

|

|

Volume
8: No. 6, November 2011
ORIGINAL RESEARCH
The Predicted Impact of Heart Disease Prevention and Treatment Initiatives on
Mortality in Lithuania, a Middle-Income Country
Thomas E. Kottke, MD, MSPH; Lina Jancaityte, MD; Abdonas
Tamosiunas, PhD; Vilius Grabauskas, DrSc
Suggested citation for this article: Kottke TE, Jancaityte L,
Tamosiunas A, Grabauskas V. The predicted impact of heart disease prevention and
treatment initiatives on mortality in Lithuania, a middle-income country. Prev
Chronic Dis 2011;8(6):A139.
http://www.cdc.gov/pcd/issues/2011/nov/10_0198.htm.
Accessed [date].
PEER REVIEWED
Abstract
Introduction
Disease-prevention programs compete with disease-treatment programs for
scarce resources. This analysis predicts the impact of heart disease prevention
and treatment initiatives for Lithuania, a middle-income Baltic country of 3.3
million people.
Methods
To perform the analysis, we used data from clinical trials,
the Lithuanian mortality registry, the Kaunas Monitoring of Trends and
Determinants in Cardiovascular Disease (MONICA) register, Kaunas University
Hospital and, when data from Lithuania were not available, the United States. We
used the predicted reduction in all-cause mortality (as potentially postponable
deaths) per 100,000 people aged 35 to 64 years as our outcome measure.
Results
The number of potentially postponable deaths from risk
factor prevention and management in the population without apparent heart
disease is 556.3 (plausible range, 282.3-878.1). The number of potentially
postponable deaths for people with stable heart disease is 280.4 (plausible
range, 90.8-521.8), 7.0 with a public-access defibrillator program (plausible
range, 3.8-8.9), and 119.0 for hospitalized patients (plausible range, 15.9-297.7).
Conclusion
Although improving treatment of acute events will
benefit individual patients, the potential impact on the larger population is
modest. Only programs that prevent and manage risk factors can generate large
declines in mortality. Significant reductions in both cardiac and noncardiac
death magnify the impact of risk-factor prevention and management.
Back to top
Introduction
Lithuania, a country of 3.3 million in Northern Europe, lies on the eastern
shore of the Baltic Sea, north of Poland, south of Latvia, and west of Belarus.
It regained independence from the Soviet Union in 1990. Having a per capita
gross national income (GNI) about one-quarter that of the United States,
Lithuania is classified by the World Bank as an upper middle-income country (1).
As with the United States, Canada, and the countries of Northern and Eastern
Europe, coronary heart disease (CHD) is the leading cause of decreased life
expectancy among middle-aged Lithuanians (2). Preventing chronic disease through
lifestyle improvement is a priority in Lithuania, but privatization of health
services, coupled with health care costs that are growing at a rate far greater
than that of the GNI, could divert resources from disease prevention (3).
Because prevention programs compete with treatment programs for scarce
resources, policy makers need evidence that allocating resources to disease
prevention programs will have the greatest effect on the population’s burden of
disease (personal communication between Lithuanian Minister of Health, Raimondas
Šukys, and Vilius Grabauskas, November 9, 2010).
To document the potential impact of public health and clinical intervention strategies, we used
a model that accounts for the entire population and is relevant to both public
health and clinical interventions (4). With this model, we can evaluate existing
or proposed interventions at any point along the heart disease continuum, from
prevention of risk factors to treatment of advanced disease. In this article, we
report the expected impact of interventions that are currently available or
might be developed to prevent and treat heart disease for the Lithuanian
population aged 35 to 64 years.
Back to top
Methods
We used the 2007 register of the Kaunas University Hospital Department of
Cardiology for medical care data for hospitalized patients. Kaunas University
Hospital, a facility with approximately 2,000 beds, is the teaching hospital for
the Kaunas University of Medicine. Lacking Lithuanian data, we used data from
the United States to estimate service-delivery rates to ambulatory patients (4).
The MONICA research protocol was approved by the Kaunas Medical University
institutional review board.
Our model divides the population into 3 prevalence pools: people with no
apparent heart disease, people with symptomatic heart disease with a left
ventricular ejection fraction (LVEF) greater than 35%, and people with
symptomatic heart disease with an LVEF of 35% or less (4). This
division takes into account the marked differences in mortality among the
pools and acknowledges that different types of interventions are most
efficacious in each of the 3 pools.
