Volume
8: No. 4, July 2011
Jamie M. Cousins, MPA; Sarah M. Langer, MPH; Lori K. Rhew, MA, CHES, PAPHS; Cathy Thomas, MAEd
Suggested citation for this article: Cousins JM,
Langer SM, Rhew LK, Thomas C. The role of state health departments in supporting community-based obesity prevention. Prev Chronic Dis 2011;8(4):A87.
http://www.cdc.gov/pcd/issues/2011/jul/10_0181.htm. Accessed [date].
PEER REVIEWED
Abstract
Background
Recent national attention to obesity prevention has highlighted the importance of community-based initiatives. State health departments are in a unique position to offer resources and support for local obesity prevention efforts.
Community Context
In North Carolina, one-third of children are overweight or obese. North Carolina’s
Division of Public Health supports community-based obesity prevention by awarding annual grants to local health departments, providing ongoing training and technical assistance, and engaging state-level partners and resources to support local efforts.
Methods
The North Carolina Division of Public Health administered grants to 5 counties to implement the Childhood Obesity Prevention Demonstration Project; counties simultaneously carried out interventions in the community, health care organizations, worksites, schools, child care centers, and faith communities.
Outcome
The North Carolina Division of Public Health worked with 5 local health departments to implement community-wide policy and environmental changes that support healthful eating and physical activity. The state health department supported this effort by working with state partners to provide technical assistance, additional funding, and evaluation.
Interpretation
State health departments are well positioned to coordinate technical assistance and leverage additional support to increase the strength of community-based obesity prevention efforts.
Back to top
Background
More than two-thirds of North Carolina’s adults and one-third of the state’s children are overweight or obese (1,2). To reverse the growing obesity epidemic, the North
Carolina Division of Public Health (NCDPH) supports community-based obesity prevention efforts through funding, training, and technical assistance. Strong partnerships at the state and local levels are necessary for these efforts.
Community partners include community coalitions, recreation centers, religious
organizations, physician’s offices, child care providers, and schools.
Recent federal initiatives provide support for community-based
interventions. In 2009, the Centers for Disease Control and Prevention (CDC)
released the Recommended Community Strategies and Measurements to Prevent Obesity in the United States (3). In 2010, CDC granted federal stimulus funding
to states, territories, tribal entities, and community initiatives for evidence-based obesity prevention strategies through the Communities
Putting Prevention to Work initiative.
For the community initiatives, CDC directly funded health districts serving
more than 500,000 people; districts serving less than 500,000 could only apply through their state health department. Additionally,
First Lady Michelle Obama launched the Let’s Move campaign in 2010, calling for comprehensive, collaborative, and community-oriented solutions to the childhood obesity epidemic (4). These national initiatives promote community-based projects that address obesity in several settings and facilitate change on the personal, interpersonal, organizational, policy, and environmental levels (3,4). Shape Up Somerville: Eat Smart, Play Hard
exemplified this multilevel, multisetting, community-based approach in Massachusetts (5) and
was the inspiration for the
Childhood Obesity Prevention Demonstration Project (COPDP).
As communities across the nation strive to reduce and prevent childhood obesity, state health departments can offer vital resources to enhance their efforts. In 2008-2009, the North
Carolina General Assembly funded an innovative community-based project to reduce and prevent childhood obesity. Administered by NCDPH, COPDP offers valuable
insight for state health departments supporting multilevel, multisetting, community-based obesity
prevention. COPDP, which was supported with substantial state funding and state health department resources, resulted in positive change in 5 North
Carolina counties. We discuss the role of NCDPH in this community-based childhood obesity prevention project. The purpose of this case study is to examine the role that state health departments play in supporting community-based
efforts.
Back to top
Community Context
In 2010, North Carolina ranked 11th in the nation for childhood obesity among
children aged 10 to 17 years (6). According to the 2007 National Survey of
Children, 18.6% of North Carolina youth aged 10 to 17 years were obese (7), compared with
16.4% nationally (8). According to North Carolina’s Child Health Assessment and
Monitoring Program, one-third of children in North Carolina aged 10 to 17 years were overweight or obese in 2009 (2).
NCDPH support for community-based obesity prevention
NCDPH dedicates resources to build the capacity of local health departments and local partnerships to address
various health issues. Specific to healthful eating and physical activity, the NCDPH Physical Activity and Nutrition (PAN) Branch uses federal Preventive Health and Health Services Block Grant funds for the
Statewide Health Promotion Program. This program supports policy and environmental change in 98 of
North Carolina's 100
counties by building local capacity through funding, training, and technical assistance. In addition, local health departments, in collaboration with their partners, compete for grants of up to $20,000 annually to encourage physical activity and healthful eating in their communities
by changing policies and environments.
