be conducted at any time in the child's life through age 8 years. A community professional was defined as a clinical or education professional with specialized training in the observation of children with developmental disabilities (e.g., a developmental pediatrician, child psychiatrist, pediatric neurologist, clinical or developmental psychologist, or speech or language pathologist). The case definition focuses on identifying the behaviors consistent with the presence of any ASD rather than on attempting to identify specific ASD subtypes. Children were classified as having cognitive impairment if they had an intellectual quotient (IQ) score of ≤70 on their most recent test of intellectual ability available in the record. Borderline cognitive functioning was defined as an IQ score of 71--85, and average to above-average functioning was defined as an IQ score of >85.
Case Ascertainment
To begin ascertainment of possible cases, investigators at each site identified data sources for health and education providers for children aged 8 years within the jurisdiction of the site that evaluated, educated, or treated children with developmental disabilities. Health sources included providers of developmental evaluations, including state health facilities, hospitals, clinics, diagnostic centers, private physicians' offices, and other clinical providers. Investigators then asked each identified provider for a list of all children whose medical records were associated with a diagnostic or billing International Criteria for Diagnosis, 9th Revision (ICD-9) (29) code for child neurodevelopmental disorder (e.g., 299.0 for autistic disorder or 315.3 for developmental speech or language disorder). Seven sites (Alabama, Arizona, Georgia, Missouri, North Carolina, South Carolina, and Wisconsin) reviewed additional records for additional ICD-9 codes for other developmental disabilities monitored by that site (e.g., cerebral palsy or intellectual disability). In addition, six sites (Arizona, Colorado, Georgia, Maryland, North Carolina, and South Carolina) (Table 1) also included education sources and the special education evaluation records of children receiving special education services during 2005--2006 and/or 2006--2007. Each child was assigned a unique identifier to prevent duplication and to link information across multiple data sources.
Investigators then reviewed the records of each provider or education source; records were selected for abstraction if the child met the residency requirement and the record contained a documented or suspected ASD classification (i.e., a diagnosis of an ASD or a special education eligibility classification of autism) and/or descriptions of social behaviors associated with an ASD diagnosis. Abstracted information included the evaluation date; data source (education or health); community professional type and degree (e.g., MD, developmental pediatrician or PhD, clinical psychologist); developmental history and indications of developmental concerns (e.g., notations in the records about parental or professional worries that the child's development was not progressing typically); verbatim behavioral descriptions associated with autism (e.g., current and past social, communication, and behavioral functioning); results from IQ, adaptive, and tests used to diagnose autism; and evaluation conclusions. The most recent eligibility classification for receiving special education services (e.g., autism or learning disability) was collected from special education records. For all abstracted evaluations, information from multiple sources was combined into one composite summary record with a unique identifier for each child and was then sent for clinician review.
Clinician Review
All abstracted evaluations from the case ascertainment phase were reviewed and scored by an ASD clinician reviewer. Clinician reviewers included professionals (e.g., medical doctors, psychologists, and speech and language pathologists) with specialized training and experience in autism assessment and diagnosis. Clinician reviewers were selected and assessed periodically for reliability. Clinician reviewers used a coding guide developed on the basis of DSM-IV-TR criteria (15) to determine whether each identified child met the ASD case definition. A child met the ASD case definition if evidence documented in the abstracted evaluations indicated the presence of autistic disorder, PDD-NOS, or Asperger disorder. The clinician reviewer classified the child as having an ASD if evidence existed of either 1) the DSM-IV-TR criteria in the social, communication, and behavior domains and evidence of delays before age 3 years or 2) the social and either communication or behavior criteria for PDD-NOS or Asperger disorder. Because the thresholds for meeting the criteria specified by DSM-IV-TR are lower for the diagnosis of PDD-NOS or Asperger disorder than for autistic disorder, a stricter requirement was included requiring that at least one of the autism-specific behaviors be of a sufficient quality or intensity to be highly indicative of an ASD (12,23). Under this additional requirement, for example, the DSM-IV-TR social criterion of "limited social or emotional reciprocity" required a specific impairment (e.g., "rarely responds verbally or nonverbally to a social approach from others in a familiar setting").
In addition to the DSM-IV-TR criteria, all evaluation information was reviewed to categorize any concerns noted in developmental evaluations concerning the child's developmental status before age 3 years; any specified concerns regarding the development of social, language, or imaginative play before age 3 years also were documented, as were any indications of regression or plateau in skill development. Descriptions of associated features (e.g., odd responses to sensory stimuli) by the community professional also were coded. The diagnostic conclusion of the community professional who evaluated the child also was summarized, including specification of any ASD diagnosis by subtype, when available. Children were classified as having a previously documented ASD classification if they had 1) received a diagnosis of autistic disorder, PDD-NOS, Asperger syndrome, PDD, or ASD by a qualified professional that was documented in an evaluation record or 2) had received special education services under an autism eligibility category.
Before clinician review began for each surveillance year, interrater reliability was established among reviewers according to standards of ≥80% agreement for overall case status and other scored items. Ongoing inter-rater reliability checks were conducted on a blinded, random sample of ≥10% of records reviewed. The percentage of agreement for the final case definition was acceptable for 2006 (range: 82%--100% across sites [Kappa range: 0.5--1.0]) and 2002 (12).
Analytic Methods
ASD prevalence estimates were calculated using as the denominator the number of children aged 8 years residing in the study area according to CDC's National Center for Health Statistics (NCHS) vintage 2007 postcensal population estimates for each site (28). NCHS datasets provide estimated population counts by county, single year of age, race, ethnic origin, and sex. The race or ethnicity of each child was determined from information contained in the source records or, if not found in the source file, from birth certificates (when available). Race- or ethnicity-specific rates were calculated for five populations: non-Hispanic white, non-Hispanic black, Hispanic, Asian/Pacific Islander, and American Indian/Alaska Native. Prevalence results are reported per 1,000 children aged 8 years identified as meeting the ASD case definition over the total number of children that age in the population. To allow comparison of ASD estimates identified by community professionals with those identified by ADDM Network data, ASD prevalence also was calculated on the basis of the number of children who had a previously documented classification of an ASD on record compared with the total number of children in the population aged 8 years. Poisson approximation to the binomial distribution was used to calculate 95% confidence intervals (CIs) for prevalence rates (30). Chi-square tests were used to compare prevalence estimates within and across sites, and rate ratios and percentage change were used to compare prevalence changes within each site for 2002 and 2006 (31,32). Data from 2002 were compared with data from 2006 because 2002 represented the largest and most complete first year of data collection for 10 of the sites reporting in 2006. A maximum value of p<0.05 was used for all tests of statistical significance.
Because the ADDM Network identifies children who meet the ASD case definition on the basis of information contained in evaluation records, variation in the components of this process could account for some differences in prevalence across sites or over time in the same site. Several aspects of the identification process were monitored to evaluate their impact on changes in identified ASD prevalence among sites and across surveillance years. The percentage of children in the population who had a record abstracted for ASD represents the number of children identified in the case ascertainment phase over the total population of children aged 8 years in that site (Table 1). Variation in the abstraction proportion is influenced primarily by 1) the number and type of data sources accessed by individual sites, including access to education sources; 2) the number of ICD-9 billing codes used for source data requests; 3) the number of evaluation records found in the files; 4) the numbers of files not located for review; and 5) the level of detail in source records, including documentation of the descriptions and assessment information consistent with ASDs.
To facilitate an evaluation of the potential effect on ASD prevalence presented by the seven sites that reviewed records for additional ICD codes, the number of children who were identified solely on the basis of those additional codes was identified, and the impact on prevalence was estimated (27). At each site, certain education and health records could not be located for review, and an analysis of the effect of these missing records on case ascertainment was conducted. All children initially identified for screening were first stratified by two factors highly associated with final case status: information source (education only, health only, or both types of sources) and the presence or absence of either an ASD ICD-9 code (299.0 or 299.8) or an autism special education eligibility. The potential number of cases missed because of missing records, and the impact on prevalence, was estimated on the assumption that within each of the strata, the proportion of children with missing records who ultimately would be confirmed as having ASD cases would have been similar to that of children for whom no records were missing.
