

|

|

Volume
6: No. 4, October 2009
ORIGINAL RESEARCH
Assessing Calcium Intake in Postmenopausal Women
Karen L. Plawecki, MS, RD; Ellen M. Evans, PhD; Mina C. Mojtahedi, MS; Edward McAuley, PhD; Karen Chapman-Novakofski, PhD, RD
Suggested citation for this article: Plawecki KL, Evans EM, Mojtahedi MC, McAuley E, Chapman-Novakofski K. Assessing calcium intake in postmenopausal women. Prev Chronic Dis 2009;6(4):A124.
http://www.cdc.gov/pcd/issues/2009/
oct/08_0197.htm. Accessed [date].
PEER REVIEWED
Abstract
Introduction
Because foods fortified with calcium are increasingly available, the calcium content of calcium-fortified foods may not be adequately captured in traditional assessments of dietary intake, such as dietary records analyzed with commercially available software.
The primary objective of our study was to design and test a calcium-focused food frequency questionnaire (CFFFQ) including foods naturally rich in calcium and calcium-fortified foods. Secondary objectives were to
review calcium sources and adequacy of intake in black and in white postmenopausal women.
Methods
We studied a convenience sample of 46 black and 139 white postmenopausal women
(mean [SD] age 69.4 [5.8] years). Participants completed a multiple-pass interview for 24-hour
recall of foods eaten and the 46-item CFFFQ.
Results
The correlation between measures for total daily calcium intake was moderately strong (r = 0.53, P < .001). The CFFFQ estimated greater total daily calcium intake
than did the 24-hour recall (mean [SD],
1,021 [624] mg/d vs 800 [433] mg/d, P < .001). As daily calcium intake increased, the 24-hour recall increasingly underreported calcium (r = 0.41, P < .001)
compared with the CFFFQ.
Cross-tabulation and Χ2 analyses found that the CFFFQ had greater specificity for lower
calcium intakes. For calcium classified by food groups, there was moderate correlation for dairy (r = 0.56, P < .001) and fruits (r = 0.43, P < .001). The CFFFQ
overestimated mean total calcium compared with the 24-hour recall by 221 mg/d (P < .001), including within racial groups (195
mg/d for black women, P = .04, and 229 mg/d for white women, P < .001). Dairy was the primary calcium source for both groups (55% of intake for black
women and 57% of intake for white women).
Conclusion
The CFFFQ can be used to identify postmenopausal women with inadequate calcium intakes (<800 mg/d) and to identify key sources of dietary calcium. Older black women
consume less daily calcium than do older white women.
Back to top
Introduction
As the prevalence of osteoporosis continues to increase, interventions targeting modifiable risk factors receive more emphasis from researchers, clinicians, and public health professionals. Although
many nutrients are important to bone health, interventions largely focus on calcium intake (1).
Clinicians often prescribe a calcium supplement but pay limited attention to dietary sources of calcium intake (2,3). Other interventions may target only dairy calcium (4,5). However, calcium
fortification of foods broadens the possible sources of calcium so that adequate calcium intake may be achieved through a diverse diet.
Sources of dietary calcium may differ across cultures and ethnicities according to food preferences and tolerances. For example, blacks and Asians have a higher prevalence of lactose intolerance,
which may lead to reduced dairy intake, but also have cultural food preferences, including not drinking milk at meals, that
affect calcium intake (6). White women eat more cheese and drink more milk than do black or American Indian women (7). However, research specifically targeting
calcium intake and food source is scarce. Previous research from our group investigating the role of socioeconomic status on calcium intake determined that black women consumed fortified grain products more frequently than did white women (8).
Because fortified foods are
increasingly available (9), the calcium content of calcium-fortified foods may not be adequately captured in traditional assessments of dietary intake, such as dietary records analyzed with commercially available software.
The primary aim of this study was to develop and evaluate the feasibility of a calcium-focused food frequency questionnaire (CFFFQ) that incorporates both natural and fortified sources of calcium. Because determining calcium intake has become more difficult
as food fortification has become more common, this study compared 2 methods: an interview for 24-hour recall of calcium intake and the CFFFQ. Although supplements can be an important source of calcium, this project focused on food-derived
calcium. Secondary aims were to compare food source of calcium between black and white women aged 60 years or older and evaluate the adequacy of calcium intake as assessed using the 24-hour recall and the CFFFQ. Postmenopausal women were studied because they are at high risk for osteoporotic fractures (1).