We categorized acute cardiac events as out-of-hospital cardiac arrest,
acute or emergent events, and disease discovered in the ambulatory setting. We
subdivided acute/emergent events into acute myocardial infarction with
ST-segment elevation (STEMI) on electrocardiogram (ECG), acute heart failure
with an LVEF of 35% or less, acute myocardial infarction without ST segment
elevation (nSTEMI) on ECG, and unstable angina or other acute cardiac events. The
model can account for any intervention that would be directed at anyone in the
population who is at risk for heart disease, has stable chronic heart disease,
or is experiencing an acute event, because each person must belong to 1 of the 3
pools, and all types of acute events are subsumed under the 3 broad categories
of acute events.
We selected the number of potentially postponable deaths (PPD) as the outcome
of interest for this analysis. A similar outcome has been used to estimate the
source of the change in death rates from heart disease in the United States and
several other countries (5-8). In this analysis, we calculated the number of
deaths that can be prevented or postponed by improving risk factors or care as
follows:
PPD = (expected mortality reduction when the intervention is implemented) x
(mortality rate) x (1 – current implementation rate) x (number in population).
The analysis used the cumulative-relative-benefit approach of Mant and Hicks
to calculate the joint effect of simultaneous interventions (9). This model has
also been used to estimate the potential impact of improving care in the United
States (4,10).
In our analysis, we used mortality from all causes, for several reasons. Most
intervention trials report outcomes in terms of total mortality. Reducing the
burden of heart disease risk reduces total mortality and deaths from other
chronic diseases, and using total mortality as the endpoint eliminates the
possibility that an intervention simply results in death from a different cause
rather than reducing the probability of death.
Prevalence and mortality data
We used the Kaunas Monitoring of Trends and Determinants in Cardiovascular
Disease (MONICA) registry to estimate the prevalence of heart disease, and we
used the Lithuanian death registry as the source of death rates for the
subpopulation without heart disease (11). We did not have access to accurate
all-cause mortality rates for the subpopulations with symptomatic heart disease
with an LVEF greater than 35% and symptomatic heart disease with an LVEF
of 35% or less. Therefore, we used the mortality rate ratios from Olmsted
County, Minnesota (12,13). We estimated that the risk of death for people with
heart disease and an LVEF greater than 35% is 2.84 times the risk of death for
those without apparent heart disease, and the risk of death for people with
heart disease and an LVEF of 35% or less is 11.02 times the risk of death for
those without apparent heart disease.
We used published reports from clinical trials to estimate what the 1-year
case-fatality rates for acute events would have been without the provision of
modern treatments. On the basis of an epidemiologic observation (13), we
estimated that the LVEF is 35% or less in half the cases of heart failure.
Risk factor data
We used the 2001 Lithuanian MONICA registry risk factor data for the analysis
(14). At least 200 men and 200 women had been screened in every 10-year age group
(35-44 y, 45-54 y, and 55-64 y). The response rate for the survey was 62.4%. The
register contains data from 625 men and 778 women. The survey included physical
measurements (blood pressure, height, body weight, and hip and waist
circumference), blood samples for serum cholesterol levels, and face-to-face
interviews by the research staff for information on smoking.
Smoking
The MONICA smoking questionnaire included questions about smoking behavior
(regular smoker, ex-smoker, never-smoker, occasional smoker), type of tobacco
smoked (cigarettes, pipe, cigars), and number of cigarettes smoked per day.
Participants who smoked at least 1 cigarette, cigar, or pipe per day were
considered regular smokers.
Blood pressure
MONICA uses standard mercury sphygmomanometers for blood pressure measurement.
Blood pressure was
measured from the right arm of the subject after 5 minutes of rest in a sitting
position. The fifth phase of Korotkoff sounds was recorded as diastolic BP. The
mean of 2 readings was used. Arterial hypertension was defined as a systolic
blood pressure level greater than 140 mm Hg, a diastolic blood pressure level
greater than 90 mm Hg,
or both. Participants who had taken antihypertensive drugs in the last 2 weeks
were classified as hypertensive regardless of their blood pressure level.
Sensitivity analysis
We used 95% confidence intervals, when available, to define a plausible range
for the estimates of mortality reduction attributable to an intervention.