Results
The 11 ADDM sites identified 5,151 children who met the criteria for abstraction as potentially meeting the ASD case definition. The proportion of children aged 8 years in the population whose records were abstracted varied (range: 0.5% [Florida]--2.4% [Georgia]) (Table 1). The median number of comprehensive evaluations abstracted per child with ASD ranged from two in Maryland to seven in Pennsylvania (Table 1). During clinician review, more than half of these children (54%; n = 2,757) were confirmed as meeting the ASD case definition (range: 42% [Georgia]--81% [Florida]).
Overall ASD Prevalence Estimates
In 2006, the overall identified ASD prevalence per 1,000 children aged 8 years varied across ADDM sites (range: 4.2 [Florida]--12.1 [Arizona and Missouri]) (Table 2). The average across all 11 sites was 9.0 (CI = 8.6--9.3) per 1,000 children. Overall estimated ASD prevalence per 1,000 children aged 8 years was significantly lower (p<0.01) in Florida (4.2; CI = 3.5--5.0) than in all other sites, whereas overall estimated ASD prevalence in Alabama (6.0; CI = 5.3--6.9) was significantly lower (p<0.05) than identified ASD prevalence in each of the remaining sites except Colorado (7.5; CI = 5.7--9.8).
In general, estimated ASD prevalence was lower in ADDM sites that relied solely on health sources to identify cases (mean: 7.5 per 1,000 population; CI = 7.0--7.9) compared with sites that also had access to education sources (mean: 10.2 per 1,000 population; CI = 9.7--10.7) (p<0.001). For sites that relied solely on health sources, identified ASD prevalence was significantly higher in Missouri (12.1) and significantly lower in Florida (4.2) (p<0.001). Among sites with access to education sources, identified ASD prevalence was significantly higher in Arizona (12.1) than in each of the other sites (p<0.05) whereas prevalence in Colorado (7.5) was significantly lower (p<0.05) than in Arizona (12.1), Georgia (10.2), and North Carolina (10.4). In sites with access to both health and education sources, the proportion of ASD cases identified exclusively from education sources ranged from 20% in North Carolina to 78% in Arizona.
Prevalence by Sex and Race or Ethnicity
A consistent finding in all sites was that ASD prevalence was significantly higher (p<0.001) among boys than among girls. ASD prevalence among males ranged from 7.3 in Florida to 19.3 in Missouri (average: 14.5 [CI = 13.9--15.1]) (Table 2). ASD prevalence among females ranged from 1.0 in Florida to 4.9 in Arizona (average: 3.2 [CI = 2.9--3.5]). The combined male-to-female prevalence ratio across all sites was 4.5:1 (range: 3.2:1 [Alabama]--7.6:1 [Florida]).
ASD prevalence also varied by race and ethnicity (Table 2). Combining data from all sites, the average prevalence among non-Hispanic white children (9.9; CI = 9.4--10.4) was significantly greater than that among non-Hispanic black children (7.2; CI = 6.6--7.8) and Hispanic children (5.9; CI = 5.3--6.6) (Table 2) (p<0.001). For five (Florida, Georgia, Missouri, North Carolina, and Wisconsin) of the 11 ADDM sites, ASD prevalence was significantly higher among non-Hispanic white children than among non-Hispanic black children (p<0.05). ASD prevalence was significantly lower among Hispanic children than among non-Hispanic white children in six sites (Alabama, Arizona, Georgia, Missouri, North Carolina, and Wisconsin), and was significantly lower than prevalence among non-Hispanic black children in four sites (Alabama, Arizona, Colorado, and Georgia). Estimates for Asian/Pacific Islander children ranged from 1.0 to 16.2, with wide CIs suggesting that findings for this subgroup should be interpreted with caution.
Special Education Eligibility
For sites that had full access to education records, information in the records indicated that the vast majority of children identified with an ASD for surveillance were receiving special education services through public schools (Table 3). Wide variation existed in the proportion of children who were documented to receive special education under an eligibility category of autism (range: 34% [Colorado]--76% [Maryland]) (Table 3). Other common special education eligibilities included "specific learning disabilities," "speech and language impairments," "other health impairments," and "intellectual disabilities," with these proportions also varying by site (Table 3).
Previously Documented Classification of ASD
Among all children meeting the ADDM ASD surveillance case definition, approximately 77% had a documented ASD classification in their records (range: 65% [Arizona]--93% [Maryland]). Overall prevalence estimates based on ADDM methods were higher than those based on an ASD classification documented by a community professional in the records (Figure 2). The median age of earliest known ASD diagnosis documented in children's records varied (range: 41 months [Florida]--60 months [Colorado]). Across all 11 ADDM sites, the average age of diagnosis was 53 months (Table 4).
Cognitive Functioning
Data on cognitive functioning are reported for sites having IQ test scores available on at least 70% of children who met the ASD case definition. The proportion of children with ASDs who had test scores indicating cognitive impairment (IQ ≤70) ranged from 29.3% in Colorado to 51.2% in South Carolina (average: 41%). In four of the six sites (Alabama, Arizona, North Carolina, and South Carolina), a higher proportion of females with ASDs had cognitive impairment compared with males (Figure 3), although Arizona was the only site for which the proportions differed significantly (p<0.05).
Developmental Characteristics
The vast majority of children with ASDs in all sites had developmental concerns noted to occur before age 3 years (Table 4) (range: 70% [Maryland]--95% [Alabama]). The most commonly documented early developmental concern was language delay. In 2006, the proportion of children with an indication of developmental regression (i.e., loss of previously acquired skills in social, communication, play, or motor areas) ranged from 13.3% in Alabama to 29.6% in Colorado and Wisconsin (Table 4), whereas the proportion indicating developmental plateau (i.e., lack of continued development without clear evidence of regression) was consistently lower (range: 3.2% [Georgia]--10.9% [Missouri]) (Table 4).
Comparison Between 2002 and 2006 Prevalence Estimates
All of the 10 ADDM sites that provided data for both 2002 and 2006 reported an increase in identified ASD prevalence among children aged 8 years within each site (range: 34%--95%; p<0.01) except Colorado, (p=0.19), with an average increase of 57% (6.0 to 9.4 cases per 1,000 population; p<0.0001) (Table 5). Although the direction and magnitude of change within various subgroups differed across sites, aggregate increases were observed within all major sex, racial/ethnic, and cognitive functioning categories.
Increases in identified ASD prevalence were found among boys in nine sites and among girls in four sites. On average, identified ASD prevalence increased 60% among males (from 9.5 to 15.2; p<0.001) and 48% among females (from 2.3 to 3.4; p<0.001).
For all sites except Colorado, Pennsylvania, and South Carolina, a significant increase was noted in identified ASD prevalence among non-Hispanic white children, with an average increase of 55% (p<0.001) (Table 5). The average increase in identified ASD prevalence among non-Hispanic black children was 41% (p<0.001) and also was significant within four sites (Alabama, Arizona, Georgia, and Pennsylvania). For Hispanic children, overall prevalence of ASDs increased 91% (p<0.001), primarily attributable to the sizable Hispanic population and an increase in prevalence of 144% in Arizona. Prevalence among Hispanic children did not change significantly within any of the other 10 sites.
For sites having IQ test scores available for ≥70% of persons identified with an ASD, a 35% increase (range: 0--96%) in identified ASD prevalence was reported among children with cognitive impairment (IQ ≤70), a 90% increase (range: 21%--180%) among children with borderline intellectual functioning (IQ 71--85), and a 72% increase (range: 24%--116%) among children with average to above-average intelligence (IQ >85) (Table 5).
During 2002--2006, the proportion of children who met the ASD case definition and had a previously documented ASD classification in their records increased <5%, on average, across the 10 sites, from 72% in 2002 to 77% in 2006. Within sites, this increase ranged from <1% in Alabama and Georgia to >15% in Colorado. Average ASD prevalence based on documented ASD classification in records increased 64% (from 4.4 to 7.2 per 1,000 population), paralleling the 57% increase in ADDM-identified ASD prevalence estimates (Figure 4). When only ASD diagnoses (i.e., excluding an autism eligibility classification for special education services) documented by a community professional were considered, the specific ASD diagnosis subtype could be examined to indicate children who ever had received a diagnosis of autism (autistic disorder) documented in records at any time through age 8 years and those who received a diagnosis of another subtype of ASD (Asperger disorder, PDD-NOS, ASD, or PDD without subtype specified). In 2002, an average of 44.9% (range: 32.7%--52.5%) of children with ADDM-identified ASD had ever received an autism diagnosis compared with 47% (range: 38.1%--61.1%) in 2006. For all those who received ASD diagnoses other than autism, no overall change was observed across all sites, with an average of 23.7% (range: 9.3%--39%) in 2002 and 23.8% (range: 7.4%--37%) in 2006 (Figure 5). No consistent pattern existed in the use of ASD subtype diagnoses across the sites from 2002 to 2006. During 2002--2006, the median age of earliest documented ASD diagnosis decreased in all sites, from a decrease of 1 month in Wisconsin to 15 months in Alabama (Table 6).