The PAN Branch also uses CDC grant funding to cultivate and sustain state-level partnerships. Strong communication among state-level partners creates a more supportive statewide context for community-based initiatives. The most notable partnership is the Eat Smart, Move More North Carolina (ESMM-NC)
leadership team, a multidisciplinary group of more than 60 statewide partner organizations. The PAN Branch provides staff support to the ESMM-NC
leadership team, which guides the ESMM-NC movement (9) to increase opportunities for healthful eating and physical activity wherever people live, learn, earn, play, and pray.
In 2008, the PAN Branch, with support from North Carolina’s state health director and
chronic disease director, worked with ESMM-NC partners to advocate for state-supported, community-based projects to address childhood obesity. Partners used data such as the correlation between physical inactivity and academic performance and obesity-related health care costs to make a case for state funding to explore best practices in preventing childhood obesity. These partners created the COPDP plan based
on the socioecological model, a multilevel, multisetting approach similar to the Shape Up Somerville project.
Funding
In state fiscal year 2008-2009, the North Carolina General Assembly awarded $1.9 million to NCDPH for COPDP. The funding was originally in the budget as recurring but was ultimately designated as nonrecurring. The North
Carolina General Assembly directed NCDPH to allocate the entire $1.9 million directly to local health departments to implement COPDP; however, the North
Carolina General Assembly did not allocate funding for the state to provide administration and technical assistance. Consequently, NCDPH identified other
resources to fund a state coordinator for the project and an external evaluation.
Objective of COPDP
The objective of COPDP was to implement a set of multilevel, multisetting interventions for preventing and reducing obesity among children in a community.
For the demonstration project, the state’s objective was to learn lessons in community-based obesity prevention, how to support
obesity-prevention efforts, and how to apply lessons learned in counties across the state.
Back to top
Methods
The demonstration project framework
COPDP included 8 required and 4 optional community interventions (Table 1).
Before the implementation of COPDP, each of the interventions had been
implemented in some North Carolina communities, but no community had implemented all of them. The interventions targeted children and their adult role models
in 6 settings: the community at-large, health care organizations, worksites,
schools, child care centers, and
religious organizations. COPDP incorporated 4 recommended strategies for physical
activity, nutrition, and obesity prevention from the Guide to Community Preventive Services: 1) community-wide campaigns (10), 2) community-scale urban design and land-use policies (11), 3) worksite programs combining nutrition and physical activity (12), and 4) enhanced physical education classes in schools (13).
COPDP required simultaneous implementation of the interventions in 5 selected counties. A community-wide media campaign united each of the separate COPDP interventions under a single brand and ensured consistent obesity prevention messages. The counties used existing resources from the ESMM-NC statewide movement to raise awareness of the interventions and
create a supportive environment for physical activity and healthful eating.
County selection
NCDPH used a 2-step, competitive application process to select counties to implement COPDP, beginning with a request for applications in July 2008. Twenty-nine counties submitted brief proposals describing their local partnerships, experiences collaborating on community-based projects, and plans to coordinate COPDP. Of these,
11 were invited to submit full applications with a detailed plan for implementing each of the interventions. The applications also included descriptions of the
capacity of each county’s project coordinator and key staff. NCDPH awarded grants of $380,000 to each of 5 selected counties beginning on October 1, 2008. In accordance with the state fiscal year, the grant period ended May 31, 2009, giving the counties 8 months to implement the program. The counties ranged in population from 34,296 to 172,223 (14) and were geographically distributed across the state.
State administration and technical assistance
NCDPH administered and provided technical assistance for COPDP. Preventive Health and Health Services Block Grant funds supported a full-time state coordinator at NCDPH. The state coordinator facilitated the involvement of state-level partners, developed a system for providing technical assistance, maintained constant contact with the county coordinators, and fostered sharing among the counties. These efforts ensured the efficient engagement of state-level expertise and resources, ongoing
quality improvement, and problem solving to support the counties throughout COPDP. The state coordinator also monitored the counties’ progress through site visits, monthly
telephone calls, and reviews of written monthly summary reports.
Statewide partners assisted with COPDP by providing additional funding, technical assistance, and training
(Table 2). For example, the North
Carolina State Board of Education provided an additional $250,000 to school districts in the 5 counties to further support obesity prevention through coordinated school health programs as part of COPDP. In addition, COPDP counties were the first counties to participate in a new initiative to enhance physical education in schools across the state. Through this
initiative, counties received technical assistance and training in an evidence-based physical education curriculum and
in fitness-testing software. NCDPH developed a centralized technical assistance infrastructure
(Figure) to support the
counties with the COPDP interventions and to streamline this support as
much as possible.
