

|

|

Volume
6: No. 2, April 2009
ORIGINAL RESEARCH
Cholesterol Screening by Marital Status and Sex in the United States
Jim P. Stimpson, PhD, Fernando A. Wilson, PhD
Suggested citation for this article: Stimpson JP, Wilson FA. Cholesterol screening by marital status and sex in the United States. Prev Chronic Dis 2009;6(2):A55.
http://www.cdc.gov/pcd/issues/2009/
apr/08_0102.htm. Accessed [date].
PEER REVIEWED
Abstract
Introduction
Marital status may be a predisposing factor related to preventive
health screenings, which may in part explain the
“healthy marriage” effect. This
study investigates differences in the likelihood of being screened for cholesterol by marital status for men and women.
Methods
Medical Expenditure Panel Surveys from 2003 through 2005 were used to calculate the likelihood of self-reported cholesterol screening in the past year by marital status and sex. Several rounds of interviews during a 2-year period resulted in
a sample of 36,594 US adults.
Results
Most married, widowed, and divorced/separated people reported cholesterol screening in the past year. The highest percentages of people being screened for cholesterol were widowed men (75%) and women (81%). By contrast, 26% of single men and 38% of single women reported cholesterol screening. In multivariate models,
being unmarried was associated with lower odds of cholesterol screening among
men and women. The lowest likelihood of screening was associated with widowed status for both men (odds
ratio, 0.56)
and women (odds ratio, 0.53).
Conclusion
Marital status is a predisposing factor for cholesterol screening. Public health
interventions aimed at improving preventive screening should focus on social
networks, especially family members.
Back to top
Introduction
Marriage is associated with positive health outcomes, the mechanisms for
which are unclear (1,2). This “healthy marriage” effect results when marital partners are motivated to maintain their health because they feel obligated to other family members who depend on them for economic security and social support (3,4). In contrast, differences in health
that are associated with marital status may be viewed as a self-selection effect.
People who marry may be healthier than those who remain single, and
people who recently were divorced or widowed will initially be less healthy compared
with people who are continuously married.
A difference in health-promoting behaviors could partly explain the healthy marriage effect. Married
people tend to eat healthier, smoke less, and drink less
than unmarried people (5-13). Health-promoting behaviors are likely to be conditional on both sex and marital status. Differences in mortality and morbidity rates are greatest for married men
compared with unmarried men, and married
women do not have better health compared with women of other marital statuses (14,15). Limited evidence suggests that women might have some influence over men's screening behavior (16-19). A recent study documented
that husbands are screened at approximately the same rate as their wives (13). However,
to our knowledge no study has specifically examined whether preventive health screenings vary by marital status and sex.
This study uses nationally representative data to determine whether the likelihood of having cholesterol screening
differs by marital status for men and women. We
expected women to be more likely to seek cholesterol screening than men. Married men and women
were expected to be more likely to seek cholesterol screenings than were unmarried men and women.
Back to top
Methods
Data
We used the most recent data available from the Medical Expenditure Panel Survey (MEPS), a set of large-scale, rotating panel surveys of
people, their medical providers, and employers across the United States (20). The panel design of the survey, which features several rounds of interviewing covering 2 full calendar years, enables us to examine changes in health service use, health conditions, and behavior. MEPS
has 2 major components: the household component is a nationally representative
subsample of people drawn from the National Health Interview Survey (NHIS), and
the medical provider component collects information from respondents’ health
care providers to supplement and verify information provided by respondents in
the household component. The breadth of information collected on health service
use and predictors of service use places MEPS among the best data sources for understanding differences in prevention screening.
Person-level weights for MEPS adjust for nonresponse over time and reflect Current Population Survey estimates
on the basis of 6 variables (race/ethnicity, sex, age, poverty status, region of residence, and urban or rural residence).
Because of this weighting scheme, estimates from MEPS are generalizable to the US civilian, noninstitutionalized population. MEPS estimates do not cover households
that were created after the NHIS interviews for the respective panels or people not covered by a given MEPS panel, such as people leaving the military, US citizens returning from residence in another country, and people leaving institutions. However, people or households not covered
make up a small proportion of the MEPS target population. The final sample size is 36,594 adults with complete information on marital status and cholesterol screening from 2003 through 2005.
Variables
The outcome variable for this study is cholesterol screening in the past year, measured as a binary self-reported indicator. The independent variable of interest is marital status, which is enumerated separately by
people reporting whether they were married, divorced/separated, widowed, or never married. Socioeconomic factors included
age, race/ethnicity, family size, urban versus rural residence, region of the
country, years of education, occupation, and mean annual household income.
Health behavior indicator variables were current smoking status, obesity status,
and physical activity (specifically, whether the respondent engaged in moderate
to vigorous physical activity at least 3 times weekly). Variables that measured
access to health care were type of health insurance and having a usual health care provider. Health conditions were assessed
by self-reports of 1) the mean annual number of
prescriptions and 2) whether a doctor had ever told the
respondent that he or she had had a stroke, heart attack, coronary heart disease, angina, other heart disease, diabetes, or high blood pressure.