Considering changes in the surveillance identification process from 2002 to 2006, data sources were stable within sites. For seven sites (Alabama, Colorado, Georgia, Maryland, Pennsylvania, South Carolina, and Wisconsin), the proportion of children identified with ASDs who were born in and still resided in the surveillance areas did not change >5%. The three sites (Arizona, Missouri, and North Carolina) that had the greatest increases in ASD prevalence also had the largest increases during 2002--2006 in the proportion of children aged 8 years who were born in and still resided in the surveillance area, indicating a more stable population by 2006. Some differences were noted in the proportion of files that were located for review. Sensitivity analyses conducted by all sites determined that files that were eligible for review but not located contributed to <5% of the change in prevalence in all sites except South Carolina, for which approximately 13% of the 43% prevalence increase from 2002 to 2006 could be explained by improved ability to locate records for review.
For the 10 sites that reported data for both 2002 and 2006, an average of four evaluations were abstracted per child in 2002 compared with five evaluations abstracted per child in 2006. In addition, a qualitative assessment of differences in the information contained in developmental evaluation records across sites conducted by polling the clinicians reviewing the records indicated that the quality and amount of information contained in the evaluation records improved steadily over time, with noticeable increases in level of detail documented on ASD symptoms by 2006.
Discussion
Across the 11 ADDM sites, retrospective estimates from the year 2006 indicated ASD prevalence ranging from 4.2 to 12.1, with most sites identifying prevalence of 7.5 to 10.4 cases per 1,000 children aged 8 years (average: 9 cases). This report provides updated data from the ADDM Network indicating an average prevalence of ASDs in the United States approaching 1%, which is substantially higher than previously reported ADDM average estimates (4,12). The first ADDM Network reports from 2000 and 2002 indicated average identified ASD prevalence among children aged 8 years of 6.7 and 6.6 cases per 1,000 children, respectively, with one site, New Jersey, identifying prevalence of approximately 10 cases per 1,000 children in 2000 and 2002 (4,12). A recent U.S. study analyzing national survey data for 2007 of parents' reports of ASDs indicated that approximately 1% of all children aged 3--17 years and 1.3% of all children aged 6--8 years had an ASD (21). Recently published international studies have reported ASD prevalence estimates upward of 1% (12,17--20). Recent studies indicating changes in ASD prevalence are consistent in finding increases in identified ASD prevalence. However, no studies have addressed the multiple complex contributions of changes in ascertainment and potential risk factors. Because ASDs are behaviorally defined conditions identified on the basis of observation and reported symptoms, evaluations of ASD prevalence across multiple studies and methodologies are especially informative. The ADDM Network provides a systematic confirmation of documented ASD classifications and symptoms. In addition, the methodology identifies children who have documented symptoms of an ASD but have not previously received an ASD diagnosis by a community professional, increasing completeness of ASD prevalence estimates.
In general, ADDM ASD prevalence estimates were lower in sites that relied solely on health sources to identify cases compared with sites that also had access to education records. In Missouri, although investigators did not have direct access to special education evaluation records, this information could be found in the regional developmental disabilities programs, which provide evaluation and treatment coordination. Lack of access to education records appears to have had the greatest impact on identified ASD prevalence in Alabama and Florida.
Consistent with findings from previous ADDM Network reports and other studies (2--4,12), data from the 2006 surveillance year indicated that ASD prevalence was 4.5 times higher in males than in females. Among children aged 8 years, ASD prevalence was 14.5 per 1,000 males compared with 3.2 per 1,000 females. Research exploring these marked sex differences suggests differences in the developmental profiles and potential etiologies between males and females with ASDs (33). Identified ASD prevalence also varied by race/ethnicity, with some sites showing higher ASD prevalence estimates among non-Hispanic white children than among non-Hispanic black children and Hispanic children. Considerable variability has been reported across studies in the racial disparities of ASDs (33). Further examination of socioeconomic factors and subgroups of children might provide more clarity on whether racial or ethnic disparities reflect differences in ascertainment issues, environmental risk factors, and genetic susceptibility.
Children identified with an ASD in 2006 reflect a group with less co-occurring cognitive impairment than the population identified ≥20 years ago, when autism was conceptualized in a more severe and singular form compared with the spectrum of disorders identified today (2,34). In 2006, of all children with an ASD for whom testing documentation was available, 41% had cognitive impairment. When modern criteria are applied, children identified are less likely to test as having general cognitive impairments, and unusual learning profiles indicating scatter in cognitive skills rather than across-the-board cognitive delays might be more salient indicators of an ASD than intellectual impairment (35).
Children with ASDs can experience a loss of developmental skills, a plateau in development, or both. Up to 30% of children identified by ADDM Network sites as having an ASD had reports of significant skill loss or regression, usually before age 2 years, whereas up to 11% experienced a reported plateau in development early in life. These findings are consistent with those provided in previous ADDM Network reports (4,12). Incorporating descriptions of loss or plateau of skills into clinical and research practices might provide insight into the possible unique etiologic pathways leading to the developmental challenges faced by a subset of children with ASDs (36).
Changes in ASD Prevalence During 2002--2006
Data from the 10 ADDM sites with results from multiple surveillance years (4,12) indicate a significant average increase (57%) in identified ASD prevalence in 2006 compared with 2002 (range: 27%--95%). The only site not showing a statistically significant increase was Colorado; this probably was attributable to the relatively small population of children aged 8 years in the surveillance area and the slightly lower magnitude of change, limiting the power to detect change compared with other sites. On average, ASD prevalence increased across all sex, racial/ethnic, and cognitive functioning subgroups. For all sites, the most consistent pattern was the increase in identified ASD prevalence for males. Otherwise, no clear subgroup patterns emerged to reflect a consistent group that accounted for the overall increase in identified ASD prevalence across all sites.
Factors Affecting Changes in Identified ASD Prevalence
Whether the increases in identified ASD prevalence observed in the ADDM Network data are attributable to a true increase in the risk for developing ASD symptoms or solely to changes in community awareness and identification patterns is not known (2,3,37--39). Understanding the relative contribution of multiple factors is important. Because the ADDM Network identifies children with ASDs on the basis of evaluation records, the primary ways in which increased identification and awareness could account for differences in ASD prevalence across sites or over time in the same site are differences in the population from which the records were drawn, the record screening process, or the way in which social and other ASD behaviors were documented in the developmental evaluation records. One possible gauge of improved community awareness is the change in the proportion of children identified as having ASDs who received a documented ASD classification from a community professional. During 2002--2006, the proportion of children identified with an ASD for surveillance who received a documented classification of an ASD by a community professional increased in all sites and paralleled the increase observed in ADDM-identified ASD prevalence overall. Although community identification of children with ASDs increased during the study period, this factor alone does not explain fully the increase in ADDM-identified prevalence.
The widening of diagnostic criteria over time to include persons who are more mildly affected has been suggested frequently as a factor influencing increases in ASD prevalence (2,3,37--39). Although not a perfect indicator of degree of impairment severity, the broader spectrum might be represented by children who received a diagnosis from a community professional of a broader ASD subtype (i.e., Asperger disorder, PDD-NOS, or ASD or PDD, broadly defined) compared with autism (autistic disorder). However, in this analysis, a clear shift was not identified from 2002 to 2006 in the use of the more broadly defined ASD diagnoses. In fact, for several sites, increases were recorded in the use by community professionals of the autism diagnosis rather than the other ASD diagnoses. Another indicator of identifying children on the more mild end of the spectrum would be a differential increase in prevalence among children with borderline or average to above-average cognitive functioning. Although the overall pattern among these higher cognitive functioning groups indicated substantial increases in ASD prevalence, increases also were observed among children with cognitive impairment. Increases varied across sites, and a clear pattern did not emerge that would permit attributing the majority of the increase in ASD prevalence to the use of the broader ASD spectrum.