Back to top
Methods
Participants
In 2005, we recruited a convenience sample of postmenopausal women aged 60 to 80 years who were enrolled in a parent study
in the Urbana-Champaign area of Illinois (10) (assessing body composition, bone health, physical activity, physical function, and self-efficacy) to complete additional nutritional assessments. Exclusion criteria for the parent study
were neurologic illness, orthopedic limitations, or cognitive limitations that precluded completion of all study testing procedures. All those in the parent study were invited to
participate in the current study of evaluation of calcium intake. The human subjects
institutional review board of the University of Illinois approved the research protocol, and all participants completed an informed consent form before data collection began.
Calcium intake
The CFFFQ and a self-reported 24-hour recall were completed on the same day to assess calcium intake and food source. The CFFFQ is a 46-item food frequency survey focusing on calcium-rich foods. Foods on the questionnaire were chosen based on calcium content and those found in previous studies to be commonly consumed. Foods on the CFFFQ
were categorized and presented according to representative food groups: dairy (6
foods), foods with dairy (5 foods), fruits (6 foods), vegetables (3 foods),
grains (10 foods), meats (8 foods), and other foods (8 foods) (Appendix). Inclusion of fortified foods was based on availability
for purchase in area grocery stores (both local and chain stores). Fortified foods were noted as such on the CFFFQ. A standard portion size was included for each specific food item. Participants entered quantity of food relative to daily, weekly, monthly, or yearly consumption. “Not eaten” was given as an option. We entered
foods and servings into a database (Microsoft Access 2003, Redmond, Washington) that calculated calcium content on a daily basis. Double entry was used for quality assurance.
Participants met with researchers to complete the 24-hour recall. The researchers used a multiple-pass interview style to elicit complete information (11). Foods from the 24-hour recall were categorized into the same food groups as on the CFFFQ
and were then entered in Nutritionist Pro version 2.3 (First DataBank, San Bruno, California) to obtain calcium values
per day.
Statistical analysis
We analyzed the data by using SPSS version 14.0 (SPSS, Inc, Chicago, Illinois). On the basis of the findings of the Kolmogorov-Smirnov
test, the primary variables of interest were not normally distributed.
Nonparametric tests were subsequently used to evaluate group or intake
assessment differences (Spearman rank correlation and Mann-Whitney). We assessed
the adequacy of calcium intake by comparing these 2 assessment methods to
two-thirds of the Institute of Medicine’s (12) adequate intake amount (used to
determine inadequate intake) for women aged 51 years or older. Comparison of the
adequacy classification as a measure of specificity of each calcium intake
method was completed by using cross-tabulation to demonstrate the relationship
between the 2 variables. Chi-square analysis was performed on the cross-tabulated variables. Significance was
defined as α = .05.
Back to top
Results
Of 245 eligible women from the parent study, 185 chose to participate in our study. Of the 185, 46 were black (mean [SD] age, 68.0 [4.85] years) and 139 were white (70.0 [6.0] years).
Comparison of CFFFQ to 24-hour recall
Calcium from the CFFFQ was significantly correlated with 24-hour recall for all food groups (P
< .001) except for vegetables (P = .08)
(Table 1). Estimates obtained
with the 24-hour recall method were significantly lower than CFFFQ estimates of total daily calcium, dairy, foods with dairy
products, fruits, and vegetables (Table 2).
The CFFFQ estimate of mean total calcium compared with the 24-hour recall was
higher by 221 mg/d (P < .001), including within racial groups (195 mg/d for
black women, P = .04, and 229 mg/d for white women, P < .001).
There was no significant difference between the CFFFQ and 24-hour recall
methods for calculated calcium intake for grains, meats, and “other” foods. This pattern was consistent for the total group and for black and white women separately (Table 2). The Bland-Altman plot illustrates the lack of agreement between methods of assessment for total daily intake (Figure). The positive correlation between the lack of agreement (error score on the Y-axis) and the daily intake indicates that
for increasing levels of daily calcium intake, the 24-hour recall of calcium intake increasingly
underestimated calcium intake compared with the CFFFQ (r = 0.41, P < .001).