Statistical analysis
Stata version 9 SE (StataCorp LP, College Station, Texas) was used to adjust for the sample weights, strata, and population sampling units. Mean values with confidence intervals for all study variables
were calculated by marital status and sex. Multivariate logit regression modeled the odds of having cholesterol screening by marital status for men and women. Correlation ratios
were calculated for a stepped-in regression to estimate which group of predictors
was most closely associated with screening.
Predicted probabilities of screening across age were computed for married and unmarried men and women. The probabilities
were generated from the multivariate logit estimates. Interaction terms for age, marital status, and sex were created to test for significant differences in cholesterol screening for married and unmarried men and women by age.
Back to top
Results
Most married, widowed, and divorced/separated people reported
cholesterol screening in the past year. The highest percentage of people who
reported being screened for cholesterol was widowed men (75%) and women
(81%). By contrast, 26% of single men and 38% of single women reported
cholesterol screening (Table 1 and Table 2).
Unmarried men and women
had significantly lower odds of getting screened for cholesterol (Table 3). The lowest likelihood of screening was associated with widowed status for both men (OR, 0.56) and women (OR, 0.53). However, among men the confidence intervals overlapped,
which suggests that cholesterol screening does not vary within categories of
unmarried respondents. Among
women, the confidence intervals for widowed status overlapped for divorced/separated but did not overlap for never married status,
which suggests some order in the odds within marital status categories.
Table 4 shows the change in correlation ratios as various categories of screening predictors are stepped into the regression equation. The baseline model shows the correlation ratio for marital status and cholesterol screening. The change in correlation ratios is used to interpret how much the correlation ratio increased from baseline. Therefore, marital status
was the strongest predictor of screening for women (0.17) and the second strongest factor for men (0.15). The
first adjustment factor stepped in was age. The change in correlation ratios column suggests that, for men, age was the strongest predictor of cholesterol screening (0.22) and, for women, it was the second strongest predictor (0.16).
For both men and women, access to care was the next predictor most strongly correlated with screening, followed by health conditions, socioeconomic factors, and health behaviors.
Screening was lowest in younger age groups and increased with age
(Figure). Most people aged 35
years or younger reported not having had cholesterol screening. By contrast,
most people aged 50 years or older reported cholesterol screening. The
difference in screening through age 50 was significant within marital status.
Until age 50, unmarried women and men were screened at lower rates. After age 50, no significant difference in screening
was seen for men or women regardless of marital status (data not shown).
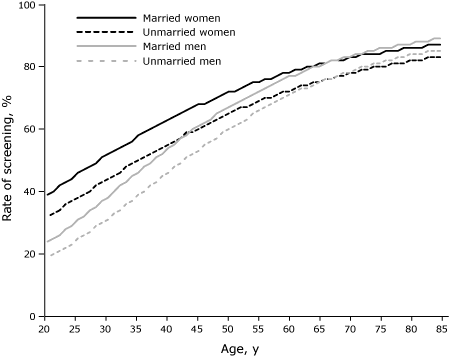
Figure. Rate of cholesterol screening during the previous
year,
by age among married and unmarried men and women, 2003-2005 Medical Expenditure Panel Survey.
[A tabular version of this figure is also available.]
Back to top
Discussion
Results from this study indicate that cholesterol screening varies by marital status among men and women. In part, this finding supports the theory that married relationships may lead people to seek preventive care because they are motivated to stay healthy for the sake of their family (3,4). Other research has speculated that a mechanism for the health-promoting effect of marriage is that women’s role in the family may be to encourage family members, especially
husbands, to be screened (14,15,18). Even if men are not the health gatekeeper for the family, most married men still acknowledge an economic and social obligation to their family, which may motivate them to
be screened.
There was a difference in the probabilities of screening across marital status categories before and after adjustment for factors related to screening. Unadjusted results suggested that people in the widowed category had the highest probability of screening, but after adjustment for relevant factors, widowed status was associated with the lowest likelihood of screening. The unadjusted rates for widowed status reflect that older people are more likely to be screened for
cholesterol than are younger people. Older people are more likely to need and seek health care
than are younger
people. In fact, sex differences in cholesterol screening early in life may be explained by recommendations that women get annual gynecologic examinations
(at which other kinds of screening may occur), but no annual examination is recommended
for young men. Therefore, adjusting for age and other factors associated with screening
allowed respondents to be considered equally on the basis of those factors,
which suggests
that widowed people of the same age, socioeconomic status, health behaviors, and conditions
are less likely than married, divorced/separated, and never married
people to be screened for cholesterol.
We also studied the strength of the association for the groups of factors
associated with cholesterol screening. These results showed that marital status
is one of the strongest factors in explaining screening differences, even beyond
health behaviors and health conditions. Although marital status had the highest correlation ratio for women and second highest for men, these results should be interpreted cautiously. Marital status is correlated with other factors such as age, income, and health behaviors
and conditions. Therefore, the initial correlation of marital status with screening also reflects unobserved correlation with these other factors. However, a reasonable conclusion to draw for this analysis is that marital status
predicts the likelihood of cholesterol screening.