Early identification and intervention of ASD is crucial to maximizing a child's potential and quality of life. Earlier identification might influence ADDM prevalence estimates (40--45). For example, if children are being identified earlier, they might be included in the prevalence estimates when previously they would not have been. This might be particularly true for children on the milder end of the ASD spectrum. In 2002, the earliest ASD diagnosis ranged from 53--66 months, compared with 50--60 months for ASD cases in 2006. All sites reported a reduction in the median age of earliest ASD diagnosis (range: 1 month [Wisconsin]--15 months [Alabama]), with an overall trend across all sites of a reduction of approximately 5 months. Although encouraging, this trend toward earlier identification was modest and still quite delayed compared with the documented concerns about the child's development occurring before age 2 years. For children identified with an ASD by age 8 years, the reduction of age of identification does not appear to be a substantial factor influencing prevalence estimates; however, further analysis of this issue is needed.
The variation in ASD prevalence among demographic subgroups might reflect local patterns in who is evaluated for developmental concerns, in how those concerns and behaviors are documented in developmental evaluation records, and in differential risk for ASD according to these subgroups. The increase in ASD prevalence among males is not unexpected given the consistently reported sex difference, but whether this is attributable to improved identification or to increased risk among some males is not known. The greater variability among increases for females is more likely to be attributable to improved recognition of ASD symptoms among females. Differences in identified ASD prevalence by race/ethnicity have been hypothesized to reflect changes in identification patterns because no clear etiologic hypotheses have been proposed that would predict differences in ASD prevalence by race or ethnicity. The role of race/ethnicity is not independent of socioeconomic factors related to community identification patterns (33,46,47). The role of these factors as risk indicators is debated (33).
Factors related to the record review process that might affect identified ASD prevalence include the type and stability of data sources, screening criteria, and ability to locate files for review over time. Data sources were relatively stable for all sites, and although sites with access to both health and education data had higher average identified ASD prevalence, the inclusion of education sources was consistent for these sites from 2002 to 2006. Application of screening criteria also was stable within sites from 2002 to 2006. For certain sites, the ability to locate records between the two time periods differed, but this factor explained <5% of the change in prevalence in each of the sites, except South Carolina; in that site, approximately 13% of the 43% increase in prevalence during 2002--2006 could be explained by improved ability to locate records for review.
Another factor that might contribute to increases in identified prevalence is the quality and quantity of behavioral information in records. Because case determination relies on descriptions in records, the existence of greater detail in records for the 2006 study year potentially would have provided more data to confirm cases in 2006 than in 2002. Improved symptom documentation most likely is connected to increased awareness and identification; however, increased documentation based on risk cannot be ruled out. In the first ADDM Network data reports (4,12), the highest ASD prevalence in the New Jersey site was speculated to be attributable either to better symptom documentation in developmental evaluation records for that site or to a true increased prevalence. If the former were the case, other sites would be expected over time to show increases approaching the estimates in New Jersey as community awareness and service availability expand, which did occur in 2006 for all sites. Although New Jersey did not participate in the ADDM Network for 2006, the site has been collecting similar data and is working with the ADDM Network to report updated prevalence results. Therefore, whether the prevalence in New Jersey also has increased over time remains to be seen. For the sites for which data are provided in this report, an assessment of the quantity of available data indicated that the average number of evaluations abstracted per child was four in 2002 and five in 2006. The average increase of one more evaluation per child might indicate that additional documentation enabled more complete case confirmation in 2006. A qualitative assessment of differences in the information contained in developmental evaluation records suggested that the quality and amount of information contained in the evaluation records improved steadily over surveillance years, with noticeable increases in level of detail on ASD symptoms by 2006. Therefore, improved information reflected in more evaluations with more detail likely contributed to some of the increases in identified ASD prevalence.
Variation in change of residence of the base population from which records are screened also might potentially affect prevalence over time. Potential indicators include the migration patterns of children residing in the surveillance area and changes in the population of children in special education from which records were screened. For seven sites, the overall patterns indicated by the proportion of children born and still residing in the surveillance areas indicated relative stability from 2002 to 2006. The three sites (Arizona, Missouri, and North Carolina) that had the greatest increases in ASD prevalence also had the largest increases during 2002--2006 in the proportion of children who were born in and still resided in the surveillance areas at age 8 years, indicating a more stable population by 2006. The improved stability of the population might have improved the site's ability to collect adequate information to confirm ASD case status on more children in these sites; however, for the majority of sites, changes in migration patterns appear to have had a minimal influence on ASD prevalence changes.
Strengths of the ADDM Network Methodology
The systematic implementation of the ADDM Network methodology, which requires standardized training of abstractors and clinician reviewers, ongoing monitoring for quality assurance, and standardization of methods to confirm cases and conduct analyses, produces highly reliable and valid data (27). The level of detail collected and reviewed on children from multiple sources improves on previous estimates based solely on administrative records or single-source surveillance. The use of consistent methods across sites and over time has enabled researchers to begin to evaluate changes in ASD prevalence. The ADDM methods have great utility given their ability to identify children with the profile consistent with an ASD regardless of whether the child was classified as having autism for services. On the basis of ADDM data, if prevalence estimates depended solely on the documented classification of ASD, prevalence would be underestimated by 5%--22%. The ability to link ADDM data with external data sources affords the ability to examine potential risk factors beyond the scope of surveillance data alone. Routine linkages of ADDM data with birth certificate and census files enables evaluation of such potential risk factors as parental age (48), multiple births (49), and socioeconomic characteristics (33,47). In addition, determining the prevalence of children at age 8 years reduces the influence of earlier ages of identification and enables the inclusion of children whose developmental issues might not be recognized until they reach school-age (37).
Limitations
The data provided in this report are subject to at least three limitations. First, multiple factors can contribute to changes in prevalence estimates obtained through retrospective record review (27). The existence of the records, the ability to locate them, and the quantity and quality of the information in the records are all relevant issues that affect ASD prevalence using ADDM methods. Because overall prevalence was lower among the sites with access to health evaluations alone, sites that lacked access to education evaluations or to another source that provides free evaluations to the public likely underestimated ASD prevalence. In addition, sites without access to education evaluations have been unable to obtain sufficient data to examine the role of cognitive functioning among children with ASDs. These points underscore the need to improve the accessibility of education sources and evaluations. Second, the majority of sites did not include private schools, charter schools, and clinical providers or service centers with small numbers of clients. Previous reports suggest that the impact of not reviewing records of children who are private or homeschooled is minimal (27). Regardless of the type of data source access, specific data sources from 2002 to 2006 were relatively stable within all sites. Finally, direct in-person evaluation of each child to determine case status is not part of a records-based approach to surveillance. However, the surveillance approach minimizes the burden on children and their families and reduces response bias and validation of the symptom profile consistent with an ASD is verified by clinician review. In addition, CDC is conducting a validation study comparing records-based to direct evaluation methods. Although the ADDM sites were not selected to be a nationally representative sample, the population included represents a substantial number of children, >300,000 (7.9%) of all children in the United States aged 8 years in 2006.
Public Health Implications
The data in this report, which indicate prevalence of ASDs approaching approximately 1% of U.S. children aged 8 years, corroborate other recently published data (12,17--21) and confirm that ASDs are an important public health concern. The progressive increases in ASD prevalence recorded during 2002--2006 further underscore the need to understand better the risk factors and causes of these conditions. Although researchers can begin to evaluate trends with the data provided in this report, caution is urged, given the likelihood of some variation over time in prevalence of behaviorally defined conditions such as ASDs. No single factor explains the changes identified in ASD prevalence over time, and much needs to be done to understand the relative contribution of the multiple factors involved. Although some of these increases can be accounted for by improved identification and awareness, the steady increase in ASD symptoms in the population possibly reflects increased risk, particularly among males. Some progress has been reported in quantifying the effect of single factors such as reduction in age of diagnosis and inclusion of milder cases (45) or shifting in diagnostic patterns (50) on increased autism prevalence. However, these analyses are limited by the use of single-source datasets, which contain primarily data on children with autism rather than on those with the whole spectrum of ASDs. More complete datasets and complex models are needed to assess further the influence of the multiple factors discussed in this report on the changing prevalence of ASDs.