Otherwise, we used ±20% of the expected value as the plausible range. For the
plausible range of the current level of implementation, we used ±20% of the
observed value. For estimates of the number of deaths prevented or postponed, we
defined the lower bounds of the plausible range by the following product: the
lower bounds of the estimates for the population size, expected mortality rate
without intervention, and expected effect of the intervention and the upper
bound of the current rate of intervention. We defined the upper bounds of the
plausible range of deaths prevented or postponed by the following product: the
upper bounds of the estimates for the population size, expected mortality rate
without intervention, and expected effect of the intervention and the lower
bound of the current rate of intervention.
Because we provided the plausible range for each of the values used in the
calculations, the reader can estimate the impact of the achievable level of
implementation. For example, the PPD associated with adequate physical activity
is calculated to be 303.6 (Table
1). If the reader were to believe that the prevalence of physically active
individuals could be increased by only 20 percentage points rather than 81
percentage points, the new PPD would be 303.6 ×
20/81, or 75.0. This PPD can be compared with the PPD for any other
intervention. For example, the maximum plausible PPD associated with increasing
the rate of primary angioplasty for all patients with a STEMI is 11.6
(Table 2).
Back to top
Results
Prevalence pools
A Lithuanian population of 100,000 adults aged 35 to 64 years would comprise 92,842
people (95% CI, 91,410-94,274) with no apparent heart disease, 5,516 (95% CI,
4,413-6,619) with symptomatic heart disease with an LVEF greater than 35%, and
1,642 (95% CI, 1,314-1,970) with symptomatic heart disease with an LVEF of 35% or less. We calculated that, during 1 year, 1,112 (95% CI,
876-1,355) people without apparent heart disease, 188 (95% CI, 120-271) with symptomatic heart disease and an LVEF greater than 35%, and 217
(95% CI, 139-312) with symptomatic heart disease with an
LVEF of 35% or less would die.
Acute events
We calculated that, in a given year, 168 people would have an out-of-hospital
cardiac arrest, 152 would have a STEMI, 207 would be hospitalized for acute
heart failure with an LVEF of 35% or less, and 233 would have an nSTEMI. Along
with these events, 1,893 people would be hospitalized for unstable angina, and
253 would receive a new diagnosis of heart disease in the ambulatory setting
(Table 3). The events associated with the greatest number of deaths during the
ensuing year would be unstable angina followed by out-of-hospital cardiac
arrest.
Interventions in the prevalence pools
Among the 5 interventions associated with a lower risk of death or known to
reduce death for people without apparent heart disease, the largest PPD is
associated with population levels of adequate physical activity (Table
1). The
analysis predicts that 556.3 deaths are potentially postponable if all 5
interventions were implemented simultaneously.
As with people without apparent heart disease, the largest PPD for patients
with symptomatic heart disease and an LVEF greater than 35% is associated with
physical activity. The composite PPD for this population pool is 114.8. The
largest PPD for patients with symptomatic heart disease with an LVEF
of 35% or less is also associated with physical activity. This PPD is followed
by the PPD associated with device therapy, smoking rates, and use of
spironolactone, a drug used to prevent sudden death in patients with cardiomyopathy.
The composite potential PPD for this population pool is 165.6. The number of potentially
postponable deaths for people with stable heart disease is 280.4 (plausible
range, 90.8-521.8)
Interventions at the time of acute events
On the basis of the assumption that community-wide placement of automated
external defibrillators (AEDs) with bystander training does not exist, the PPD
associated with bystander training and public access to AEDs is 7.0 (Table 2).
The largest PPD for patients who experience a STEMI is associated with the
rate of primary angioplasty, followed by abstinence from tobacco. The composite
PPD for STEMI is 8.6. Among the 7 interventions that have been shown to reduce
mortality in patients hospitalized for heart failure with an LVEF 35% or less,
the largest PPD is associated with cardiac rehabilitation followed by the use of
statins. The composite PPD associated with this acute event is 16.5.
Among the 8 evidence-based interventions used to treat patients with an
nSTEMI, the largest PPD is associated with immediate revascularization, followed
by abstinence from tobacco. The composite PPD for nSTEMI is 11.2.
Among the 7 evidence-based treatments used to treat patients hospitalized for
unstable angina and similar conditions, the largest PPD is associated with
cardiac rehabilitation and smoking cessation. The composite PPD for unstable
angina and similar conditions is 82.7. The combined PPD for all hospitalized
patients is 119.0.