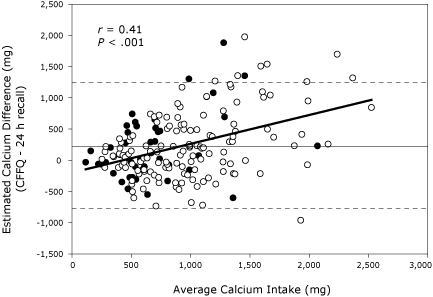
Figure. Scatterplot of agreement between the calcium-focused
food
frequency questionnaire (CFFFQ) and an interview for 24-hour recall of calcium
intake. Estimated calcium difference is the difference in calcium intake found
between the CFFFQ and the 24-hour recall. Average calcium intake is the average
of calcium intake between the 2 methods. Open circles represent white women (n =
139) and closed circles represent black women (n = 46). The parallel solid and the broken
lines represent the mean difference (2 SD) for all participants (221 [528]
mg).
Calcium adequacy assessment
The prevalence of inadequate intake (<800 mg) was 56% (n = 103) using the 24-hour recall and 45% (n = 83) using the CFFFQ method. Examining the cases where intake would be inadequate as measured by both tools, 64 (35%) women would be classified as having inadequate calcium intake. However, 39 (21%) women whose
intake would be classified as adequate by the CFFFQ would be classified as
inadequate by the 24-hour recall method. Only 19 (10%) who would be classified
as having inadequate intake by the CFFFQ would have adequate intake as classified by the 24-hour recall. Compared with the self-reported 24-hour recall, the CFFFQ indicates
more specificity for lower intakes.
Comparison of intake and source between black and white women
Regardless of dietary assessment method used, white women had higher calcium intakes than black women. When using the CFFFQ,
white women reported consuming approximately 43% more calcium than did black
women (mean [SD] 1,104 [632] mg for white women vs 768 [531] mg for black women, P < .001). When using the 24-hour recall method, mean calcium intake for white women was approximately
52% higher than intake for black women (875 [429] mg vs 573 [365] mg, P <
.001).
From the CFFFQ, the primary calcium source was dairy products (55% for black women and 57% for white women). White women obtained more calcium (630 [423] mg) from dairy than did black women (424 [373] mg, P < .004). Grains were the second highest calcium source, although grains provided a much lower percentage than dairy (13% of total calcium for each racial group). Calcium from grains primarily came from fortified foods. Dairy was also the primary calcium source when the 24-hour
recall data were analyzed, and a significant difference in mean (SD) dairy calcium intake between racial groups was found (243 [273] mg for black women, 444 [360]
mg for white women, P < .001).
Back to top
Discussion
Calcium intake has received increased attention in the last decade because of its role in bone health and as a modifiable risk factor for osteoporosis.
The number of calcium-fortified food products being developed and marketed has increased substantially
(9). Although labeling for “excellent” (>200 mg/serving) and
“good” (100-200 mg/serving) sources of calcium are regulated by the Food and Drug Administration, there is no federal regulation regarding which foods can be fortified with calcium
or the degree of fortification (13). Together, these factors make discerning calcium intake difficult for researchers, clinicians, dietitians, and consumers. The primary findings of this study are that the CFFFQ identifies low calcium intakes and identifies key sources of calcium, including calcium-fortified foods.
Other studies have included either no calcium-fortified foods (14-18), calcium-fortified mineral water (19), calcium-fortified juice alone (20), calcium-fortified juice and a grain product (21), or did not provide details regarding the inclusion of calcium-fortified foods in the assessment tool (5,7,22-26). In contrast, the CFFFQ
is unique in providing 14 fortified food choices, including 1 in fruits, 8 in grains, and 5 in “other” food
categories. Fortification of foods can contribute greatly to total calcium intake.
From our data, inclusion of calcium-fortified foods in the diet has the potential to
increase total daily calcium intake by 1,000 mg or more. Because calcium fortification of food products is not federally regulated, food items being fortified and levels of fortification vary at the discretion of the manufacturer. The lack of regulation may hinder the role that these foods can play in dietary calcium intake by affecting
the consistency of the calcium content of the product.
The second unique feature of this study is the categorization of calcium intake estimates into food groups. Although total calcium intake is the primary focus in nutritional assessment studies,
the effectiveness of nutrition education and osteoporosis interventions can be
enhanced by focusing on calcium intake
from the food groups the participants usually get their calcium. This information can be used to design more realistic and targeted nutrition education messages. In our study, the
largest percentage of total calcium for both white and black women came from dairy, followed by grains and fruits. Although
the grain category contained several fortified food items, the fruit category contained only 1 fortified food item.