Whether identified ASD prevalence estimates will plateau or continue to increase is unknown. The ADDM cohorts in this report comprise children born in 1994 (for 2002 data) and 1998 (for 2006 data). Children born starting in the mid-to-late 1990s were particularly susceptible to the changing influence of the new DSM-IV criteria in 1994 and to increased autism awareness among the public and health professionals (2,3). The impact on estimated ASD prevalence of the broadening of diagnostic criteria and the increased awareness of ASDs might reach a high point and then diminish after a period of time. Therefore, evaluating the prevalence of ASDs among children born in this millennium using the same standard for evaluating the change in ASD symptoms over time is critical to understanding the current and changing population of children with ASDs. Of note, recent research indicates that the core social traits of autism are distributed in the population along a continuum (51); where the line is drawn between trait measures regarded as normal variance in behavior versus those labeled as impairment or disability might affect ASD prevalence estimates. The landscape of ASD diagnoses is likely to change with the introduction of the next version of the DSM expected in 2012. Efforts are needed to examine prevalence changes in other childhood conditions such as attention-deficit/hyperactivity disorder, asthma, and allergies to assess whether changes in ASD prevalence are occurring in isolation (52--54).
Efforts are needed to understand how complex genetic and environmental factors interact to result in the symptoms which make up the autism spectrum. In addition to changes in ASD prevalence by race/ethnicity, sex, and cognitive functioning, other potential risk factors (e.g., variations by urban and rural area, sociodemographic status, perinatal complications, and parental age) also need to be studied further. ADDM data are being analyzed to understand better the roles of these and other factors. Studies such as the Study to Explore Early Development, a CDC-funded study examining a wide array of risk factors for ASD are being conducted and are necessary to test hypotheses more fully. In addition, the coordination of research priorities between public and private organizations through the Interagency Autism Coordinating Committee of the National Institutes of Health and acceleration of research on ASDs highlights the need for an urgent, coordinated, and multiprong approach to ASD research.
Experienced clinicians using standardized methods can diagnose autism reliably in children as young as age 2 years, and these diagnoses tend to be stable within the ASD spectrum (55,56). These data provide further evidence (57) that a significant lag exists between earliest concerns and actual reported identification of an ASD, thus contributing to potentially significant delays in intervention. Because of the benefit of early intervention (40), identification of ASDs at earlier ages is essential to ensure that children in the United States receive optimal early intervention services. In addition to community professionals providing diagnosis, many children who did not have an ASD diagnosis recorded in their record as of 2006 were receiving special education services through an autism eligibility in the public schools. Public schools are playing a crucial role in evaluating, identifying, and serving children with ASDs. CDC is working with caregiver and professional groups through the "Learn the Signs. Act Early." public awareness campaign to provide education on the early recognition of signs of ASDs and other developmental disabilities (41). In addition, in 2007, the American Academy of Pediatrics recommended that routine screening for autism occur for all children as part of ongoing developmental screening during the 18- and 24-month well-child visits (42,43). In the future, ADDM data can be used to monitor changes in early identification that potentially result from increased education efforts.
More children than ever before are receiving services for ASDs and are having symptoms of ASDs documented in developmental evaluation records. Even without fully understanding the complex causes of this increase in identified ASD prevalence, the impact on affected children, families, and communities is substantial. Prevalence estimates can be used to plan policy, educational, and intervention services needs for persons with ASDs. In addition to continued evaluation of ASD prevalence changes, major collaborative efforts are needed to improve research into what factors put certain people at risk and how to intervene to help reduce the debilitating symptoms of ASDs. Concerted efforts are essential to address the many needs of affected persons and to provide coordinated support services which improve daily functioning and long-term life outcomes.
Acknowledgments
The Autism and Developmental Disabilities Monitoring (ADDM) Network projects were funded by CDC. Additional information about these projects is available at http://www.cdc.gov/autism.
Information in this report was provided by ADDM Network Surveillance Year 2004 and 2006 principal investigators: Beverly Mulvihill, PhD, Martha Wingate, PhD, University of Alabama, Birmingham; Russell S. Kirby, PhD, University of South Florida; Sydney Pettygrove, PhD, Chris Cunniff, MD, F. John Meaney, PhD, University of Arizona, Tucson; Lisa Miller, MD, Colorado Department of Public Health and Environment, Denver; Cordelia Robinson, PhD, University of Colorado at Denver and Health Sciences Center, Denver; Gina Quintana, Colorado Department of Education; Marygrace Yale Kaiser, PhD, University of Miami, Coral Gables, Florida; Li-Ching Lee, PhD, Johns Hopkins University, Baltimore, Maryland; Rebecca Landa, PhD, Kennedy Krieger Institute, Baltimore, Maryland; Craig Newschaffer, PhD, Drexel University, Philadelphia, Pennsylvania; John Constantino, MD, Robert Fitzgerald, MPH, Washington University in St. Louis, Missouri; Julie Daniels, PhD, University of North Carolina, Chapel Hill; Ellen Giarelli, EdD, Jennifer Pinto-Martin, PhD, University of Pennsylvania, Philadelphia: Susan E. Levy, MD, The Children's Hospital of Philadelphia, Pennsylvania; Jane Charles, MD, Joyce Nicholas, PhD, Medical University of South Carolina, Charleston; Maureen Durkin, PhD, DrPH, University of Wisconsin, Madison, Catherine Rice, PhD, Jon Baio, EdS, Kim Van Naarden Braun, PhD, Marshalyn Yeargin-Allsopp, MD, Division of Birth Defects and Developmental Disabilities, National Center on Birth Defects and Developmental Disabilities, CDC. Data collection was coordinated at each site by ADDM Network project coordinators: Meredith Hepburn, Neva Garner, University of Alabama, Birmingham; Kristen Clancy Mancilla, University of Arizona, Tucson; Andria Ratchford, MSPH, Colorado Department of Public Health and Environment, Denver; Yolanda Castillo, MBA, Colorado Department of Education; Maria Kolotos, Johns Hopkins University, Baltimore, Maryland; Rob Fitzgerald, MPH, Washington University in St. Louis, Missouri; Paula Bell, University of North Carolina, Chapel Hill; Rachel Meade, University of Pennsylvania, Philadelphia; Lydia King, PhD, Medical University of South Carolina, Charleston; Carrie Arneson, MS, University of Wisconsin, Madison; Anita Washington, MPH, Research Triangle Institute, Atlanta, Georgia; Susan Graham, MSPH, Division of Birth Defects and Developmental Disabilities, CDC. Additional assistance was provided by project staff including data abstractors, clinician reviewers, epidemiologists, and data management/programming support stff. Ongoing ADDM Network support was provided by Rita Lance, Northrup Grummon, contractor to CDC; Lori Plummer, Lekeisha Jones, Research Triangle Institute, contractors to CDC; Joanne Wojcik, Nancy Doernberg, National Center on Birth Defects and Developmental Disabilities, CDC.
References
- Yeargin-Allsopp M, Rice C, Karapurkar T, Doernberg N, Boyle C, Murphy C. Prevalence of autism in a US metropolitan area. JAMA 2003;289:49--55.
- Rutter, M. Incidence of autism spectrum disorders: changes over time and their meaning. Acta Paediatrica 2005;94:2--15.
- Fombonne E. Epidemiology of pervasive developmental disorders. Pediatric Res 2009;65:591--8.
- CDC. Prevalence of autism spectrum disorders---Autism and Developmental Disabilities Monitoring Network, six sites, United States, 2000. In: Surveillance Summaries, February 9, 2007. MMWR 2007;56(No. SS-1):1--11.
- California Department of Developmental Services. Changes in the population of persons with autism and pervasive developmental disorders in California's Developmental Services System, 1987 through 1998: a report to the Legislature. Sacramento, CA: California Department of Developmental Services; 1999.
- Croen LA, Grether JK, Hoogstrate J, Selvin S. The changing prevalence of autism in California. J Autism Dev Disord 2002;32:207--15.
- US Department of Education. Number of children served under IDEA by disability and age group, during the 1989--1990 through 1998--1999 school years. To assure the free appropriate public education of all children with disabilities: twenty-second annual report to Congress on the implementation of the Individuals with Disabilities Education Act. Washington, DC: US Department of Education; 2000:11--20.
- Newschaffer C, Falb M, Gurney J. National autism prevalence trends from United States special education data. Pediatrics 2005;115:277--82.
- California Department of Developmental Services. Changes in the CA caseload: an update June 1987 through June 2007. Sacramento, CA: California Department of Developmental Services; 2007. Available at http://www.dds.ca.gov/Autism/docs/AutismReport_2007.pdf. Accessed December 7, 2009.