Among the 6 evidence-based interventions used to treat patients with heart
disease discovered in the ambulatory setting, the largest PPDs are associated
with prescription of beta blockers, followed by cardiac rehabilitation and
smoking cessation. The composite PPD for heart disease discovered in the
ambulatory setting is 3.5.
Sensitivity analysis
The results of the calculations did not substantively change when we varied
the size of the population pools, death rates, efficacy of intervention, and the
current rates of intervention. The upper bound PPD for acute events (305.1) was
less than the lower bound PPD for the prevalence pools (373.1). The upper bound
of the PPD for immediate revascularization of all patients with a STEMI or an
nSTEMI was 27.3. The lower bound of the PPD for dietary change (54.7) is twice
this number, and the lower bound of the PPD for adequate physical activity is
nearly 7 times this number. This means that, if dietary change were only as
effective as the lower-bound estimate and only half of the population adopted an
adequate diet, dietary change would still have the same population impact as
immediate revascularization for all patients with STEMI or nSTEMI under the most
optimistic assumptions about revascularization. By far the greatest opportunity to reduce mortality lies with
improving risk profiles and care for people in the 3 prevalence pools
(Figure).
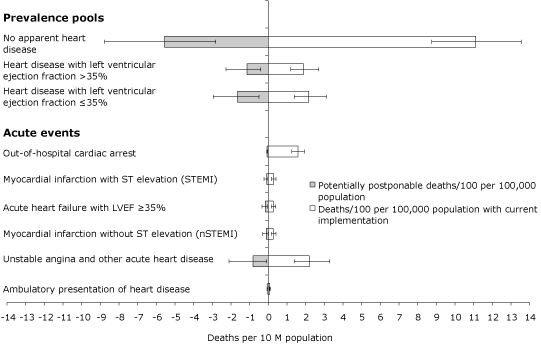
Figure. Open bars are deaths per 100 population with current level of implementation;
shaded bars are potentially postponable deaths per 100 population. Error bars
represent plausible range of estimate, defined as 1 standard deviation,
if available; otherwise, 20% of the expected value. Abbreviation: LVEF, left
ventricular ejection fraction. [A
tabular version of this figure is also available.]
Back to top
Discussion
Our analysis indicates that interventions that would increase adoption of a
low-risk lifestyle (not smoking, eating adequate fruits and vegetables,
consuming foods high in omega-3 fatty acids, and obtaining adequate physical
activity) and treatment of hypertension among people who are not known to have
heart disease could potentially postpone more than one-third of all deaths in
the Lithuanian population aged 35 to 64 years. Improving the delivery of care
and improving lifestyles for ambulatory patients with heart disease could
potentially postpone nearly 20% of all deaths. Optimizing care for people
experiencing an acute event or with newly diagnosed heart disease could
potentially postpone 8% of all deaths at most. Less favorable assumptions about
prevalence, efficacy, mortality, and the ability to produce lifestyle
changes do not substantively change the results. Risk-factor prevention and
control and attention to improving ambulatory care for patients with heart
disease is the strategy predicted to prevent or postpone the most deaths in the
population; fewer than 10% of all deaths can be prevented or postponed by
further improvements in care for patients hospitalized with heart disease.
This study has several limitations. Perhaps the most substantial is the lack
of data specific to the Lithuanian population. Although the risk-factor data are
highly reliable because they are based on carefully collected MONICA data, the
only ambulatory care data available to us were from the United States. Clearly,
Lithuanian data or data from a similar European state would have been more
appropriate. Limiting the analysis to adults aged 35 to 64 when the
highest mortality rates from heart disease occur in an older population segment
is another limitation, but neither risk factor nor clinical care data exist for
the older population. These shortcomings could all be corrected with more
complete data from Lithuania; because the analysis is driven by an Excel
spreadsheet, it can easily be updated with data from Lithuania or any other
population. A more challenging shortcoming is the unknown extent to which newly
developed interventions can lead to healthier lifestyles. Given the magnitude of
the effect of lifestyle changes on death rates, interventions that would produce
even modest movement toward healthier lifestyles would have a large effect on
mortality.
Although the number of clinical trials to prevent and treat heart disease is
very large, head-to-head comparisons of the expected effects of different
interventions that address the burden of heart disease are nearly nonexistent.