Even though consumption of fortified foods was assessed, dairy was still the primary calcium source
found in this study. An analysis (15) of food intake from the US Department of Agriculture’s 1994-1996, 1998 Continuing Survey of Food Intakes by Individuals (CSFII)
found that dairy contributed 42% of total calcium intake. A higher percentage of dairy contribution would have been expected from that study because it included no competing calcium-fortified foods. In addition, the CSFII reported 21% of
total calcium from calcium-rich mixed foods (ie, foods with 2 or more items
with calcium such as sandwiches or pizza). In our study, this category contributed only 4% to 5%. Ward et al (21) also reported that most calcium intake was derived from dairy, but a comparable calcium-rich mixed foods group is not identified. The food frequency assessment tool used by Ward et al (21) also ranked the fruits and vegetables group and grains as contributing 11% to 15% of total calcium, whereas the diet records used in the study estimated this contribution at 6% to 13%. Cook et al
(15) included no calcium-fortified foods, and the Ward et al (21) study was limited to calcium-fortified juice and 2 grain products.
There is a scarcity of information in the literature regarding calcium intake for black and white women. In our study, mean total calcium intake among black women did not meet the
adequate intake value whereas it did among white women. Other studies conclude that calcium intake is greater in white women than black women (27,28). However, an article published from the parent study of our study using the same CFFFQ found no difference in total, daily, dietary, or supplemental calcium (8). In
that analysis, black and white women were matched on age, socioeconomic status, and education level (n = 33
per group). The findings suggest that racial differences in calcium intake are somewhat influenced by
socioeconomic status and education level. Similarly, a comparison between black, white, and American Indian women also reported no significant difference in dietary calcium between black and white women (7).
In our study, grains were the second-highest calcium source for both black and white women. Grains are predominately calcium-fortified sources. This is consistent with findings from our previous work, which determined that dairy was the greatest source of calcium but more for white women, whereas black women consumed greater amounts of calcium-fortified grains (8). The prominent role of calcium-fortified foods in these studies reinforces the need for these sources to be carefully evaluated
when measuring calcium intake.
Limitations
The values from the CFFFQ were typically higher than those from the 24-hour recall, with the exception of vegetables and
“other” foods. This finding may be due in part to the limitations of using a 24-hour recall. Women may have identified foods in the CFFFQ but did not happen to consume those foods on the specific day of the recall, except for vegetables. However, Chee et al (24) found a similar trend in comparing a calcium-rich food frequency questionnaire
with a 3-day diary for postmenopausal Malaysian
women.
Assessing dietary intake by any method has inherent limitations. Validating food frequency questionnaires can be complicated without biomarkers for comparison. Because most nutrients do not yet have reliable biomarkers, 24-hour recalls or food records are the usual standard instruments. Correlations between these methods are considered adequate within the range of 0.4-0.7 (29). Although most of the correlations between total calcium and calcium from food groups when comparing CFFFQ to
24-hour recalls are significant, only total calcium intake, dairy calcium intake, and fruits fall within this acceptable statistical range.
Differences in reported calcium intake when comparing the CFFFQ and 24-hour recall could be attributed to a lack of consumer awareness of calcium fortification when responding to the 24-hour recall and a positive respondent bias on the CFFFQ. For example, participants could have responded more positively concerning calcium-fortified foods if consumption of that food was seen as a positive health behavior. Because calcium-fortified foods can essentially double calcium intake, consumer
awareness of their own calcium-fortified food product consumption and interviewer probe for each of these food items
are essential for an accurate estimate of calcium intake. To assist both the researcher and clinician, software for dietary assessment needs to be updated to include the calcium-fortified foods.
Several food frequency questionnaires that assess calcium intake have shown strong correlation
with food actually consumed (19,22-25,30,31). However, many studies report correlations but no difference between means or report findings regarding only total calcium intake and not calcium intake by individual food groups. In addition, many rapid assessment tools include either no or limited sources of calcium-fortified foods, and these foods may or may not be probed for on 24-hour recalls.