- Hertz-Picciotto E, Delwiche L. The rise in autism and the role of age at diagnosis. Epidemiology 2009;20:84--90.
- Individuals with Disabilities Education Act (IDEA) Data. Washington, DC: US Department of Education, Office of Special Education Programs; 2009. Number of children served under IDEA by disability and age group through 2007. Available at https://www.ideadata.org/PartBData.asp. Accessed December 7, 2009.
- CDC. Prevalence of autism spectrum disorders---Autism and Developmental Disabilities Monitoring Network, 14 sites, United States, 2002. In: Surveillance Summaries, February 9, 2007. MMWR 2007;56(No. SS-1):12--28.
- Fombonne E. Is there an epidemic of autism? Pediatrics 2001;107:411--2.
- Laidler JR. US department of education data on "autism" are not reliable for tracking autism prevalence. Pediatrics 2005;116:120--4.
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed., text revision of 1994 edition. Washington, DC: American Psychiatric Association; 2000.
- World Health Organization. International classification of disease. 10th ed. Geneva, Switzerland: World Health Organization; 1990.
- Baird G, Simonoff E, Pickles A, et al. Prevalence of disorders of the autism spectrum in a population cohort of children in South Thames: the Special Needs and Autism Project (SNAP). Lancet 2006;368:210--5.
- Honda H, Shimizu Y, Imai M, Nitto Y. Cumulative incidence of childhood autism: a total population study of better accuracy and precision. Dev Med Child Neur 2005;47:10--8.
- Kadesjo B, Gillberg C, Hagberg B. Brief report: autism and Asperger Syndrome in seven-year-old children: a total population study. J Autism Dev Disord 1999;29:327--31.
- Baron-Cohen S, Scott FJ, Allison C, et al. Prevalence of autism spectrum conditions: UK school-based population study. Br J Psychiatry 2009;194:500--9.
- Kogan MD, Blumberg SJ, Schieve LA, et al. The prevalence of parent-reported diagnosis of autism spectrum disorder among children in the United States, 2007. Pediatrics 2009. [Epub.] Available at http://pediatrics.aappublications.org/cgi/reprint/124/5/1395. Accessed December 7, 2009.
- Posserud MB, Lundervold AJ, Gillberg C. Autistic features in a total population of 7--9-year-old children assessed by the ASSQ (Autism Spectrum Screening Questionnaire). J Child Psychol Psychiatry 2006;47:167--75.
- Rice CE, Baio J, Van Naarden Braun K, Doernberg N, Meaney F J, Kirby RS for the ADDM Network. A public health collaboration for the surveillance of autism spectrum disorders. Paediatr Perinat Epidemiol 2007;21:179--90.
- Bertrand J, Mars A, Boyle C, Bove F, Yeargin-Allsopp M, Decoufle P. Prevalence of autism in a United States population: the Brick Township, New Jersey, investigation. Pediatrics 2001;108:1155--61.
- Yeargin-Allsopp M, Murphy C, Oakley G, Sikes K. A multiple-source method for studying the prevalence of developmental disabilities in children: the Metropolitan Atlanta Developmental Disabilities Study. Pediatrics 1992;89:624--30.
- CDC. Prevalence of selected developmental disabilities in children 3--10 years of age: the Metropolitan Atlanta Developmental Disabilities Surveillance Program, 1991. In: Surveillance Summaries, April 19, 1996. MMWR 1996;45(No. SS-2):1--14.
- CDC. Evaluation of a methodology for a collaborative multiple source surveillance network for autism spectrum disorders---Autism and Developmental Disabilities Monitoring Network, 14 sites, United States, 2002. In: Surveillance Summaries, February 9, 2007. MMWR;56(No. SS-1):29--40.
- CDC, National Center for Health Statistics. Estimates of the July 1, 2000--July 1, 2007, United States resident population from the vintage 2007 postcensal series by year, county, age, sex, race, and Hispanic origin, prepared under a collaborative arrangement with the U.S. Census Bureau. Bethesda, MD: US Department of Health and Human Services, CDC, National Center for Health Statistics; 2007. Available at: http://www.cdc.gov/nchs/nvss/bridged_race/data_documentation.htm#vintage2007. Accessed December 7, 2009.
- World Health Organization. International statistical classification of diseases and related health problems, ninth revision, clinical modification, ICD-9-CM. 4th ed. Geneva, Switzerland: World Health Organization; 1997.
- Selvin S. Statistical power and sample-size calculations. In: Selvin S, ed. Statistical analyses of epidemiologic data. 2nd ed. New York, NY: Oxford University Press; 1996.
- SAS, Inc. SAS for Windows, Rel. 9.1. Cary, NC: SAS Institute Inc.; 2004.
- SPSS, Inc. SPSS for Windows, Rel. 13. Chicago, IL: SPSS Inc.; 2005.
- Newschaffer C, Croen LA, Daniels J, et al. The epidemiology of the autism spectrum disorders. Annu Rev of Public Health 2007;28:235--58.
- Chakrabarti S, Fombonne E. Pervasive developmental disorders in preschool children. JAMA 2001;285:3093--9.
- Losh M, Adolphs R, Poe MD, et al. Neuropsychological profile of autism and the broad autism phenotype. Arch Gen Psychiatry 2009;66:518--26.
- Lord C, Shulman C, DiLavore P. Regression and word loss in autistic spectrum disorders. J Child Psychol and Psychiatry 2004;45:936--55.
- Fombonne E. The prevalence of autism. JAMA 2003;289:87--9.
- Charman T. The prevalence of the autism spectrum disorders: recent evidence and future challenges. Eur Child Adoles Psychiatry 2002;11:249--56.
- Posserud M, Lundervold AJ, Lie SA, Gillberg C. The prevalence of autism spectrum disorders: impact of diagnostic instrument and non-response bias. Soc Psychiatry Psychiatr Epidemiol 2009. [Epub]. Available at http://www.springerlink.com/content/650012524603240p. Accessed December 7, 2009.
- National Research Council, Committee on Educational Interventions for Children with Autism, Division of Behavioral and Social Sciences and Education. Educating children with autism. Washington, DC: National Academy Press; 2001.
- CDC. Learn the signs. Act early. Atlanta, GA: US Department of Health and Human Services, CDC; 2006. Available at http://www.cdc.gov/actearly. Accessed December 7, 2009.
- American Academy of Pediatrics Council on Children with Disabilities. Identifying infants and young children with developmental disorders in the medical home: an algorithm for developmental surveillance and screening. Pediatrics 2006;118:405--20.
- Johnson CP, Myers SM; American Academy of Pediatrics Council on Children With Disabilities. Identification and evaluation of children with autism spectrum disorders. Pediatrics 2007;120:1183--215.
- Parner E, Schendel D, Thorsen P. Autism prevalence trends over time in Denmark: changes in prevalence and age at diagnosis. Arch Pediatr Adolesc Med 2008;162:1150--6.
- Hertz-Picciotto I, Delwiche L. The rise in autism and the role of age at diagnosis. Epidemiology 2009;20:84--90.
- Mandell DS, Listerud J, Levy S, Pinto-Martin J. Race differences in the age of diagnosis among Medicaid-eligible children with autism. J Am Acad Child Adolesc Psychiatry 2002;41:1447--53.
- Mandell DS, Wiggins LD, Carpenter LA, et al. Racial/ethnic disparities in the identification of children with autism spectrum disorders. Am J Public Health. 2009;99:493--8.
- Durkin MS, Maenner MJ, Newschaffer CJ, et al. Advanced parental age and the risk of autism spectrum disorder. Am J Epidemiol 2008;168:1268--76.
- Van Naarden Braun K, Schieve L, Daniels J, et al. Relationships between multiple births and autism spectrum disorders, cerebral palsy, and intellectual disabilities: Autism and Developmental Disabilities Monitoring (ADDM) Network---2002 Surveillance Year. Autism Res 2008;1:265--316.
- King M, Bearman P. Diagnostic change and the increased prevalence of autism. Int J Epidemiol 200938:1224--34.
- Constantino JN, Todd RD. Autistic traits in the general population: a twin study. Arch Gen Psychiatry 2003;60:524--30.
- Atladóttir H, Parner E, Schendel D, Dalsgaard S, Thomsen P, Thorsen P. Time trends in reported diagnoses of childhood neuropsychiatric disorders: a Danish cohort study. Arch Pediatr Adolesc Med 2007;161:193--8.
