 |
|
|
|
|
|
|
| ||||||||||
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
|
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail. Progress Toward Poliomyelitis Eradication --- Angola and the Democratic Republic of Congo, January 2002--June 2003Since the World Health Assembly resolved in 1988 to eradicate poliomyelitis worldwide, the estimated global incidence of polio has decreased by 99% (1). Implementation of polio eradication activities in Angola and the Democratic Republic of Congo (DRC) began in 1996. Angola and DRC are characterized by large geographic areas, dense urban populations, recent civil conflict, and a history of polio outbreaks (2--5). This report summarizes progress made toward polio eradication during January 2002--June 2003 and highlights the remaining challenges in Angola and DRC. Routine VaccinationIn Angola, reported national routine vaccination coverage of infants aged <12 months with 3 doses of oral poliovirus vaccine (OPV3) was 33% in 2000, 44% in 2001, and 42% in 2002 (Angola Ministry of Health, unpublished data, 2003). In DRC, reported national routine OPV3 coverage was 42% in 2000, 33% in 2001, and 45% in 2002 (DRC Ministry of Health, unpublished data, 2003). Supplementary Immunization ActivitiesSince 1996, supplementary immunization activities (SIAs) targeting children aged <5 years for vaccination with OPV have been conducted annually in Angola and DRC. During January 2002--May 2003, Angola implemented three rounds of National Immunization Days* (NIDs) and one round of subnational immunization days† (SNIDs) using house-to-house vaccination. The May 2002 SNID targeted 40 municipalities with high-risk areas and reached approximately 2.8 million children aged <5 years, including persons living in 28 camps for internally displaced persons (IDPs) and in five quartering areas for former combatants and their families (4). High-risk areas were identified on the basis of various indicators, including high population density, concentration of IDPs, history of inaccessibility during the war, low vaccination coverage during the 2001 NIDs, proximity to Angolan refugee populations in Zambia and DRC, and detection of wild poliovirus (WPV) in 2001. During June--August 2002, Angola conducted three rounds of NIDs, reaching approximately 4.5 million children aged <5 years during each round, in synchronization with NIDs conducted in DRC, Republic of Congo, Gabon, Zambia, Namibia, and Sao Tomé and Principe. During July--August 2003, Angola conducted two monthly rounds of NIDs. During June--August 2002, DRC implemented three monthly rounds of NIDs, reaching approximately 12.5 million children aged <5 years during each round. During July--August 2003, two monthly rounds of SNIDs targeting high-risk areas were conducted in DRC. High-risk areas were identified on the basis of surveillance indicators, including clustering of polio-compatible cases, low vaccination coverage during the 2002 NIDs, and detection of WPV in 2000. Acute Flaccid Paralysis SurveillanceThe quality of public health surveillance for cases of acute flaccid paralysis (AFP) is evaluated by two key indicators established by the World Health Organization: annual reporting rate (target: nonpolio AFP rate of >1 case per 100,000 children aged <15 years) and completeness of specimen collection (target: two adequate stool specimens from >80% of persons with AFP). In 2002, the nonpolio AFP rate in Angola was 3.0 (Table). All 18 provinces achieved nonpolio AFP rates of >1.0. Although the geographic distribution of AFP cases detected in 2002 in western Angola was proportionate to population density, gaps existed in case detection in the central and eastern provinces (Figure). AFP cases were reported primarily from municipal centers. No cases were reported from several subprovincial areas bordering Zambia and DRC in which access and security are concerns. In 2002, the proportion of cases of persons for whom two adequate stool specimens were collected was 85%. During January--June 2003, the annualized nonpolio AFP rate was 1.4, with 13 (72%) of 18 provinces reporting at least one AFP case. Adequate stool specimens were collected from 84% of persons with AFP. The nonpolio enterovirus (NPEV) isolation rate, a combined indicator for quality of specimen transport and sensitivity of laboratory processing, was 19.3% in 2002 and 33.0% during January--June 2003 (target: >10%). AFP cases in which paralytic polio could not be reliably excluded were classified as polio-compatible. In 2002, of 186 AFP cases reported, the Angola national polio expert committee classified 17 (9%) as polio-compatible. As of June 30, no AFP cases reported in 2003 were classified polio-compatible. In 2002, the nonpolio AFP rate in DRC was 5.0, with all 11 provinces achieving nonpolio AFP rates of >1.0. During January--June 2003, the annualized nonpolio AFP rate was 3.3, with all 11 provinces reporting at least one AFP case. The proportion of AFP cases in persons for whom two adequate specimens were collected was 84% in 2002 and 92% during January--June 2003. The NPEV isolation rate for DRC was 17.5% in 2002 and 12.0% during January--June 2003. In 2002, the DRC national polio expert committee classified 59 (5%) of 1,239 AFP cases as polio-compatible; Orientale province, a site of ongoing conflict in which approximately 15% of the population reside, accounted for 24 (41%) of these 59 cases. Specimens from four (17%) of these 24 persons arrived at the laboratory in poor condition, and a single specimen existed for another case. For the remaining 19 patients with polio-compatible disease, the average time from onset of paralysis to collection of two specimens was 24 days (range: 15--37 days); for 14 (74%) patients, the period between onset of paralysis and notification was >14 days. As of July 29, one person with AFP had been classified as having polio-compatible disease during January--June 2003. Incidence of PolioDuring December 2001--February 2002, five