Using methods similar to those used in this analysis, Capewell et al calculated
the expected impact of treating more people for coronary heart disease (10).
However, their analysis addressed only medical and surgical interventions and
limited the endpoint to death from heart disease rather than total mortality. An
analysis that uses disease-specific death rates as the outcome variable
underestimates the impact of risk-factor change. One of the authors of the
current analysis (T.E.K.) published an analysis of the predicted effectiveness
of various interventions if applied in the United States (4). As might be
expected, the results were similar to those of the current analysis, because
both reports used the same intervention data, and the major burden of disease in
both countries is chronic disease.
The implications of this analysis extend beyond the borders of Lithuania.
Cardiovascular disease — heart disease and stroke — is the leading cause of
death in the world, and high-tech approaches to the problem are being
aggressively marketed worldwide by technology and pharmaceutical companies.
Particularly when specialist physicians are also advocating for large
investments in high-tech solutions by pointing to improved outcomes in
individual patients, policy makers may find it difficult to resist their
arguments for large investments in medical technology and devices. We hope that
access to analytic methods like the one used in this report can help make policy
decisions more rational, evidence-based, and beneficial for population health.
Back to top
Author Information
Corresponding Author: Thomas E. Kottke, MD, MSPH, HealthPartners, Inc, 8170
33rd Ave S, PO Box 1524, MS 21111R, Minneapolis, MN 55440-1524. Telephone:
612-580-0153. E-mail: Thomas.E.Kottke@HealthPartners.com.
Author Affiliations: Lina Jancaityte, Abdonas Tamosiunas, Vilius
Grabauskas, Kaunas University of Medicine, Kaunas, Lithuania.
Back to top
References
- Lithuania. 2010. data.worldbank.org/country/lithuania. Accessed November
5, 2010.
- Bonneux L, Huisman C. Who dies of what in Europe before the age of 65.
Luxembourg (LU): eurostat; 2009. http://epp.eurostat.ec.europa.eu/cache/ITY_OFFPUB/KS-SF-09-067/EN/KS-SF-09-067-EN.PDF.
Accessed July 7, 2011.
- Kumpiene J, Grabauskas V, Gurevicius R, Kucinskiene ZA, Maciuliene ALN,
Padaiga Z, et al. Implementation strategy of health care reform’s aims and
objectives. Vilnius (LT): Ministry of Health; 2006. http://sena.sam.lt/repository/dokumentai/veikla/Sveikatos%20EN%201-80p.pdf.
Accessed July 7, 2011.
- Kottke TE, Faith DA, Jordan CO, Pronk NP, Thomas RJ, Capewell S.
The
comparative effectiveness of heart disease prevention and treatment
strategies. Am J Prev Med 2009;36(1):82-8.
- Unal B, Critchley JA, Capewell S.
Explaining the decline in coronary
heart disease mortality in England and Wales between 1981 and 2000.
Circulation 2004;109(9):1101-7.
- Capewell S, Beaglehole R, Seddon M, McMurray J.
Explanation for the
decline in coronary heart disease mortality rates in Auckland, New Zealand,
between 1982 and 1993. Circulation 2000;102(13):1511-6.
- Capewell S, Morrison CE, McMurray JJ.
Contribution of modern
cardiovascular treatment and risk factor changes to the decline in coronary
heart disease mortality in Scotland between 1975 and 1994. Heart
1999;81(4):380-6.
- Ford ES, Ajani UA, Croft JB, Critchley JA, Labarthe DR, Kottke TE, et
al. Explaining the decrease in U.S. deaths from coronary disease, 1980-2000.
N Engl J Med 2007;356(23):2388-98.
- Mant J, Hicks N.
Detecting differences in quality of care: the
sensitivity of measures of process and outcome in treating acute myocardial
infarction. BMJ 1995;311(7008):793-6.
- Capewell S, O’Flaherty M, Ford ES, Critchley JA.
Potential reductions in
United States coronary heart disease mortality by treating more patients. Am
J Cardiol 2009;103(12):1703-9.
- Svidleriene D, Kasparaviciene L. Causes of death 2007. Vilnius (LT): Demographic Statistics Division; 2008.
- Orencia A, Bailey K, Yawn BP, Kottke TE.