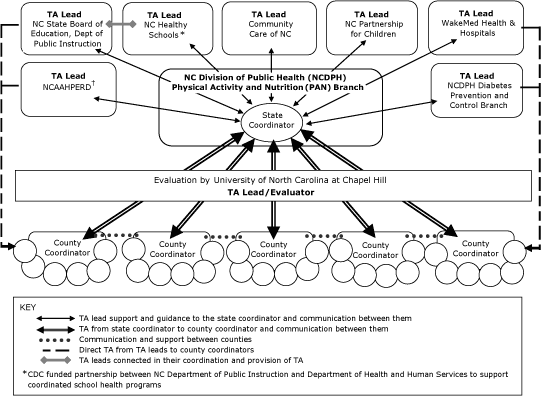
Figure. Technical Assistance (TA) Workflow for the Childhood Obesity Prevention Demonstration Project (COPDP).
Abbreviations: NC, North Carolina; NCAAHPERD, North Carolina Alliance for Athletics, Health, Physical Education, Recreation, and Dance;
CDC, Centers for Disease Control and Prevention.
[A text description of this figure is also available.]
County implementation
COPDP grants went to local health departments in each county, which
collaborated with county partnerships to implement the project. County-level implementation was directed by a county coordinator who worked closely with the
state coordinator to ensure the fulfillment of all grant requirements.
The county partnerships were well established before COPDP. Once funded, each partnership assessed its membership and added members as needed to include representation from all intervention settings. The number of agencies represented
in each partnership ranged from 9 to 16. The partnerships garnered resources (eg, volunteer time, space for classes, access to organizations
and individuals, support from local leaders and boards) through their existing
connections and relationships.
Evaluation
NCDPH funded the evaluation of COPDP through the Prevention Research Center at the University of North Carolina-Chapel Hill. A full-time COPDP evaluator worked with the state and county coordinators to 1) collect output data describing implementation, 2) measure intermediate outcomes describing changes in the communities, 3) examine the role of county partnerships in facilitating the success of the project, and 4) identify potential long-term outcome measures. The COPDP evaluator
also conducted interviews and focus groups, provided data analyses, and summarized findings. NCDPH engaged statewide partners in discussion of the evaluation results to share successes and opportunities for further collaboration. The institutional review board of the University of North Carolina
at Chapel Hill approved the evaluation.
Back to top
Outcome
Changes
The existence of COPDP resulted in immediate policy and environmental changes in the community, health care organizations, worksites, schools, child care centers, and religious organizations (Table 3). In the 5 counties, 42 child care providers made changes that
affected more than 2,400 children. Policy changes to support physical activity and healthful eating in hospital and school worksites affected more than 13,800 employees. Sixty-six children at risk for
type 2 diabetes completed a 36-session prevention program; of the 25 children who began the program with high triglycerides, 22 reduced their triglycerides
and 14 achieved a normal range. Additionally, more than 6 miles of greenways and sidewalks were constructed or designed. In some cases, the effect of these changes reached beyond county and even state lines. For instance, a child care center’s request for skim and 1% milk led to new food purchasing and distribution policies,
which provided more healthful milk options for affiliated child care centers across the nation.
The media campaign blanketed communities with consistent messages that tied interventions together. One woman claimed that seeing and hearing the same ESMM-NC messages
in multiple places — both in the community and in her workplace — made her feel connected to a larger effort. NCDPH and the counties documented success stories like these to illustrate the personal
effect on community members. These stories were used to educate policy
makers and stakeholders.
Lessons learned
The short time line, high visibility, and the large scale of COPDP presented challenges. Once the funding was awarded, NCDPH quickly leveraged support from state partners for the 5 counties in the form of additional funding, training, and technical assistance for COPDP. NCDPH’s long-standing relationships and collaboration with state partners made this possible.
The 8-month time line for the COPDP presented several challenges. Incorporating grant activities, such as staff training and a new
physical education curriculum for kindergarten through 8th grade, was challenging for schools because lesson plans and teacher professional development days had already been set for the year. Seasonal effects also limited progress; for example, farmers’ markets closed for winter just as COPDP began.