Conclusions
Our results suggest that the CFFFQ could be used to determine inadequate intakes of calcium. Primary calcium sources for all women were dairy
followed by grains, and calcium intake was higher in white women than in black women. The CFFFQ
can be used to more accurately identify calcium intakes and usual calcium
source, which is of interest because of
the increasing availability of calcium-fortified foods. Calcium-fortified sources can go unreported in 24-hour recalls and
diaries, leading to an underestimation of calcium intake. When 24-hour recalls are used to assess and quantify calcium intake, researchers and clinicians need to clarify with clients
whether the foods they ate were fortified. The CFFFQ may be used to better quantify calcium intake, including both natural and fortified sources. Accurate assessment of calcium is critical in evaluating bone health risks. This information can aid in the development of
effective interventions to increase calcium intake.
Back to top
Acknowledgments
The study was partially funded by the National Institutes of Health, R01AG020118 (principal investigator: Dr McAuley).
Back to top
Author Information
Corresponding Author: Karen L. Plawecki, MS, RD, Division of Nutritional Sciences, University of Illinois
at Urbana-Champaign, 345 Bevier Hall, 905 S Goodwin Ave, Urbana, IL 61801. Telephone: 217-244-2884. E-mail:
plawecki@illinois.edu.
Author Affiliations: Ellen M. Evans, Mina C. Mojtahedi, Edward McAuley, Karen Chapman-Novakofski, University of Illinois
at Urbana-Champaign, Urbana, Illinois.
Back to top
References
-
Nordin BE. Calcium and osteoporosis. Nutrition 1997;13(7-8):664-86.
-
Prince RL, Devine A, Dhaliwal SS, Dick IM.
Effects of calcium supplementation on clinical fracture and bone structure: results of a 5-year, double-blind, placebo-controlled trial in elderly women. Arch Intern Med 2006;24;166(8):869-75.
-
Reid IR, Mason B, Horne A, Ames R, Reid HE, Bava U, et al.
Randomized controlled trial of calcium in healthy older women. Am J Med 2006;119(9):777-85.
-
Daly RM, Bass S, Nowson C.
Long-term effects of calcium-vitamin-D3-fortified milk on bone geometry and strength in older men. Bone 2006;39(4):946-53.
-
Sebring NG, Denkinger BI, Menzie CM, Yanoff LB, Parikh SJ, Yanovski JA.
Validation of three food frequency questionnaires to assess dietary calcium intake in adults. J Am Diet Assoc 2007;107(5):752-9.
-
Jarvis JK, Miller GD.
Overcoming the barrier of lactose intolerance to reduce health disparities. J Natl Med Assoc 2002;94(2):55-66.
-
Bell RA, Quandt SA, Spangler JG, Case LD.
Dietary calcium intake and supplement use among older African American, white, and Native American women in a rural southeastern community. J Am Diet Assoc 2002;102(6):844-7.
-
Mojtahedi MC, Plawecki KL, Chapman-Novakofski KM, McAuley E, Evans EM.
Older black women differ in calcium intake source compared to age- and socioeconomic status-matched white women. J Am Diet Assoc 2006;106(7):1102-7.
-
Heaney RP, Rafferty K, Bierman J. Not all calcium-fortified beverages are equal. Nutrition Today 2005;40(1):39-44.
-
McAuley E, Morris KS, Doerksen SE, Motl RW, Liang H, White SM, et al.
Effects of change in physical activity on physical function limitations in older women: mediating roles of physical function performance and self-efficacy. J Am Geriatr Soc 2007;55(12):1967-73.
-
Dwyer J, Picciano MF, Raiten DJ, Members of the Steering Committee, National Health and Nutrition Examination Survey.
Collection of food and dietary supplement intake data: What We Eat in America — NHANES. J Nutr 2003;133(2):590S-600S.
-
Standing Committee on the Scientific Evaluation of Dietary Reference Intakes,
Food and Nutrition Board, Institute of Medicine. Dietary reference intakes for
calcium, phosphorus, magnesium, vitamin D, and fluoride. Washington (DC):
National Academy Press; 1997.
-
Food labeling guide. Silver Spring (MD): US Department of Health and Human
Services, Food and Drug Administration; 2009.
http://www.fda.gov/Food/GuidanceComplianceRegulatoryInformation/
GuidanceDocuments/FoodLabelingNutrition/FoodLabelingGuide/default.htm. Accessed June 9, 2009.