Effect of gender on long-term
outcome of angina pectoris and myocardial infarction/sudden unexpected
death. JAMA 1993;269(18):2392-7.
- Senni M, Tribouilloy CM, Rodeheffer RJ, Jacobsen SJ, Evans JM, Bailey
KR, Redfield MM.
Congestive heart failure in the community: a study of all
incident cases in Olmsted County, Minnesota, in 1991. Circulation
1998;98(21):2282-9.
- MONICA Manual, Part IV: Event Registration. Section 1: Coronary Event
Registration Data Component. Helsinki (FI): National Institute for Health and
Welfare; 1999.
- State-specific mortality from sudden cardiac death — United States,
1999. MMWR Morb Mortal Wkly Rep 2002;51(6):123-6.
- Nichol G, Stiell IG, Hebert P, Wells GA, Vandemheen K, Laupacis A.
What
is the quality of life for survivors of cardiac arrest? A prospective study. Acad Emerg Med 1999;6(2):95-102.
- Baigent C, Collins R, Appleby P, Parish S, Sleight P, Peto R.
ISIS-2: 10
year survival among patients with suspected acute myocardial infarction in randomised comparison of intravenous streptokinase, oral aspirin, both, or
neither. The ISIS-2 (Second International Study of Infarct Survival)
Collaborative Group. BMJ 1998;316(7141):1337-43.
- Flather MD, Yusuf S, Kober L, Pfeffer M, Hall A, Murray G, et al.
Long-term ACE-inhibitor therapy in patients with heart failure or
left-ventricular dysfunction: a systematic overview of data from individual
patients. ACE-Inhibitor Myocardial Infarction Collaborative Group. Lancet
2000;355(9215):1575-81.
- Peterson ED, Roe MT, Mulgund J, DeLong ER, Lytle BL, Brindis RG, et al.
Association between hospital process performance and outcomes among patients
with acute coronary syndromes. JAMA 2006;295(16):1912-20.
- Rosamund W, Flegal K, Friday G, Furie K, Go A, Greenlund
K. Heart disease and stroke statistics, 2007
update: a report from the American Heart Association Statistics
Committee and the Stroke Statistics Subcommittee. Circulation
2007;115(5):e69-171.
- Knoops KT, de Groot LC, Kromhout D, Perrin AE, Moreiras-Varela O,
Menotti A, van Staveren WA.
Mediterranean diet, lifestyle factors, and 10-year
mortality in elderly European men and women: The HALE Project. JAMA
2004;292(12):1433-9.
- Doll R, Peto R.
Mortality in relation to smoking: 20 years’ observations
on male British doctors. BMJ 1976;2(6051):1525-36.
- Andersen LB, Schnohr P, Schroll M, Hein HO.
All-cause mortality
associated with physical activity during leisure time, work, sports, and
cycling to work. Arch Intern Med 2000;160(11):1621-8.
- Kottke TE, Wu LA, Brekke LN, Brekke MJ, White RD.
Preventing sudden
death with n-3 (omega-3) fatty acids and defibrillators. Am J Prev Med
2006;31(4):316-23.
- Antikainen R, Jousilahti P, Tuomilehto J.
Systolic blood pressure,
isolated systolic hypertension and risk of coronary heart disease, strokes,
cardiovascular disease and all-cause mortality in the middle-aged
population. J Hypertens 1998;16(5):577-83.
- Antithrombotic Trialists’ Collaborative.
Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death,
myocardial infarction, and stroke in high risk patients. BMJ
2002;324(7329):71-86.
- Freemantle N, Cleland J, Young P, Mason J, Harrison J.
beta Blockade
after myocardial infarction: systematic review and meta regression analysis. BMJ 1999;318(7200):1730-7.
- Baigent C, Keech A, Kearney PM, Blackwell L, Buck G,m Pollicino C, et
al. Efficacy and safety of cholesterol-lowering treatment: prospective
meta-analysis of data from 90,056 participants in 14 randomised trials of
statins. Lancet 2005;366(9493):1267-78.
- Critchley JA, Capewell S.
Mortality risk reduction associated with
smoking cessation in patients with coronary heart disease: a systematic
review. JAMA 2003;290(1):86-97.
- Yusuf S, Sleight P, Pogue J, Bosch J, Davies R, Dagenais G.