We could not adequately test the self-selection hypothesis, which suggests that differences in health by marital status arise from unobservable, idiosyncratic characteristics of
people choosing a given marital status. A reasonable strategy to test this hypothesis would be to use prospective panel data over a sufficiently long time period that could capture changes in health behaviors associated with transitions between marital statuses. MEPS is a 2-year, rotating panel data set, and
too few cases of marital transitions occurred during a 2-year period to draw
reasonable conclusions about the self-selection hypothesis. Therefore, these results should be viewed cautiously, given
that the married population may
comprise people who are more likely to seek preventive care.
One suggestion to improve screening may be to invite both spouses for the health service visit, which has been associated with increased screening behavior (17). This initiative could be especially helpful for reducing the gap between younger married men and women. Increasing screening among unmarried men may be challenging. Men who are not tied to family responsibilities may feel less obligated to prevent
disease compared with men who have family obligations. However, marital status is only 1 component of a person’s social network. Recent studies of social networks and health behaviors found that even distant members of a social network can have profound effects on health behaviors (21,22). Therefore, public health interventions should focus on increasing screening among social networks
that include children, family members, and friends.
Back to top
Author Information
Corresponding Author: Jim P. Stimpson, PhD, Department of Social and Behavioral Sciences, University of North Texas Health Science Center, 3500 Camp Bowie Blvd, Fort Worth, TX 76107-2699. Telephone: 817-735-2365. E-mail:
jstimpso@hsc.unt.edu.
Author Affiliations: Fernando A. Wilson, University of North Texas Health Science Center, Fort Worth, Texas.
Back to top
References
- Kiecolt-Glaser JK, Newton TL.
Marriage and health: his and hers. Psychol Bull 2001;127:472-503.
- Williams K, Umberson D.
Marital status, marital transitions, and health: a sexed life course perspective. J Health Soc Behav 2004;45:81-98.
- Umberson D.
Gender, marital status, and the social control of health behavior. Soc Sci Med 1992;34:907-17.
- Lewis MA, McBride CM, Pollak KI, Puleo E, Butterfield RM, Emmons KM.
Understanding health behavior change among couples: an interdependence and communal coping approach. Soc Sci Med 2006;62:1369-80.
- Broman C.
Social relationships and health-related behavior. J Behav Med 1993;16:335-50.
- Eng PM, Kawachi I, Fitzmaurice G, Rimm EB.
Effects of marital transitions on changes in dietary and other health behaviours in US male health professionals. J Epidemiol Community Health 2005;59:56-62.
- Schone BS, Weinick RM.
Health-related behaviors and the benefits of marriage for elderly persons. Gerontologist 1998;38:618-27.
- Sobal J, Rauschenbach BS, Frongillo EA.
Marital status changes and body weight changes: a US longitudinal analysis. Soc Sci Med 2003;56:1543-55.
- Stimpson JP, Lackan NA.
Serum carotenoid levels vary by marital status. J Am Diet Assoc 2007;107:1581-5.
- Homish GG, Leonard KE.
Spousal influence on smoking behaviors in a US community sample of newly married couples. Soc Sci Med 2005;61:2557-67.
- Meyler D, Stimpson JP, Peek MK.
Health concordance within couples: a systematic review. Soc Sci Med 2007;64:2297-310.
- Stimpson JP, Masel MC, Rudkin L, Peek MK.
Shared health behaviors among older Mexican American
spouses. Am J Health Behav 2006;30:495-502.
- Falba TA, Sindelar JL.
Spousal concordance in health behavior change. Health Serv Res 2008;43:96-116.
- Chipperfield JG, Havens B.
Gender
differences in the relationship between marital status transitions and life
satisfaction in later life. J Gerontol Psychol Sci 2001;56B:P176-86.
- Stimpson JP, Kuo YF, Ray LA, Raji MA, Peek MK.
Risk of mortality related to widowhood in older Mexican Americans. Ann Epidemiol 2007;17:313-9.
- Tudiver F, Talbot Y.
Why don't men seek help? Family physicians’ perspectives on help-seeking
behavior in men. J Fam Pract 1999;48:47-52.
- van Jaarsveld CH, Miles A, Edwards R, Wardle J.
Marriage and cancer prevention: does marital status and inviting both spouses together influence colorectal cancer screening participation? J Med Screen 2006;13:172-6.
- Norcross WA, Ramirez C, Palinkas LA.
The influence of women on the health care seeking behavior of men. J Fam Pract 1996;43:475-80.
- Seymour-Smith S, Wetherell M, Phoenix A. ‘My wife ordered me to come’: a
discursive analysis of doctors’ and nurses’ accounts of men’s use of general practitioners. J Health Psychol 2002;7:253-67.
- Cohen JW, Monheit AC, Beauregard KM. The Medical Expenditure Panel Survey: a national health information resource. Inquiry 1996;33:373-89.
- Christakis NA, Fowler JH.
The spread of obesity in a large social network over 32 years. N Engl J Med 2007;357:370-9.
- Christakis NA, Fowler JH.
The collective dynamics of smoking in a large social network. N Engl J Med 2008;358:2249-58.
Back to top
|
|