- Woodruff TJ, Axelrad DA, Kyle AD, Nweke O, Miller GG, Hurley BJ. Trends in environmentally related childhood illnesses. Pediatrics 2004;113:1133--40.
- Pallapies, D. Trends in childhood disease. Mutat Res 2006;608:100--11.
- Lord C, Risi S, DiLavore PS, Shulman C, Thurm A, Pickles A. Autism from 2 to 9 years of age. Arch Gen Psychiatry 2006;63:694--701.
- Van Daalen E, Kemner C, Dietz C, Swinkels SH, Buitelaar JK, Van Engeland H. Inter-rater reliability and stability of diagnoses of autism spectrum disorder in children identified through screening at a very young age. Eur Child Adolesc Psychiatry 2009. [Epub]. Available at http://www.springerlink.com/content/b57406752324wjk6. Accessed December 7, 2009.
- Wiggins L, Baio J, Rice C. Examination of the time between first evaluation and first autism spectrum diagnosis in a population-based sample. J Dev Behav Pediatr 2006;27(2 Suppl):S79--87.
* Areas of Arizona, Georgia, Maryland, New Jersey, South Carolina, and West Virginia.
†Areas of Alabama, Arizona, Arkansas, Colorado, Georgia, Maryland, Missouri, New Jersey, North Carolina, Pennsylvania, South Carolina, Utah, West Virginia, and Wisconsin.
§ Areas of Alabama (32 counties in north and central Alabama), Arizona (one county, including metropolitan Phoenix), Colorado (1 county in metropolitan Denver), Florida (one southern county), Georgia (the CDC site in five counties in metropolitan Atlanta), Maryland (six counties in suburban Baltimore), Missouri (five counties in metropolitan St. Louis), North Carolina (10 central counties), Pennsylvania (one county in metropolitan Philadelphia), South Carolina (23 counties in the Coastal and PeeDee regions), and Wisconsin (10 counties in south eastern Wisconsin).
¶Areas of Alabama, Arizona, Georgia, Maryland, Missouri, North Carolina, South Carolina, and Wisconsin.
FIGURE 1. Surveillance methodology flowchart --- Autism and Developmental Disabilities Monitoring (ADDM) Network, United States
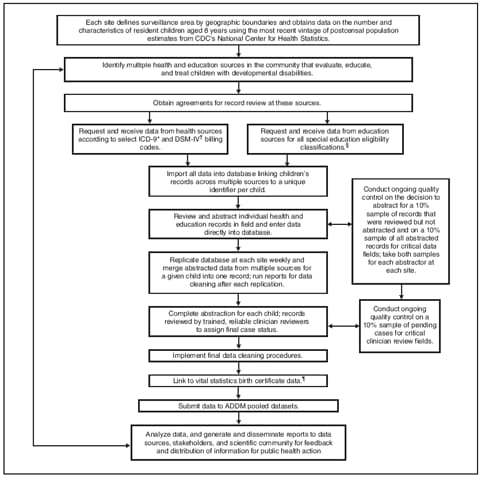
* International Classification of Diseases, 9th Revision.
† Diagnostic and Statistical Manual of Mental Disorders, 4th Edition, Text Revision.
§ All ADDM sites conducting cerebral palsy surveillance are conducting linkage of cases with vital statistics death certificates. If feasible, sites conducting ASD and intellectual development surveillance also conducted this death certificate linkage. For sites that completed this linkage no ASD cases were identified.
¶ Georgia and North Carolina did not review special education records of children whose only exceptionality was speech and language impairment (SLI). A sample of children in SLI indicated that this decision had minimal effect on prevalence estimates.
Alternate Text: This figure presents a step-by-step flowchart indicating the methods used to collect data on autism spectrum disorders in the ADDM Network surveillance sites and to submit these data to ADDM pooled datasets.
|
TABLE 1. Number* and percentage of children aged 8 years, by race/ethnicity and site --- Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2006 |
||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Site |
Site institution |
Surveillance area |
Total |
Non-Hispanic, white |
Non-Hispanic, black |
Hispanic |
API† |
AI/AN§ |
% receiving special education¶ |
% abstracted for ASD** |
No. of evaluations abstracted Median (range) |
|||||
|
No. |
No. |
(%) |
No. |
(%) |
No. |
(%) |
No. |
(%) |
No. |
(%) |
||||||
|
Sites with access to health records |
||||||||||||||||
|
Alabama |
Univ of Alabama--Birmingham |
32 counties in north and central Alabama |
35,126 |
23,967 |
(68.2) |
9,028 |
(25.7) |
1,607 |
(4.6) |
371 |
(1.1) |
153 |
(0.4) |
16.7 |
1.2 |
5 (1--32) |
|
Florida |
Univ of Miami |
1 county (Miami-Dade) in south Florida |
27,615 |
6,422 |
(23.3) |
6,267 |
(22.7) |
14,443 |
(52.3) |
429 |
(1.6) |
54 |
(0.2) |
11.8 |
0.5 |
3 (1--17) |
|
Missouri |
Washington Univ--St. Louis |
5 counties including metropolitan St. Louis |
26,533 |
18,199 |
(68.6) |
6,702 |
(25.3) |
777 |
(2.9) |
773 |
(2.9) |
82 |
(0.3) |
17.6 |
1.8 |
4 (1--17) |
|
Pennsylvania |
Univ of Pennsylvania |
1 county (Philadelphia) in metropolitan Philadelphia |
17,886 |
5,048 |
(28.2) |
8,969 |
(50.1) |
2,852 |
(15.9) |
959 |
(5.4) |
58 |
(0.3) |
13.0 |
1.9 |
7 (1--41) |
|
Wisconsin |
Univ of Wisconsin --Madison |
10 counties in south eastern Wisconsin |
34,058 |
22,361 |
(65.7) |
6,157 |
(18.1) |
4,153 |
(12.2) |
1,206 |
(3.5) |
181 |
(0.5) |
15.0 |
1.7 |
6 (1--61) |
|
Sites with access to education and health records |
||||||||||||||||
|
Arizona |
Univ of Arizona |
1 county (Maricopa) in metropolitan Phoenix |
41,650 |
19,664 |
(47.2) |
2,244 |
(5.4) |
17,577 |
(42.2) |
1,236 |
(3.0) |
926 |
(2.2) |
16.7 |
2.2 |
5 (1--19) |
|
Colorado |
Colorado Dept of Public Health and Environment |
1 county (Arapahoe) in metropolitan Denver |
7,184 |
4,009 |
(55.8) |
963 |
(13.4) |
1,761 |
(24.5) |
411 |
(5.7) |
40 |
(0.6) |
10.7 |
1.5 |
5 (2--23) |
|
Georgia |
CDC |
5 counties including metropolitan Atlanta |
46,621 |
17,871 |
(38.3) |
19,877 |
(42.6) |
6,015 |
(12.9) |
2,710 |
(5.8) |
148 |
(0.3) |
11.3 |
2.4 |
4 (1-26) |
|
Maryland |
Johns Hopkins Univ |
6 counties in suburban Baltimore |
26,489 |
18,464 |
(69.7) |
5,601 |
(21.1) |
1,109 |
(4.2) |
1,246 |
(4.7) |
69 |
(0.3) |
12.6 |
1.3 |
2 (1-8) |
|
North Carolina |
Univ of North Carolina--Chapel Hill |
10 counties in central North Carolina |
22,195 |
12,727 |
(57.3) |
6,160 |
(27.8) |
2,618 |
(11.8) |
627 |
(2.8) |
63 |
(0.3) |
13.6 |
1.7 |
5 (1--18) |
|
South Carolina |
Medical Univ of South Carolina |
23 counties in the Coastal and Pee Dee regions |
22,681 |
12,153 |
(53.6) |
9,061 |
(39.9) |
1,053 |
(4.6) |
282 |
(1.2) |
132 |
(0.6) |
15.9 |
1.3 |
5 (1--28) |
|
* Total numbers of children aged 8 years in each study area were obtained from CDC's National Center for Health Statistics (NCHS) vintage 2007 postcensal population estimates. Surveillance area denominator excludes those school districts that did not participate. † Asian/Pacific Islander. § American Indian/Alaska Native. ¶ Number of students in special education and total enrolled in districts in surveillance area for the 2005--2006 school year obtained from http:/www.nces.ed.gov. ** Autism spectrum disorder. Represents the number of children identified as possibly having an ASD divided by the total number of children aged 8 years in the population. |
||||||||||||||||
|
Site |
Race/ethnicity |
Prev ratio |