-
Magkos F, Manios Y, Babaroutsi E, Sidossis LS.
Development and validation of a food frequency questionnaire for assessing dietary calcium intake in the general population. Osteoporos Int 2006;17(2):304-12.
-
Cook AJ, Friday JE.
Food
mixture or ingredient sources for dietary calcium: shifts in food group
contributions using four grouping protocols. J Am Diet Assoc
2003;103(11):1513-9.
-
Yanek LR, Moy TF, Becker DM.
Comparison of food frequency and dietary recall methods in African-American women. J Am Diet Assoc 2001;101(11):1361-4.
-
Jensen JK, Gustafson D, Boushey CJ, Auld G, Bock MA, Bruhn CM, et al.
Development of a food frequency questionnaire to estimate calcium intake of Asian, Hispanic, and white youth. J Am Diet Assoc 2004;104(5):762-9.
-
Blalock SJ, Currey SS, DeVellis RF, Anderson JJ, Gold DT, Dooley MA.
Using a short food frequency questionnaire to estimate dietary calcium consumption: a tool for patient education. Arthritis Care Res 1998;11(6):479-84.
-
Montomoli M, Gonnelli S, Giacchi M, Mattei R, Cuda C, Rossi S, et al.
Validation of a food frequency questionnaire for nutritional calcium intake assessment in Italian women. Eur J Clin Nutr 2002;56(1):21-30.
-
Harnack LJ, Lytle LA, Story M, Galuska DA, Schmitz K, Jacobs DR Jr, et al.
Reliability and validity of a brief questionnaire to assess calcium intake of middle-school-aged children. J Am Diet Assoc 2006;106(11):1790-5.
-
Ward KD, Hunt KM, Berg MB, Slawson DA, Vukadinovich CM, McClanahan BS, et al.
Reliability and validity of a brief questionnaire to assess calcium intake in female collegiate athletes. Int J Sport Nutr Exerc Metab 2004;14(2):209-21.
-
Blalock SJ, Norton LL, Patel RA, Cabral K, Thomas CL.
Development and assessment of a short instrument for assessing dietary intakes of calcium and vitamin D. J Am Pharm Assoc (2003) 2003;43(6):685-93.
-
Musgrave KO, Giambalvo L, Leclerc HL, Cook RA, Rosen CJ.
Validation of a quantitative food frequency questionnaire for rapid assessment of dietary calcium intake. J Am Diet Assoc 1989;89(10):1484-8.
-
Chee WS, Suriah AR, Zaitun Y, Chan SP, Yap SL, Chan YM.
Dietary calcium intake in postmenopausal Malaysian women: comparison between the food frequency questionnaire and three-day food records. Asia Pac J Clin Nutr 2002;11(2):142-6.
-
Taitano RT, Novotny R, Davis JW, Ross PD, Wasnich RD.
Validity of a food frequency questionnaire for estimating calcium intake among Japanese and white women. J Am Diet Assoc 1995;95(7):804-6.
-
Xu L, Porteous JE, Phillips MR, Zheng S.
Development and validation of a calcium intake questionnaire for postmenopausal women in China. Ann Epidemiol 2000;10(3):169-75.
-
Pereira MA, Jacobs DR Jr, Van Horn L, Slattery ML, Kartashov AI, Ludwig DS.
Dairy
consumption, obesity, and the insulin resistance syndrome in young adults: the CARDIA Study. JAMA 2002;287(16):2081-9.
-
Lee JS, Weyant RJ, Corby P, Kritchevsky SB, Harris TB, Rooks R, et al.
Edentulism
and nutritional status in a biracial sample of well-functioning,
community-dwelling elderly: the Health, Aging, and Body Composition Study. Am J Clin Nutr 2004;79(2):295-302.
-
Subar AF. Developing dietary assessment tools. J Am Diet Assoc 2004;104(5):769-70.
-
Green JH, Booth CL, Bunning RL.
Assessment of a rapid method for assessing adequacy of calcium intake. Asia Pac J Clin Nutr 2002;11(2):147-50.
-
Pasco JA, Sanders KM, Henry MJ, Nicholson GC, Seeman E, Kotowicz MA.
Calcium intakes among Australian women: Geelong Osteoporosis Study. Aust N Z J Med 2000;30(1):21-7.
Back to top
|
|