NCDPH worked with counties to balance the need for fidelity in implementation with the need for flexibility to adapt interventions to the local context. County health departments were asked to adhere to specific grant requirements, even if they adapted activities. In some cases, counties were simply not able to implement the interventions as specified
because of time and other constraints. For example, several counties adapted the enrollment criteria for 1 intervention because they could
not otherwise recruit enough participants in the given time frame.
A community-based health initiative’s duration affects its sustainability, and several years of implementation are needed to institutionalize the desired change (15). Although COPDP was designed for 5 years of funding, only 1 year of funding was initially awarded. NCDPH and the counties knew that continued funding was tentative; when a state fiscal crisis ensued in 2009, funding was not allocated for COPDP.
Counties developed sustainability plans, but without additional
resources, not all of the interventions could be continued. Likewise, funding was not available to evaluate the outcomes of COPDP beyond the 8-month
time frame. Further evaluation of this project is needed to track the counties’
continued efforts and measure long-term effects. Additional results, lessons
learned, and success stories are available on the ESMM-NC website (www.EatSmartMoveMoreNC.com/ObesityDemo/ObesityDemo.html).
Back to top
Interpretation
Communities are an essential forum for obesity prevention, and state health departments are uniquely positioned to support and enhance these efforts. States can leverage support and help to build the local capacity needed to implement comprehensive projects that
effect change in multiple community settings. NCDPH found that many North
Carolina counties have already united with partners
for obesity prevention and are well positioned to increase the scale of their efforts. Examples of NCDPH’s
long-term commitment to strengthen the capacity of local partnerships and public health departments include the Statewide Health Promotion Program and the distribution of community grants.
State health departments must think strategically about investing in community-based health initiatives. States funding large-scale, multilevel, and multisetting obesity prevention projects should consider a community partnership’s previous experience
in collaborating on similar projects. Prior collaboration and existing relationships equip local partnerships to work through the challenges
of these initiatives.
States should also consider the leadership capacity and skills of local coordinators. Focus groups and in-depth interviews with key informants in the COPDP counties revealed that skilled county coordinators were instrumental to the success of the effort. From the community perspective, the coordinators were the leaders of local partnerships that provided opportunities to network, share information,
solve problems, and celebrate successes. From the state perspective, the county coordinators
were necessary for troubleshooting, problem solving, engaging state technical assistance, and facilitating data collection.
Given the state budget process, funding often comes with short notice and duration. When offering grants for community-based projects, state health departments should allow themselves enough time to develop clear expectations and allow grantees enough time to plan effectively and secure partner commitments. More time
before the start of COPDP would have allowed NCDPH and partners to better
prepare materials, organize technical assistance, and develop data collection
tools. Additionally, securing several years of funding and state resources to
support COPDP would have enhanced the degree of sustainable change. To be effective, state health departments must be prepared to work within the context of short timelines and high expectations. As shown by COPDP, maintaining strong partnerships can lead to quick mobilization and additional resources when opportunities arise.
Finally, state health department staff time and resources are needed for
community-based childhood obesity prevention programs. The state coordinator for COPDP provided guidance on implementing evidence-based and best practices, engaged state-level partners, and coordinated technical assistance. Addressing obesity is complex, requiring expertise in nutrition, physical activity, urban planning, sustainable food systems, school health, and other disciplines. Although some of this
expertise exists among the state health department staff, much of it requires collaboration with external partners. State health department staff are well positioned to work with partners to coordinate technical assistance and leverage additional support to increase the strength of community-based obesity prevention efforts.
Back to top
Acknowledgments
We thank the North Carolina General Assembly and the North Carolina State
Board of Education for recognizing the importance of obesity prevention and for
funding COPDP. Funding from the federal Preventive Health and Health Services Block Grant supported administration and evaluation of this project.
We thank the following local health departments, partnerships, and county coordinators for leading the way in community-based childhood obesity prevention: Jennifer Bryan Greene, Appalachian District Health Department and the Watauga County Healthy Carolinians; Victoria Manning, Cabarrus Health Alliance and Healthy Cabarrus; Stephanie Bowers, Dare County Health Department and the Dare County Childhood Obesity Prevention Partnership; Terri
Wallace, Henderson County Partnership for Health; Linda Charping, Henderson County Department of Public Health; and Roxanne Leopper, MooreHealth and the Moore County Health Department.