|||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
|
White, non-Hispanic, |
Black, non-Hispanic |
Hispanic |
API** |
||||||||
|
White-to-black |
White-to-Hispanic |
Black-to-Hispanic |
|||||||||
|
Prev |
95% CI |
Prev |
95% CI |
Prev |
95% CI |
Prev |
95% CI |
||||
|
Sites with access to health records |
|||||||||||
|
Alabama |
5.8 |
(5.0--6.9) |
6.8 |
(5.3--8.7) |
0.6 |
(0.1--4.4) |
2.7 |
(0.4--19.1) |
0.9 |
9.4†† |
10.9§§ |
|
Florida |
3.4 |
(2.3--5.2) |
1.6 |
(0.9--3.0) |
5.2 |
(4.1--6.5) |
---¶¶ |
--- |
2.1†† |
0.7 |
0.3 |
|
Missouri |
13.7 |
(12.1--15.5) |
5.1 |
(3.6--7.1) |
2.6 |
(0.6--10.3) |
7.8 |
(3.5--17.3) |
2.7§§ |
5.3†† |
2.0 |
|
Pennsylvania |
10.1 |
(7.7--13.3) |
7.5 |
(5.9--9.5) |
7.7 |
(5.1--11.7) |
1.0 |
(0.2--7.4) |
1.4 |
1.3 |
1.0 |
|
Wisconsin |
8.5 |
(7.4--9.8) |
3.6 |
(2.4--5.4) |
1.7 |
(0.8--3.5) |
5.8 |
(2.8--12.2) |
2.4§§ |
5.1§§ |
2.1 |
|
Sites with access to education and health records |
|||||||||||
|
Arizona |
14.8 |
(13.1--16.6) |
12.9 |
(9.0--18.6) |
8.3 |
(7.0--9.7) |
16.2 |
(10.4--25.1) |
1.1 |
1.8§§ |
1.6†† |
|
Colorado |
6.7 |
(4.6--9.8) |
12.5 |
(7.1--21.9) |
4.5 |
(2.3--9.1) |
7.3 |
(2.4--22.6) |
0.5 |
1.5 |
2.8†† |
|
Georgia |
12.0 |
(10.5--13.8) |
9.5 |
(8.2--10.9) |
4.8 |
(3.4--6.9) |
7.8 |
(5.1--11.9) |
1.3†† |
2.5§§ |
2.0§§ |
|
Maryland |
9.3 |
(8.0--10.8) |
7.9 |
(5.9--10.6) |
6.3 |
(3.0--13.2) |
9.6 |
(5.5--17.0) |
1.2 |
1.5 |
1.2 |
|
North Carolina |
12.2 |
(10.4--14.3) |
7.5 |
(5.6--10.0) |
6.1 |
(3.7--10.0) |
4.8 |
(1.5--14.8) |
1.6§§ |
2.0§§ |
1.2 |
|
South Carolina |
7.1 |
(5.7--8.7) |
7.3 |
(5.7--9.3) |
4.8 |
(2.0--11.4) |
3.6 |
(0.5--25.2) |
1.0 |
1.5 |
1.5 |
|
* Per 1,000 children aged 8 years. † All children are included in the total regardless of race or ethnicity. The total also includes children for whom race/ethnicity was unknown. § All male-to-female ratios different within sites (p<0.01). ¶ Confidence interval. ** Asian/Pacific Islander. †† Prevalence ratio significantly different within site (p<0.05). §§ Prevalence ratio significantly different within site (p<0.01). ¶¶ No children identified in this group. |
|||||||||||
FIGURE 2. Overall prevalence* of autism spectrum disorders (ASDs) among children aged 8 years and prevalence of ASDs among children with a previously documented ASD classification,† by source type and order of ASD prevalence --- Autism and Developmental Disabilities Monitoring (ADDM) Network, 11 sites, United States, 2006
![Among all children meeting the ADDM ASD surveillance case definition, approximately 77% had a documented ASD classification in their records (range: 65% [Arizona]-93% [Maryland]). Overall prevalence estimates based on ADDM methods were higher than those based on an ASD classification documented by a community professional in the records.](figures/s810a1f2.gif)
* Per 1,000 population.
† Children were classified as having a previously documented ASD classification if they had 1) received a diagnosis of autistic disorder, pervasive developmental disorder (PDD)--not otherwise specified, Asperger syndrome, PDD, or ASD by a qualified professional that was documented in an evaluation record or 2) had received special education services under an autism eligibility category.
Alternate Text: Among all children meeting the ADDM ASD surveillance case definition, approximately 77% had a documented ASD classification in their records (range: 65% [Arizona]-93% [Maryland]). Overall prevalence estimates based on ADDM methods were higher than those based on an ASD classification documented by a community professional in the records.
FIGURE 3. Intelligence quotient (IQ) of children aged 8 years with an autism spectrum disorder (ASD) for whom psychometric test data were available,* by site, sex, and IQ score --- Autism and Developmental Disabilities Monitoring Network, 11 sites, United States, 2006
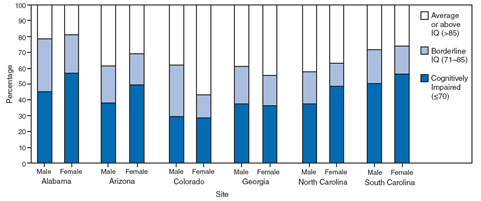
*Sites with psychometric test data on ≥70% of children identified with an ASD were included.
Alternate Text: Data on cognitive functioning are reported for sites having IQ test scores available on at least 70% of children who met the ASD case definition. The proportion of children with ASDs who had test scores indicating cognitive impairment (IQ <70) ranged from 29.3% in Colorado to 51.2% in South Carolina North Carolina, and South Carolina), a higher proportion of females with ASDs had cognitive impairment compared with males.
FIGURE 4. Change in prevalence* of autism spectrum disorders (ASDs) among children aged 8 years, by classification type --- Autism and Developmental Disabilities Monitoring Network (ADDM), 10 sites, United States, 2002 and 2006
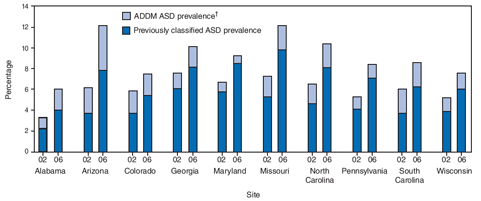
* Per 1,000 children aged 8 years in the surveillance area.
† ADDM ASD prevalence is indicated by the entire bar.
Alternate Text: During 2002-2006, the proportion of children who met the ASD case definition and had a previously documented ASD classification in their records increased <5%, on average, across the 10 sites, from 72% in 2002 to 77% in 2006. Within sites, this increase ranged from <1% in Alabama and Georgia to >15% in Colorado. Average ASD prevalence based on documented ASD classification in records increased 64% (from 4.4 to 7.2 per 1,000 population), paralleling the 57% increase in ADDM-identified ASD prevalence estimates.
FIGURE 5. Change in subtype of autism spectrum disorder (ASD) as documented in evaluation records, by year --- Autism and Developmental Disabilities Monitoring Network, 10 sites, United States, 2002 and 2006
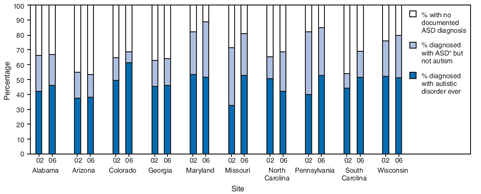
* Includes documented diagnoses of Asperger disorder, Pervasive Developmental Disorder--Not Otherwise Specified, Autism Spectrum Disorder or Pervasive Developmental Disorder, or an International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) code of 299.8.
Alternate Text: In 2002, an average of 44.9% (range: 32.7%-52.5%) of children with ADDM-identified ASD had ever received an autism diagnosis compared with 47% (range: 38.1%-61.1%) in 2006. For all those who received ASD diagnoses other than autism, no overall change was observed across all sites, with an average of 23.7% (range: 9.3%-39%) in 2002 and 23.8% (range: 7.4%-37%) in 2006.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services. |
All MMWR HTML versions of articles are electronic conversions from typeset documents. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Date last reviewed: 12/10/2009