cases of polio with isolation of WPV type 1 (P1) were detected among Angolan refugees in Western Zambia. Genetic sequencing confirmed that these isolates were related to WPV strains isolated most recently in Angola and DRC (4). The last laboratory-confirmed WPV in Angola was a P1 virus isolated in September 2001 from a person with AFP in Lunda Sul province. In 2000, a P1 outbreak in the Cape Verde islands was identified by genetic sequence analysis to have been imported from Angola (6). In 1999, a polio outbreak caused primarily by WPV type 3 affected approximately 1,100 Angolan children (4,5). In 2000, a total of 28 cases of laboratory-confirmed WPV in DRC were identified. The most recent laboratory-confirmed case of WPV was a P1 virus isolated in December 2000 from a person with AFP from Kasai Oriental province. Reported by: Ministry of Health; Country Office of the World Health Organization, Luanda, Angola. Ministry of Health; Country Office of the World Health Organization, Kinshasa, Democratic Republic of Congo. Regional Office of the World Health Organization for Africa, Harare, Zimbabwe. Vaccines and Biologicals Dept, World Health Organization, Geneva, Switzerland. Div of Viral and Rickettsial Diseases, National Center for Infectious Diseases; Global Immunization Div, National Immunization Program, CDC. Editorial Note:Progress toward polio eradication has continued in both Angola and DRC despite armed conflict. During January 2002--June 2003, both countries met or exceeded WHO-recommended standards of surveillance quality at national and provincial levels. The absence of laboratory-confirmed WPV for the preceding 21 months in Angola and for the preceding 30 months in DRC under conditions of adequate surveillance suggests that Angola and DRC have made substantial progress toward the interruption of WPV transmission. Although a cease-fire agreement ending 27 years of civil war in Angola was signed in April 2002, a legacy remains of devastated infrastructure, landmines, and displaced populations, particularly in the central and eastern provinces. Access has improved to areas never before covered by SIAs or AFP surveillance, but operations are still difficult to implement, and access in the southeastern provinces remains problematic. Although Angola achieved a nonpolio AFP rate of >1.0 in all 18 provinces in 2002, surveillance gaps exist at the subprovincial level in some areas of the eastern half of the country, and the possibility of low-grade polio virus transmission cannot be excluded. Because of the return of IDPs who had sought refuge in urban centers during the war, delivery of services to areas that were inaccessible previously should be a priority. Approximately 400,000 Angolan refugees reside in Zambia and DRC (United Nations High Commissioner for Refugees, unpublished data, 2003). The detection of WPV from five unvaccinated children of Angolan refugees in western Zambia highlights the potential for circulation of poliovirus in these poorly vaccinated, high-risk populations. Vaccination and surveillance activities should be supported and extended, particularly in areas where refugees or IDPs are likely to settle or congregate. Although a peace accord ending >4 years of civil war in DRC was signed in April 2003, ethnic conflict continues in the northeastern part of the country, particularly in the Ituri region of Orientale province and in North Kivu province. As of January 2003, approximately 1.6 million IDPs resided in these provinces (United Nations Office for Coordination of Humanitarian Affairs, unpublished data, 2003). A substantial number of AFP cases detected in Orientale province in 2002 were classified as polio-compatible, primarily because of delayed notification and poor specimen condition. These compatible cases might be attributable to suboptimal surveillance because of the war, but uncertainty about possible low-grade poliovirus transmission exists. With the cessation of hostilities nationwide, the potential exists for improvement of surveillance quality in areas such as Orientale province. The aftermath of civil war in DRC poses a challenge to sustaining the gains made in polio eradication. Low routine vaccination coverage and the decision to implement only SNIDs might compromise the attainment of levels of population immunity required to ensure protection against a re-emergence of endemic poliovirus transmission. Maintaining the highest quality surveillance uniformly within provinces and improving routine vaccination coverage are key priorities, particularly because the number and geographic scope of SIAs are being scaled down. Angola and its development partners have embarked on a phase of national reconstruction, and DRC has launched a representative interim government. To ensure that political commitment to polio eradication is maintained, every effort should be made to ensure that polio eradication remains a national priority. Sustained commitment from the national governments and donors§ is critical for polio to be eradicated in Angola and the DRC. References
* Mass campaigns over a short period (days) in which 2 doses of OPV are administered to all children in the target group (usually those aged <5 years) regardless of previous vaccination history. † Campaigns similar to NIDs but confined to part of the country. § Polio eradication efforts in Angola and DRC are supported by the governments of Angola, DRC, Belgium, Italy, Japan, and the Netherlands; the Department for International Development, United Kingdom; the Bill and Melinda Gates Foundation; the United Nations Foundation; Aventis Pasteur; DeBeers; the United Nations Children's Fund (UNICEF); Rotary International; the U.S. Agency for International Development; the Canadian International Development Agency; WHO; and CDC. Table  Return to top. Figure 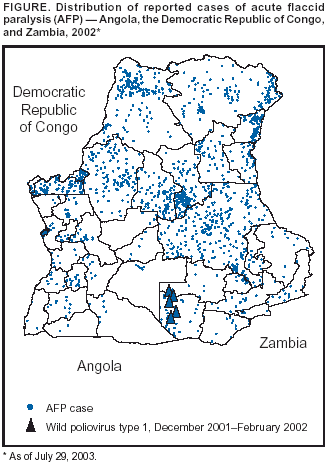 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 8/28/2003 |
|||||||||
This page last reviewed 8/28/2003
|