We also thank the following state-level partners for providing support and technical assistance throughout this project: the North
Carolina State Board of Education; North Carolina Healthy Schools Initiative (a collaboration of the North
Carolina Department of Public Instruction and NCDPH); WakeMed Health and Hospitals; the North
Carolina Alliance for Athletics, Health, Physical Education, Recreation, and Dance; Community Care of North
Carolina; North Carolina Partnership for Children; the North Carolina Hospital
Association; and the University of North Carolina at Chapel Hill’s Prevention
Research Center. Several agencies within NCDPH also contributed: North
Carolina Office of Healthy Carolinians and Health Education, North Carolina Diabetes Prevention and Control Branch, North
Carolina State Center for Health Statistics, and the Women’s and Children’s Health Section in NCDPH.
Finally, we thank Jenni Albright, Sharon Nelson, Mary Bea Kolbe, and Sheree Vodicka
with the NCDPH and also Phyllis Fleming, PhD, with the University of
North Carolina at Chapel Hill’s Prevention Research Center for their
contributions to COPDP and review of this manuscript.
Back to top
Author Information
Corresponding Author: Jamie M. Cousins, MPA, Chronic Disease and Injury Section,
North Carolina Division of Public Health, 1915 Mail Service Center, Raleigh, NC 27699-1915. Telephone: 919-707-5241. E-mail:
jamie.cousins@dhhs.nc.gov.
Author Affiliations: Sarah M. Langer, North Carolina State University, Raleigh, North Carolina; Cathy Thomas, Lori K. Rhew,
Eat Smart, Move More North Carolina, Raleigh, North Carolina. At the time of this study, Sarah Langer was
affiliated with the University of North Carolina at Chapel Hill, Chapel Hill,
North Carolina; during the
writing of this article, she was affiliated with the North Carolina Division of
Public Health, Raleigh, North Carolina. At the time of this study, Lori Rhew was
affiliated with the North Carolina Division of Public Health, Raleigh, North
Carolina.
Back to top
References
- Behavioral Risk Factor Surveillance System Survey, 2009. North Carolina
State Center for Health Statistics. http://www.epi.state.nc.us/SCHS/brfss/2009/nc/all/rf2.html. Accessed July 9, 2010.
- Child Health Assessment and Monitoring Program, 2009. North Carolina State
Center for Health Statistics. http://www.schs.state.nc.us/SCHS/champ/2009/bmi_cat10.html. Accessed July 9, 2010.
- Khan LK, Sobush K, Kenner D, Goodman K, Lowry A, Kakietek J, et al.
Recommended community strategies and measurements to prevent obesity in the United States. MMWR Recomm
Rep 2009;58(RR-7):1-26.
- First Lady Michelle Obama launches Let’s Move: America’s move to raise a healthier generation of kids.
The White House; 2010. http://www.whitehouse.gov/the-press-office/first-lady-michelle-obama-launches-lets-move-americas-move-raise-a-healthier-genera. Accessed July 9, 2010.
- Economos CD, Hyatt RR, Goldberg JP, Must A, Naumova EN, Collins JJ, et al.
A community intervention reduces BMI z-score in children: Shape Up Somerville first year results. Obesity 2007;15(5):1325-36.
- F as in fat: how obesity threatens America’s future. Trust for
America’s Health; 2010. http://healthyamericans.org/reports/obesity2010/. Accessed July 9, 2010.
- Childhood Obesity Action Network.
Query: North Carolina, weight status of children based on
body mass index for age. http://nschdata.org. Accessed July 13, 2010.
- Childhood Obesity Action Network.
Query: nationwide, weight status of children based on
body mass index for age. http://nschdata.org. Accessed July 13, 2010.
- Eat Smart, Move More North Carolina. http://www.eatsmartmovemorenc.com/. Accessed July 9, 2010.
- Promoting physical activity: campaigns and informational approaches. Guide to
Community Preventive Services.
http://www.thecommunityguide.org/pa/campaigns/index.html. Last updated February 10, 2009. Accessed July 12, 2010.
- Promoting physical activity: environmental and policy approaches. Guide to
Community Preventive Services. http://www.thecommunityguide.org/pa/environmental-policy/index.html. Accessed July 12, 2010.
- Worksite health promotion. Guide to Community Preventive Services. http://www.thecommunityguide.org/worksite/index.html. Accessed July12, 2010.
- Promoting good nutrition. Guide to Community Preventive Services. http://www.thecommunityguide.org/nutrition/index.html. Accessed July 12, 2010.
- US Census Bureau. Population finder, 2009. Geographic areas: Cabarrus and Dare Counties, North Carolina. http://www.census.gov/. Accessed July 9, 2010.
- Shediac-Rizkallah MC, Bone LR.
Planning for the sustainability of community-based health programs: conceptual frameworks and future directions for research, practice and policy. Health Educ Res 1998;13(1):87-108.
Back to top