Effects of
an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular
events in high-risk patients. The Heart Outcomes Prevention Evaluation Study
Investigators. N Engl J Med 2000;342(3):145-53.
- Dietary supplementation with n-3 polyunsaturated fatty acids and vitamin
E after myocardial infarction: results of the GISSI-Prevenzione trial.
Gruppo Italiano per lo Studio della Sopravvivenza nell’Infarto miocardico.
Lancet 1999;354(9177):447-55.
- Wannamethee SG, Shaper AG, Walker M.
Physical activity and mortality in
older men with diagnosed coronary heart disease. Circulation
2000;102(12):1358-63.
- Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, et al.
The
effect of spironolactone on morbidity and mortality in patients with severe
heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J
Med 1999;341(10):709-17.
- Belardinelli R, Georgiou D, Cianci G, Purcaro A.
Randomized, controlled
trial of long-term moderate exercise training in chronic heart failure:
effects on functional capacity, quality of life, and clinical outcome.
Circulation 1999;99(9):1173-82.
- Lam SK, Owen A.
Combined resynchronisation and implantable
defibrillator therapy in left ventricular dysfunction: Bayesian network
meta-analysis of randomised controlled trials. BMJ 2007;335(7626):925.
- Hallstrom AP, Ornato JP, Weisfeldt M, Travers A, Christenson J, McBurnie
MA, et al.
Public-access defibrillation and survival after out-of-hospital
cardiac arrest. N Engl J Med 2004;351(7):637-46.
- Indications for ACE inhibitors in the early treatment of acute
myocardial infarction: systematic overview of individual data from 100,000
patients in randomized trials. ACE Inhibitor Myocardial Infarction
Collaborative Group. Circulation 1998;97(22):2202-12.
- Hartwell D, Colquitt J, Loveman E, Clegg AJ, Brodin H, Waugh N, et al.
Clinical effectiveness and cost-effectiveness of immediate angioplasty for
acute myocardial infarction: systematic review and economic evaluation.
Health Technol Assess 2005;9(17):1-99, iii-iv.
- Taylor RS, Brown A, Ebrahim S, Jolliffe J, Noorani H, Rees K, et al.
Exercise-based rehabilitation for patients with coronary heart disease:
systematic review and meta-analysis of randomized controlled trials. Am J
Med 2004;116(10):682-92.
- Shibata MC, Flather MD, Wang D.
Systematic review of the impact of beta
blockers on mortality and hospital admissions in heart failure. Eur J Heart
Fail 2001;3(3):351-7.
- Foody JM, Shah R, Galusha D, Masoudi FA, Havranek EP, Krumholz HM.
Statins and mortality among elderly patients hospitalized with heart
failure. Circulation 2006;113(8):1086-92.
- Piepoli MF, Davos C, Francis DP, Coats AJ.
Exercise training
meta-analysis of trials in patients with chronic heart failure (ExTraMATCH). BMJ 2004;328(7433):189.
- Mehta SR, Yusuf S.
The Clopidogrel in Unstable angina to prevent Recurrent Events (CURE)
trial programme. Rationale, design and baseline characteristics including a
meta-analysis of the effects of thienopyridines in vascular disease. Eur
Heart J 2000;21(24):2033-41.
- Ottervanger JP, Armstrong P, Barnathan ES, Boersma E, Cooper JS, Ohman
EM, et al.
Long-term results after the glycoprotein IIb/IIIa inhibitor
abciximab in unstable angina: one-year survival in the GUSTO IV-ACS (Global
Use of Strategies To Open Occluded Coronary Arteries IV
— Acute Coronary
Syndrome) Trial. Circulation 2003;107(3):437-42.
- Bavry AA, Kumbhani DJ, Quiroz R, Ramchandani SR, Kenchaiah S, Antman EM.
Invasive therapy along with glycoprotein IIb/IIIa inhibitors and
intracoronary stents improves survival in non–ST-segment elevation acute
coronary syndromes: a meta-analysis and review of the literature. Am J Cardiol 2004;93(7):830-5.
- Al-Mallah MH, Tleyjeh IM, Abdel-Latif AA, Weaver WD.
Angiotensin-converting
enzyme inhibitors in coronary artery disease and preserved left ventricular
systolic function: a systematic review and meta-analysis of randomized
controlled trials. J Am Coll Cardiol 2006;47(8):1576-83.
Back to top
|
|
